Abstract
We aimed to bring a more understandable and applicable technique to the literature instead of “massage therapy” in CTS. We compared our new technique with the splint wear, of which the efficacy in CTS has been proven with many studies. Eighty-four patients between 31 and 65 years of age were included in the study. The patients were divided into two equal groups. In the first group, splint and “Madenci” hand massage technique were applied, and in the second group only splint was applied. A splint was provided for all patients with tendon and nerve gliding exercises, and also when needed analgesic drugs were given. When the pretreatment and posttreatment parameters were compared via repetitive measurement analysis, it was found that PGA and MDPGA were significantly decreased in both groups (P = 0.001), whereas grip strength was significantly increased (P = 0.001). While no statistically significant difference was found between the groups regarding pretreatment values (P > 0.05), the posttreatment PGA, MDPGA, and grip strength scores were significantly improved in Group I compared to Group II (P < 0.05). To the best our knowledge, the present study is the first and largest study in the literature conducted on the massage technique that will contribute to the treatment of CTS. As this new massage technique is easy for self-application, cheap, and practical, every patient with CTS can apply the massage to him/herself easily.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Carpal tunnel syndrome (CTS) is the most commonly encountered peripheral neuropathy of the entrapment neuropathy group [1]. CTS are defined as the signs and symptoms that appear due to compression of median nerve within the carpal tunnel [2]. In the previous studies, CTS prevalence has been reported between 0.1 and 0.5% in the general population [3].
The primary step in the treatment of CTS, which is prevalent among the population and negatively affect the daily activities of the individuals, should be the identification of the etiological factor, if any, and accordingly deciding on conservative and/or surgical management. The diagnosis of CTS is based on the anamnesis, clinical symptoms, physical examination findings, and as well as electroneurophysiological verification of these findings [4].
Conservative treatment of CTS includes splint wear, steroid injection, non-steroidal anti-inflammatory drugs, diuretics, vitamin B6, physical therapy agents, activity modifications, and job change [5]. The superiority of these methods over each other is controversial. Moreover, there are studies reporting that alternative therapies such as exercise and yoga programs, low-level laser therapy, acupuncture, and massage therapy alleviate the symptoms in the patients with CTS [6–8]. It is known that massage therapy reduces pain, particularly in certain pain syndromes result from local sympathetic activation, by means of decreasing the sympathetic activity or increasing the serotonin level and vagal activity [8, 9].
There are limited numbers of studies showing that the massage therapy remarkably alleviates the symptoms in the patients with CTS, and leads to an improvement in anxiety and depression scores [8, 9]. However, in these studies there is no consensus or a complete explanation about the massage methods, longer duration of application, and the use of all massage modalities. While we were planning the present study, we intended to standardize the massage therapy that would be applied to the patients with CTS. We thought that if this therapy method has a standardized name, it would be easier to apply. In brief, we aimed to bring a more understandable and applicable technique to the literature instead of “massage therapy” in CTS. We compared our new technique with the splint wear, of which the efficacy in CTS has been proven with many studies. We aimed to show the applicability of this technique by means of analyzing the effects of the results on the symptoms and functional capacity of hand, as well as on the electroneurophysiological parameters.
Materials and methods
Patients
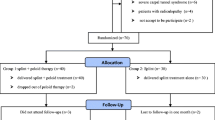
Eighty-four patients between 31 and 65 years of age were included in the study that were admitted to the Physical Therapy and Rehabilitation Department of the Medical School of Gaziantep University between 2009 and 2010 and diagnosed with CTS. The patients were divided into two equal groups. Group I was determined as “splint + massage group” and Group II was determined as “splint group.” Massage, as we called “Madenci” hand massage technique (MHMT), was applied.
Both group I and group II were received tendon and nerve gliding exercises, and also when needed analgesic drugs were given. Among the patients, two patients from group I and two patients from the group II were excluded from the study because of poor compliance with the therapy and follow-up visits. Thus, the study population comprised 80 patients (76 women, 4 men, 151 hands, 71 bilateral). Forty patients were included group I, and 40 patients were included group II.
Approval of the ethical committee was obtained prior to the study. The present study was designed as prospective randomized controlled study.
