Abstract
Background
Understanding the burden of diseases requiring surgical care at national levels is essential to advance universal health coverage. The PREvalence Study on Surgical COnditions (PRESSCO) 2020 is a cross-sectional household survey to estimate the prevalence of physical conditions needing surgical consultation, to investigate healthcare-seeking behavior, and to assess changes from before the West African Ebola epidemic.
Methods
This study (ISRCTN: 12353489) was built upon the Surgeons Overseas Surgical Needs Assessment (SOSAS) tool, including expansions. Seventy-five enumeration areas from 9671 nationwide clusters were sampled proportional to population size. In each cluster, 25 households were randomly assigned and visited. Need for surgical consultations was based on verbal responses and physical examination of selected household members.
Results
A total of 3,618 individuals from 1,854 households were surveyed. Compared to 2012, the prevalence of individuals reporting one or more relevant physical conditions was reduced from 25 to 6.2% (95% CI 5.4–7.0%) of the population. One-in-five conditions rendered respondents unemployed, disabled, or stigmatized. Adult males were predominantly prone to untreated surgical conditions (9.7 vs. 5.9% women; p < 0.001). Financial constraints were the predominant reason for not seeking care. Among those seeking professional health care, 86.7% underwent surgery.
Conclusion
PRESSCO 2020 is the first surgical needs household survey which compares against earlier study data. Despite the 2013–2016 Ebola outbreak, which profoundly disrupted the national healthcare system, a substantial reduction in reported surgical conditions was observed. Compared to one-time measurements, repeated household surveys yield finer granular data on the characteristics and situations of populations in need of surgical treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Understanding the surgical disease burden and care options available for patients in low- and middle-income countries (LMICs) is vital to raise awareness on the magnitude of treatable conditions and to allocate resources for safeguarding essential surgical services [1].
According to the 2012 Sierra Leone Surgeons Overseas Surgical Needs Assessment (SOSAS), 25% of respondents indicated that they were in need of surgical care at the time of the interview [2]. Since 2012, Sierra Leone has experienced shocks to its health system, most notably the 2013–2016 West African Ebola Virus Disease (EVD) outbreak during which healthcare provision was disrupted, and health-seeking behavior severely altered [3,4,5,6]. However, there have also been several major interventions strengthening the health system in Sierra Leone during the past decade. Examples within the surgical domain include the expansion of a surgical task-sharing training program [7, 8], employment of regionally hired medical doctors to support first-level hospitals [9, 10], implementation of a health finance protection scheme [11], and the establishment of national ambulance and emergency services [12].
The PREvalence Study on Surgical COnditions 2020 (PRESSCO 2020) is a replication of the the SOSAS survey [2] and expanded with additional survey topics and a physical examination. The aim of PRESSCO 2020 was to assess the prevalence of physical conditions needing surgical attention and changes over the past decade in Sierra Leone. The type of surgical condition and associated anatomical location, health-seeking behavior, and reasons for not receiving surgical care were also investigated.
Methods
Located in West Africa, Sierra Leone has a population of 8.3 million and is considered a low-income country [13, 14]. Between October 2019 and March 2020, we conducted a population-based cross-sectional household survey in Sierra Leone.
Sample size calculation
Sample size calculation was identical with the SOSAS study [2], resulting in an estimated sample size of 3745 individuals. Out of a total of 9671 nationwide clusters, the lowest administrative unit, Statistics Sierra Leone (Stats SL), the governmental institution in charge of statistics and census data, sampled 75 enumeration areas (EA). To select an EA with a probability proportional to the population size, a weighted random cluster design was used. All EAs were located using a global positioning system. Within each cluster, all the households were counted, and 25 households were randomly selected. For each household, a random calculator assigned two household members. A household was defined as one or more people, living together, sharing meals and sleeping in the same structure the night before the interview. If a selected household member was not present, the household was visited up to four times before assigning another household member.
Study design
PRESSCO 2020 applied the validated SOSAS tool [2, 15]. Based on the self-critique that all data were previously obtained after a verbal examination only, a physical examination was added. This examination was performed if a groin hernia was suspected, when a wound had a diameter of ≥ 5 cm, or was present ≥ 1 month, and to assess the fundal height of pregnant women. Other local adaptions included additional questions on five disease-specific survey topics and blood pressure measurements [16]. Findings from the additional disease specific health topics will be reported in detail separately.
