Abstract
Rationale
Predicting length of stay in the intensive care unit (ICU) in children with Guillain–Barre syndrome may help decision-making at admission.
Materials and methods
Between 1996 and 2003, we attended to 30 children with Guillain–Barre syndrome who required ventilatory support in ICU. We prospectively collected different variables that could potentially predict prolonged length of stay and ventilatory support in ICU.
Conclusion
Using Cox proportional hazard analysis we found that lack of electrical excitability was the best predictor.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Twenty percent of children with Guillain–Barre syndrome (GBS) require ventilatory support for periods that range between 1 week and 6 months. The number of days with ventilatory support has been associated with long-term functional prognosis [1], and several clinical and laboratory variables at disease onset have shown association with length of ventilatory support [2–5]. However, we did not find studies analyzing electrophysiological evaluation and duration of ventilatory support.
Predicting duration of ventilatory support is useful not only to reassure children and their parents, but also to select the appropriate ventilator, to program tracheostomy and gastrostomy, or perhaps to plan referral to a higher-level institution.
The objective of our study was to determine which electrophysiological variables at admission could predict duration of ventilatory support.
Materials and methods
Study design: This is a prospective, descriptive, case-series study.
Study sample: We included every child with GBS, according to Asbury’s diagnostic criteria [6], admitted to our intensive care unit (ICU) requiring ventilatory support.
Predictive variables considered:
-
1.
Age and gender
-
2.
Muscular strength at day 10 of disease initiation
-
3.
Presence of dysautonomia
-
4.
Cranial nerve impairment
-
5.
Electrophysiological pattern
We prospectively collected demographic variables and, on day 10, the muscular strength of biceps, digital flexors, quadriceps, and ankle dorsiflexors, according to the Medical Research Council as well as the presence of dysautonomia or cranial nerve involvement. We counted the days of ventilatory support starting at intubation and ending when no further ventilatory support of any kind was required. All patients received similar treatment (human immune globulin). None received plasmapheresis.
Electrophysiological studies
One of us (FOC) performed all the EMG evaluations using Viking IIe equipment. All of them were performed at the ICU between days 5 and 10 of disease initiation. We used conventional techniques to assess median (unilateral), ulnar (unilateral), tibial (bilateral), and sural nerves (bilateral). We used Ho’s criteria [7] for a physiopathological classification of GBS subtype (Table 1).
Electric inexcitability: Patients whose nerve conduction studies showed absent motor responses were classified as inexcitable (complete absence of motor nerve excitation in the four nerves). An electric impulse of 100 mA and 1 ms of duration was used in all cases with a gain in the monitor from 5 mV to 200 μV/division.
For group comparisons, we used non-parametric tests (Mann–Whitney) to detect association between the length of ventilatory support and different risk factors, as well as Cox proportional hazards and Kaplan–Meier survival analysis.
Results
Between 1996 and 2003, 30 children diagnosed as GBS were admitted at our ICU requiring ventilatory support.
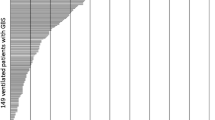
The ages of our 30 patients ranged between 1.5 and 16 years (average=7.3, median=6.2); 16 were male. Average duration of ventilatory support was 29.8 days (range 1–98; median=26), and was longer in patients with facial paresis (n=21; 34.1 vs 19.7 days; p=0.63), in patients with dysautonomia (n=22; 34.0 vs 18.2 days; p=0.045) and in those with quadriplegia (n=16; 36.6 vs 22.1 days; p=0.058).
According to EMG findings, we divided our patients in two groups: those with the classic GBS patterns (demyelinating form and acute motor axonal neuropathy variant; n=16) and those with complete absence of motor nerve excitation (n=14). There was a highly significant difference in the duration of ventilatory support between them (p=0.003): 18.3±4.6 days (average±SD) for the first group compared with 43.0±11.3 days for the latter. The median duration was 16 and 39 days, respectively. Figure 1 shows the Kaplan–Meier survival curves of these two groups.
When we included quadriplegia and dysautonomia in the Cox regression analysis, lack of electrical excitability remained as the most significant risk factor [p=0.007; exp (B)=4.9; IC 95%=1.5–15.6], while quadriplegia and dysautonomia decreased their statistical significance level (p=0.2 and p=0.8, respectively).
Discussion
Our study has several important limitations. Criteria for initiating or suspending ventilatory support differ between specialists [9], as does the type of support provided [13, 14], or indications for tracheostomy [15]. These factors could influence un-blinded decisions and, therefore, modify our main outcome.
Despite this limitation, we consider that duration of ventilatory support in patients with GBS is a practical and clinically relevant indicator of disease severity. Most studies (for example, [8]) have looked at clinical variables, like cranial nerve involvement or severity of motor deficit, that could be associated with ventilatory support.
In their paper on tracheostomy and GBS [8], Lawn and Wijdicks divide their patients in those that require less or more than 21 days of ventilatory support. They conclude, as did Henderson et al. [9], that age (older patients) and history of pulmonary disease are risk factors for prolonged ventilatory support [8, 9]. Few of their patients, however, were children.