Inclusion criteria:
-
Pain, paresthesia, and/or vasomotor symptoms in the hand in the area of median nerve distribution,
-
Symptom duration longer than 6 weeks,
-
The positivity of at least one of the following tests on the physical examination: Tinel, Phalen, Buda, and Carpal compression tests,
-
Having median motor distal latency (mMDL) >4.2 ms and median sensory nerve conduction velocity (mSNCV) <42 m/s or having peak latency difference of >0.5 ms between the median and ulnar nerves in the same hand,
-
Absence of predisposing etiologic factors in CTS (such as diabetes mellitus, hypothyroidism, hyperthyroidism, acute trauma, rheumatologic diseases, pregnancy),
-
The elimination of conditions such as cervical radiculopathy or polyneuropathy that should be considered in the differential diagnosis of CTS
-
Absence of thenar atrophy or weakness of the thenar muscle,
-
Absence of medical therapy such as oral steroid or non-steroidal anti-inflammatory drug or being not included in a physical therapy program within a previous month,
-
Not being applied steroid injection within the previous 3 months,
-
Absence of any serious health problem that would prevent the application of electrophysiological tests,
-
Absence of medical problems contraindicated for massage therapy.
Pretreatment evaluation
All the patients underwent locomotor system examination prior to the treatment by the same physician. Physical examination included Spurling test, Adson test, median and ulnar Tinel tests, Phalen test, and Carpal compression test. Motor and sensory examination was performed and deep tendon reflexes, as well as pathologic reflexes, were evaluated. Additionally, routine blood tests were performed. Patients were questioned in terms of the symptoms including pain, paresthesia, vasomotor symptoms, and loss of strength. Questioning for vasomotor symptoms included hyperemia in the hands and fingers, sweating or dry skin (xerosis), and bruising on the tip of the fingers with cold. Vasomotor symptom was considered positive in the presence of at least one of these symptoms. The symptoms and the physical examination findings of the patients were recorded.
The level of pain in all patients was questioned via the Patient Global Assessment (PGA, 0–10 cm) and the Physician Global Assessment (MDPGA, 0–10 cm). Hand grip strength was measured by Jamar Hand Dynamometer (Sammons Preston Inc., Bolingbrook, IL, USA). Electrophysiological examination included mMDL, median motor nerve conduction velocity (mMNCV), and mSNCV.
All the patients were informed about the study and their consents were obtained. All the parameters were re-evaluated at the sixth week of the study.
Therapies
The patients were randomly divided into two equal groups. Simple randomization was performed by a different physician according to the hospital admission order of the patients. Both hands of the patients with bilateral CTS were included in the same group; however, evaluations were performed separately for each hand.
Splint therapy
All the patients were asked to wear wrist-hand resting splint during night sleep for 6 months. Wrist-hand resting splints made up of elastic cotton fabric with Velcro bandage on the dorsal side and supported by aluminum bar were provided to the symptomatic hands of the patients to keep wrist at in the neutral position during 0–15° extension. The splint has been designed to cover the proximal half of the palmar area and distal one-third of the forearm by allowing movement of the metacarpophalangeal joints in all directions (Fig. 1).
Massage therapy
Wrist-hand resting splint to wear at night and additionally MHMT were applied to the group I of patients for 6 weeks. The massage therapy was taught to the patients practically on the first day of their therapy from an experienced physical therapy and rehabilitation physician. On the other days, patients were asked to do the massage by themselves. Furthermore, in case they forgot, in order to remember the massage technique, a CD (compact disk) including visual clip of training was given to the patients. The patients were asked to attend the weekly follow-up visits. The patients who could not attend the follow-up visits were phoned and provided to do the massage completely. Those who attended the follow-up visits were asked to do the massage themselves under physician supervision. They were instantly intervened to correct their mistakes, if any. The patients maintained their therapies under specialist supervision.
“Madenci” hand massage technique (MHMT): The characteristics of this technique are as follows: can be applied by the patient him/herself, easy, can be improved according to the patient, and is therapeutic. Treatment primarily depends on the principal of patient’s learning how to do self-massage under the physician supervision. It is possible to support the training either via face-to-face interview, or by telephone, or via education tools (CD, DVD).
MHMT begins with 30-s effleurage, continues with 60-s friction, 30-s petrissage, 30-s shaking, and ends with 30-s effleurage. It takes totally 3 min. This method provides rapid and effective approach to the hand and forearm tissues. It includes massage modalities consisted of effleurage, friction, petrissage, and shaking. Effleurage manipulation has muscle-relaxing effect and sedation effect on nerves [10]. Friction manipulation accelerates the return flow with the pressure in the direction of lymphatic and venous drainage, thus, relieves the edema in the tissues with venous and lymphatic stasis, and plays a role in the treatment of the scar tissues and adhesions as well [10]. Petrissage manipulation causes the metabolic residues, which accumulate in the tired and atrophic muscles and under the skin as well, to join the circulation and improves the tonus and elasticity by means of preventing atrophy [10]. Shaking manipulation has pain-relieving effect and strengthens the atonic muscles [10]. Patient applies these manipulations him/herself; the physician acts only as a trainer (Fig. 2).
