Abstract
Today, SF is a natural polymer with unique features, such as excellent mechanical properties, biocompatibility, biodegradability, and low toxicity, which characterize this material with diverse forms for different purposes. Silk nanoparticles, scaffolds, films, and mats are used in various therapeutic and diagnostic strategies including drug/gene delivery, tissue engineering, biomolecule detection, and wound healing. Therefore, a study that examines all SF applications and evaluates its toxicity helps researchers in future projects. In this study, we comprehensively searched all sources of databases in different years about the medical application of various types of SF. Also, we reviewed the toxicity of SF. Several newer papers were selected for reporting and conclusions. In conclusion, the evaluation of the literature revealed that SF is a promising candidate for a wide range of biomedical applications.
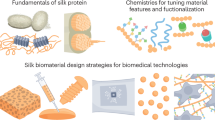
Graphical abstract







Similar content being viewed by others
Abbreviations
- 3D:
-
Three-dimensional
- 5-FU:
-
5-Fluorouracil
- Aβ1–40:
-
40-Aminoacid-long amyloid-β peptides
- ACL:
-
Anterior cruciate ligament
- AIHA:
-
Autoimmune hemolytic anemia
- BFGF:
-
Basic fibroblast growth factor
- CBMN:
-
Cytokinesis-blocked micronucleus
- Ce6:
-
Chlorin e6
- CHO-K1:
-
Comet assay using Chinese hamster ovary cells
- CM:
-
Cardiomyocyte
- DOX:
-
Doxorubicin
- DPSCs:
-
Dental pulp stem cells
- ECM:
-
Extracellular matrix
- EGF:
-
Endothelial growth factor
- G-EFT:
-
Graphene-based field-effect transistors
- GO:
-
Graphene oxide
- Gox:
-
Glucose oxidase
- HCV:
-
Hepatitis C virus
- HRP:
-
Horseradish peroxidase
- HMSCs:
-
Human mesenchymal stem cells
- HUVECs:
-
Human umbilical vein endothelial cells
- LbL:
-
Layer-by-layer
- MAbIMUG:
-
Monoclonal antibodies against human immunoglobulin
- MCF-7:
-
Michigan cancer foundation
- MSPPs:
-
Magnetic-silk/PEI core–shell nanoparticles
- MI:
-
Myocardial infarction
- NO:
-
Nitric oxide
- NP:
-
Nanoparticle
- ODNs:
-
Oligodeoxynucleotides
- OECs:
-
Olfactory ensheathing cells
- PCL:
-
Polycaprolactone
- PDMS:
-
Polydimethylsiloxane
- pDNA:
-
Plasmid deoxyribonucleic acid
- PDT:
-
Photodynamic therapy
- PEDOT:
-
Poly (3, 4 ethylenedioxythiophene)
- PEG:
-
Polyethylene glycol
- PEI:
-
Polyethyleneimine
- PGA:
-
Polyglycolic acid
- PLA:
-
Polylactic acid
- PLGA:
-
Polylactic-co-glycolic acid
- PLGA-SF-COL:
-
PLGA-SF-collagen
- RBCs:
-
Red blood cells
- SF:
-
SF
- SF/HAp:
-
SF/hydroxyapatite
- SF-HT-3GEN:
-
SF-based nanofibrous hardystonite-gentamicin
- SNAP:
-
S-Nitroso-N-acetylpenicillamine
- SPP:
-
Silk–polyethyleneimine
- TGF-β3:
-
Transforming growth factor beta-3
- THP:
-
Tumor-homing peptides
- TiO2:
-
Titanium dioxide
- UTS:
-
Ultimate tensile strength
- VEGF:
-
Vascular endothelial growth factor
References
Lewis R (1996) Unraveling the weave of spider silk. Bioscience 46(9):636–638. https://doi.org/10.2307/1312891
Janani G, Kumar M, Chouhan D, Moses JC, Gangrade A, Bhattacharjee S, Mandal BB (2019) Insight into silk-based biomaterials: from physicochemical attributes to recent biomedical applications. ACS Appl Bio Mater 2(12):5460–5491. https://doi.org/10.1021/acsabm.9b00576
Altman GH, Diaz F, Jakuba C, Calabro T, Horan RL, Chen J, Helen Lu, Richmond J, Kaplan DL (2003) Silk-based biomaterials. Biomaterials 24(3):401–416. https://doi.org/10.1016/S0142-9612(02)00353-8
Zhu B, Li W, Lewis RV, Segre CU, Wang R (2015) E-spun composite fibers of collagen and dragline silk protein: fiber mechanics, biocompatibility, and application in stem cell differentiation. Biomacromol 16(1):202–213. https://doi.org/10.1021/bm501403f
Ayoub NA, Garb JE, Tinghitella RM, Collin MA, Hayashi CY (2007) Blueprint for a high-performance biomaterial: full-length spider dragline silk genes. PLoS ONE 2(6):e514. https://doi.org/10.1371/journal.pone.0000514
Shimura K, Kikuchi A, Ohtomo K, Yōtarō KATAGATA, Hyodo A (1976) Studies on silk fibroin of Bombyx mori. I. Fractionation of fibroin prepared from the posterior silk gland. J Biochem 80(4):693–702. https://doi.org/10.1093/oxfordjournals.jbchem.a131328
Kundu B, Rajkhowa R, Kundu SC, Wang X (2013) Silk fibroin biomaterials for tissue regenerations. Adv Drug Deliv Rev 65(4):457–470. https://doi.org/10.1016/j.addr.2012.09.043
Engler AJ, Shamik Sen H, Sweeney L, Discher DE (2006) Matrix elasticity directs stem cell lineage specification. Cell 126(4):677–689. https://doi.org/10.1016/j.cell.2006.06.044
Wells RG (2008) The role of matrix stiffness in regulating cell behavior. Hepatology 47(4):1394–1400. https://doi.org/10.1002/hep.22193
Tran TT, Hamid ZA, Cheong KY (2018) A review of mechanical properties of scaffold in tissue engineering: aloe vera composites. J Phys: Conf Ser. IOP Publishing
Azizah Intan Pangesty and Mitsugu Todo (2021) Improvement of mechanical strength of tissue engineering scaffold due to the temperature control of polymer blend solution. J Funct Biomater 12(3):47. https://doi.org/10.3390/jfb12030047
Winkler S, Kaplan DL (2000) Molecular biology of spider silk. Rev Mol Biotechnol 74(2):85–93. https://doi.org/10.1016/S1389-0352(00)00005-2
Cunniff PM, Fossey SA, Auerbach MA, Song JW, Kaplan DL, Wade Adams W, Eby RK, Mahoney D, Vezie DL (1994) Mechanical and thermal properties of dragline silk from the spider nephila clavipes. Polym Adv Technol 5(8):401–410. https://doi.org/10.1002/pat.1994.220050801
Wang Y, Rudym DD, Walsh A, Abrahamsen L, Kim H-J, Kim HS, Kirker-Head C, Kaplan DL (2008) In vivo degradation of three-dimensional silk fibroin scaffolds. Biomaterials 29(24–25):3415–3428. https://doi.org/10.1016/j.biomaterials.2008.05.002