The first section of the survey included demographic information about all household members, surgical procedures, and deaths for any household member during the past year. For the second section, two randomly selected household members were interviewed on surgical conditions covering: face, head, and neck; chest and breast; abdomen; groin, genitals, and buttocks; back; and extremities. The ‘need for surgical care’ labeling depended on the respondent’s judgment. Need for major surgery referred to conditions that required regional or general anesthesia; other procedures were categorized minor surgery. A referral and transport were arranged when medical conditions in need of immediate attention were diagnosed.
Data were collected by nurses, surgically trained community health officers (SACHO) [8] and employees of Stats SL with previous experience from collecting data for the Sierra Leone Demographic Health Survey. All had Sierra Leonean nationality and collectively received a four-day training, followed by an individual assessment prior to the start of the data collection. Physical examination was performed by SACHOs only. Password protected tablets with mobile internet and software application REDCap (Research Electronic Data Capture; Vanderbilt University, Nashville, TN, USA) were used [17, 18]. At two occasions, retrieved data were checked for completeness and potential flaws; prior to departure from the EA by a field supervisor, and after it was uploaded to a cloud-based server by the study group. Traditional leaders provided community approval. Informed consent was obtained from all respondents or parents in cases of children.
Statistical analysis
Household and individual respondent characteristics were described using central tendency measures, frequencies, and percentages. Findings were compared against earlier study data from 2012 [2]. Bivariate associations were analyzed with Chi-square tests for contingency tables and t-tests for normally distributed data. All tests were conducted as two-tailed, and statistical significance was set at p < 0.05. Stata® 15.1 (StataCorp, College Station, Texas, USA) and Microsoft Excel® (Microsoft, Redmond, Washington, USA) were used.
Ethics
The study was registered with the ISRCTN registry (No. 12353489). Ethics approval was obtained from the Norwegian Regional Committee for Medical and Health Research Ethics (REC (2019/31932), and Sierra Leone Ethics and Scientific Review Committee (SLESRC 2019/October/03).
Results
Enumeration areas
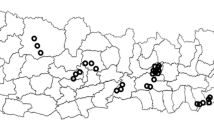
In total, 75 EAs (Fig. 1) were visited between October and November 2019 and between February and March 2020; the 3-month pause was because of a Lassa fever outbreak. Three EAs were substituted as data entries were missing upon checking for completeness by the data quality team. In total, 3618 household members from 1854 households were included for analysis (Fig. 2).
Comparison with SOSAS (2012)
Compared to SOSAS, PRESSCO 2020 included a larger proportion of rural (66.9 vs 61.2%, p < 0.001) households with a smaller household size (mean 5.2 vs 6.4 individuals, p < 0.001) [2]. The distribution of other baseline data did not significantly differ (Table 1). In total, 278 (7.7%, 95% CI 6.8–8.6%) individuals reported 308 surgical conditions ranging from at least having acquired one wound, burn, mass, deformity, to having undergone at least one surgical procedure within the previous year. In Sierra Leone, this means an estimated 564,000 to 713,800 individuals have a surgical condition. At the time of the interview, 223 (6.2%, 95% CI 5.4–7.0%) individuals reported 255 conditions in need of surgical care. Compared to Groen et al. [2] the present study observed the prevalence of individuals reporting one or more possible surgical conditions decreasing from a reported 25% to 6.2%.
Of the 255 physical conditions distributed over six anatomical locations, the most commonly reported surgical conditions were hard and soft masses (85; 33.3%), wounds (72; 28.2%), and acquired deformities (63; 24.7%) (Table 2). Compared to 2012, we documented that both fewer surgical conditions were reported, and a difference in distribution and anatomical location of the reported conditions (p < 0.001). Of the 308 conditions that existed during the last 12 months, 38 (12.3%) left the respondents incapacitated, caused shame (16; 5.2%), or required assistance with daily activities (5; 1.6%) or during transport (2; 0.6%) (Supplementary Table).
Surgical conditions
Surgical conditions were more common among men (9.7 vs 5.9% among women, p < 0.001) and predominantly reported among people older than 18 years. Need for a surgical consultation was equally distributed among members of rural and urban communities (7.8 vs 7.5%; p = 0.842) (Table 3).
Seeking and receiving surgical care
Of the 278 individuals with at least one possible surgical condition, the majority visited a health facility (210, 75.5%). People living in rural areas were more likely to visit a traditional healer compared to those from urban areas (23.8 vs. 9.0%, p = 0.003). Of the 210 respondents visiting a health facility for their suspected surgical condition, 33 (15.7%) and 149 (71.0%) underwent major and minor surgery, respectively.
