Abstract
Comparative data are virtually missing about the performance of different electro-anatomical mapping (EAM) system platforms on outflow tract (OT) premature ventricular complex (PVC) ablation outcomes with manual ablation catheters. We aimed to compare the acute success-, complication-, and long-term recurrence rates of impedance-based (IMP) and magnetic field-based (MAG) EAM platforms in manual OT PVC ablation. Single-centre, propensity score matched data of 39–39 patients ablated for OT PVCs in 2015–17 with IMP or MAG platforms were analysed. Acute success rate, peri-procedural complications, post-ablation daily PVC burden, and long-term recurrence rates were compared on intention-to-treat basis. Acute success rate was similar in the IMP and MAG group (77 vs. 82%, p = 0.78). There was a single case of femoral pseudo-aneurysm and no cardiac tamponade occurred. PVC burden fell significantly from baseline 24.0% [15.0–30.0%] to 3.3% [0.25–10.5%] (p < 0.001) post-ablation, with no difference between EAM platforms (IMP: 2.6% [0.5–12.0%] vs. MAG: 4.0% [2.0–6.5%]; p = 0.60). There was no significant difference in recurrence-free survival of the intention-to-treat cohort of the IMP and MAG groups (54 vs. 60%, p = 0.82, respectively) during 12 months of follow-up. Ablation with the aid of both impedance- and magnetic field-based EAM platforms can considerably reduce OT PVC burden and give similar acute- and long-term freedom from arrhythmia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The right- (RVOT) and left ventricular outflow tracts (LVOT) are the regions where the majority of idiopathic ventricular arrhythmias arise with premature ventricular complexes (PVC) being the most frequent of them. Other sources of outflow tract (OT) PVCs include the sinuses of the aortic valve, the pulmonary trunk, and the epicardial aspect of the OT area. While OT PVCs are overwhelmingly benign in prognosis, they can cause palpitations, pounding, and a feeling of skipped beats that could lead to significant discomfort and reduced quality of life. Moreover, Penela et al. [1] reported that a high daily PVC burden can decrease left ventricular ejection fraction (LVEF) leading to PVC-induced cardiomyopathy. Zhong et al. [2] demonstrated in their retrospective study that PVC ablation significantly reduced arrhythmia burden and improved LVEF compared with antiarrhythmic drug therapy only. Radiofrequency catheter ablation has become a feasible and efficient treatment recommended by the 2015 ESC Guidelines of ventricular arrhythmia management [3]. Long-term success of ablation not only can reverse the decline in LVEF but can also improve clinical prognosis of PVC-induced cardiomyopathy by reducing the composite of mortality, indication for heart transplant, and hospitalisation as it was proven in the landmark prospective multicentre trial by Berruezzo et al. [4].
The acute procedural success rate of OT PVC ablation is around 80–90% but long-term recurrence rates are variable in the literature, even reaching 52% in RVOT cases with a mean time to recurrence of 6.3 years according to Ventura et al. [5].
Unlike in atrial fibrillation ablation [6], the use of manual contact force sensing (CFS) catheters in OT PVC ablation does not seem to outperform traditional manual ablation catheters in reducing PVC recurrence as it has been independently pointed out by a recent retrospective multicentre study of Reichlin et al. [7] and by Ábrahám et al. [8] in a propensity-matched retrospective cohort. An explanation could be that ablation in the OT region is rather focal and activation-based in an anatomically quite variable region and it is not a matter of creating a homogenous, anatomically driven lesion set, such as in atrial fibrillation ablation. Therefore, the performance of the electro-anatomical mapping (EAM) system could theoretically influence ablation success, as well. The most widespread 3-dimensional EAM platforms are magnetic field-based (MAG) and impedance-based (IMP) in their fundamental design. There is virtually no data available on the performance and clinical outcome of different EAM systems in manual OT PVC ablation. Outcomes with the two EAM systems were only compared in remote magnetic navigation (RMN) environment by Dang et al. [9], notably with neutral results.
We aimed to compare the change in PVC burden, acute success rates, and 12 month follow-up results of MAG- and IMP-guided manual endocardial ablation on an intention-to-treat basis in a balanced patient population treated exclusively for OT PVCs.
