Abstract
Purpose
Approximately 90% of concussions are transient, with symptoms resolving within 10–14 days. However, a minority of patients remain symptomatic several months post-injury, a condition known as post-concussion syndrome (PCS). The treatment of these patients can be challenging. The goal of our study was to assess the utility and cost-effectiveness of neurologic imaging two or more weeks post-injury in a cohort of youth with PCS.
Methods
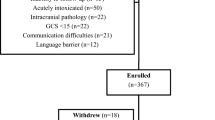
We conducted a retrospective study of 52 pediatric patients with persistent post-concussion symptoms after 3 months. We collected demographics and neuroimaging results obtained greater than 2 weeks post-concussion. Neuroimaging ordered in the first 2 weeks post-concussion was excluded, except to determine the rate of re-imaging. Descriptive statistics and corresponding cost data were collected.
Results
Of 52 patients with PCS, 23/52 (44 %) had neuroimaging at least 2 weeks after the initial injury, for a total of 32 diagnostic studies. In summary, 1/19 MRIs (5.3 %), 1/8 CTs (13 %), and 0/5 x-rays (0 %) yielded significant positive findings, none of which altered clinical management. Chronic phase neuroimaging estimated costs from these 52 pediatric patients totaled $129,025. We estimate the cost to identify a single positive finding was $21,000 for head CT and $104,500 for brain MRI.
Conclusions
In this cohort of pediatric PCS patients, brain imaging in the chronic phase (defined as more than 2 weeks after concussion) was pursued in almost half the study sample, had low diagnostic yield, and had poor cost-effectiveness. Based on these results, outpatient management of pediatric patients with long-term post-concussive symptoms should rarely include repeat neuroimaging beyond the acute phase.
Similar content being viewed by others
References
Choe MC et al (2012) A pediatric perspective on concussion pathophysiology. Curr Opin Pediatr 24(6):689–695. doi:10.1097/MOP.0b013e32835a1a44
McCrea M et al (2013) Incidence, clinical course, and predictors of prolonged recovery time following sport-related concussion in high school and college athletes. J Int Neuropsychol Soc 19(1):22–33
Meehan WP 3rd, d'Hemecourt P, Comstock RD (2010) High school concussions in the 2008–2009 academic year: mechanism, symptoms, and management. Am J Sports Med 38(12):2405–9
Makdissi M et al (2013) The difficult concussion patient: what is the best approach to investigation and management of persistent (>10 days) postconcussive symptoms? Br J Sports Med 47(5):308–13
Lau BC, Collins MW, Lovell MR (2012) Cutoff scores in neurocognitive testing and symptom clusters that predict protracted recovery from concussions in high school athletes. Neurosurgery 70(2):371–9, discussion 379
Ruff RM, Camenzuli L, Mueller J (1996) Miserable minority: emotional risk factors that influence the outcome of a mild traumatic brain injury. Brain Inj 10(8):551–65
American Psychiatric, A., A. American Psychiatric, and D.-I. Task Force on (2000) Diagnostic and statistical manual of mental disorders : DSM-IV-TR. American Psychiatric Association, Washington, DC
Pulsipher DT et al (2011) A critical review of neuroimaging applications in sports concussion. Curr Sports Med Rep 10(1):14–20
Davis GA et al (2009) Contributions of neuroimaging, balance testing, electrophysiology and blood markers to the assessment of sport-related concussion. Br J Sports Med 43(Suppl 1):i36–45
Kuppermann N et al (2009) Identification of children at very low risk of clinically-important brain injuries after head trauma: a prospective cohort study. Lancet 374(9696):1160–70
Osmond MH et al (2010) CATCH: a clinical decision rule for the use of computed tomography in children with minor head injury. CMAJ 182(4):341–8
Morgan C, et al. Predictors of post-concussion syndrome (PCS) after sports-related concussion in young athletes: a matched case–control study. Journal of Neurosurgery: Pediatrics, In Press
Babcock L et al (2013) Inability of S100B to predict postconcussion syndrome in children who present to the emergency department with mild traumatic brain injury: a brief report. Pediatr Emerg Care 29(4):458–61
Babcock L et al (2013) Predicting postconcussion syndrome after mild traumatic brain injury in children and adolescents who present to the emergency department. JAMA Pediatr 167(2):156–61
Heitger MH, Jones RD, Anderson TJ (2008) A new approach to predicting postconcussion syndrome after mild traumatic brain injury based upon eye movement function. Conf Proc IEEE Eng Med Biol Soc 2008:3570–3
Ma M et al (2008) Serum cleaved tau does not predict postconcussion syndrome after mild traumatic brain injury. Am J Emerg Med 26(7):763–8