Hollister SJ (2005) Porous scaffold design for tissue engineering. Nat Mater 4(7):518–524. https://doi.org/10.1038/nmat1421
Afjeh-Dana E, Naserzadeh P, Nazari H, Mottaghitalab RSF, Naser BA, Mehravi F, Tajik MTR, Joghataei K, Mousavizadeh (2019) Gold nanorods reinforced silk fibroin nanocomposite for peripheral nerve tissue engineering applications. Int J Biol Macromol 129:1034–1039. https://doi.org/10.1016/j.ijbiomac.2019.02.050
Zhou J, Cao C, Ma X, Lan Hu, Chen L, Wang C (2010) In vitro and in vivo degradation behavior of aqueous-derived electrospun silk fibroin scaffolds. Polym Degrad Stab 95(9):1679–1685. https://doi.org/10.1016/j.polymdegradstab.2010.05.025
Johari N, Moroni L, Samadikuchaksaraei A (2020) Tuning the conformation and mechanical properties of silk fibroin hydrogels. Eur Polym J 134:109842. https://doi.org/10.1016/j.eurpolymj.2020.109842
Das S, Sharma M, Saharia D, Sarma KK, Sarma MG, Borthakur BB, Bora U (2015) In vivo studies of silk based gold nano-composite conduits for functional peripheral nerve regeneration. Biomaterials 62:66–75. https://doi.org/10.1016/j.biomaterials.2015.04.047
Scaffaro R, Lopresti F, Maio A, Sutera F, Botta L (2017) Development of polymeric functionally graded scaffolds: a brief review. J Appl Biomater Funct Mater 15(2):107–121. https://doi.org/10.5301/jabfm.5000332
Zhou J, Cao C, Ma X (2009) A novel three-dimensional tubular scaffold prepared from silk fibroin by electrospinning. Int J Biol Macromol 45(5):504–510. https://doi.org/10.1016/j.ijbiomac.2009.09.006
Akturk O, Kismet K, Yasti AC, Kuru S, Duymus ME, Kaya F, Caydere M, Hucumenoglu S, Keskin D (2016) Wet electrospun silk fibroin/gold nanoparticle 3D matrices for wound healing applications. Rsc Adv 6(16):13234–13250. https://doi.org/10.1039/C5RA24225H
Naskar D, Ghosh AK, Mandal M, Das P, Nandi SK, Kundu SC (2017) Dual growth factor loaded nonmulberry silk fibroin/carbon nanofiber composite 3D scaffolds for in vitro and in vivo bone regeneration. Biomaterials 136:67–85. https://doi.org/10.1016/j.biomaterials.2017.05.014
Reeves ARD, Spiller KL, Freytes DO, Vunjak-Novakovic G, Kaplan DL (2015) Controlled release of cytokines using silk-biomaterials for macrophage polarization. Biomaterials 73:272–283. https://doi.org/10.1016/j.biomaterials.2015.09.027
Shi P, Goh JCH (2011) Release and cellular acceptance of multiple drugs loaded silk fibroin particles. Int J Pharm 420(2):282–289. https://doi.org/10.1016/j.ijpharm.2011.08.051
Long K, Liu Y, Li W, Wang L, Liu Sa, Wang Y, Wang Z, Ren Li (2015) Improving the mechanical properties of collagen-based membranes using silk fibroin for corneal tissue engineering. J Biomed Mater Res, Part A 103(3):1159–1168. https://doi.org/10.1002/jbm.a.35268
Afjeh-Dana E, Ashtari K, Amini N (2019) Scaffolds for tarsal repair in eyelids, In: Handbook of tissue engineering scaffolds: Volume Two. Elsevier, pp 721–738. https://doi.org/10.1016/B978-0-08-102561-1.00030-0
Hong H, Seo YB, Lee JS, Lee YJ, Lee H, Olatunji Ajiteru Md, Sultan T, Lee OJ, Kim SH et al (2020) Digital light processing 3D printed silk fibroin hydrogel for cartilage tissue engineering. Biomaterials 232:119679. https://doi.org/10.1016/j.biomaterials.2019.119679
Park YR, Hyung Woo Ju, Lee JM, Kim D-K, Lee OJ, Moon BM, Park HJ, Jeong JY, Yeon YK et al (2016) Three-dimensional electrospun silk-fibroin nanofiber for skin tissue engineering. Int J Biol Macromol 93:1567–1574. https://doi.org/10.1016/j.ijbiomac.2016.07.047
Farokhi M, Mottaghitalab F, Samani S, Shokrgozar MA, Kundu SC, Reis RL, Fatahi Y, Kaplan DL (2018) Silk fibroin/hydroxyapatite composites for bone tissue engineering. Biotechnol Adv 36(1):68–91. https://doi.org/10.1016/j.biotechadv.2017.10.001
Zhou J, Cao C, Ma X, Lin J (2010) Electrospinning of silk fibroin and collagen for vascular tissue engineering. Int J Biol Macromol 47(4):514–519. https://doi.org/10.1016/j.ijbiomac.2010.07.010
Boni R, Ali A, Giteru SG, Shavandi A, Clarkson AN (2020) Silk fibroin nanoscaffolds for neural tissue engineering. J Mater Sci: Mater Med 31(9):1–17. https://doi.org/10.1007/s10856-020-06422-5
Afjeh-Dana E, Ashtari K, Milan PB (2019) Scaffolds for auditory nerve regeneration, In: Handbook of tissue engineering scaffolds: volume two, Elsevier, pp 123–143. https://doi.org/10.1016/B978-0-08-102561-1.00005-1
Bhardwaj N, Kundu SC (2012) Chondrogenic differentiation of rat MSCs on porous scaffolds of silk fibroin/chitosan blends. Biomaterials 33(10):2848–2857. https://doi.org/10.1016/j.biomaterials.2011.12.028
Mieszawska AJ, Fourligas N, Georgakoudi I, Ouhib NM, Belton DJ, Perry CC, Kaplan DL (2010) Osteoinductive silk–silica composite biomaterials for bone regeneration. Biomaterials 31(34):8902–8910. https://doi.org/10.1016/j.biomaterials.2010.07.109
Vollrath F, Porter D (2009) Silks as ancient models for modern polymers. Polymer 50(24):5623–5632. https://doi.org/10.1016/j.polymer.2009.09.068
Mahmoodi NM, Arami M (2009) Numerical finite volume modeling of dye decolorization using immobilized titania nanophotocatalysis. Chem Eng J 146(2):189–193. https://doi.org/10.1016/j.cej.2008.05.036
Thurber AE, Omenetto FG, Kaplan DL (2015) In vivo bioresponses to silk proteins. Biomaterials 71:145–157. https://doi.org/10.1016/j.biomaterials.2015.08.039
Feng Y, Lin J, Niu L, Wang Y, Cheng Z, Sun X, Li M (2020) High molecular weight silk fibroin prepared by papain degumming. Polymers 12(9):2105. https://doi.org/10.3390/polym12092105
Dou H, Zuo B (2015) Effect of sodium carbonate concentrations on the degumming and regeneration process of silk fibroin. J Text Ins 106(3):311–319. https://doi.org/10.1080/00405000.2014.919065
