Abstract
Objective
The purpose of this study was to evaluate the prognostic value of novel geometric variables obtained from pre-treatment [18F]FDG PET/CT with respect to classical ones in patients with non-small cell lung cancer (NSCLC).
Methods
Retrospective study including stage I–III NSCLC patients with baseline [18F]FDG PET/CT. Clinical, histopathologic, and metabolic parameters were obtained. After tumor segmentation, SUV and volume-based variables, global texture, sphericity, and two novel parameters, normalized SUVpeak to centroid distance (nSCD) and normalized SUVmax to perimeter distance (nSPD), were obtained. Early recurrence (ER) and short-term mortality (STM) were used as end points. Univariate logistic regression and multivariate logistic regression with respect to ER and STM were performed.
Results
A cohort of 173 patients was selected. ER was detected in 49/104 of patients with recurrent disease. Additionally, 100 patients died and 53 had STM. Age, pathologic lymphovascular invasion, lymph nodal infiltration, TNM stage, nSCD, and nSPD were associated with ER, although only age (aOR = 1.06, p = 0.002), pathologic lymphovascular invasion (aOR = 3.40, p = 0.022), and nSPD (aOR = 0.02, p = 0.018) were significant independent predictors of ER in multivariate analysis. Age, lymph nodal infiltration, TNM stage, nSCD, and nSPD were predictors of STM. Age (aOR = 1.05, p = 0.006), lymph nodal infiltration (aOR = 2.72, p = 0.005), and nSPD (aOR = 0.03, p = 0.022) were significantly associated with STM in multivariate analysis. Coefficient of variation (COV) and SUVmean/SUVmax ratio did not show significant predictive value with respect to ER or STM.
Conclusion
The geometric variables, nSCD and nSPD, are robust biomarkers of the poorest outcome prediction of patients with NSCLC with respect to classical PET variables.
Key Points
• In NSCLC patients, it is crucial to find prognostic parameters since TNM system alone cannot explain the variation in lung cancer survival.
• Age, lymphovascular invasion, lymph nodal infiltration, and metabolic geometrical parameters were useful as prognostic parameters.
• The displacement grade of the highest point of metabolic activity towards the periphery assessed by geometric variables obtained from [18F]FDG PET/CT was a robust biomarker of the poorest outcome prediction of patients with NSCLC.



Similar content being viewed by others
Abbreviations
- Ach:
-
Adjuvant chemotherapy
- ADC:
-
Adenocarcinoma
- aOR:
-
Adjusted odds ratio
- CCI:
-
Charlson Comorbidity Index
- COV:
-
Coefficient of variation
- DFS:
-
Disease-free survival
- ER:
-
Early recurrence
- MTV:
-
Metabolic tumor volume
- NSCLC:
-
Non-small cell lung carcinoma
- OR:
-
Odds ratio
- OS:
-
Overall survival
- PORT:
-
Postoperative radiotherapy
- SCC:
-
Squamous cell carcinoma
- STM:
-
Short-term mortality
- SUV:
-
Standardized uptake value
- TLG:
-
Total lesion glycolysis
- TNM:
-
Tumor node metastasis
- VOI:
-
Volume of interest
References
Barta JA, Powell CA, Wisnivesky JP (2019) Global epidemiology of lung cancer. Ann Glob Health 85:8. https://doi.org/10.5334/aogh.2419
Yoshino I, Yohena T, Kitajima M et al (2001) Survival of non-small cell lung cancer patients with postoperative recurrence at distant organs. Ann Thorac Cardiovasc Surg 7:204–209
Sugimura H, Nichols FC, Yang P et al (2007) Survival after recurrent nonsmall-cell lung cancer after complete pulmonary resection. Ann Thorac Surg 83:409–418. https://doi.org/10.1016/j.athoracsur.2006.08.046
