Abstract
Objectives
The aim of this study was to determine whether diffusion and perfusion imaging parameters demonstrate different diagnostic values for predicting pseudoprogression between glioblastoma subgroups stratified by O6-mythylguanine-DNA methyltransferase (MGMT) promoter methylation status.
Methods
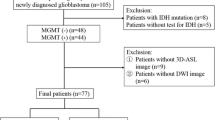
We enrolled seventy-five glioblastoma patients that had presented with enlarged contrast-enhanced lesions on magnetic resonance imaging (MRI) one month after completing concurrent chemoradiotherapy and undergoing MGMT promoter methylation testing. The imaging parameters included 10 or 90 % histogram cutoffs of apparent diffusion coefficient (ADC10), normalized cerebral blood volume (nCBV90), and initial area under the time signal-intensity curve (IAUC90). The results of the areas under the receiver operating characteristic curve (AUCs) with cross-validation were compared between MGMT methylation and unmethylation groups.
Results
MR imaging parameters demonstrated a trend toward higher accuracy in the MGMT promoter methylation group than in the unmethylation group (cross-validated AUCs = 0.70–0.95 and 0.56–0.87, respectively). The combination of MGMT methylation status with imaging parameters improved the AUCs from 0.70 to 0.75–0.90 for both readers in comparison with MGMT methylation status alone. The probability of pseudoprogression was highest (95.7 %) when nCBV90 was below 4.02 in the MGMT promoter methylation group.
Conclusions
MR imaging parameters could be stronger predictors of pseudoprogression in glioblastoma patients with the methylated MGMT promoter than in patients with the unmethylated MGMT promoter.
Key Points
• The glioblastoma subgroup was stratified according to MGMT promoter methylation status.
• Diagnostic values of diffusion and perfusion parameters for predicting pseudoprogression were compared.
• Imaging parameters showed higher diagnostic accuracy in the MGMT promoter methylation group.
• Imaging parameters were independent to MGMT promoter methylation status for predicting pseudoprogression.
• Imaging biomarkers might demonstrate different diagnostic values according to MGMT promoter methylation.






Similar content being viewed by others
Abbreviations
- CCRT:
-
Concurrent chemoradiotherapy
- MR:
-
Magnetic resonance
- CBV:
-
Cerebral blood volume
- ADC:
-
Apparent diffusion coefficient
- MGMT:
-
O6-mythylguanine-DNA methyltransferase
- DWI:
-
Diffusion-weighted imaging
- DSC:
-
Dynamic susceptibility contrast-enhanced
- DCE:
-
Dynamic contrast-enhanced
- IAUC:
-
Initial area under the time–signal intensity curve
- ROC:
-
Receiver operating characteristic
References
Wen PY, Macdonald DR, Reardon DA et al (2010) Updated response assessment criteria for high-grade gliomas: response assessment in neuro-oncology working group. J Clin Oncol 28:1963–1972
Brandes AA, Rigon A, Zampieri P et al (1998) Carboplatin and teniposide concurrent with radiotherapy in patients with glioblastoma multiforme: a phase II study. Cancer 82:355–361
Kong DS, Kim ST, Kim EH et al (2011) Diagnostic dilemma of pseudoprogression in the treatment of newly diagnosed glioblastomas: the role of assessing relative cerebral blood flow volume and oxygen-6-methylguanine-DNA methyltransferase promoter methylation status. AJNR Am J Neuroradiol 32:382–387
Catalaa I, Henry R, Dillon WP et al (2006) Perfusion, diffusion and spectroscopy values in newly diagnosed cerebral gliomas. NMR Biomed 19:463–475
Castillo M, Smith JK, Kwock L, Wilber K (2001) Apparent diffusion coefficients in the evaluation of high-grade cerebral gliomas. AJNR Am J Neuroradiol 22:60–64
Pope WB, Kim HJ, Huo J et al (2009) Recurrent glioblastoma multiforme: ADC histogram analysis predicts response to bevacizumab treatment. Radiology 252:182–189
Pope WB, Lai A, Mehta R et al (2011) Apparent diffusion coefficient histogram analysis stratifies progression-free survival in newly diagnosed bevacizumab-treated glioblastoma. AJNR Am J Neuroradiol 32:882–889