Arami M, Rahimi S, Mivehie L, Mazaheri F, Mahmoodi NM (2007) Degumming of Persian silk with mixed proteolytic enzymes. J Appl Polym Sci 106(1):267–275. https://doi.org/10.1002/app.26492
Chung-haur Howard Lo (2020) Degumming silk by CO2 supercritical fluid and their dyeing ability with plant indigo. Int J Cloth Sci Technol. https://doi.org/10.1108/IJCST-06-2019-0072
Khan MMR, Tsukada M, Gotoh Y, Morikawa H, Freddi G, Shiozaki H (2010) Physical properties and dyeability of silk fibers degummed with citric acid. Biores Technol 101(21):8439–8445. https://doi.org/10.1016/j.biortech.2010.05.100
Wang R, Zhu Y, Shi Z, Jiang W, Liu X, Ni Q-Q (2018) Degumming of raw silk via steam treatment. J Clean Prod 203:492–497. https://doi.org/10.1016/j.jclepro.2018.08.286
Kim HJ, Kim MK, Lee KH, Nho SK, Han MS, Um IC (2017) Effect of degumming methods on structural characteristics and properties of regenerated silk. Int J Biol Macromol 104:294–302. https://doi.org/10.1016/j.ijbiomac.2017.06.019
Mahmoodi NM, Arami M, Mazaheri F, Rahimi S (2010) Degradation of sericin (degumming) of Persian silk by ultrasound and enzymes as a cleaner and environmentally friendly process. J Clean Prod 8(2):146–151. https://doi.org/10.1016/j.jclepro.2009.10.003
Guzmán Carissimi A, Lozano-Pérez A, Montalbán MG, Aznar-Cervantes SD, Cenis JL, Víllora G (2019) Revealing the influence of the degumming process in the properties of silk fibroin nanoparticles. Polymers 11(12):2045. https://doi.org/10.3390/polym11122045
Pandey S, Son N, Kim S, Balakrishnan D, Kang M (2022) Locust Bean gum-based hydrogels embedded magnetic iron oxide nanoparticles nanocomposite: advanced materials for environmental and energy applications. Environ Res 214:114000. https://doi.org/10.1016/j.envres.2022.114000
Sargazi S, Laraib U, Barani M, Rahdar A, Fatima I, Bilal M, Pandey S, Sharma RK, Kyzas GZ (2022) Recent trends in the mesoporous silica nanoparticles with rode-like morphology for cancer theranostics: a review. J Mol Struct. https://doi.org/10.1016/j.molstruc.2022.132922
Saman Sargazi ER, Simge SS, Gelen AR, Bilal M, Arshad R, Ajalli N, Khan MFA, Pandey S (2022) Application of titanium dioxide nanoparticles in photothermal and photodynamic therapy of cancer: an updated and comprehensive review. J Drug Deliv Sci Technol. https://doi.org/10.1016/j.jddst.2022.103605
Kumar A, Sharipov M, Turaev A, Azizov S, Azizov I, Makhado E, Rahdar A, Kumar D, Pandey S (2022) Polymer-based hybrid nanoarchitectures for cancer therapy applications. Polymers 14(15):3027. https://doi.org/10.3390/polym14153027
Arshad R, Kiani MH, Rahdar A, Sargazi S, Barani M, Shojaei S, Bilal M, Kumar D, Pandey S (2022) Nano-based theranostic platforms for breast cancer: a review of latest advancements. Bioengineering 9(7):320. https://doi.org/10.3390/bioengineering9070320
Philipp Seib F, Jones GT, Rnjak-Kovacina J, Lin Y, Kaplan DL (2013) pH-dependent anticancer drug release from silk nanoparticles. Adv Healthc Mater 2(12):1606–1611. https://doi.org/10.1002/adhm.201300034
Wang Qi, Jian M, Wang C, Zhang Y (2017) Carbonized silk nanofiber membrane for transparent and sensitive electronic skin. Adv Funct Mater 27(9):1605657. https://doi.org/10.1002/adfm.201605657
Choi M, Choi D, Hong J (2018) Multilayered controlled drug release silk fibroin nanofilm by manipulating secondary structure. Biomacromol 19(7):3096–3103. https://doi.org/10.1021/acs.biomac.8b00687
Totten JD, Wongpinyochit T, Philipp Seib F (2017) Silk nanoparticles: proof of lysosomotropic anticancer drug delivery at single-cell resolution. J Drug Target 25(9–10):865–872. https://doi.org/10.1080/1061186X.2017.1363212
Xiao L, Guozhong Lu, Qiang Lu, Kaplan DL (2016) Direct formation of silk nanoparticles for drug delivery. ACS Biomater Sci Eng 2(11):2050–2057. https://doi.org/10.1021/acsbiomaterials.6b00457
Hongchun Wu, Liu S, Xiao L, Dong X, Qiang Lu, Kaplan DL (2016) Injectable and pH-responsive silk nanofiber hydrogels for sustained anticancer drug delivery. ACS Appl Mater Interfaces 8(27):17118–17126. https://doi.org/10.1021/acsami.6b04424
Wang X, Yucel T, Qiang Lu, Xiao Hu, Kaplan DL (2010) Silk nanospheres and microspheres from silk/pva blend films for drug delivery. Biomaterials 31(6):1025–1035. https://doi.org/10.1016/j.biomaterials.2009.11.002
Jing Qu, Liu Yu, Yanni Yu, Li J, Luo J, Li M (2014) Silk fibroin nanoparticles prepared by electrospray as controlled release carriers of cisplatin. Mater Sci Eng C 44:166–174. https://doi.org/10.1016/j.msec.2014.08.034
Zhang Y-Q, Shen W-D, Xiang R-L, Zhuge L-J, Gao W-J, Wang W-B (2007) Formation of silk fibroin nanoparticles in water-miscible organic solvent and their characterization. J Nanopart Res 9(5):885–900. https://doi.org/10.1007/s11051-006-9162-x
Zhao Z, Li Yi, Chen A-Z, Zheng Z-J, Jun-Yan Hu, Li J-S, Li G (2013) Generation of silk fibroin nanoparticles via solution-enhanced dispersion by supercritical CO2. Ind Eng Chem Res 52(10):3752–3761. https://doi.org/10.1021/ie301907f|
Lammel AS, Xiao Hu, Park S-H, Kaplan DL, Scheibel TR (2010) Controlling silk fibroin particle features for drug delivery. Biomaterials 31(16):4583–4591. https://doi.org/10.1016/j.biomaterials.2010.02.024
Kazemimostaghim M, Rajkhowa R, Tsuzuki T, Wang X (2013) Ultrafine silk powder from biocompatible surfactant-assisted milling. Powder Technol 249:253–257. https://doi.org/10.1016/j.powtec.2013.08.028
Myung SJ, Kim H-S, Kim Y, Chen P, Jin H-J (2008) Fluorescent silk fibroin nanoparticles prepared using a reverse microemulsion. Macromol Res 16(7):604–608. https://doi.org/10.1007/BF03218567