Reasons for not seeking or receiving surgical care
For 80 (26%) of the 308 reported conditions that occurred during the past year, no care was sought or could be obtained despite visiting a health facility. Insufficient financial resources (48, 60.0%) were the main reason why no care was sought or obtained. Other reasons were a perception that the condition did not require surgical care (19, 23.8%) or lack of confidence in the health system (4, 5.0%) (Supplementary Table).
Deaths
A total of 354 (179 men and 174 women) deaths during the 12 months preceding the survey were reported from 294 households. Based on a mean household size of 5.2, the crude death rate was 36.6 per 1000 population/year (Table 4).
Discussion
Following SOSAS that was performed in Sierra Leone and subsequently has been administered in other LMICs [2, 19,20,21,22], PRESSCO 2020 is the first surgical household survey that can compare its data to an earlier version of the same study. Nearly a decade after its initial surveillance, and 6 years after the onset of the West African EVD outbreak, the number of individuals reporting one or more possible surgical conditions was 6.2%, compared with 25% in 2012 [2]. A prevalence consistent with similar studies from Uganda (10.6%) and Nepal (10.0%), of which the latter survey included a visual physical examination [21, 22]. A validation study from northern Rwanda on a community-based survey including physical examination found an overall specificity of 97.7% for the structured interview [23]. The implied conformity between respondents without reported surgical conditions and absent findings by physical examination suggests that an underestimation of the reported prevalence is less likely.
To track progress on the development of the rapidly changing surgical ecosystem, PRESSCO 2020 re-applied a previously validated questionnaire [22]. When compared to one-time measurements, repeated household surveys yield finer granular data on the characteristics and situations of populations in need of surgical treatment [24]. Repeated household surveys generate timely data for program outcome monitoring and supplement hospital data to gain a better understanding of progress toward universal health coverage and the surgical volume indicator of the Lancet Commission on Global Surgery [1, 25, 26]. PRESSCO 2020 was developed in collaboration with members of SOSAS and carried out in collaboration with Stats SL. Our local adaptations on the SOSAS tool did not result in an increment of study costs [2]. The strengths of this study are that interviews and examinations were conducted by trained and local healthcare personnel and data checking and validation was carried out by a data quality team. The expansion of Sierra Leone’s telephone network during the interim period also facilitated the ease of transmission and verification of study data [27]. However, flaws during data collecting or misreporting of conditions that led to an overestimating of conditions in 2012, or underestimation of the true burden of surgical conditions in 2020 cannot be excluded.
Interpretation
Compared to 2012, attention on access to essential surgical services has increased [25, 26]. However, an unequivocal explanation for the observed decrease in the surgery-requiring physical conditions is hard to provide. PRESSCO’s 2020 additional survey topics, physical examination, expanding from one to three enumerator teams, a total data gathering increase from three to seven weeks, but also more rigorous data checking procedures were the main methodological differences between the studies. Furthermore, except for Malawi, the prevalence of surgical conditions among other SOSAS-derived studies was more in line with the present findings [19,20,21,22]. Across other SOSAS publications, there are, however, discrepancies in the way results are presented, which renders direct comparisons difficult [19,20,21,22]. Four years after SOSAS Rwanda, a comparable survey also including a physical examination was repeated in northern Rwanda. A 12% prevalence of surgically treatable conditions was found among all examined individuals [28]. While more consistent with our finding, Rwanda has a higher HDI ranking (160 vs. 182 for Sierra Leone), and 70–80% of the population are enrolled in a community-based health insurance, covering in-and-outpatient services [14, 29]. This could suggest that our reported prevalence might lean on the low side; however, the data concerned came from only one district in Rwanda, and comparability of each dataset is unclear.
The gradual annual increase in health spending per capita might have been another contributing factor to the reduced surgical need. That notwithstanding, expenditures during and after the EVD outbreak were mainly due to external aid [30], and out-of-pocket payments remained responsible for roughly 45% of all healthcare-related expenses [31]. This is despite the rollout of the Free Health Care Initiative (FHCI) for pregnant women, lactating mothers, under five children and recently EVD survivors [11, 32]. If FHCI did not exist, 66.8% of women in Sierra Leone would experience catastrophic health expenditures [33]. As 60% of the reasons provided for not seeking health care were financial concerns, expanding the FHCI beneficiaries’ group [34], providing in-hospital meals for patients, facilitating road access to health clinics, and initiating a community-based health insurance are important [35].
