Abstract
Objectives
To evaluate the performance of extreme gradient boosting (XGBoost) combined with multiparameters from dual-energy computed tomography (mpDECT) to differentiate between multiple myeloma (MM) of the spine and vertebral osteolytic metastases (VOM).
Methods
For this retrospective study, 28 patients (83 lesions) with MM of the spine and 23 patients (54 lesions) with VOM who underwent DECT were included. The mpDECT for each lesion, including normalized effective atomic number, slope of the spectral Hounsfield unit curve, CT attenuation, and virtual noncalcium (VNCa), was obtained. Boruta was used to select the key parameters, and then subsequently merged with XGBoost to yield a prediction model. The lesions were divided into the training and testing group in a 3:1 ratio. The highest performance of the univariate analysis was compared with XGBoost using the Delong test.
Results
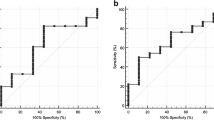
The mpDECT of MM was significantly lower than that of VOM (all p < 0.05). In univariate analysis, VNCa had the highest area under the receiver operating characteristic curve (AUC) in the training group (0.81) and testing group (0.87). Based on Boruta, 6 parameters of DECT were selected for XGBoost model construction. The XGBoost model achieved an excellent and stable diagnostic performance, as shown in the training group (AUC of 1.0) and testing group (AUC of 0.97), with a sensitivity of 80%, a specificity of 95%, and an accuracy of 88%, which was superior to VNCa (p < 0.05).
Conclusions
XGBoost combined with mpDECT yielded promising performance in differentiating between MM of the spine and VOM.
Key Points
• The multiparameters obtained from dual-energy CT of multiple myeloma differed significantly from those of vertebral osteolytic metastases.
• The virtual noncalcium offered the highest AUC in the univariate analysis to distinguish multiple myeloma from vertebral osteolytic metastases.
• Extreme gradient boosting combined with multiparameters from dual-energy CT had a promising performance to distinguish multiple myeloma from vertebral osteolytic metastases.






Similar content being viewed by others
Data Availability
The datasets generated and/or analysed during the current study are not publicly available but are available from the corresponding author on reasonable request.
Abbreviations
- AUC:
-
Area under the receiver operating characteristic curve
- DECT:
-
Dual-energy computed tomography
- ICC:
-
Intraclass correlation coefficient
- MM:
-
Multiple myeloma
- MRI:
-
Magnetic resonance imaging
- ROI:
-
Region of interest
- SPECT:
-
Single photon emission computed tomography
- VNCa:
-
Virtual noncalcium
- VOM:
-
Vertebral osteolytic metastases
- XGBoost:
-
Extreme gradient boosting
References
Lang N, Su M-Y, Yu HJ, Lin M, Hamamura MJ, Yuan H (2013) Differentiation of myeloma and metastatic cancer in the spine using dynamic contrast-enhanced MRI. Magn Reson Imaging 31:1285–1291
Iizuka Y, Iizuka H, Tsutsumi S et al (2009) Diagnosis of a previously unidentified primary site in patients with spinal metastasis: diagnostic usefulness of laboratory analysis, CT scanning and CT-guided biopsy. Eur Spine J 18:1431–1435
Agarwal A, Chirindel A, Shah BA, Subramaniam RM (2013) Evolving role of FDG PET/CT in multiple myeloma imaging and management. AJR Am J Roentgenol 200:884–890
Kosmala A, Weng AM, Heidemeier A et al (2018) Multiple myeloma and dual-energy CT: diagnostic accuracy of virtual noncalcium technique for detection of bone marrow infiltration of the spine and pelvis. Radiology 286:205–213
D’Oronzo S, Coleman R, Brown J, Silvestris F (2019) Metastatic bone disease: pathogenesis and therapeutic options: Up-date on bone metastasis management. J Bone Oncol 15:004–004
Coleman R, Hadji P, Body JJ et al (2020) Bone health in cancer: ESMO Clinical Practice Guidelines. Ann Oncol 31:1650–1663
Kumar SK, Callander NS, Adekola K et al (2020) Multiple myeloma, version 3.2021, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw 18:1685–1717
Kosmala A, Bley T, Petritsch B (2019) Imaging of Multiple Myeloma. Rofo 191:805–816
King A, Vlantis A, Bhatia K et al (2011) Primary nasopharyngeal carcinoma: diagnostic accuracy of MR imaging versus that of endoscopy and endoscopic biopsy. Radiology 258:531–537
Gosangi B, Mandell JC, Weaver MJ et al (2020) Bone marrow edema at dual-energy CT: a game changer in the emergency department. Radiographics 40:859–874
Zheng S, Dong Y, Miao Y et al (2014) Differentiation of osteolytic metastases and Schmorl’s nodes in cancer patients using dual-energy CT: advantage of spectral CT imaging. Eur J Radiol 83:1216–1221
Mallinson P, Coupal T, McLaughlin P, Nicolaou S, Munk P, Ouellette H (2016) Dual-Energy CT for the Musculoskeletal System. Radiology 281:690–707
Wu H, Dong S, Li X et al (2020) Clinical utility of dual-energy CT used as an add-on to 18F FDG PET/CT in the preoperative staging of resectable NSCLC with suspected single osteolytic metastases. Lung Cancer 140:80–86
Fervers P, Celik E, Bratke G et al (2021) Radiotherapy response assessment of multiple myeloma: a dual-energy CT approach with virtual non-calcium images. Front Oncol 11:734819
Fehr D, Schmidtlein CR, Hwang S, Deasy JO, Veeraraghavan H (2016) Automatic detection and tracking of longitudinal changes of multiple bone metastases from dual energy CT. Proc IEEE Int Symp Biomed Imaging 2016:168–171
