Abstract
Purpose
The supplementary motor area (SMA) syndrome affects adults after tumour resection in SMA neighbouring motor cortex. Cerebellar mutism syndrome (CMS) affects children after tumour resection in the posterior fossa. Both syndromes include disturbances in speech and motor function. The causes of the syndromes are unknown; however, surgical damage to the dentato-thalamo-cortical pathway (DTCP) has been associated with CMS. Thus, an anatomical link between the areas associated with the syndromes is possible.
We discuss the syndromes and their possible relationship through the DTCP.
Methods
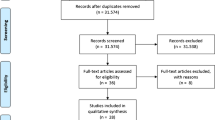
We identified 61 articles (cohort studies, case reports and reviews) in MEDLINE and Embase searching for CMS, SMA syndrome or DTCP or synonyms and reviewed for evidence linking CMS and SMA.
Results
We found that SMA syndrome and CMS are similar regarding (1) surgical causation; (2) symptoms including speech impairment, disturbance in motor function and facial dysfunction; (3) delayed onset; (4) the courses of the syndromes are transient; and (5) long-term sequelae are seen in both. Relevant differences include age predominance of adults in SMA syndrome versus children in CMS.
Conclusions
The similarities of the two syndromes could be traced back to their mutual connection through the DTCP and their membership to a cerebro-cerebellar circuit. The connectivity network could explain the emotional changes and speech reduction in CMS. The difference in time of post-surgical onset may be related to the anatomical distance between the surgical damage to the cerebellum and the SMA, respectively, and the effector neural loop underpinning symptoms.

Similar content being viewed by others
References
Akil H (2006) Re: cerebellar mutism in adults after posterior fossa surgery: a report of 2 cases (Sherman JH et al. Surg Neurol 2005;63:476-9). Surg Neurol 65:424. https://doi.org/10.1016/j.surneu.2005.12.023
Akkal D, Dum RP, Strick PL (2007) Supplementary motor area and presupplementary motor area: targets of basal ganglia and cerebellar output. J Neurosci 27:10659–10673. https://doi.org/10.1523/jneurosci.3134-07.2007
Avula S, Spiteri M, Kumar R, Lewis E, Harave S, Windridge D, Ong C, Pizer B (2016) Post-operative pediatric cerebellar mutism syndrome and its association with hypertrophic olivary degeneration. Quant Imaging Med Surg 6:535–544. https://doi.org/10.21037/qims.2016.10.11
Baker CM, Burks JD, Briggs RG, Smitherman AD, Glenn CA, Conner AK, Wu DH, Sughrue ME (2018) The crossed frontal aslant tract: a possible pathway involved in the recovery of supplementary motor area syndrome. Brain Behav 8:e00926. https://doi.org/10.1002/brb3.926
Basu AP, Taylor PN, Lowther E, Forsyth EO, Blamire AM, Forsyth RJ (2015) Structural connectivity in a paediatric case of anarchic hand syndrome. BMC Neurol 15:234. https://doi.org/10.1186/s12883-015-0477-z
Cakir Y, Karakisi D, Kocanaogullari O (1994) Cerebellar mutism in an adult: case report. Surg Neurol 41:342–344
Catani M, Dell'acqua F, Vergani F, Malik F, Hodge H, Roy P, Valabregue R, Thiebaut de Schotten M (2012) Short frontal lobe connections of the human brain. Cortex 48:273–291. https://doi.org/10.1016/j.cortex.2011.12.001
Crutchfield JS, Sawaya R, Meyers CA, Moore BD 3rd (1994) Postoperative mutism in neurosurgery. Report of two cases. J Neurosurg 81:115–121. https://doi.org/10.3171/jns.1994.81.1.0115
Dailey AT, McKhann GM 2nd, Berger MS (1995) The pathophysiology of oral pharyngeal apraxia and mutism following posterior fossa tumor resection in children. J Neurosurg 83:467–475. https://doi.org/10.3171/jns.1995.83.3.0467
D'Avanzo R, Scuotto A, Natale M, Scotto P, Cioffi FA (1993) Transient "cerebellar" mutism in lesions of the mesencephalic-cerebellar region. Acta Neurol 15:289–296
De Smet HJ, Baillieux H, Wackenier P, De Praeter M, Engelborghs S, Paquier PF, De Deyn PP, Marien P (2009) Long-term cognitive deficits following posterior fossa tumor resection: a neuropsychological and functional neuroimaging follow-up study. Neuropsychology 23:694–704. https://doi.org/10.1037/a0016106