Brandes AA, Franceschi E, Tosoni A et al (2008) MGMT promoter methylation status can predict the incidence and outcome of pseudoprogression after concomitant radiochemotherapy in newly diagnosed glioblastoma patients. J Clin Oncol 26:2192–2197
Brandes AA, Tosoni A, Franceschi E et al (2009) Recurrence pattern after temozolomide concomitant with and adjuvant to radiotherapy in newly diagnosed patients with glioblastoma: correlation With MGMT promoter methylation status. J Clin Oncol 27:1275–1279
Weller M, Tabatabai G, Kastner B et al (2015) MGMT promoter methylation is a strong prognostic biomarker for benefit from dose-intensified temozolomide rechallenge in progressive glioblastoma: the DIRECTOR trial. Clin Cancer Res 21:2057–2064
Drabycz S, Roldan G, de Robles P et al (2010) An analysis of image texture, tumor location, and MGMT promoter methylation in glioblastoma using magnetic resonance imaging. NeuroImage 49:1398–1405
Park JE, Kim HS, Goh MJ, Kim SJ, Kim JH (2015) Pseudoprogression in patients with glioblastoma: assessment by using volume-weighted voxel-based multiparametric clustering of MR imaging data in an independent test set. Radiology 275:792–802
Esteller M, Garcia-Foncillas J, Andion E et al (2000) Inactivation of the DNA-repair gene MGMT and the clinical response of gliomas to alkylating agents. N Engl J Med 343:1350–1354
Esteller M, Hamilton SR, Burger PC, Baylin SB, Herman JG (1999) Inactivation of the DNA repair gene O6-methylguanine-DNA methyltransferase by promoter hypermethylation is a common event in primary human neoplasia. Cancer Res 59:793–797
Evelhoch JL, LoRusso PM, He Z et al (2004) Magnetic resonance imaging measurements of the response of murine and human tumors to the vascular-targeting agent ZD6126. Clin Cancer Res 10:3650–3657
Kim HS, Goh MJ, Kim N, Choi CG, Kim SJ, Kim JH (2014) Which combination of MR imaging modalities is best for predicting recurrent glioblastoma? Study of diagnostic accuracy and reproducibility. Radiology 273:831–843
Youden WJ (1950) Index for rating diagnostic tests. Cancer 3:32–35
Wong AJ, Bigner SH, Bigner DD, Kinzler KW, Hamilton SR, Vogelstein B (1987) Increased expression of the epidermal growth factor receptor gene in malignant gliomas is invariably associated with gene amplification. Proc Natl Acad Sci U S A 84:6899–6903
Moon WJ, Choi JW, Roh HG, Lim SD, Koh YC (2012) Imaging parameters of high grade gliomas in relation to the MGMT promoter methylation status: the CT, diffusion tensor imaging, and perfusion MR imaging. Neuroradiology 54:555–563
Chahal M, Xu Y, Lesniak D et al (2010) MGMT modulates glioblastoma angiogenesis and response to the tyrosine kinase inhibitor sunitinib. Neuro-Oncology 12:822–833
Acknowledgments
The scientific guarantor of this publication is Prof. Sang Joon Kim. This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education, Science and Technology (grant number: NRF-2014R1A2A2A01004937). The Institutional Review Board approved our human study (The Institutional Review Board of Asan Medical Center [http://eirb.amc.seoul.kr]: S2014-2090-0001). Written informed consent was waived by the Institutional Review Board. Methodology: retrospective, diagnostic or prognostic study, performed at one institution. The authors thank the Biomedical Imaging Infrastructure, Department of Radiology, Asan Medical Center for the technical support of image processing. Some subjects or cohorts have been previously reported in Park JE, Kim HS, Goh MJ, Kim SJ, Kim JH. Pseudoprogression in patients with glioblastoma: assessment by using volume-weighted voxel-based multiparametric clustering of MR imaging data in an independent test set. Radiology 2015 Jun;275(3):792–802).
Author information
Authors and Affiliations
Corresponding author
Additional information
Ra Gyoung Yoon and Wooyul Paik contributed equally to this work.
Rights and permissions
About this article
Cite this article
Yoon, R.G., Kim, H.S., Paik, W. et al. Different diagnostic values of imaging parameters to predict pseudoprogression in glioblastoma subgroups stratified by MGMT promoter methylation. Eur Radiol 27, 255–266 (2017). https://doi.org/10.1007/s00330-016-4346-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-016-4346-y