Abstract
Purpose
To study the thyroid image reporting and data system (TI-RADS) classification and the contrast-enhanced ultrasound (CEUS) enhancement pattern of thyroid nodules, and to determine whether combined use of both methods is helpful in the diagnosis of thyroid nodules.
Methods
A total of 319 thyroid nodules in 246 patients were assessed with TI-RADS, CEUS and a combination of both methods. The diagnostic performance of TI-RADS, CEUS and a combination of both methods was compared.
Results
The accuracy in the diagnosis of thyroid nodules was 90.3 % for TI-RADS, 90.0 % for CEUS and 96.0 % for a combination of both methods respectively. A statistically significant difference was not observed in the diagnostic accuracy of CEUS and TI-RADS (P > 0.05). However, a significant difference was observed between a combination of both methods and either alone (P < 0.01). A combination of both methods showed high sensitivity, specificity and accuracy for TI-RADS classifications of 4a and 4b thyroid nodules compared with TI-RADS alone (P < 0.01) and a statistically significant difference was not observed for thyroid nodules classified as 2, 3, and 5 (P > 0.05).
Conclusions
The improved TI-RADS, when combined with CEUS, could significantly improve the diagnostic accuracy for thyroid nodules, especially for TI-RADS class-4 thyroid nodules.
Key Points
• TI-RADS can be used as the primary diagnostic standard for thyroid nodules
• CEUS can be used as an important complement to TI-RADS
• The improved TI-RADS can significantly improve the qualitative diagnostic accuracy
Similar content being viewed by others
Explore related subjects
Find the latest articles, discoveries, and news in related topics.Avoid common mistakes on your manuscript.
Introduction
The wide application of ultrasound (US) and other technologies in recent years has led to an increasing number of thyroid nodule diagnoses [1]. The pathological nature of thyroid nodules directly affects the therapeutic methodology and patient prognosis; therefore, the correct diagnosis of thyroid nodules at an early stage has important clinical significance. However, conventional sonographic diagnoses for thyroid nodules presents limitations related to overlapping boundaries, morphologies, internal blood streams, and echoes between malignant and benign nodules. In addition, subjective factors related to the diagnostician can also affect the accuracy of the diagnosis. Therefore, research by Park et al. [2], Horvath et al. [3] and Kwak et al. [4] indicates that the thyroid imaging reporting and data system (TI-RADS), which is based on the breast imaging reporting and data system (BI-RADS), can be used to improve the diagnostic accuracy of thyroid nodules by US, which will provide improvements that can be used in clinical practice.
Contrast-enhanced ultrasound (CEUS) is a focus of current medical US research. CEUS has developed rapidly and is now widely used in many areas of medical US, particularly in diagnoses of liver tumour, and it has greatly improved the specificity and sensitivity of US diagnoses and achieved great clinical value. In recent years, an increasing number of CEUS applications have been developed for thyroid diagnoses in clinical practice, and a number of investigations have been performed to evaluate the different contrast modes in the diagnosis of thyroid nodules. Studies have reported that CEUS can help accurately diagnose both benign and malignant thyroid nodules [5–10].
Currently, studies have reported that both TI-RADS and CEUS can effectively diagnose thyroid nodules; thus, a new scale standard for TI-RADS classification that includes CEUS should be proposed. This paper presents the results of studies performed on 319 thyroid nodules in 246 thyroid patients using TI-RADS, CEUS and combined method with the goal of investigating the value of diagnosing thyroid nodules with the combined CEUS and TI-RADS classification and determining a new and more effective TI-RADS diagnosis standard.