De Smet HJ, Paquier P, Verhoeven J, Marien P (2013) The cerebellum: its role in language and related cognitive and affective functions. Brain Lang 127:334–342. https://doi.org/10.1016/j.bandl.2012.11.001
Della Sala S, Francescani A, Spinnler H (2002) Gait apraxia after bilateral supplementary motor area lesion. J Neurol Neurosurg Psychiatry 72:77–85
Duffau H (2012) Cortical and subcortical brain mapping. In: Schmidek and sweet - operative neurosurgical techniques, pp 80–93
Duffau H, Lopes M, Denvil D, Capelle L (2001) Delayed onset of the supplementary motor area syndrome after surgical resection of the mesial frontal lobe: a time course study using intraoperative mapping in an awake patient. Stereotact Funct Neurosurg 76:74–82. https://doi.org/10.1159/000056496
Dunwoody GW, Alsagoff ZS, Yuan SY (1997) Cerebellar mutism with subsequent dysarthria in an adult: case report. Br J Neurosurg 11:161–163
Fontaine D, Capelle L, Duffau H (2002) Somatotopy of the supplementary motor area: evidence from correlation of the extent of surgical resection with the clinical patterns of deficit. Neurosurgery 50:297–303 discussion 303-295
Gedik GK, Sari O, Koktekir E, Akdemir G (2017) Fluorodeoxyglucose positron emission tomography/computed tomography findings in a patient with cerebellar mutism after operation in posterior fossa. Asian J Surg 40:166–170. https://doi.org/10.1016/j.asjsur.2014.01.004
Gudrunardottir T, Morgan AT, Lux AL, Walker DA, Walsh KS, Wells EM, Wisoff JH, Juhler M, Schmahmann JD, Keating RF, Catsman-Berrevoets C (2016) Consensus paper on post-operative pediatric cerebellar mutism syndrome: the Iceland Delphi results. Child’s Nervous Syst 32:1195–1203. https://doi.org/10.1007/s00381-016-3093-3
Han S, Wang Z, Wang Y, Wu A (2013) Transcerebellomedullary fissure approach to lesions of the fourth ventricle: less is more? Acta Neurochir 155:1011–1016. https://doi.org/10.1007/s00701-013-1689-x
Heiferman DM, Ackerman PD, Hayward DM, Primeau MJ, Anderson DE, Prabhu VC (2014) Bilateral supplementary motor area syndrome causing akinetic mutism following parasagittal meningioma resection. Neurosci Discov 2. https://doi.org/10.7243/2052-6946-2-7
Ildan F, Tuna M, Erman T, Gocer AI, Zeren M, Cetinalp E (2002) The evaluation and comparison of cerebellar mutism in children and adults after posterior fossa surgery: report of two adult cases and review of the literature. Acta Neurochir 144:463–473. https://doi.org/10.1007/s007010200067
Kasasbeh AS, Yarbrough CK, Limbrick DD, Steger-May K, Leach JL, Mangano FT, Smyth MD (2012) Characterization of the supplementary motor area syndrome and seizure outcome after medial frontal lobe resections in pediatric epilepsy surgery. Neurosurgery 70:1152–1168; discussion 1168. https://doi.org/10.1227/NEU.0b013e31823f6001
Krainik A, Duffau H, Capelle L, Cornu P, Boch AL, Mangin JF, Le Bihan D, Marsault C, Chiras J, Lehericy S (2004) Role of the healthy hemisphere in recovery after resection of the supplementary motor area. Neurology 62:1323–1332
Laplane D, Talairach J, Meininger V, Bancaud J, Orgogozo JM (1977) Clinical consequences of corticectomies involving the supplementary motor area in man. J Neurol Sci 34:301–314
Law N, Greenberg M, Bouffet E, Taylor MD, Laughlin S, Strother D, Fryer C, McConnell D, Hukin J, Kaise C, Wang F, Mabbott DJ (2012) Clinical and neuroanatomical predictors of cerebellar mutism syndrome. Neuro-oncology 14:1294–1303. https://doi.org/10.1093/neuonc/nos160
Marien P, De Smet HJ, Wijgerde E, Verhoeven J, Crols R, De Deyn PP (2013) Posterior fossa syndrome in adults: a new case and comprehensive survey of the literature. Cortex 49:284–300. https://doi.org/10.1016/j.cortex.2011.06.018
Marien P, Ackermann H, Adamaszek M, Barwood CH, Beaton A, Desmond J, De Witte E, Fawcett AJ, Hertrich I, Kuper M, Leggio M, Marvel C, Molinari M, Murdoch BE, Nicolson RI, Schmahmann JD, Stoodley CJ, Thurling M, Timmann D, Wouters E, Ziegler W (2014) Consensus paper: language and the cerebellum: an ongoing enigma. Cerebellum (London, England) 13:386–410. https://doi.org/10.1007/s12311-013-0540-5