Methods
Patients
We analysed observational data of a single-centre, retrospective cohort of 177 consecutive adult patients who underwent their first OT PVC ablation between 2015 and 2017 in our centre. Patients with symptoms characteristic for PVC with a high (> 15%) daily arrhythmia burden refractory to medical therapy or patients refusing to take antiarrhythmic drugs were included. Data of 177 patients underwent propensity score matching to create balanced cohorts. Informed consent was obtained from patients prior to inclusion to the study. Antiarrhythmic medication was discontinued 48 h before ablation. For lateralisation of the source of origin the V2S/V3R amplitude ratio of the OT PVC beats measured on the 12-lead ECG was used as described by Yoshida et al. [10]. The study protocol was reviewed and approved by the Institutional Review Board and was in accordance with the Declarations of Helsinki.
Procedure and follow-up
Procedures were performed under local anaesthesia using a femoral venous and/or arterial vascular access. There was neither a transseptal approach for left-sided ablation nor a direct subxyphoid access for epicardial ablation. Three-dimensional EAM was performed in all patients to map the earliest endocardial activation of OT PVC and to guide ablation using either a MAG system: CARTO 3® (Biosense Webster Inc., Diamond Bar, CA, USA) or an IMP platform: EnSite NavX® (Abbott Inc., Abbott Park, IL, USA). Although the latter platform has been upgraded to a hybrid IMP + MAG system, called EnSite Precision® since 2016 only cases without magnetic sensor-enabled ablation catheters were selected from 2016 to 17 for data consistency purposes of the IMP group. Only contact mapping was used.
Activation mapping identified sites for ablation with earliest local activation advancing the onset of PVC QRS by at least 30 ms. During traditional pace-mapping, a site with a minimum match of 11/12 was considered a target to energy delivery. Automated morphology matching programs, PASO® (Biosense Webster Inc., Diamond Bar, CA, USA) and ScoreMap® (Abbott Inc., Abbott Park, IL, USA) were also used when they became available on the relevant platform. When spontaneous, clinically relevant PVCs were absent during the procedure isoproterenol was used in 10 µg boluses for induction of the arrhythmia. Commercially available 3.5 mm open-irrigated tip radiofrequency catheters were used for mapping and ablation with or without CFS capabilities. Radiofrequency energy was delivered in 60 s duration impulses with an energy setting of 30–40 W, in power-controlled mode with a temperature limit of 43 °C. The definition of acute procedural success was complete abolition of the clinical PVC during the post-ablation waiting period after isoproterenol challenge. Arrhythmia recurrence during follow-up was defined as a > 5% daily PVC burden on a 24 h Holter-ECG. Visits and Holter-ECGs were performed at 3 months post-ablation, and then every 6 months on, or in between these periods when symptoms recurred. Left-sided ablations included PVCs originating from the LVOT region or from the left- and right sinuses of Valsalva.
Statistical analysis
Variables included in the logistic regression model for propensity score matching were age, sex, hypertension, use of CFS catheters, and left-sided ablations. A 1:1 ratio and nearest neighbour method was used by the algorithm to create a propensity-matched cohort. A value of 0.1 was set for maximum allowed difference in matching. Continuous variables were expressed as median and interquartile ranges [25–75% IQR], whereas categorical ones in numbers and %. We compared dichotomous variables with Fisher’s exact test. Continuous variables with normal distribution were compared using t test, or by Mann–Whitney U test for the variables with non-normal distribution. We assessed normality of distribution with a Shapiro–Wilk test. Recurrence-free survival was computed by the Kaplan–Meier method and differences in recurrence rates were compared with log-rank test. We evaluated recurrence-free survival rates on an intention-to-treat basis between the MAG and IMP group, hence not only acutely successful cases were included in the analysis. We accepted a two-tailed p value of < 0.05 as statistically significant. We used SPSS Statistics 27 (IBM Corp., Armonk, NY, USA) software for calculations.
Results
Baseline characteristics
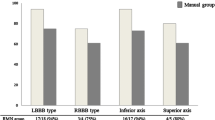
Out of the 177 OT PVC patients (41 IMP and 136 MAG cases) propensity matching algorithm created a group of 78 paired cases and in 99 cases matching was ineffective. 39 patients underwent IMP-guided manual ablation and 39 matched patients had a procedure with MAG guidance. The IMP and MAG groups created by matching were balanced and there was no significant difference in baseline clinical variables (Table 1). The median age of patients was 53 [42–66] years, 45 (58%) of them being female. Median LVEF was 55% [45–60%], and 36% of the cohort had a reduced (< 50%) LVEF, with no significant difference in their distribution between the two EAM groups (p = 0.06). The site of origin was equally represented with 39–39 (50–50%) cases localised to the RVOT and LVOT. There was no significant difference in baseline antiarrhythmic medication with beta-blockers being the most frequent in 43 (55%) patients (Table 2). All procedural parameters showed insignificant differences (Table 3). Median procedure time was 65 [55–80] min. A contralateral ablation approach, when the successful ablation site of the clinical PVC was finally in the opposite OT to the initial approach indicated by surface ECG, was needed in 27% of the cases, with no significant difference between groups (p = 0.31). We used pace-mapping in 58 cases (74%) and their distribution between the MAG and IMP groups did not show significant difference (p = 0.19) as shown in Table 3. There was no difference in median baseline PVC burden between groups whether pace-mapping was performed or not (25 vs. 26%, p = 0.81).