YongLi HUANG, Qiang LU, MingZhong LI, Bing ZHANG, HeSun ZHU (2011) Silk fibroin microsphere drug carriers perpared under electric fields. Chin Sci Bull 56(13):1013–1018
Gupta V, Aseh A, Ríos CN, Aggarwal BB, Mathur AB (2009) Fabrication and characterization of silk fibroin-derived curcumin nanoparticles for cancer therapy. Int J Nanomed 4:115. https://doi.org/10.2147/ijn.s5581
Ghalei S, Mondal A, Hopkins S, Singha P, Devine R, Handa H, Nanoparticles S (2020) A natural polymeric platform for nitric oxide delivery in biomedical applications. ACS Appl Mater Interfaces 12(48):53615–53623. https://doi.org/10.1021/acsami.0c13813
Wongpinyochit T, Uhlmann P, Urquhart AJ, Philipp Seib F (2015) PEGylated silk nanoparticles for anticancer drug delivery. Biomacromol 16(11):3712–3722. https://doi.org/10.1021/acs.biomac.5b01003
Subia B, Kundu SC (2012) Drug loading and release on tumor cells using silk fibroin–albumin nanoparticles as carriers. Nanotechnology 24(3):035103. https://doi.org/10.1088/0957-4484/24/3/035103
Kundu J, Chung Y-I, Kim YH, Tae G, Kundu SC (2010) Silk fibroin nanoparticles for cellular uptake and control release. Int J Pharm 388(1–2):242–250. https://doi.org/10.1016/j.ijpharm.2009.12.052
Herold HM, Döbl A, Wohlrab S, Humenik M, Scheibel T (2020) Designed spider silk-based drug carrier for redox-or pH-triggered drug release. Biomacromol 21(12):4904–4912. https://doi.org/10.1021/acs.biomac.0c01138
Kim J-H, Sheikh FA, Hyung Woo Ju, Park HJ, Moon BM, Lee OJ, Park CH (2014) 3D silk fibroin scaffold incorporating titanium dioxide (TiO2) nanoparticle (NPs) for tissue engineering. Int J Biol Macromol 68:158–168. https://doi.org/10.1016/j.ijbiomac.2014.04.045
Zafar B, Mottaghitalab F, Shahosseini Z, Negahdari B, Farokhi M (2020) Silk fibroin/alumina nanoparticle scaffold using for osteogenic differentiation of rabbit adipose-derived stem cells. Materialia 9:100518. https://doi.org/10.1016/j.mtla.2019.100518
Sridhar S, Venugopal JR, Sridhar R, Ramakrishna S (2015) Cardiogenic differentiation of mesenchymal stem cells with gold nanoparticle loaded functionalized nanofibers. Colloids Surf B: Biointerfaces 134:346–354. https://doi.org/10.1016/j.colsurfb.2015.07.019
Guoxu Zhao Xu, Zhang BL, Huang G, Feng Xu, Zhang X (2020) Solvent-free fabrication of carbon nanotube/silk fibroin electrospun matrices for enhancing cardiomyocyte functionalities. ACS Biomater Sci Eng 6(3):1630–1640. https://doi.org/10.1021/acsbiomaterials.9b01682
Yang Yi, Ding X, Zou T, Peng Ge, Liu H, Fan Y (2017) Preparation and characterization of electrospun graphene/silk fibroin conductive fibrous scaffolds. RSC Adv 7(13):7954–7963. https://doi.org/10.1039/C6RA26807B
Tian L, Prabhakaran MP, Jue Hu, Chen M, Besenbacher F, Ramakrishna S (2015) Coaxial electrospun poly (lactic acid)/silk fibroin nanofibers incorporated with nerve growth factor support the differentiation of neuronal stem cells. RSC Adv 5(62):49838–49848. https://doi.org/10.1039/C5RA05773F
Kim BN, Ko Y-G, Yeo T, Kim EJ, Kwon OK, Kwon OH (2019) Guided regeneration of rabbit calvarial defects using silk fibroin nanofiber-poly (glycolic acid) hybrid scaffolds. ACS Biomater Sci Eng 5(10):5266–5272. https://doi.org/10.1021/acsbiomaterials.9b00678
Nazeer MA, Yilgor E, Yilgor I (2019) Electrospun polycaprolactone/silk fibroin nanofibrous bioactive scaffolds for tissue engineering applications. Polymer 168:86–94. https://doi.org/10.1016/j.polymer.2019.02.023
Zhang X, Reagan MR, Kaplan DL (2009) Electrospun silk biomaterial scaffolds for regenerative medicine. Adv Drug Deliv Rev 61(12):988–1006. https://doi.org/10.1016/j.addr.2009.07.005
Bhardwaj N, Kundu SC (2010) Electrospinning: a fascinating fiber fabrication technique. Biotechnol Adv 28(3):325–347. https://doi.org/10.1016/j.biotechadv.2010.01.004
Chutipakdeevong J, Ruktanonchai UR, Supaphol P (2013) Process optimization of electrospun silk fibroin fiber mat for accelerated wound healing. J Appl Polym Sci 130(5):3634–3644. https://doi.org/10.1002/app.39611
Navone SE, Pascucci L, Dossena M, Ferri A, Invernici G, Acerbi F, Cristini S, Bedini G, Tosetti V et al (2014) Decellularized silk fibroin scaffold primed with adipose mesenchymal stromal cells improves wound healing in diabetic mice. Stem cell Res Therapy 5(1):1–15. https://doi.org/10.1186/scrt396
Wang S, Zhang Y, Wang H, Yin G, Dong Z (2009) Fabrication and properties of the electrospun polylactide/silk fibroin-gelatin composite tubular scaffold. Biomacromol 10(8):2240–2244. https://doi.org/10.1021/bm900416b
Yifeng Yu, Xiaofeng Yu, Tian D, Aixi Yu, Wan Y (2021) Thermo-responsive chitosan/silk fibroin/amino-functionalized mesoporous silica hydrogels with strong and elastic characteristics for bone tissue engineering. Int J Biol Macromol 182:1746–1758. https://doi.org/10.1016/j.ijbiomac.2021.05.166
Liu X, Chen Bo, Li Y, Kong Y, Ming Gao Lu, Zhang Z, Ning Gu (2021) Development of an electrospun polycaprolactone/silk scaffold for potential vascular tissue engineering applications. J Bioact Compat Polym 36(1):59–76. https://doi.org/10.1177/0883911520973244
Keirouz A, Zakharova M, Kwon J, Robert C, Koutsos V, Callanan A, Chen X, Fortunato G, Radacsi N (2020) High-throughput production of silk fibroin-based electrospun fibers as biomaterial for skin tissue engineering applications. Mater Sci Eng C 112:110939. https://doi.org/10.1016/j.msec.2020.110939
Kim SH, Seo YB, Yeon YK, Lee YJ, Park HS, Sultan MT, Lee JM, Lee JS, Lee OJ et al (2020) 4D-bioprinted silk hydrogels for tissue engineering. Biomaterials 260:120281. https://doi.org/10.1016/j.biomaterials.2020.120281