Materials and methods
Study subjects
In this study, 246 patients who had received conventional US examinations and CEUS examinations as well as postoperative pathological diagnoses or fine-needle aspiration biopsies (FNABs) between December 2012 and December 2014 in our hospital were recruited. In total, 319 nodule lesions were identified. The patients included 161 women and 85 men; their ages ranged from 19-74 years, and the average was (46.1 ± 15.2) years. The diameter range of the lesions was 2.5-46 mm, and the average was (11.9 ± 3.3) mm. FNAB was performed on 230 nodules, and resection was performed on 89 nodules. The details of the pathological types of thyroid nodules are as follows: 319 nodules included 244 benign nodules and 75 malignant nodules; the benign nodules included 210 nodular goitres, 23 adenomas, 6 adenomatous nodular goitres and 5 inflammatory nodules, and there were 8 thyroid nodules coexisting with Hashimotoʼs thyroiditis in 210 nodular goitres; and the malignant nodules included 58 papillary carcinomas, 8 nodular goitres with complications of local papillary carcinoma, 4 follicular carcinomas, 4 nodular goitres with complications of local follicular cancer and 1 medullary carcinoma. All of the lesions were accompanied by postoperative pathological results or FNAB results. The present study was approved by the hospital ethics committee, and all of the patients provided informed consent.
Instruments and examination methods
The instrument used in the diagnoses performed here is a Siemens Acuson S2000 colour Doppler US system (Siemens; Mountain View, CA, USA), with contrast pulsed sequencing (CPS) and equipped with an 14 L5 transducer for conventional US and an 9 L4 transducer for CEUS. Every section of the thyroid was carefully scanned, the ultrasonic characteristics of the thyroid structure were observed and recorded, and the images were saved. TI-RADS was used to evaluate and classify every thyroid nodule. The CPS technique and SonoVue contrast agent (Bracco, Milan, Italy) were used. A 20-G needle was inserted into the patientsʼ peripheral veins to establish intravenous access. The contrast agent was mixed with 5 ml saline and shaken to homogeneity, and 2.4 ml of the suspension was then quickly pushed into the peripheral vein with the probe and body position unchanged, and the patient was told not to swallow. The dynamic perfusion process of the lesion was continuously monitored in real time, and the images were saved on the hard drive of the ultrasound diagnosis instrument.
All examinations were performed by an experienced radiologist with more than a decade of experience each in US diagnosis and more than 1 years’ experience of performing CEUS of thyroid nodules in order to exclude the bias from different operators. The US imaging data were respectively analysed by two other experienced radiologists with more than a decade of experience in US diagnosis and with more than 1 years’ experience of performing CEUS. They performed blind independent analyses of the TI-RADS and CEUS images to retrospectively analyse the nature of the thyroid nodules. Then the combined methodology was comprehensively analysed by the third radiologist.
The 4a, 4b thyroid nodules which were categorised by TI-RADS and a combination of TI-RADS and CEUS were studied retrospectively. The correlation between US or CEUS features and pathological findings was analysed statistically. Logistic regression was used to improve the analytical results. The inter-observer variability between experienced and inexperienced examiners using TI-RADS and CEUS was evaluated retrospectively. The US imaging data were independently analysed by an experienced and inexperienced examiner using TI-RADS and CEUS, respectively.
Diagnostic criteria
TI-RADS diagnostic criteria
We have proposed a new classification standard based on the TI-RADS classification criteria proposed by Park et al. [2], Horvath et al. [3] and Kwak et al. [4], and the five ultrasound signs (solid component, marked hypoechogenicity, irregular margins, microcalcifications, taller than wide shape) proposed by Kwak et al. [4]. The new standard was compared with the TI-RADS classification standard proposed by Kwak et al. [4].
Kwak et al. [4] TI-RADS classification criteria:
-
TI-RADS score 1:
normal thyroid
-
TI-RADS score 2:
no malignant sign, benign lesions
-
TI-RADS score 3:
no malignant sign, high probability of benignity
-
TI-RADS score 4a:
one malignant sign; possible benignity
-
TI-RADS score 4b:
two malignant signs; possible malignancy
-
TI-RADS score 4c:
three or four malignant signs; high possibility of malignancy
-
TI-RADS score 5:
five malignant signs, highly indicative of malignancy
TI-RADS classification criteria in the present study:
-
TI-RADS score 1:
normal thyroid
-
TI-RADS score 2:
no malignant sign, benign lesions
-
TI-RADS score 3:
one malignant sign, high probability of benignity
-
TI-RADS score 4a:
two malignant signs, possible benignity
-
TI-RADS score 4b:
three malignant signs, high probability of malignancy
-
TI-RADS score 5:
four to five malignant signs, highly suggestive of malignancy
Benign and malignant diagnostic criteria by TI-RADS classification: scores 1-4a are diagnosed as benign and scores 4b-5 are diagnosed as malignant.