Application of “Madenci” hand massage technique manipulations: Effleurage: Thirty seconds, scrubbing the surface, from distal to proximal, on forearm. Friction: Sixty seconds, stroking deep tissues, from distal to proximal, clock wise, on solar surface. Petrissage: Thirty seconds, scouring depths, from distal to proximal, on forearm. Shaking: Thirty seconds. Effleurage: Thirty seconds, scrubbing the surface, from distal to proximal, on forearm
Tendon gliding exercises
All the patients trained about tendon and nerve gliding exercises by the same physiotherapist on the first day of diagnosis, and they were recommended to perform these exercises at home. It was performed in the way that the fingers would be in five positions; straight, hook, fist, tabletop, and straight fist [11] (Fig. 3).
Tendon gliding exercises [11]
Nerve gliding exercises
The mobilization of median nerve was enabled performing the exercise in a way that the hand and the wrist would be in six different positions:
-
1.
The wrist is in neutral position, fingers and thumb are in flexion
-
2.
The wrist is in neutral position, fingers and thumb are in extension
-
3.
The wrist and fingers are in extension, thumb is in neutral position
-
4.
The wrist, fingers, and thumb are in extension
-
5.
Same as in position 4, but forearm is in supination
-
6.
Same as in position 5, but gently stretching the thumb with the other hand (Fig. 4).
Fig. 4 Median nerve gliding exercises [11]
During these exercises, the neck and shoulder were in neutral position, and the elbow was in 90° flexion and supination. The patients were asked to do the each position for a 5 s, and repeat each position 10 times for at least three times a day.
Medical treatment
In the course of the study, the patients were allowed to use paracetamol (1 g/day) in case of pain, except for the days of evaluation.
Parameters used in the study
-
1.
Electroneurophysiological examinations; mMDL, mMNCV, mSNCV
-
2.
Evaluation of pain; PGA and MDPGA
-
3.
Evaluation of strength; Hand grip strength
-
4.
Boston symptom severity scale and the functional capacity scale.
Electroneurophysiological examinations
All of the patients presented with typical signs and symptoms of CTS. The patients clinically diagnosed with CTS were electrophysiologically evaluated and the diagnosis was confirmed. All the electrophysiological examinations were performed by the same physician. Prior to the examination, the hands of the patients were prepared by resting the patients for 15 min at a room temperature of 22–24°C. Dantec-Keypoint (Medtronic, Skovlunde, Denmark) electroneurophysiological examination unit was used in the present study.
mMDL: Active recorder electrode was attached to the abductor pollicis brevis muscle, whereas the reference electrode was attached to the distal part of the first finger, and recording was performed with supramaximal stimulation by providing the distance of 8 cm between the stimulator electrode cathode and the active electrode. Patients with a distal latency >4.2 ms were included in the study.
mMNCV: For the motor stimulation, the median nerve was supramaximally stimulated at the stimulation point on the wrist and the recording was performed on the abductor pollicis brevis.
mSNCV: Active and reference electrodes in the shape of ring electrode were placed on the metacarpophalangeal and distal interphalangeal joints of the second finger. Recording was performed with supramaximal stimulation on the wrist by providing the distance of 14 cm between the stimulator electrode and active electrode. Patients with a conduction velocity of <42 m/s were included in the study.
The patient global assessment and the physician global assessment
Level of the pain in the hands and fingers of the patients within the last week was questioned using a visual scale with a length of 0–10 cm. In this scale, “0” indicated no pain and “10” indicated unbearable pain.
Hand grip strength and holding power measurements
Grip strength (in kg) was measured in the symptomatic hand of the patients using Jamar hand dynamometer. All the measurements were preformed when the patient was in a sitting position, shoulder in adduction and neutral rotation, elbow in 90° flexion, forearm in neutral position, wrist in 0° to 30° dorsiflexion and 0° to 15° ulnar flexion. The patients were asked to maintain maximum grip strength. Measurements were repeated for three times and their mean was calculated. During measurement, Jamar dynamometer was hold from the top and the bottom in order to prevent the measurement to be affected by the weight of the device.