Lau K, Akhavan B, Lord MS, Bilek MM, Rnjak-Kovacina J (2020) Dry surface treatments of silk biomaterials and their utility in biomedical applications. ACS Biomater Sci Eng 6(10):5431–5452. https://doi.org/10.1021/acsbiomaterials.0c00888
Chouhan D, Mandal BB (2020) Silk biomaterials in wound healing and skin regeneration therapeutics: from bench to bedside. Acta Biomater 103:24–51. https://doi.org/10.1016/j.actbio.2019.11.050
Pandey V, Haider T, Jain P, Gupta PN, Soni V (2020) Silk as a leading-edge biological macromolecule for improved drug delivery. J Drug Deliv Sci Technol 55:101294. https://doi.org/10.1016/j.jddst.2019.101294
Chambre L, Martín-Moldes Z, Parker RN, Kaplan DL (2020) Bioengineered elastin-and silk-biomaterials for drug and gene delivery. Adv Drug Deliv Rev. https://doi.org/10.1016/j.addr.2020.10.008
Wang J, Yin Z, Xue X, Kundu SC, Mo X, Shenzhou Lu (2016) Natural non-mulberry silk nanoparticles for potential-controlled drug release. Int J Mol Sci 17(12):2012. https://doi.org/10.3390/ijms17122012
Mao B, Liu C, Zheng W, Li X, Ge R, Shen H, Guo X, Lian Q, Shen X et al (2018) Cyclic cRGDfk peptide and Chlorin e6 functionalized silk fibroin nanoparticles for targeted drug delivery and photodynamic therapy. Biomaterials 161:306–320. https://doi.org/10.1016/j.biomaterials.2018.01.045
Numata K, Reagan MR, Goldstein RH, Rosenblatt M, Kaplan DL (2011) Spider silk-based gene carriers for tumor cell-specific delivery. Bioconjugate Chem 22(8):1605–1610. https://doi.org/10.1021/bc200170u
Song W, Gregory DA, Al-Janabi H, Muthana M, Cai Z, Zhao X (2019) Magnetic-silk/polyethyleneimine core-shell nanoparticles for targeted gene delivery into human breast cancer cells. Int J Pharm 555:322–336. https://doi.org/10.1016/j.ijpharm.2018.11.030
Khorshidi S, Solouk A, Mazinani S, Mirzadeh H (2016) A review on different approaches for improving cell infiltration in electrospun nanofibrous scaffolds. Pathobiol Res 18(4):1–22. https://doi.org/10.1002/term.1978
Fergal JO (2011) Biomaterials and scaffolds for tissue engineering. Mater Today 14(3):88–95. https://doi.org/10.1016/S1369-7021(11)70058-X
Narmatha Christy P, Khaleel Basha S, Sugantha Kumari V, Bashir AKH, Maaza M, Kaviyarasu K, Arasu MV, Al-Dhabi NA, Ignacimuthu S (2020) Biopolymeric nanocomposite scaffolds for bone tissue engineering applications–a review. J Drug Deliv Sci Technol 55:101452. https://doi.org/10.1016/j.jddst.2019.101452
Anjum S, Rahman F, Pandey P, Arya DK, Alam M, Rajinikanth PS, Qiang AO (2022) Electrospun biomimetic nanofibrous scaffolds: a promising prospect for bone tissue engineering and regenerative medicine. Int J Mol Sci 23(16):9206. https://doi.org/10.3390/ijms23169206
Tandon S, Kandasubramanian B, Ibrahim SM (2020) Silk-based composite scaffolds for tissue engineering applications. Ind Eng Chem Res 59(40):17593–17611. https://doi.org/10.1021/acs.iecr.0c02195
Yang M, Shuai Y, He W, Min S, Zhu L (2012) Preparation of porous scaffolds from silk fibroin extracted from the silk gland of Bombyx mori (B. mori). Int J Mol Sci 13(6):7762–7775. https://doi.org/10.3390/ijms13067762
Zhang Li, Zhang W, Yejun Hu, Fei Y, Liu H, Huang Z, Wang C, Ruan D, Heng BC et al (2021) Systematic review of silk scaffolds in musculoskeletal tissue engineering applications in the recent decade. ACS Biomater Sci Eng 7(3):817–840. https://doi.org/10.1021/acsbiomaterials.0c01716
Afjeh-Dana E, Naserzadeh P, Moradi E, Hosseini N, Seifalian AM, Ashtari B (2022) Stem cell differentiation into cardiomyocytes: current methods and emerging approaches. Stem cell Rev Rep. https://doi.org/10.1007/s12015-022-10395-z
Wang Y, Kim U-J, Blasioli DJ, Kim H-J, Kaplan DL (2005) In vitro cartilage tissue engineering with 3D porous aqueous-derived silk scaffolds and mesenchymal stem cells. Biomaterials 26(34):7082–7094. https://doi.org/10.1016/j.biomaterials.2005.05.022
Li X, Snedeker JG (2013) Wired silk architectures provide a biomimetic ACL tissue engineering scaffold. J Mech Behav Biomed Mater 22:30–40. https://doi.org/10.1016/j.jmbbm.2013.03.015
Hadisi Z, Bakhsheshi-Rad HR, Walsh T, Dehghan MM, Farzad-Mohajeri S, Gholami H, Diyanoush A, Pagan E, Akbari M (2020) In vitro and in vivo evaluation of silk fibroin-hardystonite-gentamicin nanofibrous scaffold for tissue engineering applications. Polym Test 91:106698. https://doi.org/10.1016/j.polymertesting.2020.106698
Yang J-W, Zhang Y-F, Sun Z-y, Song G-T, Chen Z (2015) Dental pulp tissue engineering with bFGF-incorporated silk fibroin scaffolds. J Biomater Appl 30(2):221–229. https://doi.org/10.1177/0885328215577296
Wang G, Xudong Hu, Lin W, Dong C, Hui Wu (2011) Electrospun PLGA–silk fibroin–collagen nanofibrous scaffolds for nerve tissue engineering. Vitro Cell Develop Biol-Animal 47(3):234–240. https://doi.org/10.1007/s11626-010-9381-4
Shen Y, Qian Y, Zhang H, Zuo B, Zhenfeng Lu, Fan Z, Zhang P, Zhang F, Zhou C (2010) Guidance of olfactory ensheathing cell growth and migration on electrospun silk fibroin scaffolds. Cell Transplant 19(2):147–158. https://doi.org/10.3727/096368910X492616
Gupta P, Kumar M, Bhardwaj N, Kumar JP, Krishnamurthy CS, Nandi SK, Mandal BB (2016) Mimicking form and function of native small diameter vascular conduits using mulberry and non-mulberry patterned silk films. ACS Appl Mater Interfaces 8(25):15874–15888. https://doi.org/10.1021/acsami.6b00783
Rockwood DN, Preda RC, Yücel T, Wang X, Lovett ML, Kaplan DL (2011) Materials fabrication from Bombyx mori silk fibroin. Nat Protocols 6(10):1612–1631. https://doi.org/10.1038/nprot.2011.379