CEUS diagnostic criteria
In the present study, the CEUS diagnostic criteria are divided into circular enhancement, high enhancement, equal enhancement and low enhancement based on the different US contrast modes. If the contrast indicates high enhancement, circular enhancement or equal enhancement, then the nodule is diagnosed as benign. If the contrast indicates low enhancement, then the nodule is diagnosed as malignant.
Improved TI-RADS diagnostic criteria in combination with CEUS
If the CEUS indicates high enhancement or circular enhancement, then one score is subtracted from the TI-RADS classification and score 2 is kept the same. If the CEUS indicates low enhancement, then one score is added to the TI-RADS classification, and score 5 remains the same. If the CEUS indicates equal enhancement, then the TI-RADS classification remains the same.
Statistical analysis
SPSS 19.0 software was used for the statistical analysis. Quantitative data are expressed as the means ± standard deviation. The χ2 test was used to compare the distribution of US indicators for benign and malignant thyroid nodule. The sensitivity, specificity, accuracy, positive prediction value (PPV) and negative prediction value (NPV) of the benign and malignant thyroid nodule diagnoses by TI-RADS, CEUS and combined method were calculated, and the χ2 test was used to compare the three methods, with a value of P < 0.05 representing significant differences. The diagnostic accuracy of score 2-5 thyroid nodules by a combination of both methods and by TI-RADS alone was compared, with P < 0.05 representing significant differences. In addition, logistic regression was used to evaluate the diagnostic performance of the 4a, 4b thyroid nodules, which were categorised by TI-RADS and a combination of TI-RADS and CEUS. Inter-observer variability between experienced and inexperienced examiners using TI-RADS and CEUS were obtained and analysed with the Cohen’s statistic.
Results
TI-RADS results
TI-RADS diagnostic information
The malignancy rates of TI-RADS score 2, score 3, score 4a score 4b, score 5 were 0,3.0,10.8,67.2, and 92.9 %, respectively (Table 1).
TI-RADS diagnostic classification by Kwak et al.
A comparative study was performed between the classification criteria proposed by Kwak et al. [4] and the classification criteria presented here, and the results show that there is a significant difference between the two classification methods (χ2 = 27.9, P < 0.01) (Tables 2 and 3).
CEUS results
Among the 75 malignant nodules in the present study, 58 (77.3 %) indicated low-enhancement mode, 13 (17.3 %) indicated equal enhancement mode, 2 (2.7 %) indicated high-enhancement mode and 2 (2.7 %) indicated circular enhancement. Among the 244 benign nodules, 15 (6.1 %) indicated low-enhanced mode, and 229 (93.9 %) indicated equal enhancement, circular enhancement or high-enhancement mode (Table 4).
Accuracy of thyroid nodule diagnoses by CEUS combined with TI-RADS
When CEUS and TI-RADS were used together for diagnosis, the malignancy rate of nodules classified as 4a and below was decreased compared with that of TI-RADS alone, whereas the malignancy rate of nodules classified as 4b and above was increased compared with that of TI-RADS alone (Table 5). The results from FNAB and pathological tests were used to verify the accuracy of the tested methods, and the sensitivity, specificity, accuracy, PPV and NPV of malignant thyroid nodule diagnoses by TI-RADS, CEUS and the combined method were compared. Significant differences were not observed between the diagnoses by CEUS alone and TI-RADS alone (χ2 = 0.01, P > 0.05), whereas significant differences were observed between the diagnoses of the combined method and that of TI-RADS alone and CEUS alone (χ2 = 9.0, P < 0.01; χ2 = 9.8, P < 0.01) (Table 6, Figs. 1, 2, 3 and 4).