McEvoy SD, Lee A, Poliakov A, Friedman S, Shaw D, Browd SR, Ellenbogen RG, Ojemann JG, Mac Donald CL (2016) Longitudinal cerebellar diffusion tensor imaging changes in posterior fossa syndrome. NeuroImage Clin 12:582–590. https://doi.org/10.1016/j.nicl.2016.09.007
Miller NG, Reddick WE, Kocak M, Glass JO, Lobel U, Morris B, Gajjar A, Patay Z (2010) Cerebellocerebral diaschisis is the likely mechanism of postsurgical posterior fossa syndrome in pediatric patients with midline cerebellar tumors. AJNR Am J Neuroradiol 31:288–294. https://doi.org/10.3174/ajnr.A1821
Morris EB, Phillips NS, Laningham FH, Patay Z, Gajjar A, Wallace D, Boop F, Sanford R, Ness KK, Ogg RJ (2009) Proximal dentatothalamocortical tract involvement in posterior fossa syndrome. Brain 132:3087–3095. https://doi.org/10.1093/brain/awp241
Moxon-Emre I, Bouffet E, Taylor MD, Laperriere N, Scantlebury N, Law N, Spiegler BJ, Malkin D, Janzen L, Mabbott D (2014) Impact of craniospinal dose, boost volume, and neurologic complications on intellectual outcome in patients with medulloblastoma. J Clin Oncol 32:1760–1768. https://doi.org/10.1200/jco.2013.52.3290
Nachev P, Kennard C, Husain M (2008) Functional role of the supplementary and pre-supplementary motor areas. Nat Rev Neurosci 9:856–869. https://doi.org/10.1038/nrn2478
Palmer SL, Hassall T, Evankovich K, Mabbott DJ, Bonner M, Deluca C, Cohn R, Fisher MJ, Morris EB, Broniscer A, Gajjar A (2010) Neurocognitive outcome 12 months following cerebellar mutism syndrome in pediatric patients with medulloblastoma. Neuro-oncology 12:1311–1317. https://doi.org/10.1093/neuonc/noq094
Patay Z (2015) Postoperative posterior fossa syndrome: unraveling the etiology and underlying pathophysiology by using magnetic resonance imaging. Child’s Nervous Syst 31:1853–1858. https://doi.org/10.1007/s00381-015-2796-1
Patay Z, Enterkin J, Harreld JH, Yuan Y, Lobel U, Rumboldt Z, Khan R, Boop F (2014) MR imaging evaluation of inferior olivary nuclei: comparison of postoperative subjects with and without posterior fossa syndrome. AJNR Am J Neuroradiol 35:797–802. https://doi.org/10.3174/ajnr.A3762
Peraud A, Meschede M, Eisner W, Ilmberger J, Reulen HJ (2002) Surgical resection of grade II astrocytomas in the superior frontal gyrus. Neurosurgery 50:966–975 discussion 975-967
Pitsika M, Tsitouras V (2013) Cerebellar mutism. J Neurosurg Pediatr 12:604–614. https://doi.org/10.3171/2013.8.peds13168
Pollack IF, Polinko P, Albright AL, Towbin R, Fitz C (1995) Mutism and pseudobulbar symptoms after resection of posterior fossa tumors in children: incidence and pathophysiology. Neurosurgery 37:885–893
Potgieser AR, de Jong BM, Wagemakers M, Hoving EW, Groen RJ (2014) Insights from the supplementary motor area syndrome in balancing movement initiation and inhibition. Front Hum Neurosci 8:960. https://doi.org/10.3389/fnhum.2014.00960
Radman N, Cacioppo S, Spierer L, Schmidlin E, Mayer E, Annoni JM (2013) Posterior SMA syndrome following subcortical stroke: contralateral akinesia reversed by visual feedback. Neuropsychologia 51:2605–2610. https://doi.org/10.1016/j.neuropsychologia.2013.08.004
Ramnani N (2006) The primate cortico-cerebellar system: anatomy and function. Nat Rev Neurosci 7:511–522. https://doi.org/10.1038/nrn1953
Reed-Berendt R, Phillips B, Picton S, Chumas P, Warren D, Livingston JH, Hughes E, Morrall MC (2014) Cause and outcome of cerebellar mutism: evidence from a systematic review. Child's Nervous Syst 30:375–385. https://doi.org/10.1007/s00381-014-2356-0
Robertson PL, Muraszko KM, Holmes EJ, Sposto R, Packer RJ, Gajjar A, Dias MS, Allen JC (2006) Incidence and severity of postoperative cerebellar mutism syndrome in children with medulloblastoma: a prospective study by the Children’s Oncology Group. J Neurosurg 105:444–451. https://doi.org/10.3171/ped.2006.105.6.444
Rostomily RC, Berger MS, Ojemann GA, Lettich E (1991) Postoperative deficits and functional recovery following removal of tumors involving the dominant hemisphere supplementary motor area. J Neurosurg 75:62–68. https://doi.org/10.3171/jns.1991.75.1.0062