Mehrotra S, Nandi SK, Mandal BB (2017) Stacked silk-cell monolayers as a biomimetic three dimensional construct for cardiac tissue reconstruction. J Mater Chem B 5(31):6325–6338. https://doi.org/10.1039/C7TB01494E
Yin H, Zhou Y, Jing Xu, Ai S, Cui L, Zhu L (2010) Amperometric biosensor based on tyrosinase immobilized onto multiwalled carbon nanotubes-cobalt phthalocyanine-silk fibroin film and its application to determine bisphenol A. Anal Chim Acta 659(1–2):144–150. https://doi.org/10.1016/j.aca.2009.11.051
Lawrence BD, Omenetto F, Chui K, Kaplan DL (2008) Processing methods to control silk fibroin film biomaterial features. J Mater Sci 43:6967–6985. https://doi.org/10.1007/s10853-008-2961-y
Prakash NJ, Mane PP, George SM, Kandasubramanian B (2021) Silk fibroin as an immobilization matrix for sensing applications. ACS Biomater Sci Eng. https://doi.org/10.1021/acsbiomaterials.1c00080
Meng Xu, Yadavalli VK (2019) Flexible biosensors for the impedimetric detection of protein targets using silk-conductive polymer biocomposites. ACS Sens 4(4):1040–1047. https://doi.org/10.1021/acssensors.9b00230
Gonçalves JM, Lima LR, Moraes ML, Ribeiro SJL (2016) Immunosensor for diagnosis of Alzheimer disease using amyloid-β 1–40 peptide and silk fibroin thin films. Mater Sci Eng C 68:338–342. https://doi.org/10.1016/j.msec.2016.05.101
Jia Z, Gong J, Zeng Y, Ran J, Liu J, Wang K, Xie C, Xiong Lu, Wang J (2021) Bioinspired conductive silk microfiber integrated bioelectronic for diagnosis and wound healing in diabetes. Adv Funct Mater 31(19):2010461. https://doi.org/10.1002/adfm.202010461
Moraes ML, Lima LR, Vicentini-Oliveira JC, de Aparecida Vitória G, Souza ON, Oliveira ED, Ribeiro SJL (2019) Immunosensor for the diagnostics of autoimmune hemolytic anemia (AIHA) based on immobilization of a monoclonal antibody on a layer of silk fibroin. J Nanosci Nanotechnol 19(7):3772–3776. https://doi.org/10.1166/jnn.2019.16305
Moraes ML, Lima LR, Silva RR, Cavicchioli M, Ribeiro SJL (2013) Immunosensor based on immobilization of antigenic peptide NS5A-1 from HCV and silk fibroin in nanostructured films. Langmuir 29(11):3829–3834. https://doi.org/10.1021/la304404v
Rafieian S, Mirzadeh H, Mahdavi H, Masoumi ME (2019) A review on nanocomposite hydrogels and their biomedical applications. Sci Eng Compos Mater 26(1):154–174. https://doi.org/10.1515/secm-2017-0161
Zheng H, Lin N, He Y, Zuo B (2021) Self-healing, self-adhesive silk fibroin conductive hydrogel as a flexible strain sensor. ACS Appl Mater Interfaces 13(33):40013–40031. https://doi.org/10.1021/acsami.1c08395
Pollini M, Paladini F (2020) Bioinspired materials for wound healing application: the potential of silk fibroin. Materials 13(15):3361. https://doi.org/10.3390/ma13153361
Li G, Liu H, Li TianDuo, Wang J (2012) Surface modification and functionalization of silk fibroin fibers/fabric toward high performance applications. Mater Sci Eng C 32(4):627–636. https://doi.org/10.1016/j.msec.2011.12.013
Gangrade A, Gawali B, Jadi PK, Naidu VG, Mandal BB (2020) Photoelectro active nanocomposite silk hydrogel for spatiotemporal controlled release of chemotherapeutics. Vivo, pp 27905–16. https://doi.org/10.1021/acsami.0c02470
Raia NR, Jia Di, Ghezzi CE, Muthukumar M, Kaplan DL (2020) Characterization of silk-hyaluronic acid composite hydrogels towards vitreous humor substitutes. Biomaterials 233:119729. https://doi.org/10.1016/j.biomaterials.2019.119729
Wani SU, Din SP, Gautam Qadrie ZL, Gangadharappa HV (2020) Silk fibroin as a natural polymeric based bio-material for tissue engineering and drug delivery systems-a review. Int J Biol Macromol 163:2145–2161
Wang Z, Haiyang Yu, Zhao Z (2021) Silk fibroin hydrogel encapsulated graphene filed-effect transistors as enzyme-based biosensors. Microchem J 169:106585. https://doi.org/10.1016/j.microc.2021.106585
Ziadlou R, Rotman S, Teuschl A, Salzer E, Barbero A, Martin I, Alini M, Eglin D, Grad S (2021) Optimization of hyaluronic acid-tyramine/silk-fibroin composite hydrogels for cartilage tissue engineering and delivery of anti-inflammatory and anabolic drugs. Mater Sci Eng C 120:111701. https://doi.org/10.1016/j.msec.2020.111701
Zheng H, Zuo B (2021) Functional silk fibroin hydrogels: preparation, properties and applications. J Mater Chem B 9(5):1238–1258. https://doi.org/10.1039/D0TB02099K
Xiao Hu, Qiang Lu, Sun L, Cebe P, Wang X, Zhang X, Kaplan DL (2010) Biomaterials from ultrasonication-induced silk fibroin−hyaluronic acid hydrogels. Biomacromol 11(11):3178–3188. https://doi.org/10.1021/bm1010504
Chouhan D, Lohe T-u, Samudrala PK, Mandal BB (2018) In situ forming injectable silk fibroin hydrogel promotes skin regeneration in full thickness burn wounds. Adv Healthc Mater 7(24):1801092. https://doi.org/10.1002/adhm.201801092
Kim U-J, Park J, Li C, Jin H-J, Valluzzi R, Kaplan DL (2004) Structure and properties of silk hydrogels. Biomacromol 5(3):786–792
Sun W, Incitti T, Migliaresi C, Quattrone A, Casarosa S, Motta A (2016) Genipin-crosslinked gelatin–silk fibroin hydrogels for modulating the behaviour of pluripotent cells. J Tissue Eng Regenerat Med 10(10):876–887. https://doi.org/10.1002/term.1868
Wang Y, Niu C, Shi J, Wenlong Yu, Zhu C, Zhang Q, Mizuno M (2021) A carbodiimide cross-linked silk fibroin/sodium alginate composite hydrogel with tunable properties for sustained drug delivery. Macromol Mater Eng 306(11):2100470. https://doi.org/10.1002/mame.202100470
Lin Y, Xia X, Shang Ke, Elia R, Huang W, Cebe P, Leisk G, Omenetto F, Kaplan DL (2013) Tuning chemical and physical cross-links in silk electrogels for morphological analysis and mechanical reinforcement. Biomacromol 14(8):2629–2635. https://doi.org/10.1021/bm4004892