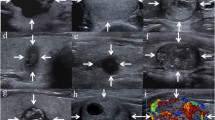
A 35-year-old man was found to have an 8 × 6-mm solid hypoechoic nodule in the left lobe of his thyroid. a A conventional two-dimensional image. This nodule had three malignant indicators (solid, markedly hypoechoic, and microcalcifications), and it was classified to a 4b TI-RADS score. b The ultrasound contrast status and the enhancement mode indicated high enhancement. The improved TI-RADS combined with CEUS returned a score of 4a, which indicates a benign nodule. c The pathological image of the lesion, which was of a nodular goitre
A 42-year-old woman was found to have a 32 × 15-mm solid nodule in the left lobe of her thyroid. a A conventional two-dimensional image. This nodule had two malignant indicators (solid and irregular margin), and it was classified to a 4a TI-RADS score. b An ultrasound contrast image, and the enhancement mode indicates low enhancement. The improved TI-RADS combined with CEUS returned a score of 4b, and the diagnosis indicated a malignant nodule. c The pathological image of the lesion, which is a thyroid papillary carcinoma
A 38-year-old woman was found to have a 12 × 12.5-mm solid hypoechoic nodule in the left lobe of her thyroid. a A conventional two-dimensional image. This nodule had three malignant indicators (solid, aspect ratio greater than 1 and markedly hypoechoic) and was classified to a 4b TI-RADS score. b An ultrasound contrast image; the enhancement mode was low enhancement. The improved TI-RADS combined with CEUS returned a score of 5, and the diagnosis indicates a malignant nodule. c The pathological image of the lesion, which is a thyroid papillary carcinoma
A 48-year-old woman was found to have a 14 × 12-mm solid hypoechoic nodule in the right lobe of her thyroid. a A conventional two-dimensional image. This nodule had four malignant indicators (solid, irregular margin, markedly hypoechoic and microcalcifications); it was classified to a TI-RADS score of 5. b An ultrasound contrast image; the enhancement mode was low enhancement. The improved TI-RADS combined with CEUS returned a score of 5, and the diagnosis indicates a malignant nodule. c The pathological image of the lesion, which is a thyroid papillary carcinoma
A combination of both methods diagnoses of thyroid nodules classified as 2-5
The results show that a significant difference occurred between the thyroid nodule diagnoses classified as 4a (P < 0.01) and 4b (P < 0.01) by a combination of both methods and TI-RADs alone, whereas a significant difference was not observed for diagnoses classified as 2, 3 and 5 (P > 0.05) (Table 7).
Logistic regression analysis
At logistic regression analysis of 4a, 4b thyroid nodules, the following features showed a association with malignancy: solid component, marked hypoechogenicity, irregular margins, microcalcifications, taller than wide shape and low enhancement (Tables 8 and 9).
Inter-observer variability between experienced and inexperienced examiners
The inter-examiner measurement agreement for TI-RADS and CEUS had a high positive correlation even between experienced and inexperienced examiners (k = 0.885, k = 0.990, respectively, Tables 10 and 11).
Discussion
Early diagnosis, correct identification and diagnosis of the benignity and malignancy of thyroid nodules has important significance for clinical treatment method selections and prognosis predictions. TI-RADS classification identifies the benignity and malignancy of nodules through a comprehensive analysis of nodule morphological characteristics, and this classification provides a standard for the diagnosis of thyroid nodules; however, improvements can be made in its application for the identification of benignity and malignancy among thyroid nodules [2–4, 11]. CEUS is a recently developed ultrasound imaging technology, and studies have shown that monitoring microcirculation perfusions after the injection of microbubble contrast agents can be used to identify the benignity and malignancy of thyroid nodules [5–10]. However, to our knowledge, studies presenting TI-RADS classification criteria that also consider CEUS diagnoses have not been reported. Thus, the primary goal of the present study was to develop a new and effective TI-RADS classification standard by investigating the value of diagnosing thyroid nodules using CEUS combined with TI-RADS and determining whether improvements were made to the diagnostic accuracy.
