Abstract
Background
Myelomeningocele (MMC) is often related to hydrocephalus and Chiari malformation (CM) type 2; however, other brain abnormalities have been reported in this population. In order to better understand and quantify other forebrain abnormalities, we analyzed magnetic resonance imaging (MRI) of MMC patients treated in utero or postnatal.
Methods
Between January 2014 and March 2017, 59 MMC were treated in our hospital. Thirty-seven patients (32 postnatal and 5 intrautero repair) had brain MRI and were enrolled at the study. MRI was analyzed by two experienced neuroradiologists to identify the supra and infratentorial brain abnormalities.
Results
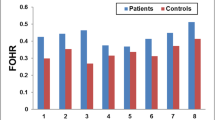
A wide range of brain abnormalities was consistently identified in MMC patients. As expected, the most common were hydrocephalus (94.5%) and CM type II (89.1%). Of note, we found high incidence of corpus callosum abnormalities (86.4%), mostly represented by dysplasia (46%).
Conclusions
The data are consistent with the concept that brain abnormalities related to MMC can be both infratentorial and supratentorial, cortical, and subcortical. More studies are needed to correlate these forebrain abnormalities to long-term functional outcome and their prognostic value for these patients.





Similar content being viewed by others
References
Alexiou GA, Zarifi MK, Georgoulis G et al (2011) Cerebral abnormalities in infants with myelomeningocele. Neurol Neurochir Pol 45:18–23. https://doi.org/10.1016/S0028-3843(14)60055-4
Bekiesinska-Figatowska M, Duczkowska A, Brągoszewska H et al (2014) Stenogyria - Not only in Chiari II malformation. J Neurol Sci 347:337–340. https://doi.org/10.1016/j.jns.2014.09.022
Copp AJ, DE Greene N (2014) Europe PMC Funders Group Neural tube defects – disorders of neurulation and related embryonic processes. Wiley Interdiscip Rev Dev Biol 2:213–227. https://doi.org/10.1002/wdev.71.Neural
Crawley JT, Hasan K, Hannay HJ et al (2014) Structure, integrity, and function of the hypoplastic corpus callosum in spina bifida myelomeningocele. Brain Connect 4:608–618. https://doi.org/10.1089/brain.2014.0237
Dias M, Partington M (2015) Congenital Brain and Spinal Cord Malformations and Their Associated Cutaneous Markers. Pediatrics 136:e1105–e1119. https://doi.org/10.1542/peds.2015-2854
Gilbert JN, Jones KL, Rorke LB et al (1986) Central Nervous System Anomalies Associated with Meningomyelocele, Hydrocephalus, and the Arnold-Chiari Malformation: Reappraisal of Theories Regarding the Pathogenesis of Posterior Neural Tube Closure Defects. Neurosurgery 18:559–564
Glenn OA, Barkovich AJ (2006) Magnetic resonance imaging of the fetal brain and spine: an increasingly important tool in prenatal diagnosis, part 1. Am J Neuroradiol 27:1604
Hasan KM, Eluvathingal TJ, Kramer LA et al (2008) White matter microstructural abnormalities in children with spina bifida myelomeningocele and hydrocephalus: a diffusion tensor tractography study of the association pathways. J Magn Reson Imaging 27:700–709. https://doi.org/10.1002/jmri.21297
Kawamura T, Marioka T, Nishio S et al (2001) Cerebral abnormalities in lumbosacral neural tube closure defect: MR imaging evaluation. Childs Nerv Syst 17:405–410. https://doi.org/10.1007/s003810000439
McLone DG, Knepper PA (1989) The cause of Chiari II malformation: a unified theory. Pediatr Neurosci 15:1–12
Miller E, Widjaja E, Blaser S et al (2008) The old and the new: Supratentorial MR findings in Chiari II malformation. Childs Nerv Syst 24:563–575. https://doi.org/10.1007/s00381-007-0528-x
Glenn OA, Barkovich AJ (2006) Magnetic resonance imaging of the fetal brain and spine: An increasingly important tool in prenatal diagnosis: Part 2. Am J Neuroradiol 27:1604–1611
O’Hayon BB, Drake JM, Ossip MG et al (1998) Frontal and occipital horn ratio: A linear estimate of ventricular size for multiple imaging modalities in pediatric hydrocephalus. Pediatr Neurosurg 29:245–249. https://doi.org/10.1159/000028730
Rethmann C, Scheer I, Meuli M et al (2017) Evolution of posterior fossa and brain morphology after in utero repair of open neural tube defects assessed by MRI. Eur Radiol 27:4571–4580. https://doi.org/10.1007/s00330-017-4807-y
Treble A, Juranek J, Stuebing KK et al (2013) Functional significance of atypical cortical organization in spina bifida myelomeningocele: Relations of cortical thickness and gyrification with IQ and fine motor dexterity. Cereb Cortex 23:2357–2369. https://doi.org/10.1093/cercor/bhs226
Tulipan N, Bruner JP, Hernanz-Schulman M et al (1999) Effect of intrauterine myelomeningocele repair on central nervous system structure and function. Pediatr Neurosurg 31:183–188. https://doi.org/10.1159/000028859
Ware AL, Juranek WVJ et al (2014) Anatomical and diffusion MRI of deep gray matter in pediatric spina bifida. NeuroImage Clin 5:120–127. https://doi.org/10.1016/j.nicl.2014.05.012
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 88 kb)
Rights and permissions
About this article
Cite this article
Morais, B.A., Solla, D.J.F., Yamaki, V.N. et al. Brain abnormalities in myelomeningocele patients. Childs Nerv Syst 36, 1507–1513 (2020). https://doi.org/10.1007/s00381-019-04386-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-019-04386-8