Quadriplegia, at the peak of the disease and a prolonged plateau, has been associated with delayed motor recovery, but the relationship with prolonged ventilatory support is not so clear. In our study, bivariate analysis showed that quadriplegia at day 10, as well as dysautonomia, were associated with longer requirements of ventilatory support (despite the lack of statistical significance of the former, perhaps attributable to the relatively small sample size). But the strength of the association of these two variables was reduced when electrical excitability of motor nerves was considered.
Several studies have established that a decrease in amplitude of compound muscle action potentials is associated with a bad prognosis and a longer recovery up to Hughes functional stage III [10]. Other authors have found that lack of electrical excitability of motor nerves is associated with a poor functional prognosis [1]. The relationship between electrophysiologic findings and clinical outcomes in the ICU have been addressed toward predicting the need more than the duration of ventilatory support [11].
Furthermore, most researches on GBS come from developing countries where the demyelinating form predominates. In our study, we found both demyelinating and acute motor axonal neuropathy variants, but found no statistical difference in the duration of ventilatory support between them. On the other hand, patients with lack of electrical excitability of motor nerves had a different clinical progression, with a need for longer ventilatory support. Whether this lack of electrical excitability of motor nerves is a severe form of acute motor axonal neuropathy cannot be proved with electrophysiological methods alone. Some studies have shown through histopathology that this EMG response can also be found in severe demyelinating polyneuropathies [12].
We conclude that both clinical and electrophysiological variables provide useful information with regards to ventilatory support duration both for the patient and for the caregivers. EMG findings, particularly, can help decision-making in the ICU.
References
Fletcher DD, Lawn ND, Wolter TD, Wijdicks EF (2000) Long-term outcome in patients with Guillain–Barre syndrome requiring mechanical ventilation. Neurology 54:2311–2315
Kaida K, Kusunoki S, Kanzaki M, Kamakura K, Motoyoshi K, Kanazawa I (2004) Anti-GQ1b antibody as a factor predictive of mechanical ventilation in Guillain–Barre syndrome. Neurology 62:821–824
Sharshar T, Chevret S, Bourdain F, Raphael JC (2003) French cooperative group on plasma exchange in Guillain–Barre syndrome. Early predictors of mechanical ventilation in Guillain–Barre syndrome. Crit Care Med 31:278–283
Lawn ND, Fletcher DD, Henderson RD, Wolter TD, Wijdicks EF (2001) Anticipating mechanical ventilation in Guillain–Barre syndrome. Arch Neurol 58:893–898
Rantala H, Uhari M, Cherry JD, Shields WD (1995) Risk factors of respiratory failure in children with Guillain–Barre syndrome. Pediatr Neurol 13:289–292
Asbury AK, Cornblath DR (1990) Assessment of current diagnostic criteria for Guillain–Barre syndrome. Ann Neurol 27(Suppl):S21–S24
Ho TW, Cornblath DR, Gao CY, Asbury AK, Griffin JW, McKhann GM (1997) Patters of recovery in the Guillain–Barré syndromes. Neurology 48:695–700
Lawn ND, Wijdicks EF (1999), Tracheostomy in Guillain–Barre syndrome. Muscle Nerve 22:1058–1062
Henderson RD, Lawn ND, Fletcher DD, McClelland RL, Wijdicks EFM (2003) The morbidity of Guillain–Barre syndrome admitted to the intensive care unit. Neurology 60:17–21
Cornblath DR, Mellits ED, Griffin JW (1988) Motor conduction studies in Guillain–Barre syndrome: description and prognostic value. Ann Neurol 23:354–359
Durand MC, Lofaso F, Lefaucheur JP, Chevret S, Gajdos P, Raphael JC et al (2003) Electrophysiology to predict mechanical ventilation in Guillain–Barre syndrome. Eur J Neurol 10:39–44
Massaro ME, Rodriguez EC, Pociecha J, Arroyo HA, Sacolitti M, Taratuto AL (1998) Nerve biopsy in children with severe Guillain–Barre syndrome and inexcitable motor nerves. Neurology 51:394–398
Borel CO, Guy J (1995) Ventilatory management in critical neurologic illness. Neurol Clin 13:627–644
Chevrolet JC, Deleamont P (1991) Repeated vital capacity measurements as predictive parameters for mechanical ventilation need and weaning success in the Guillain–Barré syndrome. Am Rev Respir Dis 144:814–818
Plummer AL, Gracey DR (1989) Consensus conference on artificial airways in patients receiving mechanical ventilation. Chest 96:178–180
Acknowledgement
We thank Diego Rosselli, M.D. for his editorial assistance.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ortiz-Corredor, F., Díaz-Ruiz, J. & Izquierdo-Bello, A. EMG and duration of ventilatory support in children with Guillain–Barre syndrome. Childs Nerv Syst 22, 1328–1331 (2006). https://doi.org/10.1007/s00381-006-0092-9
Received:
Revised:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00381-006-0092-9