Currently, a number of scholars have begun applying TI-RADS classifications to thyroid nodules [2–4]; however, a generalised standard has not been developed. In the present study, we have referenced BI-RADS classifications and the classifications by Park et al. [2], Horvath et al. [3] and Kwak et al. [4] to classify thyroid nodules as score 1-5, with score 4 divided into the subscores 4a and 4b. Clinical practice has confirmed that this classification is simple and practical. To develop an objective classification, the American scholar Horvath et al. [3] first proposed a classification using ten US sonographic characteristics, whereas Park et al. [2] proposed using 12 US sonographic characteristics. Recently, Korean scholars Kwak et al. [4] proposed using five ultrasound sonographic characteristics for the classification, and these characteristics are simple and generalised, and highly practical in clinical practice. Therefore, in the present study, we used these five US signs for the classification of each thyroid nodule, although certain flaws were noted [4]. In the classification, malignant indicators are not available for scores 2 and 3; therefore, the difference between these two scores is vague. In the present study, we separated score 2 from score 3 and classified nodules with one malignant sign as score 3. This classification facilitates the standardisation of scores 2 and 3, and reduces the subjectivity of their classification. In addition, the standard presented here classifies nodules with one malignant sign as score 4a and nodules with two malignant signs as score 4b; thus, there may be higher false-positive rates.
To verify the accuracy and effectiveness of the classification standard in the present study, we performed a comparative analysis with the classification method by Kwak et al. [4]. The results showed that our classification method has a higher accuracy than the classification method by Kwak et al. (90.3 % vs 73.8 %). Moreover, because the criteria presented here classify nodules with two malignant signs as score 4a and nodules with three malignant signs as score 4b, the false-positive rate is significantly reduced, which may prevent unnecessary surgical treatment. In the present study, we misdiagnosed 31 nodules based on TI-RADS standards, which accounted for 9.7 % of the diagnoses. The misdiagnosed nodules were mainly in scores 4a and 4b, indicating that these two scores have a degree of overlap.
As an important technique in US medicine, CEUS has played an important role in the diagnosis of thyroid lesions over the last decade [5–10, 12]. Studies from numerous researchers suggest that most of the contrasts indicating low enhancement and heterogeneous enhancement are malignant thyroid nodules [5, 9], whereas most contrast modes indicating high enhancement and circular enhancement are benign nodules [7]. CEUS has been proposed to evaluate the thyroid nodules and the sensitivity, specificity and accuracy for the diagnosis of malignant thyroid nodules were reported to be 76.9–88.2 %, 84.8–95.1 % and 82.6–90.4 % [5–7], respectively. The results presented here are consistent with the results of the above-mentioned studies, which indicates that CEUS has clinical value in the identification and diagnosis of benignity and malignancy of thyroid nodules. In this study, 31 nodules were misdiagnosed based only on TI-RADS standards, and 32 nodules were misdiagnosed based only on CEUS standards. A statistically significant difference was not observed in the diagnostic accuracy of CEUS and TI-RADS. Nineteen misdiagnosed nodules based only on TI-RADS standards were correctly diagnosed by CEUS, and 20 misdiagnosed nodules based only on CEUS standards were correctly diagnosed by TI-RADS. The results indicated that the two methods may have complementary effects in the differential diagnosis of thyroid nodules.
In our study, there were eight thyroid nodules coexisting with Hashimotoʼs thyroiditis in our study, which were all accurately diagnosed by CEUS and partly misdiagnosed by TI-RADS. The result was consistent with that of Zhao et al. [13]. The result indicated that CEUS is also effective in the diagnosis of malignant thyroid nodules coexisting with Hashimotoʼs thyroiditis and can improve the diagnostic accuracy. Of five inflammatory lesions, three nodules showed low-enhancement mode and were misdiagnosed. It indicated that CEUS may not be able to provide more valuable information for inflammatory lesions, and further studies with greater sample size are required to validate the study results.