Anwar H, Vogl TJ, Abougabal MA et al (2018) The value of different [18F]FDG PET/CT baseline parameters in risk stratification of stage I surgical NSCLC patients. Ann Nucl Med 32:687–694. https://doi.org/10.1007/s12149-018-1301-9
Goldstraw P, Crowley J, Chansky K et al (2007) The IASLC Lung Cancer Staging Project: proposals for the revision of the TNM stage groupings in the forthcoming (seventh) edition of the TNM classification of malignant tumours. J Thorac Oncol 2:706–714. https://doi.org/10.1097/JTO.0b013e31812f3c1a
Ávila Martínez RJ (2018) Invasión de la pleura visceral como factor pronóstico del carcinoma brocogenético no células pequeñas. Doctoral thesis, Universidad Complutense de Madrid
Mizuno T, Arimura T, Kuroda H, Sakakura N, Yatabe Y, Sakao Y (2018) Current outcomes of postrecurrence survival in patients after resection of non-small cell lung cancer. J Thorac Dis 10:1788–1796. https://doi.org/10.21037/jtd.2018.01.148
Choi PJ, Jeong SS, Yoon SS (2013) Prognosis of recurrence after complete resection in early-stage non-small cell lung cancer. The Korean Journal of Thoracic and Cardiovascular Surgery 46:449–456. https://doi.org/10.5090/kjtcs.2013.46.6.449
Battafarano RJ, Piccirillo JF, Meyers BF et al (2002) Impact of comorbidity on survival after surgical resection in patients with stage I non-small cell lung cancer. J Thorac Cardiovasc Surg 123:280–287. https://doi.org/10.1067/mtc.2002.119338
Bauml J, Mick R, Zhang Y et al (2013) Determinants of survival in advanced non-small-cell lung cancer in the era of targeted therapies. Clin Lung Cancer 14:581–591. https://doi.org/10.1016/j.cllc.2013.05.002
Ettinger DS, Wood DE, Aisner DL et al (2017) Non–small cell lung cancer, version 5.2017, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw 15:504–535. https://doi.org/10.6004/jnccn.2017.0050
Postmus PE, Kerr KM, Oudkerk M et al (2017) Early and locally advanced non-small-cell lung cancer (NSCLC): ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 28:iv1–iv21. https://doi.org/10.1093/annonc/mdx222
Ahn HK, Lee H, Kim SG, Hyun SH (2019) Pre-treatment [18F]FDG PET-based radiomics predict survival in resected non-small cell lung cancer. Clin Radiol 74:467–473. https://doi.org/10.1016/j.crad.2019.02.008
Kirienko M, Cozzi L, Antunovic L et al (2018) Prediction of disease-free survival by the PET/CT radiomic signature in non-small cell lung cancer patients undergoing surgery. Eur J Nucl Med Mol Imaging 45:207–217. https://doi.org/10.1007/s00259-017-3837-7
Im H-J, Pak K, Cheon GJ et al (2015) Prognostic value of volumetric parameters of 18 F-FDG PET in non-small-cell lung cancer: a meta-analysis. Eur J Nucl Med Mol Imaging 42:241–251. https://doi.org/10.1007/s00259-014-2903-7
Dong M, Liu J, Sun X, Xing L (2017) Prognostic significance of SUV(max) on pretreatment (18) F-FDG PET/CT in early-stage non-small cell lung cancer treated with stereotactic body radiotherapy: a meta-analysis. J Med Imaging Radiat Oncol 61:652–659. https://doi.org/10.1111/1754-9485.12599
Na F, Wang J, Li C, Deng L, Xue J, Lu Y (2014) Primary tumor standardized uptake value measured on F18-fluorodeoxyglucose positron emission tomography is of prediction value for survival and local control in non-small-cell lung cancer receiving radiotherapy: meta-analysis. J Thorac Oncol 9:834–842. https://doi.org/10.1097/jto.0000000000000185
