Abstract
Objectives
To evaluate the impact of slice-encoding for metal artefact correction (SEMAC) on image quality, findings, and therapy decision in patients with unicompartmental knee arthroplasty (UKA).
Methods
Forty-five painful UKAs were examined at 1.5T-MRI (STIR, proton-density(PD)-weighted sequence, each with SEMAC and high-bandwidth). Artefact size, image quality, anatomic depiction, and clinically relevant findings were compared between SEMAC and high-bandwidth (2 readers). In 30 patients, therapy decision was retrospectively assessed by two orthopaedic surgeons without MRI, with high-bandwidth-MRI, and with SEMAC-MRI.
Results
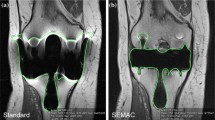
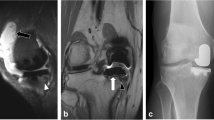
SEMAC reduced mean artefact size for STIR (11.8 cm2 vs. 37.7 cm2) and PD (16.8 cm2 vs. 18.9 cm2), p < 0.0005 for both comparisons. SEMAC showed more blurring than high-bandwidth, p < 0.0005. STIR-SEMAC revealed more bone marrow oedema (29 vs. 18 patients, p = 0.001, 30 vs. 13 patients, p < 0.0005, for reader 1 and 2 respectively). PD-SEMAC was worse in detecting meniscal lesions (6 missed, p = 0.031, 9 missed, p = 0.004, by reader 1 and 2 respectively) than PD-high-bandwidth. Revision-surgery was chosen in 12 and 11 patients without MRI (surgeon 1 and 2), with high-bandwidth-MRI in 15 and 14 patients, and with SEMAC-MRI in 19 and 14 patients.
Conclusions
STIR-SEMAC was useful in detecting bone marrow oedema and influenced the orthopaedic surgeons’ decisions towards surgery, while PD-SEMAC showed no clinical benefit.
Key Points
• Slice-encoding for metal artefact correction (SEMAC) MRI reduces metal-induced artefact size.
• STIR SEMAC detects more bone marrow oedema in painful unicompartmental knee arthroplasty.
• STIR SEMAC can help the orthopaedic surgeon with decision making.
• PD SEMAC suffers from blurring of images, potentially masking relevant meniscal lesions.
• PD SEMAC does not improve cartilage lesion detection in the non-operated compartments.





Similar content being viewed by others
Abbreviations
- SEMAC:
-
Slice-encoding for metal artefact correction
- hiBW:
-
High bandwidth
References
Nguyen US, Zhang Y, Zhu Y, Niu J, Zhang B, Felson DT (2011) Increasing prevalence of knee pain and symptomatic knee osteoarthritis: survey and cohort data. Ann Intern Med 155:725–732
Murphy L, Schwartz TA, Helmick CG et al (2008) Lifetime risk of symptomatic knee osteoarthritis. Arthritis Rheum 59:1207–1213
Beard DJ, Holt MD, Mullins MM, Malek S, Massa E, Price AJ (2012) Decision making for knee replacement: variation in treatment choice for late stage medial compartment osteoarthritis. Knee 19:886–889
Niinimaki T, Eskelinen A, Makela K, Ohtonen P, Puhto AP, Remes V (2014) Unicompartmental knee arthroplasty survivorship is lower than TKA survivorship: a 27-year Finnish Registry Study. Clin Orthop Relat Res 472:1496–1501
Baker PN, Petheram T, Avery PJ, Gregg PJ, Deehan DJ (2012) Revision for unexplained pain following unicompartmental and total knee replacement. J Bone Joint Surg Am 94:e126
Sutter R, Hodek R, Fucentese SF, Nittka M, Pfirrmann CW (2013) Total knee arthroplasty MRI featuring slice-encoding for metal artifact correction: reduction of artifacts for STIR and proton density-weighted sequences. AJR Am J Roentgenol 201:1315–1324
Aliprandi A, Sconfienza LM, Randelli P et al (2011) Magnetic resonance imaging of the knee after medial unicompartmental arthroplasty. Eur J Radiol 80:e416–e421
Aliprandi A, Perona F, Bandirali M, Randelli P, Cabitza P, Sardanelli F (2009) MR imaging of the knee in patients with medial unicompartmental arthroplasty: comparison among sequences at 1.5 T. Radiol Med 114:301–311
Heyse TJ, Figiel J, Hahnlein U et al (2012) MRI after unicondylar knee arthroplasty: the preserved compartments. Knee 19:923–926
Chen CA, Chen W, Goodman SB et al (2011) New MR imaging methods for metallic implants in the knee: artifact correction and clinical impact. J Magn Reson Imaging 33:1121–1127
Ai T, Padua A, Goerner F et al (2012) SEMAC-VAT and MSVAT-SPACE sequence strategies for metal artifact reduction in 1.5T magnetic resonance imaging. Investig Radiol 47:267–276
Sutter R, Ulbrich EJ, Jellus V, Nittka M, Pfirrmann CW (2012) Reduction of metal artifacts in patients with total hip arthroplasty with slice-encoding metal artifact correction and view-angle tilting MR imaging. Radiology 265:204–214
Butts K, Pauly JM, Gold GE (2005) Reduction of blurring in view angle tilting MRI. Magn Reson Med 53:418–424
Lu W, Pauly KB, Gold GE, Pauly JM, Hargreaves BA (2009) SEMAC: slice encoding for metal artifact correction in MRI. Magn Reson Med 62:66–76
Felson DT, Chaisson CE, Hill CL et al (2001) The association of bone marrow lesions with pain in knee osteoarthritis. Ann Intern Med 134:541–549
Acknowledgements
The scientific guarantor of this publication is Christoph Agten. The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article. The authors state that this work has not received any funding. No complex statistical methods were necessary for this paper. Institutional Review Board issued a waiver. Written informed consent was obtained from all patients in this study. Methodology: prospective, performed at one institution.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Agten, C.A., Del Grande, F., Fucentese, S.F. et al. Unicompartmental knee arthroplasty MRI: impact of slice-encoding for metal artefact correction MRI on image quality, findings and therapy decision. Eur Radiol 25, 2184–2193 (2015). https://doi.org/10.1007/s00330-015-3596-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-015-3596-4