Acute success
Acute success rates were not statistically different between the MAG and IMP groups with 32 (82%) and 30 (77%) cases (p = 0.78), respectively (Table 3).
Clinical follow-up
During the follow-up time of 12 months, 4 patients (5%) were lost to follow-up. These patients were reported being alive on telephone interview, but declined to take part in follow-up visits, therefore, they were excluded from the analysis of recurrence. The 24 h PVC burden plunged significantly from a baseline median value of 24.0% [15.0–30.0%] to 3.3% [0.25–10.5%], p < 0.001. The magnitude of reduction was similar in the MAG (from 25.0% [15.0–30.0%] to 4.0% [2.0–6.5%]; p < 0.01) and in the IMP group (from 20.0% [15.0–30.0%] to 2.6% [0.5–12.0%]; p < 0.001) without a significant between-group difference (p = 0.60), as one can see on Fig. 1.
Including all but lost patients into the analysis on an intention-to-treat basis there was no significant difference in recurrence-free survival rates between the MAG (60%) and IMP (54%) groups (log-rank p = 0.82) over 12 months of follow-up, as depicted on Fig. 2.
Complications
Access-site complications included two (2.6%) groin haematomas and one (1.3%) pseudo-aneurysm, the latter requiring surgical closure and transfusion (Table 3). No patient developed cardiac tamponade just a hemodynamically insignificant pericardial effusion occurred in a single case post-ablation. There was no procedure-related death.
Discussion
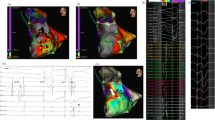
Precise electro-anatomical activation mapping is fundamental in targeting foci with earliest activation and in achieving a durable success after OT PVC ablation. Spatial resolution and accuracy of mapping has already been validated both in MAG- and IMP-based platforms by using a phantom model by Bourier et al. [11]. They found that the 3D localisation offset of mapped points against the phantom-based reality with CT-scan segmentation was 1.62 ± 0.77 mm in CARTO3® and 2.02 ± 1.21 mm in EnSite®, the difference being clinically irrelevant.
The performance of MAG and IMP platforms in OT PVC ablation was only tested in RMN environment, but not with traditional manual ablation catheters. Dang et al. [9] pointed it out in their 43 patients that there was no difference in procedural parameters including ablation duration and X-ray exposure between EnSite Precision® and CARTO3® systems used with magnetic navigation. Long-term success rates were also comparable (86.4% vs. 81.0%, p = 0.631) during their 16.2 ± 6.2 months of follow-up. Our novel results in OT PVC ablation with manual catheters are in accordance with their findings. Procedural parameters, the magnitude of decline in PVC burden, and 12 month follow-up results did not show any significant difference between the MAG and IMP groups in our propensity-matched cohort of 78 patients. It is worth mentioning that we had a balanced proportion of left- and right sided ablation targets and the use of CFS catheters was also represented proportionally in both groups.
Mapping in the OT region could be quite a challenge, therefore, more and more sophisticated features were developed and integrated into 3D EAM systems in the last decade.
High-density mapping features like Confidense® in MAG (launched in June 2015) and EnSite Precision® in IMP system (launched in January 2016) create much more detailed anatomical voltage- and activation maps with a high level of automation. In the case of rarely occurring PVCs, pace-mapping can help target the focus albeit with less spatial accuracy than activation mapping [12]. Development of the MAG platform in pace-mapping resulted in the PASO module to better quantify surface ECG QRS morphology match in 2013. ScoreMap has been serving the same purpose in the IMP platform since 2016. Year 2015 was dominated in PVC ablation in our centre by the MAG platform in this propensity-matched cohort with 84%, and our practice remarkably shifted towards the IMP platform from 2016. As much as 74% and 88% of the cases in 2016 and 2017 were performed by IMP-based mapping.