Liu J, Dong M, Sun X, Li W, Xing L, Yu J (2016) Prognostic value of [18F]FDG PET/CT in surgical non-small cell lung cancer: a meta-analysis. PLoS One 11:e0146195. https://doi.org/10.1371/journal.pone.0146195
Paesmans M, Berghmans T, Dusart M et al (2010) Primary tumor standardized uptake value measured on fluorodeoxyglucose positron emission tomography is of prognostic value for survival in non-small cell lung cancer: update of a systematic review and meta-analysis by the European Lung Cancer Working Part. J Thorac Oncol 5:612–619. https://doi.org/10.1097/JTO.0b013e3181d0a4f5
Domachevsky L, Groshar D, Galili R, Saute M, Bernstine H (2015) Survival prognostic value of morphological and metabolic variables in patients with stage I and II non-small cell lung cancer. Eur Radiol 25:3361–3367. https://doi.org/10.1007/s00330-015-3754-8
Han S, Woo S, Suh CH, Kim YJ, Oh JS, Lee JJ (2018) A systematic review of the prognostic value of texture analysis in 18 F-FDG PET in lung cancer. Ann Nucl Med 32:602–610. https://doi.org/10.1007/s12149-018-1281-9
Tello Galán MJ, García Vicente AM, Pérez Beteta J et al (2019) Global heterogeneity assessed with [18F]FDG PET/CT. Relation with biological variables and prognosis in locally advanced breast cancer. Rev Esp Med Nucl Imagen Mol (Engl Ed) 38:290–297. https://doi.org/10.1016/j.remn.2019.02.004
Kirienko M, Gallivanone F, Sollini M et al (2017) FDG PET/CT as theranostic imaging in diagnosis of non-small cell lung cancer. Front Biosci (Landmark Ed) 22:1713–1723. https://doi.org/10.2741/4567
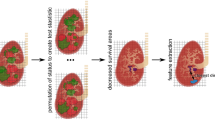
Jiménez-Sánchez J, Bosque JJ, Jiménez Londoño GA et al (2021) Evolutionary dynamics at the tumor edge reveal metabolic imaging biomarkers. Proc Natl Acad Sci (U S A) 118:e2018110118. https://doi.org/10.1073/pnas.2018110118
Detterbeck FC, Boffa DJ, Kim AW, Tanoue LT (2017) The eighth edition lung cancer stage classification. Chest 151:193–203. https://doi.org/10.1016/j.chest.2016.10.010
Majem M, Juan O, Insa A et al (2018) SEOM clinical guidelines for the treatment of non-small cell lung cancer. Clin Transl Oncol 21(2019):3–17. https://doi.org/10.1007/s12094-018-1978-1
Travis WD, Brambilla E, Nicholson AG et al (2015) The 2015 World Health Organization classification of lung tumors: impact of genetic, clinical and radiologic advances since the 2004 classification. J Thorac Oncol 10:1243–1260. https://doi.org/10.1097/JTO.0000000000000630
Jiménez Londoño GA, Pérez-Beteta J, Bosque JJ, Honguero-Martinez AF, García Vicente AM (2020) Segmentation in non–small cell lung tumors using [18F]FDG PET/CT. Clin Nucl Med 45:e477–e482. https://doi.org/10.1097/rlu.0000000000003166
Coroller TP, Agrawal V, Huynh E et al (2017) Radiomic-based pathological response prediction from primary tumors and lymph nodes in NSCLC. J Thorac Oncol 12:467–476. https://doi.org/10.1016/j.jtho.2016.11.2226
Pérez-Beteta J, Molina-García D, Ortiz-Alhambra JA et al (2018) Tumor surface regularity at MR imaging predicts survival and response to surgery in patients with glioblastoma. Radiology. 288:218–225. https://doi.org/10.1148/radiol.2018171051
Siegel RL, Miller KD, Jemal A (2020) Cancer statistics, 2020. CA Cancer J Clin 70:7–30. https://doi.org/10.3322/caac.21590
Walters S, Maringe C, Coleman MP et al (2013) Lung cancer survival and stage at diagnosis in Australia, Canada, Denmark, Norway, Sweden and the UK: A population-based study, 2004-2007. Thorax 68:551–564. https://doi.org/10.1136/thoraxjnl-2012-202297