All the measurements were evaluated by the same person both before and after the treatment.
Boston symptom severity scale and functional capacity scale
Boston questionnaire: Boston CTS questionnaire, which was developed by Levine et al. in [12], is a self-rating scale and consists of two parts: symptom severity scale and functional capacity scale. As the scale was originated from Boston “Brigham and Women’s” Hospital, it has been presented in the literature as “Boston Carpal Tunnel Questionnaire.”
Boston symptom severity scale: The questionnaire consists of 11 items. Each item is scored between one and five. The average score is obtained by dividing the total score by the number of questions and ranges from one to five. High scores indicate severe symptom.
Boston functional capacity scale: The questionnaire consists of eight items and again each item is scored between one and five. The average score is obtained by dividing the total score by the number of questions and ranges from one to five. High score indicates decreased functional capacity. The average score is calculated both for symptom severity and functional capacity.
Statistical analysis
The statistical analysis of the data was performed by Statistical Package for Social Sciences (SPSS Inc., Chicago, IL, USA) 16.0 for Windows. Student’s t test was used for the intergroup comparison of independent variables, whereas paired t test was used for the time-dependent changes of intragroup variables. For the comparison of the qualitative data (discrete variables) such as symptoms and physical examination findings, the chi-square test was used. The results were presented as mean ± standard deviation, and a P value < 0.05 was considered statistically significant.
Results
There was no statistically significant difference between the two groups in terms of age, gender, body mass index (BMI), and symptom duration (P > 0.05, Table 1).
There was no statistically significant difference between the groups in terms of initial symptoms such as pain, paresthesia, and loss of strength, as well as vasomotor symptoms and physical examination findings including Tinel, Phalen, Buda, and Carpal compression tests (P > 0.05).
When the pretreatment and posttreatment parameters were compared via repetitive measurement analysis, it was found that PGA and MDPGA were significantly decreased in both groups (P = 0.001), whereas grip strength was significantly increased (P = 0.001). While no statistically significant difference was found between the groups regarding pretreatment values (P > 0.05), the posttreatment PGA, MDPGA, and grip strength scores were significantly improved in Group I compared to Group II (P < 0.05, Table 2).
When electrophysiological parameters were compared, no statistically significant difference was found between the groups in terms of pretreatment values of mMDL, mMNCV, and mSNCV (P > 0.05). In Group I, there was a significant decrease in the posttreatment values of mMDL (left) and mMDL (right), whereas a significant increase in mSNCV (P = 0.002, P = 0.005, P = 0.008, respectively, Table 3). However, there was no significant difference in the posttreatment values of Group II. Group I and II were compared in terms of posttreatment values, there were no significant differences found between the groups (P > 0.05, Table 4).
According to the Boston symptom severity scale and functional capacity scale, significant difference was found in both groups in terms of posttreatment values (P = 0.001, Table 5). When the posttreatment values of groups were compared, the difference was more significant in favor of Group I (P = 0.001, Table 5).
Discussion
The mean age of the patients in the present study, as well as the gender distribution and the rate of positivity in the provocative tests, was in consistent with the literature [13]. We believe that the prevalence of CTS is higher among women, because the works such as house cleaning, knitting, and sewing are in their responsibility.
Splint was first used in CTS in 1947 with the study conducted by Roaf [14, 15]. The pressure in the carpal tunnel is the lowest in neutral position and significantly increases when the wrist is in flexion or extension [16]. In the present study, we compared the splint therapy, of which the validity and reliability is well known, with our massage technique. The aim of the present study was to evaluate the efficacy and reliability of this massage technique; meantime, we applied splint and exercise program to all the patients in order to maintain the treatment CTS. However, we presumed that this massage technique would be as simple and easy to apply as the splint therapy used in the treatment of CTS. Therefore, we compared the results of the group applied splint and massage with the group applied only splint in order to determine the efficacy of this technique. The results revealed that improvement was higher in the group applied massage technique. Therefore, the new massage technique can be considered as a beneficial therapy method. Further studies conducted on larger patient groups are needed to show that this massage technique alone is also an effective and reliable therapy.