Complications
Procedure-related complications were infrequent as they occurred in four cases (5%) in our cohort and only one patient (1.3%) had a major complication that required surgical intervention at the femoral access site and transfusion. Complication rates were not statistically different regarding EAM platforms, as shown in Table 3. De Vires et al. [13] reported a 10% overall and 3% major complication rate in their 73 patients treated with catheter ablation for outflow tract arrhythmias.
Limitations
A major limitation of this work lies in its non-randomized nature that might give chance to an unmeasured confounder. Nevertheless, the balanced proportion of 11 baseline clinical variables and 8 procedural parameters, and the similar pattern of antiarrhythmic drug use probably could reduce this chance to a minimum. It is important to emphasize that our sample size was quite small to arrive to any solid conclusion regarding complications when comparing manual MAG and IMP-guided ablation in the OT region.
Since the introduction of EnSite Precision® a hybrid 3D EAM system has been operating in this platform, where the incorporation of a magnetic sensor further enhanced mapping precision. Therefore, one cannot label this novel hybrid mapping platform as purely IMP based. On the other hand, we deliberately selected cases without sensor-enabled ablation catheters to the IMP group to keep this group purely IMP-based in mapping. As a consequence, the full functionality of the hybrid Precision® module cannot be assessed in this work.
By the time those ablations were performed there had not been other EAM platforms available than CARTO 3® (Biosense Webster Inc., Diamond Bar, CA, USA) and EnSite® (Abbott Inc. Abbott Park, IL, USA) in our institution. Because RHYTHMIA® (Boston Scientific Inc., Marlborough, MA, USA) was installed later in our lab, our comparative work could not cover the full spectrum of commercially available high-resolution mapping solutions.
We did not use non-contact mapping at all, therefore, our ablation results with sparsely occurring PVCs might have been affected by this fact.
Conclusions
To the best of our knowledge, this is the first work that directly compares clinical outcomes of the most widespread MAG and IMP EAM platform-based catheter ablation techniques in OT PVC ablation. In our propensity-matched population of 78 patients, there was no difference in OT PVC ablation outcomes regardless of the mapping platform used. What makes the value of our work is the balanced inclusion of patients with homogenous baseline characteristics between the MAG and IMP group. Most noteworthy, the representation of right- and left-sided cases was also equal.
References
Penela D, Fernández-Armenta J, Aguinaga L, Tercedor L, Ordoñez A, Bisbal F, Acosta J, Rossi L, Borras R, Doltra A, Ortiz-Pérez JT, Bosch X, Perea RJ, Prat-González S, Soto-Iglesias D, Tolosana JM, Vassanelli F, Cabrera M, Linhart M, Martinez M, Mont L, Berruezo A (2017) Clinical recognition of pure premature ventricular complex-induced cardiomyopathy at presentation. Heart Rhythm 14(12):1864–1870
Zhong L, Lee YH, Huang XM, Asirvatham SJ, Shen WK, Friedman PA, Hodge DO, Slusser JP, Song ZY, Packer DL, Cha YM (2014) Relative efficacy of catheter ablation vs antiarrhythmic drugs in treating premature ventricular contractions: a single-center retrospective study. Heart Rhythm 11(2):187–193
Priori SG, Blomström-Lundqvist C, Mazzanti A, Blom N, Borggrefe M, Camm J, Elliott PM, Fitzsimons D, Hatala R, Hindricks G, Kirchhof P, Kjeldsen K, Kuck KH, Hernandez-Madrid A, Nikolaou N, Norekvål TM, Spaulding C, Van Veldhuisen DJ (2015) ESC scientific document group. 2015 ESC guidelines for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death: the task force for the management of patients with ventricular arrhythmias and the prevention of sudden cardiac death of the European society of cardiology (ESC). Endorsed by: association for European paediatric and congenital cardiology (AEPC). Eur Heart J 36(41):2793–2867
Berruezo A, Penela D, Jáuregui B, Soto-Iglesias D, Aguinaga L, Ordóñez A, Fernández-Armenta J, Martínez M, Tercedor L, Bisbal F, Acosta J, Martí-Almor J, Aceña M, Anguera I, Rossi L, Linhart M, Borràs R, Doltra A, Sánchez P, Ortiz-Pérez JT, Perea RJ, Prat-González S, Teres C, Bosch X (2019) Mortality and morbidity reduction after frequent premature ventricular complexes ablation in patients with left ventricular systolic dysfunction. Europace 21(7):1079–1087
