Abstract
Background
3D bone reconstructions performed during general clinical practice are of limited use for preclinical research, education, and training purposes. For this reason, we are constructing a database of human 3D virtual bone models compiled from computer tomography (CT) scans.
Materials and methods
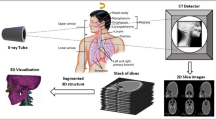
CT data sets were post-processed using Amira® 5.2 software. In each cut, bone structures were isolated using semiautomatic labeling program codes. The software then generated extremely precise 3D bone models in STL format (standard triangulated language). These bone models offer a sustainable source of information for morphologic studies and investigations of biomechanical bony characteristics in complex anatomic regions. Regarding educational value and student acceptance models were introduced during bedside teaching and evaluated by medical students.
Results
The current database is comprised of 131 pelvises and 120 femurs (ø 60 years, ø 172 cm, ø 76 kg), and is continuously growing. To date, 3D morphometric analyses of the posterior ring and the acetabulum have been successfully completed. Eighty students (96 %) evaluated instruction with virtual 3D bone models as “good” or “very good“. The majority of students want to increase learning with virtual bone models covering various regions and diseases.
Conclusion
With consistent and steadily increasing case numbers, the database offers a sustainable alternative to human cadaver work for practical investigations. In addition, it offers a platform for education and training.



Similar content being viewed by others
References
Blake T (1977) Motion in instructional media: some subject-display mode interactions. Percept Mot Skills 44:975–985
Jerosch J, Wetzel R, Aldinger G, Weipert A, Hanusek S, Filler TJ, Peuker ET (2000) Virtual simulation for optimizing the range of motion in hip alloarthroplasty using an adapted thrust-plate prosthesis model. Der Orthopade 29(7):605–613
Kamer L, Noser H, Schramm A, Hammer B (2010) Orbital form analysis: problems with design and positioning of precontoured orbital implants: a serial study using post-processed clinical CT data in unaffected orbits. Int J Oral Maxillofac Surg 39(7):666–672. doi:10.1016/j.ijom.2010.03.005
Kamer L, Noser H, Schramm A, Hammer B, Kirsch E (2010) Anatomy-based surgical concepts for individualized orbital decompression surgery in graves orbitopathy. I. Orbital size and geometry. Ophthalmic Plast Reconstr Surg 26(5):348–352. doi:10.1097/IOP.0b013e3181c9bb52
Kwan MK, Jeffry A, Chan CY, Saw LB (2012) A radiological evaluation of the morphometry and safety of S1, S2 and S2-ilium screws in the Asian population using three dimensional computed tomography scan: an analysis of 180 pelvis. Surg Radiol Anat SRA 34(3):217–227. doi:10.1007/s00276-011-0919-2
Lewalter D (1997) Lernen mit Bildern und Animationen. Studie zum Einfluß von Lernmerkmalen auf die Effektivität von Illustrationen, vol 1. Waxmann, Münster
Mendel T, Noser H, Wohlrab D, Stock K, Radetzki F (2011) The lateral sacral triangle–a decision support for secure transverse sacroiliac screw insertion. Injury 42(10):1164–1170
Mittelmeier W, Peters P, Ascherl R, Gradinger R (1997) Rapid prototyping. Construction of a model in the preoperative planning of reconstructive pelvic interventions. Der Orthopade 26(3):273–279
Noser H, Heldstab T, Schmutz B, Kamer L (2011) Typical accuracy and quality control of a process for creating CT-based virtual bone models. J Digit Imaging 24(3):437–445. doi:10.1007/s10278-010-9287-4
Noser H, Radetzki F, Stock K, Mendel T (2011) A method for computing general sacroiliac screw corridors based on CT scans of the pelvis. J Digit Imaging 24(4):665–671. doi:10.1007/s10278-010-9327-0
Rathnayaka K, Momot KI, Noser H, Volp A, Schuetz MA, Sahama T, Schmutz B (2012) Quantification of the accuracy of MRI generated 3D models of long bones compared to CT generated 3D models. Med Eng Phys 34(3):357–363. doi:10.1016/j.medengphy.2011.07.027
Rieber LP (1991) Animation, incidental learning, and continuing motivation. J Educ Psychol 83(3):318–328
Rieber LP, Kini AS (1991) Theoretical foundations of instructional applications of computer-generated animated visuals. J Comput Based Instr 18(3):83–88
Savoldelli C, Bouchard PO, Loudad R, Baque P, Tillier Y (2012) Stress distribution in the temporo-mandibular joint discs during jaw closing: a high-resolution three-dimensional finite-element model analysis. Surg radiol anat SRA 34(5):405–413. doi:10.1007/s00276-011-0917-4
Schmutz B, Rathnayaka K, Wullschleger ME, Meek J, Schuetz MA (2010) Quantitative fit assessment of tibial nail designs using 3D computer modelling. Injury 41(2):216–219. doi:10.1016/j.injury.2009.10.012
Schmutz B, Wullschleger ME, Kim H, Noser H, Schutz MA (2008) Fit assessment of anatomic plates for the distal medial tibia. J Orthop Trauma 22(4):258–263. doi:10.1097/BOT.0b013e31816b10ba
Seddon G, Eniaiyeju PA, Jusoh I (2009) The visualization of rotation in diagrams of threedimensional structures. Am Educ Res J 21:25–28
Seebeck J, Goldhahn J, Stadele H, Messmer P, Morlock MM, Schneider E (2004) Effect of cortical thickness and cancellous bone density on the holding strength of internal fixator screws. J Orthop Res Off Publ Orthop Res Soc 22(6):1237–1242. doi:10.1016/j.orthres.2004.04.001
Surber SR, Leeder JA (1988) The effect of graphic feedback on student motivation. J Comp Based Instr 15(1):14–17
Tam MD (2010) Building virtual models by postprocessing radiology images: a guide for anatomy faculty. Anat Sci Educ 3(5):261–266. doi:10.1002/ase.175
Trelease RB, Rosset A (2008) Transforming clinical imaging data for virtual reality learning objects. Anat Sci Educ 1(2):50–55. doi:10.1002/ase.13
Wohlrab D, Radetzki F, Noser H, Mendel T (2012) Cup positioning in total hip arthoplasty: spatial alignment of the acetabular entry plane. Arch Orthop Trauma Surg 132(1):1–7. doi:10.1007/s00402-011-1379-1
Yagci AB, Kiroglu Y, Ozdemir B, Kara CO (2008) Three-dimensional computed tomography of a complete stylohyoid ossification with articulation. Surg Radiol Anat Sra 30(2):167–169. doi:10.1007/s00276-008-0302-0
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Radetzki, F., Mendel, T., Noser, H. et al. Potentialities and limitations of a database constructing three-dimensional virtual bone models. Surg Radiol Anat 35, 963–968 (2013). https://doi.org/10.1007/s00276-013-1118-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00276-013-1118-0