Wen Z, Jiang F, Feng Wu, Yin Z, Kaur K, Chakraborty J, Ghosh S, Shenzhou Lu (2020) Photocurable silk fibroin-polyvinylpyrrolidone hydrogel. Materialia 9:100525. https://doi.org/10.1016/j.mtla.2019.100525
Kuang D, Jiang F, Feng Wu, Kaur K, Ghosh S, Kundu SC, Shenzhou Lu (2019) Highly elastomeric photocurable silk hydrogels. Int J Biol Macromol 134:838–845. https://doi.org/10.1016/j.ijbiomac.2019.05.068
Nier Wu, Huilei Yu, Sun M, Li Z, Zhao F, Ao Y, Chen H (2019) Investigation on the structure and mechanical properties of highly tunable elastomeric silk fibroin hydrogels cross-linked by γ-ray radiation. ACS Appl Bio Mater 3(1):721–734. https://doi.org/10.1021/acsabm.9b01062
Kim MH, Kim BS, Lee J, Donghwan Cho Oh, Kwon H, Park WH (2017) Silk fibroin/hydroxyapatite composite hydrogel induced by gamma-ray irradiation for bone tissue engineering. Biomater Res 21(1):1–9. https://doi.org/10.1186/s40824-017-0098-2
Chirila TV, Suzuki S, Papolla C (2017) A comparative investigation of Bombyx mori silk fibroin hydrogels generated by chemical and enzymatic cross-linking. Biotechnol Appl Biochem 64(6):771–781. https://doi.org/10.1002/bab.1552
Grabska-Zielińska S, Sionkowska A (2021) How to improve physico-chemical properties of silk fibroin materials for biomedical applications?—blending and cross-linking of silk fibroin—a review. Materials 14(6):1510. https://doi.org/10.3390/ma14061510
Gonzalez ACDO, Costa TF, Andrade ZDA, Medrado ARAP (2016) Wound healing-a literature review. An Bras Dermatol 91:614–620
Ghomi ER, Khalili S, Khorasani SN, Neisiany RE, Ramakrishna S (2019) Wound dressings: current advances and future directions. J Appl Polym Sci 136(27):47738. https://doi.org/10.1002/app.47738
Gholipourmalekabadi M, Sapru S, Samadikuchaksaraei A, Reis RL, Kaplan DL, Kundu SC (2020) Silk fibroin for skin injury repair: where do things stand? Adv Drug Deliv Rev 153:28–53. https://doi.org/10.1016/j.addr.2019.09.003
Saghazadeh S, Rinoldi C, Schot M, Kashaf SS, Sharifi F, Jalilian E, Nuutila K, Giatsidis G, Mostafalu P et al (2018) Drug delivery systems and materials for wound healing applications. Adv Drug Deliv Rev 127:138–166. https://doi.org/10.1016/j.addr.2018.04.008
Unger RE, Ghanaati S, Orth C, Sartoris A, Barbeck M, Halstenberg S, Motta A, Migliaresi C, James Kirkpatrick C (2010) The rapid anastomosis between prevascularized networks on silk fibroin scaffolds generated in vitro with cocultures of human microvascular endothelial and osteoblast cells and the host vasculature. Biomaterials 31(27):6959–6967. https://doi.org/10.1016/j.biomaterials.2010.05.057
Ding Z, Zhang Y, Guo P, Duan T, Cheng W, Guo Y, Zheng X, Guozhong Lu, Qiang Lu et al (2021) Injectable desferrioxamine-laden silk nanofiber hydrogels for accelerating diabetic wound healing. ACS Biomater Sci Eng 7(3):1147–1158. https://doi.org/10.1021/acsbiomaterials.0c01502
Wang Q, Shuiqing Zhou Lu, Wang RY, Yan S, Zhang Q, Li M (2021) Bioactive silk fibroin scaffold with nanoarchitecture for wound healing. Compos Part B: Eng 224:109165. https://doi.org/10.1016/j.compositesb.2021.109165
Farokhi M, Mottaghitalab F, Fatahi Y, Khademhosseini A, Kaplan DL (2018) Overview of silk fibroin use in wound dressings. Trends Biotechnol 36(9):907–922. https://doi.org/10.1016/j.tibtech.2018.04.004
Park YR, Sultan MT, Park HJ, Lee JM, Hyung Woo Ju, Lee OJ, Lee DJ, Kaplan DL, Park CH (2018) NF-κB signaling is key in the wound healing processes of silk fibroin. Acta Biomater 67:183–195. https://doi.org/10.1016/j.actbio.2017.12.006
He S, Shi D, Han Z, Dong Z, Xie Y, Zhang F, Zeng WenXin, Yi Q (2019) Heparinized silk fibroin hydrogels loading FGF1 promote the wound healing in rats with full-thickness skin excision. Biomed Eng Online 18(1):1–12. https://doi.org/10.1186/s12938-019-0716-4
Kundu B, Kurland NE, Bano S, Patra C, Engel FB, Yadavalli VK, Kundu SC (2014) Silk proteins for biomedical applications: bioengineering perspectives. Progress Polym Sci 39(2):251–267. https://doi.org/10.1016/j.progpolymsci.2013.09.002
Numata K, Katashima T, Sakai T (2011) State of water, molecular structure, and cytotoxicity of silk hydrogels. Biomacromol 12(6):2137–2144. https://doi.org/10.1021/bm200221u
Wang X, Kluge JA, Leisk GG, Kaplan DL (2008) Sonication-induced gelation of silk fibroin for cell encapsulation. Biomaterials 29(8):1054–1064. https://doi.org/10.1016/j.biomaterials.2007.11.003
Leal-Egana A, Scheibel T (2012) Interactions of cells with silk surfaces. J Mater Chem 22(29):14330–14336. https://doi.org/10.1039/C2JM31174G
Deptuch T, Florczak A, Lewandowska A, Leporowska E, Penderecka K, Marszalek A, Mackiewicz A, Dams-Kozlowska H (2021) MS1-type bioengineered spider silk nanoparticles do not exhibit toxicity in an in vivo mouse model. Nanomedicine 16(18):1553–1565. https://doi.org/10.2217/nnm-2021-0029
Dams-Kozlowska H, Majer A, Tomasiewicz P, Lozinska J, Kaplan DL, Mackiewicz A (2013) Purification and cytotoxicity of tag-free bioengineered spider silk proteins. J Biomed Mater Res Part A 101(2):456–464. https://doi.org/10.1002/jbm.a.34353
Westermark P, Lundmark K, Westermark GT (2009) Fibrils from designed non-amyloid-related synthetic peptides induce AA-amyloidosis during inflammation in an animal model. PLoS ONE 4(6):e6041. https://doi.org/10.1371/journal.pone.0006041
Katarzyna Lundmark, Gunilla T Westermark, Arne Olsén, and Per Westermark, Protein fibrils in nature can enhance amyloid protein A amyloidosis in mice: Cross-seeding as a disease mechanism. Proceedings of the National Academy of Sciences, 2005. 102(17): p. 6098–6102,www.pnas.org/cgi/doi/https://doi.org/10.1073/pnas.0501814102.