Ventura R, Steven D, Klemm HU, Lutomsky B, Müllerleile K, Rostock T, Servatius H, Risius T, Meinertz T, Kuck KH, Willems S (2007) Decennial follow-up in patients with recurrent tachycardia originating from the right ventricular outflow tract: electrophysiologic characteristics and response to treatment. Eur Heart J 28(19):2338–2345
Afzal MR, Chatta J, Samanta A, Waheed S, Mahmoudi M, Vukas R, Gunda S, Reddy M, Dawn B, Lakkireddy D (2015) Use of contact force sensing technology during radiofrequency ablation reduces recurrence of atrial fibrillation: a systematic review and meta-analysis. Heart Rhythm 12(9):1990–1996
Reichlin T, Baldinger SH, Pruvot E, Bisch L, Ammann P, Altmann D, Berte B, Kobza R, Haegeli L, Schlatzer C, Mueller A, Namdar M, Shah D, Burri H, Conte G, Auricchio A, Knecht S, Osswald S, Asatryan B, Seiler J, Roten L, Kühne M, Sticherling C (2021) Impact of contact force sensing technology on outcome of catheter ablation of idiopathic pre-mature ventricular contractions originating from the outflow tracts. Europace 23(4):603–609
Ábrahám P, Ambrus M, Herczeg S, Szegedi N, Nagy KV, Salló Z, Osztheimer I, Széplaki G, Tahin T, Merkely B, Gellér L (2021) Similar outcomes with manual contact force ablation catheters and traditional catheters in the treatment of outflow tract premature ventricular complexes. Europace 23(4):596–602
Dang S, Jons C, Jacobsen PK, Pehrson S, Chen X (2019) Feasibility of a novel mapping system combined with remote magnetic navigation for catheter ablation of premature ventricular contractions. J Arrhythm 35(2):244–251
Yoshida N, Yamada T, McElderry HT, Inden Y, Shimano M, Murohara T, Kumar V, Doppalapudi H, Plumb VJ, Kay GN (2014) A novel electrocardiographic criterion for differentiating a left from right ventricular outflow tract tachycardia origin: the V2S/V3R index. J Cardiovasc Electrophysiol 25(7):747–753
Bourier F, Fahrig R, Wang P, Santangeli P, Kurzidim K, Strobel N, Moore T, Hinkel C, Al-Ahmad A (2014) Accuracy assessment of catheter guidance technology in electrophysiology procedures: a comparison of a new 3D-based fluoroscopy navigation system to current electroanatomic mapping systems. J Cardiovasc Electrophysiol 25(1):74–83
Bogun F, Taj M, Ting M, Kim HM, Reich S, Good E, Jongnarangsin K, Chugh A, Pelosi F, Oral H, Morady F (2008) Spatial resolution of pace mapping of idiopathic ventricular tachycardia/ectopy originating in the right ventricular outflow tract. Heart Rhythm 5(3):339–344
de Vries LJ, Hendriks AA, Yap SC, Theuns DAMJ, van Domburg RT, Szili-Torok T (2018) Procedural and long-term outcome after catheter ablation of idiopathic outflow tract ventricular arrhythmias: comparing manual, contact force, and magnetic navigated ablation. Europace 20(suppl_2):ii22–ii27
Acknowledgements
Authors express their sincere gratitude to Tünde Bettenbuch, Marianna Srej, Dániel Kira, Károly Ladunga, Dávid Tasnádi and József Nagy for their continuous and unconditional help in realising the project.
Funding
Open access funding provided by Semmelweis University. Project no. NVKP_16-1–2016–0017 (‘National Heart Program’) has been implemented with the support provided from the National Research, Development and Innovation Fund of Hungary, financed under the NVKP_16 funding scheme. The research was financed by the Thematic Excellence Programme (2020–4.1.1.-TKP2020) of the Ministry for Innovation and Technology in Hungary, within the framework of the Therapeutic Development and Bioimaging thematic programmes of the Semmelweis University.
Author information
Authors and Affiliations
Contributions
PA, MA and LG designed the study. MA and AP collected data. Statistical analysis and drafting of the article was performed by PA and MA. All authors critically reviewed the manuscript and commented on it. All authors have responsibly read and accepted the manuscript in its final form.
Corresponding author
Ethics declarations
Conflict of interest
GS reports personal fees from Abbott, Bayer and Johnson and Johnson Medical outside the submitted work. All other authors have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Ábrahám, P., Ambrus, M., Herczeg, S. et al. Selection of an impedance- or magnetic field-based electro-anatomical mapping platform does not affect outcomes of outflow tract premature ventricular complex manual ablation. Heart Vessels 37, 1769–1775 (2022). https://doi.org/10.1007/s00380-022-02081-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00380-022-02081-4