Janssen RJ, Mourao-Miranda J, Schnack HG (2018) Making individual prognoses in psychiatry using neuroimaging and machine learning. Biol Psychiatr-Cogn Neurosci Neuroimaging 3:798–808
Handelman GS, Kok HK, Chandra RV, Razavi AH, Lee MJ, Asadi H (2018) eDoctor: machine learning and the future of medicine. J Intern Med 284:603–619
Chen T, Guestrin C (2016). XGBoost. https://doi.org/10.1145/2939672.2939785:785-794
Klontzas ME, Manikis GC, Nikiforaki K et al (2021) Radiomics and machine learning can differentiate transient osteoporosis from avascular necrosis of the hip. Diagnostics (Basel) 11(9):1686
Zhao Y, Chen R, Zhang T et al (2021) MRI-based machine learning in differentiation between benign and malignant breast lesions. Front Oncol 11:552634
Rajkumar SV, Dimopoulos MA, Palumbo A et al (2014) International Myeloma Working Group updated criteria for the diagnosis of multiple myeloma. Lancet Oncol 15:e538–e548
Li C, Chen J, Qin G (2019) Partial Youden index and its inferences. J Biopharm Stat 29:385–399
Kursa MB, Rudnicki WR (2010) Feature selection with the boruta package. J Stat Softw 36:1–13
Dong Y, Zheng S, Machida H et al (2015) Differential diagnosis of osteoblastic metastases from bone islands in patients with lung cancer by single-source dual-energy CT: advantages of spectral CT imaging. Eur J Radiol 84:901–907
Deniffel D, Sauter A, Dangelmaier J, Fingerle A, Rummeny EJ, Pfeiffer D (2019) Differentiating intrapulmonary metastases from different primary tumors via quantitative dual-energy CT based iodine concentration and conventional CT attenuation. Eur J Radiol 111:6–13
McCollough CH, Leng SA, Yu LF, Fletcher JG (2015) Dual- and multi-energy CT: principles, technical approaches, and clinical applications. Radiology 276:637–653
Wang Y, Chen Y, Zheng H, Huang X, Shan C, Bao Y (2020) Detection of different degree traumatic vertebral bone marrow oedema by virtual non-calcium technique of dual-source dual-energy CT. Clin Radiol 75(2):156-e11
Abdullayev N, Grosse Hokamp N, Lennartz S et al (2019) Improvements of diagnostic accuracy and visualization of vertebral metastasis using multi-level virtual non-calcium reconstructions from dual-layer spectral detector computed tomography. Eur Radiol 29:5941–5949
Issa G, Davis D, Mulligan ME (2018) The ability of dual-energy computed tomography to distinguish normal bone marrow from metastases using bone marrow color maps. J Comput Assist Tomogr 42:552–558
Barwick BG, Gupta VA, Vertino PM, Boise LH (2019) Cell of origin and genetic alterations in the pathogenesis of multiple myeloma. Front Immunol 10:1121
Hall MN, Jagannathan JP, Ramaiya NH, Shinagare AB, Van den Abbeele AD (2010) Imaging of extraosseous myeloma: CT, PET/CT, and MRI features. AJR Am J Roentgenol 195:1057–1065
Oliveira MB, Mello FC, Paschoal ME (2016) The relationship between lung cancer histology and the clinicopathological characteristics of bone metastases. Lung Cancer 96:19–24
Karatas M, Zengel B, Durusoy R et al (2021) Clinicopathologic features of single bone metastasis in breast cancer. Medicine (Baltimore) 100:e24164
Kursa MB, Jankowski A, Rudnicki WR (2010) Boruta – a system for feature selection. Fund Inform 101:271–285
Ahmed AAM, Deo RC, Ghahramani A et al (2021) LSTM integrated with Boruta-random forest optimiser for soil moisture estimation under RCP4.5 and RCP8.5 global warming scenarios. Stoch Env Res Risk Assess 35:1851–1881
Li W, Yin Y, Quan X, Zhang H (2019) Gene expression value prediction based on XGBoost algorithm. Front Genet 10:1077
Hou N, Li M, He L et al (2020) Predicting 30-days mortality for MIMIC-III patients with sepsis-3: a machine learning approach using XGboost. J Transl Med 18(1):1–14
Ogunleye A, Wang Q-G (2020) XGBoost model for chronic kidney disease diagnosis. IEEE-Acm Trans Comput Biol Bioinforma 17:2131–2140
Acknowledgements
We thank the study participants and referring technicians for their participation in this study.
Funding
This study has received funding from the National Natural Science Foundation of China (82071883), the Chongqing Natural Science Foundation (cstc2021jcyj-msxmX0313), Chongqing medical research project of a combination of science and medicine (grant No. 2021MSXM035), 2020 SKY Imaging Research Fund of the Chinese International Medical Foundation (project No. Z-2014–07-2003–24), an open fund from Chongqing Key Laboratory of Translational Research for Cancer Metastasis and Individualized Treatment, Chongqing University of Cancer Hospital.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Guarantor
The scientific guarantor of this publication is Jiuquan Zhang, from the Department of Radiology, Chongqing University Cancer Hospital, Chongqing, P.R. China.
E-mail: zhangjq_radiol@foxmail.com
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• Retrospective
• Observational
• Performed at one institution
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Xiaoxia Wang and Jiuquan Zhang are co-corresponding authors.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Shi, J., Huang, H., Xu, S. et al. XGBoost-based multiparameters from dual-energy computed tomography for the differentiation of multiple myeloma of the spine from vertebral osteolytic metastases. Eur Radiol 33, 4801–4811 (2023). https://doi.org/10.1007/s00330-023-09404-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-023-09404-7