Coelho F, Cavicchioli M, Specian SS, Cilli EM, Ribeiro SJL, Scarel-Caminaga RM, SidorenkoOliveira Capot T (2020) Silk fibroin/hydroxyapatite composite membranes: production, characterization and toxicity evaluation. Toxicol Vitro 62:104670. https://doi.org/10.1016/j.tiv.2019.104670
Naserzadeh P, Mortazavi SA, Ashtari K, Salimi A, Farokhi M, Pourahmad J (2018) Evaluation of the toxicity effects of silk fibroin on human lymphocytes and monocytes. J Biochem Mol Toxicol 32(6):e22056. https://doi.org/10.1002/jbt.22056
Naserzadeh P, Mortazavi SA, Ashtari K, Seydi E, Pourahmad J (2018) Evaluation of the toxicity effects of silk fibroin on isolated fibroblast and huvec cells. Iran J Pharm Res 17(Suppl2):134
Reddy N, Reddy R, Jiang Q (2015) Crosslinking biopolymers for biomedical applications. Trends Biotechnol 33(6):362–369. https://doi.org/10.1016/j.tibtech.2015.03.008
Samouillan V, Dandurand-Lods J, Lamure A, Maurel E, Lacabanne C, Gerosa G, Venturini A, Casarotto D, Gherardini L et al (1999) Thermal analysis characterization of aortic tissues for cardiac valve bioprostheses. J Biomed Mater Res 46(4):531–538. https://doi.org/10.1002/(SICI)1097-4636(19990915)46:4
Yan LP, Silva-Correia J, Ribeiro VP, Miranda-Gonçalves V, Correia C, da Silva Morais A, Sousa RA, Reis RM, Oliveira AL et al (2016) Tumor growth suppression induced by biomimetic silk fibroin hydrogels. Sci Rep 6(1):31037. https://doi.org/10.1038/srep31037
Yan H-B, Zhang Y-Q, Ma Y-L, Zhou L-X (2009) Biosynthesis of insulin-silk fibroin nanoparticles conjugates and in vitro evaluation of a drug delivery system. J Nanopart Res 11(8):1937–1946. https://doi.org/10.1007/s11051-008-9549-y
Wongpinyochit T, Johnston BF, Philipp Seib F (2016) Manufacture and drug delivery applications of silk nanoparticles. J Visual Exp 116:e54669. https://doi.org/10.3791/54669
Gobin AS, Rhea R, Newman RA, Mathur AB (2006) Silk-fibroin-coated liposomes for long-term and targeted drug delivery. Int J Nanomed 1(1):81. https://doi.org/10.2147/nano.2006.1.1.81
Puyuan Wu, Liu Q, Li R, Jing Wang Xu, Zhen GY, Wang H, Cui F, Fenglei Wu et al (2013) Facile preparation of paclitaxel loaded silk fibroin nanoparticles for enhanced antitumor efficacy by locoregional drug delivery. ACS Appl Mater Interfaces 5(23):12638–12645. https://doi.org/10.1021/am403992b
Andiappan M, Sundaramoorthy S, Panda N, Meiyazhaban G, Winfred SB, Venkataraman G, Krishna P (2013) Electrospun eri silk fibroin scaffold coated with hydroxyapatite for bone tissue engineering applications. Progress Biomater 2(1):1–11. https://doi.org/10.1186/2194-0517-2-6
Lv XiangGuo, Li Z, Chen ShiYan, Xie MinKai, Huang JianWen, Peng XuFeng, Yang RanXing, Wang HuaPing, YueMin Xu et al (2016) Structural and functional evaluation of oxygenating keratin/silk fibroin scaffold and initial assessment of their potential for urethral tissue engineering. Biomaterials 84:99–110. https://doi.org/10.1016/j.biomaterials.2016.01.032
Yun Gu, Zhu J, Xue C, Li Z, Ding F, Yang Y, Xiaosong Gu (2014) Chitosan/silk fibroin-based, Schwann cell-derived extracellular matrix-modified scaffolds for bridging rat sciatic nerve gaps. Biomaterials 35(7):2253–2263. https://doi.org/10.1016/j.biomaterials.2013.11.087
Zhang K, Jinglei W, Huang C, Mo X (2013) Fabrication of silk fibroin/P (LLA-CL) aligned nanofibrous scaffolds for nerve tissue engineering. Macromol Mater Eng 298(5):565–574
Kuihua Zhang Wu, Jinglei CH, Mo X (2013) Fabrication of silk fibroin/P (LLA-CL) aligned nanofibrous scaffolds for nerve tissue engineering. Macromol Mater Eng 298(5):565–574. https://doi.org/10.1002/mame.201200038
Nune M, Manchineella S, Govindaraju T, Narayan KS (2019) Melanin incorporated electroactive and antioxidant silk fibroin nanofibrous scaffolds for nerve tissue engineering. Mater Sci Eng: C 94:17–25
Lv Q, Feng Q, Kun Hu, Cui F (2005) Three-dimensional fibroin/collagen scaffolds derived from aqueous solution and the use for HepG2 culture. Polymer 46(26):12662–12669. https://doi.org/10.1016/j.polymer.2005.10.137
Lv Q, Kun Hu, Feng Q, Cui F, Cao C (2007) Preparation and characterization of PLA/fibroin composite and culture of HepG2 (human hepatocellular liver carcinoma cell line) cells. Compos Sci Technol 67(14):3023–3030. https://doi.org/10.1016/j.compscitech.2007.05.003
Chang G, Kim HJ, Vunjak-Novakovic G, Kaplan DL, Kandel R (2010) Enhancing annulus fibrosus tissue formation in porous silk scaffolds. J Biomed Mater Res Part A 92(1):43–51. https://doi.org/10.1002/jbm.a.32326
Chung T-W, Chen W-P, Tai P-W, Lo H-Y, Ting-Ya Wu (2020) Roles of silk fibroin on characteristics of hyaluronic acid/silk fibroin hydrogels for tissue engineering of nucleus pulposus. Materials 13(12):2750. https://doi.org/10.3390/ma13122750
Ribeiro M, De Moraes MA, Beppu MM, Garcia MP, Fernandes MH, Monteiro FJ, Ferraz MP (2015) Development of silk fibroin/nanohydroxyapatite composite hydrogels for bone tissue engineering. Eur Polym J 67:66–77. https://doi.org/10.1016/j.eurpolymj.2015.03.056
Jin Y, Kundu B, Cai Y, Kundu SC, Yao J (2015) Bio-inspired mineralization of hydroxyapatite in 3D silk fibroin hydrogel for bone tissue engineering. Colloids Surfaces B: Biointerfaces 134:339–345. https://doi.org/10.1016/j.colsurfb.2015.07.015
Zhou Y, Liang K, Zhao S, Zhang C, Li J, Yang H, Liu X, Yin X, Chen D et al (2018) Photopolymerized maleilated chitosan/methacrylated silk fibroin micro/nanocomposite hydrogels as potential scaffolds for cartilage tissue engineering. Int J Biol Macromol 108:383–390. https://doi.org/10.1016/j.ijbiomac.2017.12.032
Wang Lu, Rongjian Lu, Hou J, Nan X, Xia Y, Guo Y, Meng K, Changzhen Xu, Wang X et al (2020) Application of injectable silk fibroin/graphene oxide hydrogel combined with bone marrow mesenchymal stem cells in bone tissue engineering. Colloids Surfaces A: Physicochem Eng Aspects 604:125318. https://doi.org/10.1016/j.colsurfa.2020.125318
Acknowledgements
The authors would like to thank the faculty of advanced technologies in medicine, Iran University of Medical Sciences colleagues, for their valuable assistance.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The author reports no conflicts of interest in this work.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Afjeh-Dana, E., Javadmoosavi, S.A., Rahvar, M. et al. Nanostructures and biomaterials based on silk polymer for medical diagnostic and therapeutic applications. Polym. Bull. 81, 4737–4769 (2024). https://doi.org/10.1007/s00289-023-04949-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00289-023-04949-5