To increase the accuracy and reduce misdiagnoses as well as missed diagnoses, we have combined CEUS with TI-RADS to identify the benignity and malignancy of thyroid nodules. Significant differences were observed when the combined method was compared with CEUS alone or TI-RADS alone, suggesting that a combined method can significantly increase the accuracy of qualitative diagnoses of thyroid nodules and effectively lower the misdiagnosis rate and missed diagnosis rate. In the present study, we combined CEUS with TI-RADS for further diagnosis analyses and found that nodules with TI-RADS scores of 2, 4 and 5 did not present significant differences (P > 0.05) when using the combined diagnosis, whereas nodules with TI-RADS scores of 4a and 4b presented improved diagnoses by a combination of both methods. Among the 56 4a-nodules, 55 were accurately diagnosed, and among the 52 4b-nodules, 44 were accurately diagnosed. These results indicate that a combination of both methods primarily improved the identification and diagnosis of scores 4a and 4b, which are difficult to identify by TI-RADS alone, and it avoids the errors produced by TI-RADS alone. Thus, we suggest that for thyroid nodules, particularly for nodules with a TI-RADS score of 4a and 4b, a combination of both methods should be used for further analysis.
At logistic regression analysis of 4a and 4b thyroid nodules, the following features showed an association with malignancy: solid component, marked hypoechogenicity, irregular margins, microcalcifications, taller than wide shape and low enhancement. These results were consistent with those of Hyobin et al. [14]. It further confirmed that the above features are effective in the diagnosis of malignant thyroid nodules. To use TI-RADS and CEUS on a regular basis in clinical routine it is important that it is highly reliable. The inter-examiner measurement agreement for TI-RADS and CEUS had a high positive correlation even between experienced and inexperienced examiners (k = 0.885, k = 0.990, respectively). It indicated that TI-RADS descriptors and CEUS mode are simple, objective and are less influenced by US physicians’ experience.
Although a combination of both methods presents significant improvements in diagnostic accuracy, 15 nodules were still misdiagnosed, which may have been caused by the following: (1) certain benign nodules may have fibroplasias during hyperplasia and form calcified fibrous septa and calcified nodule walls, thereby affecting the interpretation of CEUS images; (2) the contrast enhancement modes of certain benign and malignant nodules in scores 4a and 4b could have overlapped; (3) two malignant nodules that were diagnosed as benign nodules were the nodular goitres with complications from local papillary carcinoma and from local follicular cancer; this local carcinoma increased the difficulty of providing a correct diagnosis; (4) the pathological results of the two misdiagnosed TI-RADS score-5 nodules were inflammatory lesions, and conventional US and CEUS results for such lesions are similar to malignant nodules, thereby increasing the difficulty of providing a correct diagnosis.
The present study included the following limitations. (1) Most of the malignant nodules were papillary carcinomas, whereas most of the benign nodules were nodular goitres, and fewer additional pathological types were analysed. Therefore, the present study mainly confirms the diagnostic value of TI-RADS and CEUS for papillary carcinoma and nodular goitre, whereas the diagnostic value of these methods for other benign and malignant thyroid pathological types requires further investigation. (2) The present study represents a single thyroid clinic’s work; thus, results have to be confirmed with multi-centre studies and a large sample size.
In summary, CEUS and TI-RADS showed similar accuracy in the identification of benign and malignant thyroid nodules. The improved TI-RADS combined with CEUS can significantly increase the diagnostic accuracy for the qualitative identification of thyroid nodules, particularly for TI-RADS score 4a and 4b lesions, and if these findings can be replicated, then it may be possible to reduce the number of patients subjected to FNAB or short-term follow-up for benign-appearing solid thyroid nodules.