There are limited studies in the literature about massage therapy in CTS. Based on these data, we applied a new technique, which was easy to apply to the hands, included all massage modalities and had a name. Investigators have shown that massage therapy is not only beneficial in hands but also associated with significant decrease in pain scores in the locomotor diseases, particularly in fibromyalgia, back pain, arthritis, and migraine [13]. Pugatch et al. [17] found that serotonin was increased after the massage therapy in the patients who underwent massage therapy because of pain syndrome. In the present study, we did not measure the hormone levels of the patients; however, we used the scales developed to evaluate pain and functional capacity of the hand. We, therefore, thought that we could have an idea about the symptom severity and functional capacity of the hand via the questionnaires. We observed that the improvement in the group applied massage technique was higher than the group applied splint only.
Studies have suggested that massage plays a role in the reduction of the pain severity by decreasing the muscular tonus and increasing the local sympathetic activity [18]. Furthermore, it has been reported that “gate control mechanism” is also effective in the pain-relieving role of massage therapy and that massage therapy increases the level of oxytocin hormone, which has pain-relieving feature [18].
In the study of Field et al. [9] about efficacy of massage on CTS, they have suggested that significant improvement was observed in the massage group in terms of pain, anxiety, depression, hand grip strength, and median nerve peak latency scores; however, the increase in median nerve conduction velocity was not significant. Moreover, no statistically significant improvement was also found in any of the parameters in the control group [9]. The most important difference between the abovementioned successful study and the present study was the massage technique that we used. Moreover, in the present study the duration of massage was 3 min. This shorter duration of massage may be advantageous during the busy days; thus, the time that the patients would use for therapy is of great importance. On the other hand, each massage modality has individual benefit. All of these effects can be provided also with MHMT. The compliance of the patient with the therapy and efficacy and reliability of the technique suggest that MHMT can be recommended as the first choice of therapy in the future likewise the splint technique.
In another study by Moraska et al. [18] about efficacy of massage on CTS, as a result, statistically significant improvement was obtained regarding symptomatic pain scores; whereas only the group that received CTS-related hand massage showed significant improvement regarding the scores of functional hand evaluation and hand grip strength [18]. This successful study suggested that local massage was likely to be effective in the treatment of CTS. In the present study, the significant improvement in pain scores in the massage group can be attributed to the local massage therapy performed via MHMT, particularly to the decreased pressure on the median nerve due to the decreased muscle tonus and the increased local sympathetic activity as well as the lymphatic and venous return resulted from effleurage process, and to the increased pain threshold via friction process. We believe that effectively and accurately applied massage can provide these benefits. In the present study, we also applied an effective and accurate massage in a short duration of time and the results confirmed us.
The mechanism of action of message shows parallelism with the benefits of ultrasound (US) which is among the physical therapy modality. US are primarily used to warm the tissues of muscle-skeletal system such as joint structures, muscle and tendon, and penetration into the deep tissues are associated with its frequency [19]. In the present study, the fact that the improvement in patient-related and electrophysiological parameters with the massage therapy was similar to that obtained with the US therapy suggested that both the thermal and mechanical effects of these two therapies had an important role on the treatment. In the literature, it has been shown that the conduction velocity is increased in the peripheral nerves due to the thermal effect resulted from US therapy [19]. In the present study, we thought that the massage therapy might have led to an increase in the nerve conduction velocity via the same effect.
In a study conducted by Akalin et al. [11] with CTS, patients were performed splint and splint together with tendon and nerve stretching exercises. They reported statistically significant improvement in the clinical, patient-related, and neurophysiological findings in both groups [11]. In the present study as well, all the patients were asked to do these exercises in order the outcomes not to be affected. The only difference was the massage technique in the massage group.
Boston Scale is used for the patient-based evaluation of the symptom severity and functional capacity [20]. In the present study, we also used the Boston Questionnaire to observe the efficacy of splint and massage therapy. The symptom severity was decreased and the functional capacity was increased in both groups, being more significant in the massage group.
To the best our knowledge, the present study is the first and largest study in the literature conducted on the massage technique that will contribute to the treatment of CTS. As this new massage technique is easy for self-application, cheap, and practical, every patient with CTS can apply the massage to him/herself easily.
Conclusion and recommendations
-
Statistically more significant improvement was observed in PGA, MDPGA, hand grip strength scores, and electrophysiological parameters in the group applied MHMT as compared to the group applied splint therapy only.
-
After the treatment, statistically significant improvement was observed in certain electrophysiological parameters only in the massage group.
-
MHMT can be considered as an alternative therapy in CTS because it does not require a special treatment area and equipment, the patient can apply by him/herself, and it rapidly and effectively reaches to the tissues in the forearm and in the hand.
