Abstract
Purpose
Rhenium-186 (186Re) and rhenium-188 (188Re) are promising radionuclides for the inhibition of restenosis after percutaneous transluminal angioplasty or other vascular interventions. Until now the maximal dose tolerance of endothelial cells has not been clearly known.
Materials and Methods
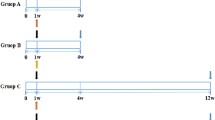
To characterize the effects of local irradiation treatment, human aortic endothelial cells (ECs) were incubated with different doses of 186Re and 188Re. Two days after plating, ECs received treatment for a period of 5 days. The total radiation doses applied were 1, 4, 8, 16, and 32 Gy. On days 1, 3, 5, 7, and 12 after initial rhenium incubation, cell growth, clonogenic activity, cell-cycle distribution, and cytoskeletal architecture were evaluated.
Results
From the first day on, a dose-dependent growth inhibition was observed. Cumulative doses of ≥32 Gy caused a weak colony formation and significant alterations in the cytoskeletal architecture. An increased fraction of cells in G2/M phase was seen for cumulative radiation doses of ≥16 Gy. Interestingly, there were no significant differences between 186Re and 188Re.
Conclusion
Even for low dose rates of β particles a dose-dependent proliferation inhibition of ECs is seen. Doses beyond 32 Gy alter the cytoskeletal architecture with possibly endothelial dysfunction and late thrombosis.





Similar content being viewed by others
References
Patel SD, Waltham M, Wadoodi A et al (2010) The role of endothelial cells and their progenitors in intimal hyperplasia. Ther Adv Cardiovasc Dis 4:129–141
Shoji M, Sata M, Fukuda D et al (2004) Temporal and spatial characterization of cellular constituents during neointimal hyperplasia after vascular injury: potential contribution of bone-marrow-derived progenitors to arterial remodeling. Cardiovasc Pathol 13:306–312
Smith SH, Geer JC (1983) Morphology of saphenous vein–coronary artery bypass grafts: seven to 116 months after surgery. Arch Pathol Lab Med 107:13–18
Landmesser U, Hornig B, Drexler H (2004) Endothelial function: a critical determinant in atherosclerosis? Circulation 109:27–33
Patti G, Pasceri V, Melfi R et al (2005) Impaired flow-mediated dilation and risk of restenosis in patients undergoing coronary stent implantation. Circulation 111:70–75
McEver RP, Cummings RD (1997) Role of PSGL-1 binding to selectins in leukocyte recruitment. J Clin Invest 100:S97–S103
Welt FG, Rogers C (2002) Inflammation and restenosis in the stent era. Arterioscler Thromb Vasc Biol 22:1769–1776
Werner N, Junk S, Laufs U et al (2003) Intravenous transfusion of endothelial progenitor cells reduces neointima formation after vascular injury. Circ Res 93:e17–e24
Bonetti PO, Lerman LO, Lerman A (2003) Endothelial dysfunction: a marker of atherosclerotic risk. Arterioscler Thromb Vasc Biol 23:168–175
Snow AD, Bolender RP, Wight TN, Clowes AW (1990) Heparin modulates the composition of the extracellular matrix domain surrounding arterial smooth muscle cells. Am J Pathol 137:313–330
Costa MA, Simon DI (2005) Molecular basis of restenosis and drug-eluting stents. Circulation 111:2257–2273
Liermann D, Bottcher HD, Kollath J et al (1994) Prophylactic endovascular radiotherapy to prevent intimal hyperplasia after stent implantation in femoropopliteal arteries. Cardiovasc Intervent Radiol 17:12–16
Wohlgemuth WA, Leissner G, Wengenmair H et al (2008) Endovascular brachytherapy in the femoropopliteal segment using 192Ir and 188Re. Cardiovasc Intervent Radiol 31:698–708
Wyttenbach R, Gallino A, Alerci M et al (2004) Effects of percutaneous transluminal angioplasty and endovascular brachytherapy on vascular remodeling of human femoropopliteal artery by noninvasive magnetic resonance imaging. Circulation 110:1156–1161
Christen T, Verin V, Bochaton-Piallat M et al (2001) Mechanisms of neointima formation and remodeling in the porcine coronary artery. Circulation 103:882–888
Koshy SK, Kleiman NS, George LK et al (2008) Vascular changes and black hole phenomenon after coronary brachytherapy: a pathologically distinct entity. J Invasive Cardiol 20:560–562
Wohlgemuth WA, Bohndorf K (2003) Endovascular brachytherapy to prevent restenosis after angioplasty. Rofo 175:246–252
Sureka CS, Sunny CS, Subbaiah KV et al (2007) Dose distribution for endovascular brachytherapy using Ir-192 sources: comparison of Monte Carlo calculations with radiochromic film measurements. Phys Med Biol 52:525–537
Hsieh BT, Hsieh JF, Tsai SC et al (1999) Rhenium-188-labeled DTPA: a new radiopharmaceutical for intravascular radiation therapy. Nucl Med Biol 26:967–972
Eriksson JE, Dechat T, Grin B et al (2009) Introducing intermediate filaments: from discovery to disease. J Clin Invest 119:1763–1771
Meyer JM, Nowak B, Schuermann K et al (2003) Inhibition of neointimal proliferation with 188Re-labeled self-expanding nitinol stent in a sheep model. Radiology 229:847–854
Fareh J, Martel R, Kermani P, Leclerc G (1999) Cellular effects of beta-particle delivery on vascular smooth muscle cells and endothelial cells: a dose-response study. Circulation 99:1477–1484
Albiero R, Nishida T, Adamian M et al (2000) Edge restenosis after implantation of high activity 32P radioactive beta-emitting stents. Circulation 101:2454–2457
Kotzerke J, Gertler R, Buchmann I et al (2000) Different radiosensitivity of smooth muscle cells and endothelial cells in vitro as demonstrated by irradiation from a Re-188 filled balloon catheter. Atherosclerosis 152:35–42
van Tongeren RB, van Sambeek MR, van Overhagen H et al (2005) Endovascular brachytherapy for the prevention of restenosis after femoropopliteal angioplasty. Results of the VARA trial. J Cardiovasc Surg 46:437–443
Hall EJ, Miller RC, Brenner DJ (1999) Radiobiological principles in intravascular irradiation. Cardiovasc Radiat Med 1:42–47
Henning E, Dittmann H, Wiskirchen J et al (2004) Dose dependent effects of the combined beta-gamma-emitter 188rhenium on the growth of human vessel wall cells. Rofo 176:404–408
Kehlbach R, Dittmann H, Schmid T et al (2006) Early effects of rhenium-188 treatment on proliferation, migration, and matrix synthesis of cultured human aortic smooth muscle cells. Strahlenther Onkol 182:164–171
Milliat F, Francois A, Isoir M et al (2006) Influence of endothelial cells on vascular smooth muscle cells phenotype after irradiation: implication in radiation-induced vascular damages. Am J Pathol 169:1484–1495
Wiskirchen J, Dittmann H, Kehlbach R et al (2001) Rhenium-188 for inhibition of human aortic smooth muscle cell proliferation. Int J Radiat Oncol Biol Phys 49:809–815
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Sauter, A., Arthasana, D., Dittmann, H. et al. In Vitro Comparison of the Antiproliferative Effects of Rhenium-186 and Rhenium-188 on Human Aortic Endothelial Cells. Cardiovasc Intervent Radiol 34, 816–823 (2011). https://doi.org/10.1007/s00270-010-0003-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00270-010-0003-z