Abbreviations
- TI-RADS:
-
thyroid imaging reporting and data system
- BI-RADS:
-
breast imaging reporting and data system
- CEUS:
-
contrast-enhanced ultrasound
- CPS:
-
contrast pulsed sequences
- FNAB:
-
fine-needle aspiration biopsy
References
Moon WJ, Baek JH, Junget SL et al (2011) Ultrasonography and the ultrasound-based management of thyroid nodules: consensus statement and recommendations. Korean J Radiol 12:1–14
Park JY, Lee HJ, Jang HW et al (2009) A proposal for a thyroid imaging reporting and data system for ultrasound features of thyroid carcinoma. Thyroid 19:1258–1264
Horvath E, Majlis S, Rossi R et al (2009) An ultrasonogram reporting system for thyroid nodules stratifying cancer risk for clinical management. J Clin Endocrinol Metab 94:1748–1751
Kwak JY, Han KH, Yoon JH et al (2011) Thyroid imaging reporting and data system for US features of nodules: a step in establishing better stratification of cancer risk. Radiology 260:892–899
Yuan Z, Quan J, Yunxiao Z et al (2015) Contrast enhanced ultrasound in the diagnosis of solitary thyroid nodules. J Can Res Ther 11:41–45
Nemec U, Nemec SF, Novotny C et al (2012) Quantitative evaluation of contrast-enhanced ultrasound after intravenous administration of a microbubble contrast agent for differentiation of benign and malignant thyroid nodules: assessment of diagnostic accuracy. Eur Radiol 22:1357–1365
Deng J, Zhou P, Tian SM et al (2014) Comparison of diagnostic efficacy of contrast-enhanced ultrasound, acoustic radiation force impulse imaging, and their combined use in differentiating focal solid thyroid nodules. PLoS One 9:e90674
Cantisani V, Consorti F, Guerrisi A et al (2013) Prospective comparative evaluation of quantitative-elastosonography (Q-elastography) and contrast-enhanced ultrasound for the evaluation of thyroid nodules: Preliminary experience. Eur J Radiol 82:1892–1898
Li FS, Luo HT (2013) Comparative study of thyroid puncture biopsy guided by contrast- enhanced ultrasonography and conventional ultrasound. Exp Ther Med 5:1381–1384
Giusti M, Orlandi D, Melle G et al (2013) Is there a real diagnostic impact of elastosonography and contrast-enhanced ultrasonography in the management of thyroid nodules. J Zhejiang Univ Sci B 14:195–206
Russ G, Bigorgne C, Royer B et al (2011) The Thyroid Imaging Reporting and Data System (TIRADS) for ultrasound of the thyroid. J Radiol 92:701–713
Friedrich-Rust M, Sperber A, Holzer K et al (2010) Real-time elastography and contrast-enhanced ultrasound for the assessment of thyroid nodules. Exp Clin Endocrinol Diabetes 118:602–609
Zhao RN, Zhang B, Yang X et al (2015) Diagnostic value of contrast-enhanced ultrasound of thyroid nodules coexisting with Hashimotoʼs thyroiditis. Zhongguo Yi Xue Ke Xue Yuan Xue Bao 37:66–70
Seo H, Na DG, Kim J-H et al (2015) Ultrasound-based risk stratification for malignancy in thyroid nodules: a four-tier categorization system. Eur Radiol 25:2153–2162
Acknowledgements
The scientific guarantor of this publication is Zhou Ping. The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. All the authors were involved in writing the manuscript. Yan Zhang did the first draft. Ping Zhou provided instructive advice and useful suggestions for this manuscript. Shuang-ming Tian and Yong-feng Zhao provided statistical advice for this manuscript. Jia-le Li and Lan Li contributed to the figure and the review. No complex statistical methods were necessary for this paper. Institutional Review Board approval was obtained. Written informed consent was obtained from all subjects (patients) in this study. No study subjects or cohorts have been previously reported. Methodology: prospective/retrospective.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License (http://creativecommons.org/licenses/by/4.0/), which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made.
About this article
Cite this article
Zhang, Y., Zhou, P., Tian, SM. et al. Usefulness of combined use of contrast-enhanced ultrasound and TI-RADS classification for the differentiation of benign from malignant lesions of thyroid nodules. Eur Radiol 27, 1527–1536 (2017). https://doi.org/10.1007/s00330-016-4508-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-016-4508-y