Health system-strengthening initiatives [9,10,11,12], including the establishment of a task-sharing surgical training program in 2011 [8], nearly doubled the surgical workforce and enhanced the annual surgical volume by 15.6% to approximately 28.000 operations in 2017 [36]. Based on our findings, 86.7% of the people who visited the hospital actually underwent an operation. This high percentage suggests that people only visit the hospital when it is absolutely necessary. Consequently, 20% of the reported surgical conditions rendered respondents unemployed, disabled, or stigmatized—meaning that failure to amend surgical conditions in Sierra Leone has a negative effect on the country’s capacity to meet the SDG objectives; specifically, for inclusion, when so meeting the health needs of so many marginalized groups are a critical element to ending poverty [1, 37]. It is desirable to standardize collecting and reporting nationally representative data on surgical access [38]. Ideally, one validated surgical survey would be added as a special focus topic within the Demographic and Health Surveys (DHS) Program. In 2018, Zambia demonstrated that this was feasible [39].
Limitations
A sub-analysis of the 2015 Global Burden of Disease study demonstrated a female/male ratio in the prevalence of surgical conditions of approximately 3:1 [40]. We found that surgical conditions were mostly reported by men. As men fall outside the FHCI beneficiaries’ group, this may contribute to their predominant presence among the respondents with a physical complaint. It is also plausible that healthy men could not be included as they worked away from home, which could have led to a selection bias. In comparison with SOSAS, the ranking of conditions and reported anatomical locations differed. These differences may be explained by minor differences in how patient’s history was taken, which could limit the internal validity of the survey. Lastly, the PRESSCO 2020 tool is not validated and surveys may not be as adept in explaining why people think or act as they do [41]. While surveys can tell how many respondents had a possible surgical condition or had surgery, they can be limited in the information they can provide in terms of personal reasons and sociocultural factors. It might have been better to answer these questions through qualitative research that is ethnographically informed [41].
PRESSCO 2020 is the first household survey into surgical need, which can compare its data to an earlier study. The reported prevalence was consistent with data from recent similar studies in other LMICs. Compared with 2012, the proportion of people with a surgical condition was found to be lower. Repeated household surveys related to health may help to properly measure and monitor surgery-related indicators in LMICs.
References
Roa L, Jumbam DT, Makasa E, Meara JG (2019) Global surgery and the sustainable development goals. Br J Surg 106(2):e44–e52. https://doi.org/10.1002/bjs.11044
Groen RS, Samai M, Stewart KA et al (2012) Untreated surgical conditions in Sierra Leone: a cluster randomised, cross-sectional, countrywide survey. Lancet 380(9847):1082–1087. https://doi.org/10.1016/S0140-6736(12)61081-2
Parpia AS, Ndeffo-Mbah ML, Wenzel NS, Galvani AP (2016) Effects of response to 2014–2015 ebola outbreak on deaths from malaria, HIV/AIDS, and tuberculosis. West Africa. Emerg Infectious Dis 22(3):433–441. https://doi.org/10.3201/eid2203.150977
Brolin Ribacke KJ, van Duinen AJ, Nordenstedt H et al (2013) The impact of the West Africa Ebola outbreak on obstetric health care in Sierra Leone. PLoS ONE 11(2). https://doi.org/10.1371/journal.pone.0150080
Bolkan HA, van Duinen A, Samai M et al (2018) Admissions and surgery as indicators of hospital functions in Sierra Leone during the west-African Ebola outbreak. BMC Health Services Res 18(1). https://doi.org/10.1186/s12913-018-3666-9
Huizenga E, van der Ende J, Zwinkels N et al (2019) A modified case definition to facilitate essential hospital care during Ebola outbreaks. Clin Infect Dis 68(10):1763–1768. https://doi.org/10.1093/cid/ciy798/5100701
Bolkan HA, von Schreeb J, Samai MM et al (2015) Met and unmet needs for surgery in Sierra Leone: a comprehensive, retrospective, countrywide survey from all health care facilities performing operations in 2012. Surgery (United States) 157(6):992–1001. https://doi.org/10.1016/j.surg.2014.12.028
Bolkan HA, van Duinen A, Waalewijn B et al (2017) Safety, productivity and predicted contribution of a surgical task-sharing programme in Sierra Leone. Br J Surg 104(10):1315–1326. https://doi.org/10.1002/bjs.10552
Cancedda C, Davis SM, DIerberg KL et al (2016) Strengthening Health Systems while Responding to a Health Crisis: Lessons Learned by a Nongovernmental Organization during the Ebola Virus Disease Epidemic in Sierra Leone. J Infectious Dis 214:S153–S163. https://doi.org/10.1093/infdis/jiw345
Haja R (2014) Wurie and Sophie Witter. In depth interviews of health workers in Sierra Leone report. Published online 2014. Accessed March 31, 2022. https://assets.publishing.service.gov.uk/media/57a089cded915d3cfd00042c/IDIreport-SL-final-230614.pdf
Government of Sierra Leone. Free healthcare services for pregnant and lactating women and young children in Sierra Leone. Published online 2009. Accessed March 31, 2022. https://unipsil.unmissions.org/sites/default/files/old_dnn/free_services_framewk_nov09.pdf
Shiqing Li (2022) Hope on Wheels: A first-of-its-kind National Emergency Medical Service (NEMS) in Sierra Leone. Accessed March 31, 2022. https://blogs.worldbank.org/health/hope-wheels-first-its-kind-national-emergency-medical-service-nems-sierra-leone
Togoh GPY, Turay AB, Komba A (2017) Sierra Leone 2015 Population and Housing Census Thematic Report on Population Projections.