Russell SM, Kelly PJ (2003) Incidence and clinical evolution of postoperative deficits after volumetric stereotactic resection of glial neoplasms involving the supplementary motor area. Neurosurgery 52:506–516 discussiom 515-506
Ryu JS, Chun MH, You DS (2013) Supplementary motor area syndrome and flexor synergy of the lower extremities. Ann Rehabil Med 37:735–739. https://doi.org/10.5535/arm.2013.37.5.735
Salvati M, Missori P, Lunardi P, Orlando ER (1991) Transient cerebellar mutism after posterior cranial fossa surgery in an adult. Case report and review of the literature. Clin Neurol Neurosurg 93:313–316
Sherman JH, Sheehan JP, Elias WJ, Jane JA Sr (2005) Cerebellar mutism in adults after posterior fossa surgery: a report of 2 cases. Surg Neurol 63:476–479. https://doi.org/10.1016/j.surneu.2004.06.015
Strata P (2015) The emotional cerebellum. Cerebellum (London, England) 14:570–577. https://doi.org/10.1007/s12311-015-0649-9
Tellmann S, Bludau S, Eickhoff S, Mohlberg H, Minnerop M, Amunts K (2015) Cytoarchitectonic mapping of the human brain cerebellar nuclei in stereotaxic space and delineation of their co-activation patterns. Front Neuroanat 9:54. https://doi.org/10.3389/fnana.2015.00054
Tomasello F, Conti A, Angileri FF, Cardali S (2015) Telo-velar approach to fourth-ventricle tumours: how I do it. Acta Neurochir 157:607–610. https://doi.org/10.1007/s00701-015-2358-z
Van Calenbergh F, Van de Laar A, Plets C, Goffin J, Casaer P (1995) Transient cerebellar mutism after posterior fossa surgery in children. Neurosurgery 37:894–898
Vassal M, Charroud C, Deverdun J, Le Bars E, Molino F, Bonnetblanc F, Boyer A, Dutta A, Herbet G, Moritz-Gasser S, Bonafe A, Duffau H, de Champfleur NM (2017) Recovery of functional connectivity of the sensorimotor network after surgery for diffuse low-grade gliomas involving the supplementary motor area. J Neurosurg 126:1181–1190. https://doi.org/10.3171/2016.4.jns152484
Vergani F, Lacerda L, Martino J, Attems J, Morris C, Mitchell P, Thiebaut de Schotten M, Dell'Acqua F (2014) White matter connections of the supplementary motor area in humans. J Neurol Neurosurg Psychiatry 85:1377–1385. https://doi.org/10.1136/jnnp-2013-307492
Wells EM, Khademian ZP, Walsh KS, Vezina G, Sposto R, Keating RF, Packer RJ (2010) Postoperative cerebellar mutism syndrome following treatment of medulloblastoma: neuroradiographic features and origin. J Neurosurg Pediatr 5:329–334. https://doi.org/10.3171/2009.11.peds09131
Wibroe M, Rochat P, Juhler M (2017) Cerebellar mutism syndrome and other complications following surgery in the posterior fossa in adults: a prospective study. World Neurosurg 110:e738–e746. https://doi.org/10.1016/j.wneu.2017.11.100
Wilson TW, Slason E, Asherin R, Kronberg E, Reite ML, Teale PD, Rojas DC (2010) An extended motor network generates beta and gamma oscillatory perturbations during development. Brain Cogn 73:75–84. https://doi.org/10.1016/j.bandc.2010.03.001
Wolpe N, Ingram JN, Tsvetanov KA, Geerligs L, Kievit RA, Henson RN, Wolpert DM, Rowe JB (2016) Ageing increases reliance on sensorimotor prediction through structural and functional differences in frontostriatal circuits. Nat Commun 7:13034. https://doi.org/10.1038/ncomms13034
Yildiz O, Kabatas S, Yilmaz C, Altinors N, Agaoglu B (2010) Cerebellar mutism syndrome and its relation to cerebellar cognitive and affective function: review of the literature. Ann Indian Acad Neurol 13:23–27. https://doi.org/10.4103/0972-2327.61272
Zaheer SN, Wood M (2010) Experiences with the telovelar approach to fourth ventricular tumors in children. Pediatr Neurosurg 46:340–343. https://doi.org/10.1159/000321539
Funding
This project was partially funded by Danish Cancer Society (Kræftens Bekæmpelse) and Danish Child Cancer Foundation (Børnecancerfonden).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
The authors declare that they have no conflict of interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Grønbæk, J., Molinari, E., Avula, S. et al. The supplementary motor area syndrome and the cerebellar mutism syndrome: a pathoanatomical relationship?. Childs Nerv Syst 36, 1197–1204 (2020). https://doi.org/10.1007/s00381-019-04202-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-019-04202-3