Abstract
Introduction
Various techniques are used for spinal cord untethering. The purpose of this study was to compare patient characteristics, postoperative course, and early complications after laminotomy vs. laminoplasty for transection of the filum terminale for tethered cord release.
Methods
Retrospective analysis of clinical and magnetic resonance imaging data was undertaken for all patients (<18 years) who underwent tethered cord release by transection of the filum terminale at Oregon Health & Science University, Doernbecher Children’s Hospital, from 2000 to 2011.
Results
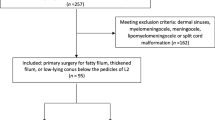
Data from two hundred and forty-eight patients were analyzed. Mean age was 5.2 years (range 0.3 to 16.8 years). Access to the thecal space during surgery was achieved using laminotomy or laminoplasty in 82 (33.1 %) and 166 (66.9 %) patients, respectively. Laminoplasty patients were significantly younger than laminotomy patients (3.2 vs. 9.3 years, p < 0.0001); other clinical and radiographic characteristics were similar between the groups. Nine patients (3.6 %) experienced early complications, including cerebrospinal fluid leak (n = 2), suprafascial infection requiring surgical management and intravenous (IV) antibiotics (n = 3) or IV antibiotics alone (n = 1), a small area of peri-incisional cutaneous necrosis (n = 1), perioperative seizures (n = 1), and mild, transient malignant hyperthermia (n = 1). There was no difference in the number of early complications between the two groups. Univariate and multivariate analyses revealed no significant risk factor for postoperative complication associated with technique. As judged by caregivers, independent of surgical technique, 97 % of patients improved after surgery.
Conclusion
There was no difference in complication risk when performing transection of the filum terminale for tethered cord release using laminotomy or laminoplasty.

Similar content being viewed by others
References
Hertzler DA, DePowell JJ, Stevenson CB, Mangano FT (2010) Tethered cord syndrome: a review of the literature from embryology to adult presentation. Neurosurg Focus 29(1):E1. doi:10.3171/2010.3.FOCUS1079
Barson A (1970) The vertebral level of termination of the spinal cord during normal and abnormal development. J Anat 106:489–497
Hoffman H, Hendrick E, Humphreys R (1976) The tethered spinal cord: its protean manifestations, diagnosis and surgical correction. Childs Brain 2(3):145–155
Khoury A, Hendrick E, McLorie G, Kulkarni A, Churchill B (1990) Occult spinal dysraphism: clinical and urodynamic outcome after division of the filum terminale. J Urol 144:426–428
Selden NR (2006) Occult tethered cord syndrome: the case for surgery. J Neurosurg 104(5):302–304. doi:10.3171/ped.2006.104.5.302
Selden NR, Nixon RR, Skoog SR, Lashley DB (2006) Minimal tethered cord syndrome associated with thickening of the terminal filum. J Neurosurg 105(3):214–218. doi:10.3171/ped.2006.105.3.214
Wehby M, O'Hollaren P, Abtin K, Hume J, Richards B (2004) Occult tight filum terminale syndrome: results of surgical untethering. Pediatr Neurosurg 40(2):51–58
Chern JJ, Tubbs RS, Patel AJ, Gordon AS, Bandt SK, Smyth MD, Jea A, Oakes WJ (2011) Preventing cerebrospinal fluid leak following transection of a tight filum terminale. J Neurosurg 8(1):35–38. doi:10.3171/2011.4.PEDS10502
Nazar G, Casale A, Roberts J, Linden R (1995) Occult filum terminale syndrome. Pediatr Neurosurg 23(5):228–235
La Marca F, Grant J, Tomita T, McLone D (1997) Spinal lipomas in children: outcome of 270 procedures. Pediatr Neurosurg 26(1):8–16
Thompson EM, Strong MJ, Warren G, Woltjer RL, Selden NR (2014) Clinical significance of imaging and histological characteristics of filum terminale in tethered cord syndrome. J Neurosurg Pediat Ahead Print (0):1–5. doi:10.3171/2013.12.PEDS13370
Kesler H, Dias MS, Kalapos P (2007) Termination of the normal conus medullaris in children: a whole-spine magnetic resonance imaging study. Neurosurg Focus 23(2):1–5. doi:10.3171/FOC-07/08/E7
Mourgela S, Anagnostopoulou S, Sakellaropoulos A, Koulousakis A, Warnke J (2008) Sectioning of filum terminale externum using a rigid endoscope through the sacral hiatus. Cadaver study. J Neurosurg Sci 52(3):71–74
Pierre-Kahn A, Zerah M, Renier D, Cinalli G, Sainte-Rose C, Lellouch-Tubiana A, Brunelle F, Merrer ML, Giudicelli Y, Pichon J, Kleinknecht B, Fo N (1997) Congenital lumbosacral lipomas. Child Nerv Syst 13(6):298–334. doi:10.1007/s003810050090
Colak A, Pollack I, Albright A (1998) Recurrent tethering: a common long-term problem after lipomyelomeningocele repair. Pediatr Neurosurg 29(4):184–190
Herman J, McLone D, Storrs B, Dauser R (1993) Analysis of 153 patients with myelomeningocele or spinal lipoma reoperated upon for a tethered cord. Presentation, management and outcome. Pediatr Neurosurg 19(5):243–249
Yong RL, Habrock-Bach T, Vaughan M, Kestle JR, Steinbok P (2011) Symptomatic retethering of the spinal cord after section of a tight filum terminale. Neurosurgery 68(6):1594–1602
Acknowledgments
The authors would like to thank Shirley McCartney, Ph.D., for the editing assistance and Andy Rekito, M.S., for the medical illustration and figure preparation. This research was supported by the Oregon Health & Science University Campagna Scholarship to MJS. MJS is currently supported by the Ruth L. Kirschstein National Research Service Award (F30 CA177267-02) from the National Cancer Institute.
Conflict of interest
The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. A distinct but largely overlapping population of pediatric and adult patients was analyzed and reported separately in a manuscript focusing on the histopathology of filum terminale specimens in tethered cord release [11].
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Strong, M.J., Thompson, E.M., Roundy, N. et al. Use of lumbar laminoplasty vs. laminotomy for transection of the filum terminale does not affect early complication rates or postoperative course. Childs Nerv Syst 31, 597–601 (2015). https://doi.org/10.1007/s00381-015-2615-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-015-2615-8