Abstract
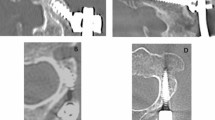
The purpose of this study was to investigate the temporal evolution of type-1 end-plate changes on MRI in patients with degenerative disease of the lumbar spine and to evaluate whether any correlation exists between such evolution and the change in patients’ symptoms. Forty-four patients with 48 Modic type-1 end-plate changes (low TI signal and high T2 signal) were studied. All patients had an initial and a follow-up non-contrast lumbar MRI with variable intervals between the studies (12–72 months). Severity of the end-plate changes was assessed by eyeball estimation. Correlation with patients’ symptoms was studied with the help of the Visual Analogue Score (VAS), Oswestry Questionnaire Score (OQS) and patients’ subjective assessment. Of the 48 disc levels with type-1 changes, 18 (37.5%) converted fully to type 2 (high T1 signal and intermediate to high T2 signal), 7 (14.6%) partially converted to type 2, 19 (39.6%) became worse (i.e. type 1 changes became more extensive) and 4 (8.3%) showed no change. Higher average VAS (5.7) and OQS (42.3) scores were noted in patients where there was worsening type-1 change and lower scores (3.8 and 27, respectively) were seen in those where there was conversion to type-2 change. These trends, however, did not reach statistical significance (P values 0.16 and 0.09 for VAS and OQS, respectively). The statistical relationship was stronger after exclusion of patients with confounding factors (i.e. changes in lumbar MRI other than end-plate changes that could independently explain the evolution of patients’ symptoms) with P-values of 0.08 and 0.07 for VAS and OQS, respectively. Type-1 end-plate change represents a dynamic process and in a large majority of cases either converts to type-2 change or becomes more extensive. The evolution of type-1 change relates to change in patient’s symptoms, but not to a statistically significant level.



Similar content being viewed by others
References
De Roos D, Kressel H, Spritzer C, Dalinka M (1987) MR imaging of marrow changes adjacent to end-plates in degenerative lumbar disk disease. Am J Roentgenol 149:531–534
Modic M, Steinberg P, Ross J, Masaryk T, Carter J (1988) Degenerative disk disease: assessment of changes in vertebral body marrow with MR imaging. Radiology 166:193–199
Modic M, Masaryk T, Ross J, Carter J (1988) Imaging of degenerative disk disease. Radiology 168:177–186
Toyone T, Takahashi K, Kitahara H, Yamagata M, Murakami M, Moriya H (1994) Vertebral bone marrow changes in degenerative lumbar disc disease. J Bone Joint Surg 76B:757–764
McCall IW, Cassar-Pullicino VN, Tyrrell PN (1998) MR vertebral changes and back pain. Abstracts presented at the 25th annual meeting of the International Society for the Study of the Lumbar Spine, Singapore
Braithwaite I, White J, Saifuddin A, Renton P, Taylor B (1998) Vertebral end-plate (Modic) changes on lumbar spine MRI: correlation with pain reproduction at lumbar discography. Eur Spine J 7:363–368
Weishaupt D, Zanetti M, Hodler J, Min K, Fuchs B, Pfirrmann C, Boos (2001) Painful lumbar disk derangement: relevance of endplate abnormalities at MR imaging. Radiology 218:420–427
Fairbank J, Couper J, Davies J et al (1980) The Oswestry low back pain questionnaire. Physiotherapy 66:271–273
Weishaupt D, Zannetti M, Hodler J, Boos N (1998) MR imaging of the lumbar spine: prevalence of intervertebral disc extrusion and sequestration, nerve root compression, end-plate abnormalities, and osteoarthritis of the facet joints in asymptomatic volunteers. Radiology 209:661–666
Crock H (1986) Internal disc disruption. A challenge to disc prolapse fifty years on. Spine 11:650–653
Bram J, Zanetti M, Min K, Hodler J (1998) MR abnormalities of the intervertebral disks and adjacent bone marrow as predictors of segmental instability of the lumbar spine. Acta Radiol 39:18–23
Lang P, Chafetz N, Genant HK, Morris JM (1990) Lumbar spinal fusion. Assessment of functional stability with MRI. Spine 21:79
Kang JD, Giorgescu HI, McIntyre-Larkin L, Stefanovic-Racic M, Donaldson WF, Evans CH (1996) Herniated lumbar intervertebral discs spontaneously produce matrix metalloproteinases, nitric acid, interleukin-6 and prostaglandin E2. Spine 21:271–277
Specchia N, Pagnotta A, Toesca A, Greco F (2002) Cytokines and growth factors in the protruded intervertebral disc of the lumbar spine. Eur Spine J 11:145–151
Nygaard OP, Mellgre SI, Osterud B (1997) The inflammatory properties of contained and non-contained lumbar disc herniation. Spine 22:2484–2488
Takahashi H, Suguro T, Okazima Y, Motegi M, Okada Y, Kakiuchi T (1996) Inflammatory cytokines in herniated disc of the lumbar spine. Spine 21:218–224
Burke JG, Watson RWG, McCormack D, Dowling FE, Walsh MG, Fitzpatrick JM (2002) Intervertebral discs which cause low back pain secrete high levels of proinflammatory mediators. J Bone Joint Surg 84B:196–201
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Mitra, D., Cassar-Pullicino, V.N. & Mccall, I.W. Longitudinal study of vertebral type-1 end-plate changes on MR of the lumbar spine. Eur Radiol 14, 1574–1581 (2004). https://doi.org/10.1007/s00330-004-2314-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-004-2314-4