Preiss-Farzanegan SJ et al (2009) The relationship between gender and postconcussion symptoms after sport-related mild traumatic brain injury. PM R 1(3):245–53
American Psychiatric, A., A. American Psychiatric, and D.S.M.T. Force (2013) Diagnostic and statistical manual of mental disorders : DSM-5., Available from: http://dsm.psychiatryonline.org/book.aspx?bookid=556
Losey-Flores K et al (2014) Free hernia surgery for the underserved is possible in the United States. Hernia 18(2):305–310
Millhiser WP, Veral EA, Valenti BC (2012) Assessing appointment systems’ operational performance with policy targets. IIE Transactions on Healthcare Systems Engineering 2(4):274–289
Riley D (2014) The art of a pediatric exam. Nurse Pract 39(6):50–4
Sannino G, De Falco I, De Pietro G (2013) Automatic extraction of effective rule sets for Obstructive Sleep Apnea detection for a real-time mobile monitoring system. in Information Reuse and Integration (IRI), 2013 I.E. 14th International Conference on
Shetty V et al (2013) The “Shetty test” in ankle injuries: validation of a novel test to rule out ankle fractures. European Journal of Orthopaedic Surgery & Traumatology 23(7):831–833
Trinh L, Ikeda DM, Miyake KK, Trinh J, Lee KK, Dave H, Hanafusa K, Lipson J (2015) Patient awareness of breast density and interest in supplemental screening tests: comparison of an academic facility and a county hospital. J Am Coll Radiol 12(3):249–255
Zamosky L. Cutting Medical Costs, in Healthcare, Insurance, and You. 2013, Apress. p. 75–88
Baker JG et al (2012) Return to full functioning after graded exercise assessment and progressive exercise treatment of postconcussion syndrome. Rehabil Res Pract 2012:705309
Leddy JJ et al (2011) Reliability of a graded exercise test for assessing recovery from concussion. Clin J Sport Med 21(2):89–94
Solomon GS, Sills AK (2013) Pharmacologic treatment of sport-related concussion: a review. J Surg Orthop Adv 22(3):193–7
Reddy CC et al (2013) Efficacy of amantadine treatment on symptoms and neurocognitive performance among adolescents following sports-related concussion. J Head Trauma Rehabil 28(4):260–5
Packard RC (2000) Treatment of chronic daily posttraumatic headache with divalproex sodium. Headache 40(9):736–9
Peterlin BL et al (2008) Post-traumatic stress disorder in episodic and chronic migraine. Headache 48(4):517–22
Weiss HD, Stern BJ, Goldberg J (1991) Post-traumatic migraine: chronic migraine precipitated by minor head or neck trauma. Headache 31(7):451–6
Gonzalez PG, Walker MT (2011) Imaging modalities in mild traumatic brain injury and sports concussion. PM&R 3(10, Supplement 2):S413–S424
Forbes JA et al (2013) Subdural hemorrhage in two high-school football players: post-injury helmet testing. Pediatr Neurosurg 49(1):43–9
Brenner DJ (2002) Estimating cancer risks from pediatric CT: going from the qualitative to the quantitative. Pediatr Radiol 32(4):228–1, discussion 242–4
Brenner DJ, Hall EJ (2007) Computed tomography—an increasing source of radiation exposure. N Engl J Med 357(22):2277–84
Parizel PM et al (2005) New developments in the neuroradiological diagnosis of craniocerebral trauma. Eur Radiol 15(3):569–81
Schrader H et al (2009) Magnetic resonance imaging after most common form of concussion. BMC Med Imaging 9:11
McCrory P et al (2009) Consensus statement on concussion in sport—the 3rd International Conference on concussion in sport held in Zurich, November 2008. J Sci Med Sport 12(3):340–51
Yuh EL, Hawryluk GW, Manley GT (2014) Imaging concussion: a review. Neurosurgery 75(Suppl 4):S50–63
Zuckerman SL (2012) Structural brain injury in sports-related concussion. Neurosurg Focus 33(6):E6, 1–12
Sener RN (1997) Arachnoid cysts associated with post-traumatic and spontaneous rupture into the subdural space. Comput Med Imaging Graph 21(6):341–4
Parsch CS et al (1997) Arachnoid cysts associated with subdural hematomas and hygromas: analysis of 16 cases, long-term follow-up, and review of the literature. Neurosurgery 40(3):483–90
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Support for this study came from an unrestricted educational grant from Rawlings. Dr. Solomon is a consultant for ImPACT, Nashville Predators, and Tennessee Titans. Otherwise, the study authors have no conflicts of interest or financial interests to report.
Rights and permissions
About this article
Cite this article
Morgan, C.D., Zuckerman, S.L., King, L.E. et al. Post-concussion syndrome (PCS) in a youth population: defining the diagnostic value and cost-utility of brain imaging. Childs Nerv Syst 31, 2305–2309 (2015). https://doi.org/10.1007/s00381-015-2916-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-015-2916-y