-
In brief, MHMT is a non-invasive, cheap, and easily applicable treatment option with high patient compliance.
References
Greer BG, Jenkins WM, Roberts R (1992) Carpal tunnel syndrome: a challenge for rehabilitation. J Rehabil 43–46
Kostopoulos D (2004) Treatment of carpal tunnel syndrome: a review of the non-surgical approaches with emphasis in neural mobilization. J Bodyw Mov Ther 8:2–8
Tanaka S, Wild DK, Seligman PJ et al (1994) The US prevalence of self-reported carpal tunnel syndrome: 1988 national health interview survey data. Am J Public Health 84(11):1846–1848
Bengston KA, Brault JS (2005) Hand disorders. In: Delisa JA (ed) Physical medicine & rehabilitation principles and practice, 3rd edn. Lippincott Williams & Wilkins, USA, pp 843–854
Piazzini DB, Aprile I, Ferrara PE et al (2007) A systematic review of conservative treatment of carpal tunnel syndrome. Clin Rehabil 21(4):299–314
Seradge H, Bear C, Bithell D (2000) Preventing carpal tunnel syndrome and cumulative trauma disorder: effect of carpal tunnel decompression exercises: an Oklahoma experience. J Okla State Med Assoc 93:150–153
Braco K, Naeser MA (1999) Carpal tunnel syndrome: clinical outcome after low-level laser acupuncture, microamps transcutaneous electrical nerve stimulation, and other alternative therapies-an open protocol study. J Altern Complement Med 5:5–26
Sunshine W, Field T, Quintino O et al (1996) Massage therapy and transcutaneous electrical stimulation effects on fibromyalgia. J Clin Rheumtol 2:8–22
Field T, Diego M, Cullen C et al (2004) Carpal tunnel syndrome symptoms are lessened following massage therapy. J Bodyw Mov Ther 8:9–14
Ostrom Kurrve W (2000) Massage and the original Swedish movements. Philadelphia, Copyright, 1918, By P. Blakiston’s Son & Co. The Maple Press, York, pp 8–18
Akalin E, El O, Peker O et al (2002) Treatment of carpal tunnel syndrome with nerve and tendon gliding exercises. Am J Phys Med Rehabil 81(2):108–113
Levine DW, Simmons BP, Koris MJ et al (1993) A self-administered questionnaire for the assessment of severity of symptoms and functional status in carpal tunnel syndrome. J Bone Joint Surg Am 75(11):1585–1592
Ross K (1997) Carpal tunnel syndrome diagnosis and treatment guideline. Workers’ Compensation Division, pp 12–49
Heathfield KWG (1957) Acroparaesthesiae and the carpal-tunnel syndrome. Lancet 2:663–666
Roaf R (1947) Compression of median nerve in carpal tunnel [letter]. Lancet 1:387
Luchetti R, Schoenhuber R, De Cicco G, Alfarano M, Deluca S, Landi A (1989) Carpal-tunnel pressure. Acta Orthop Scand 60:397–399
Pugatch et al (1969) Predictors and patterns of change associated with the course of time-limited psychotherapy. Mimeo Report
Moraska A, Chandler C, Edmiston-Schaetzel A, Franklin G, Calenda EL, Enebo B (2008) Comparison of a targeted and general massage protocol on strength, function, and symptoms associated with carpal tunnel syndrome: a randomized pilot study. J Altern Complement Med 14(3):259–267
Hong CZ, Liu HH, Yu J (1988) Ultrasound thermotherapy effect on the recovery of nerve conduction in experimental compression neuropathy. Arch Phys Med Rehabil 69(6):410–414
Leite JC, Jerosch-Herold C, Song F (2006) A systematic review of the psychometric properties of the Boston Carpal Tunnel Questionnaire. BMC Musculoskelet Disord 7:78
Open Access
This article is distributed under the terms of the Creative Commons Attribution Noncommercial License which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
Open Access This is an open access article distributed under the terms of the Creative Commons Attribution Noncommercial License (https://creativecommons.org/licenses/by-nc/2.0), which permits any noncommercial use, distribution, and reproduction in any medium, provided the original author(s) and source are credited.
About this article
Cite this article
Madenci, E., Altindag, O., Koca, I. et al. Reliability and efficacy of the new massage technique on the treatment in the patients with carpal tunnel syndrome. Rheumatol Int 32, 3171–3179 (2012). https://doi.org/10.1007/s00296-011-2149-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00296-011-2149-7