Luo J, Wang R, Han B et al (2017) Solid predominant histologic subtype and early recurrence predict poor postrecurrence survival in patients with stage I lung adenocarcinoma. Oncotarget 8:7050–7058. https://doi.org/10.18632/oncotarget.12540
Hung JJ, Jeng WJ, Hsu WH et al (2010) Prognostic factors of postrecurrence survival in completely resected stage I non-small cell lung cancer with distant metastasis. Thorax 65:241–245. https://doi.org/10.1136/thx.2008.110825
Cho BC, De Pas T, Kalofonos H et al (2019) Prognostic Factors in Early-stage NSCLC: Analysis of the Placebo Group in the MAGRIT Study. Anticancer Res 39:1403–1409. https://doi.org/10.21873/anticanres.13255
Wei S, Asamura H, Kawachi R, Sakurai H, Watanabe SI (2011) Which is the better prognostic factor for resected non-small cell lung cancer: the number of metastatic lymph nodes or the currently used nodal stage classification? J Thorac Oncol 6:310–318. https://doi.org/10.1097/JTO.0b013e3181ff9b45
Lopez Guerra JL, Gomez DR, Lin SH et al (2013) Risk factors for local and regional recurrence in patients with resected N0-N1 non-small-cell lung cancer, with implications for patient selection for adjuvant radiation therapy. Ann Oncol 24:67–74. https://doi.org/10.1093/annonc/mds274
Kiankhooy A, Taylor MD, Lapar DJ et al (2014) Predictors of early recurrence for node-negative t1 to T2B non-small cell lung cancer. Ann Thorac Surg 98:1175–1183. https://doi.org/10.1016/j.athoracsur.2014.05.061
Kim K, Kim S-J, Kim I-J, Kim YS, Pak K, Kim H (2012) Prognostic value of volumetric parameters measured by F-18 FDG PET/CT in surgically resected non-small-cell lung cancer. Nucl Med Commun 33:613–620. https://doi.org/10.1097/MNM.0b013e328351d4f5
Berghmans T, Dusart M, Paesmans M et al (2008) Primary tumor standardized uptake value (SUVmax) measured on fluorodeoxyglucose positron emission tomography (FDG-PET) is of prognostic value for survival in non-small cell lung cancer (NSCLC): a systematic review and meta-analysis (MA) by the European Lu. J Thorac Oncol 3:6–12. https://doi.org/10.1097/JTO.0b013e31815e6d6b
Hyun SH, Choi JY, Kim K et al (2013) Volume-based parameters of 18F-fluorodeoxyglucose positron emission tomography/computed tomography improve outcome prediction in early-stage non–small cell lung cancer after surgical resection. Ann Surg 257:364–370. https://doi.org/10.1097/SLA.0b013e318262a6ec
Liao S, Penney BC, Wroblewski K et al (2012) Prognostic value of metabolic tumor burden on 18 F-FDG PET in nonsurgical patients with non-small cell lung cancer. Eur J Nucl Med Mol Imaging 39:27–38. https://doi.org/10.1007/s00259-011-1934-6
Finkle JH, Jo SY, Ferguson MK et al (2017) Risk-stratifying capacity of PET/CT metabolic tumor volume in stage IIIA non-small cell lung cancer. Eur J Nucl Med Mol Imaging 44:1275–1284. https://doi.org/10.1007/s00259-017-3659-7
Park SY, Cho A, Yu WS et al (2015) Prognostic value of total lesion glycolysis by [18F]FDG PET/CT in surgically resected stage IA non–small cell lung cancer. J Nucl Med 56:45–49. https://doi.org/10.2967/jnumed.114.147561
Hyun SH, Ahn HK, Kim H et al (2014) Volume-based assessment by 18 F-FDG PET/CT predicts survival in patients with stage III non-small-cell lung cancer. Eur J Nucl Med Mol Imaging 41:50–58. https://doi.org/10.1007/s00259-013-2530-8
Melloni G, Gajate AMS, Sestini S et al (2013) New positron emission tomography derived parameters as predictive factors for recurrence in resected stage I non-small cell lung cancer. Eur J Surg Oncol 39:1254–1261. https://doi.org/10.1016/j.ejso.2013.07.092
Vesselle H, Freeman JD, Wiens L et al (2007) Fluorodeoxyglucose uptake of primary non-small cell lung cancer at positron emission tomography: new contrary data on prognostic role. Clin Cancer Res 13:3255–3263. https://doi.org/10.1158/1078-0432.CCR-06-1128
Agarwal M, Brahmanday G, Bajaj SK, Ravikrishnan KP, Wong C-YO (2010) Revisiting the prognostic value of preoperative 18 F-fluoro-2-deoxyglucose (18 F-FDG) positron emission tomography (PET) in early-stage (I & II) non-small cell lung cancers (NSCLC). Eur J Nucl Med Mol Imaging 37:691–698. https://doi.org/10.1007/s00259-009-1291-x
Hoang JK, Hoagland LF, Coleman RE, Coan AD, Herndon JE, Patz EF (2008) Prognostic value of fluorine-18 fluorodeoxyglucose positron emission tomography imaging in patients with advanced-stage non-small-cell lung carcinoma. J Clin Oncol 26:1459–1464. https://doi.org/10.1200/JCO.2007.14.3628
Kurtipek E, Çayc M, Düzgün N et al (2015) [18F]FDG PET/CT mean SUV and metabolic tumor volume for mean survival time in non–small cell lung cancer. Clin Nucl Med 40:459–463. https://doi.org/10.1097/RLU.0000000000000740
Yoo IR, Chung SK, Park HL et al (2014) Prognostic value of SUVmax and metabolic tumor volume on [18F]FDG PET/CT in early stage non-small cell lung cancer patients without LN metastasis. Biomed Mater Eng 24:3091–3103. https://doi.org/10.3233/BME-141131
Lin Y, Lin W-Y, Kao C-H, Yen K-Y, Chen S-W, Yeh J-J (2012) Prognostic value of preoperative metabolic tumor volumes on PET-CT in predicting disease-free survival of patients with stage I non-small cell lung cancer. Anticancer Res 32:5087–5091
Grabinska K, Pelak M, Wydmanski J, Tukiendorf A, D’Amico A (2015) Prognostic value and clinical correlations of 18-fluorodeoxyglucose metabolism quantifiers in gastric cancer. World J Gastroenterol 21:5901–5909. https://doi.org/10.3748/wjg.v21.i19.5901
Bundschuh RA, Dinges J, Neumann L et al (2014) Textural parameters of tumor heterogeneity in [18F]FDG PET/CT for therapy response assessment and prognosis in patients with locally advanced rectal cancer. J Nucl Med 55:891–897. https://doi.org/10.2967/jnumed.113.127340
Apostolova I, Rogasch J, Buchert R et al (2014) Quantitative assessment of the asphericity of pretherapeutic FDG uptake as an independent predictor of outcome in NSCLC. BMC Cancer 14:896. https://doi.org/10.1186/1471-2407-14-896
Apostolova I, Ego K, Steffen IG et al (2016) The asphericity of the metabolic tumour volume in NSCLC: correlation with histopathology and molecular markers. Eur J Nucl Med Mol Imaging 43:2360–2373. https://doi.org/10.1007/s00259-016-3452-z
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Germán Andrés Jiménez Londoño.
Conflict of interest
The authors of this manuscript declare no relationships with any companies whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was obtained from all subjects (patients) in this study.
Ethical approval
Institutional review board approval was obtained.
Methodology
• retrospective
• prognostic study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(DOCX 18 kb)
Rights and permissions
About this article
Cite this article
Jiménez Londoño, G.A., García Vicente, A.M., Bosque, J.J. et al. SUVmax to tumor perimeter distance: a robust radiomics prognostic biomarker in resectable non-small cell lung cancer patients. Eur Radiol 32, 3889–3902 (2022). https://doi.org/10.1007/s00330-021-08523-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-021-08523-3