United Nations (2022) Human Development Reports. Published 2022. Accessed March 31, 2022. http://hdr.undp.org/en/countries/profiles/SLE
Groen RS, Samai M, Petroze RT et al (2012) Pilot testing of a population-based Surgical Survey Tool in Sierra Leone. World J Surg 36(4):771–774. https://doi.org/10.1007/s00268-012-1448-9
Geraedts TJM, Boateng D, Lindenbergh KC et al (2021) Evaluating the cascade of care for hypertension in Sierra Leone. Tropical Med Int Health. Published online 2021. https://doi.org/10.1111/tmi.13664
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG (2009) Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J Biomed Inform 42(2):377–381. https://doi.org/10.1016/J.JBI.2008.08.010
Harris PA, Taylor R, Minor BL et al (2019) The REDCap consortium: Building an international community of software platform partners. J Biomed Informatics 95. https://doi.org/10.1016/j.jbi.2019.103208
Petroze RT, Groen RS, Niyonkuru F et al (2013) Estimating operative disease prevalence in a low-income country: Results of a nationwide population survey in Rwanda. Surgery (United States) 153(4):457–464. https://doi.org/10.1016/j.surg.2012.10.001
Varela C, Young S, Groen R, Banza L, Mkandawire NC, Viste A (2017) Untreated surgical conditions in Malawi: a randomised cross-sectional nationwide household survey. Malawi Med J 29(3):231–236. https://doi.org/10.4314/mmj.v29i3.1
Tran TM, Fuller AT, Butler EK et al (2017) Burden of surgical conditions in Uganda: aCross-sectional Nationwide Household Survey. Ann Surg 266(2):389–399. https://doi.org/10.1097/SLA.0000000000001970
Gupta S, Shrestha S, Ranjit A et al (2015) Conditions, preventable deaths, procedures and validation of a countrywide survey of surgical care in Nepal. Br J Surg 102(6):700–707. https://doi.org/10.1002/bjs.9807
Linden AF, Maine RG, Hedt-Gauthier BL et al (2016) Validation of a community-based survey assessing nonobstetric surgical conditions in Burera District. Rwanda Surgery (United States) 159(4):1217–1226. https://doi.org/10.1016/j.surg.2015.10.012
World Health Organization. Framework and Standards for Country Health Information Systems/Health Metrics Network. 2nd edition. Published 2012. Accessed March 31, 2022. https://www.who.int/healthinfo/country_monitoring_evaluation/who-hmn-framework-standards-chi.pdf
Meara JG, Leather AJM, Hagander L et al (2015) Global Surgery 2030: evidence and solutions for achieving health, welfare, and economic development. Lancet 386(9993):569–624. https://doi.org/10.1016/S0140-6736(15)60160-X
World Health Organization. Strengthening emergency and essential surgical care and anaesthesia as a component of universal health coverage. Report by the Secretariat. Published online 2015. Accessed March 31, 2022. https://apps.who.int/gb/ebwha/pdf_files/WHA68/A68_31-en.pdf
The World Bank. Individuals using the Interne - Sierra Leone | Data. Accessed March 31, 2022. https://data.worldbank.org/indicator/IT.NET.USER.ZS?locations=SL
Maine RG, Linden AF, Riviello R et al (2017) Prevalence of untreated surgical conditions in Rural Rwanda: A population-based cross-sectional study in burera district. JAMA Surg 152(12). https://doi.org/10.1001/jamasurg.2017.4013
Mukangendo M, Nzayirambaho M, Hitimana R, Yamuragiye A (2018) Factors Contributing to Low Adherence to Community-Based Health Insurance in Rural Nyanza District, Southern Rwanda. J Environ Public Health. https://doi.org/10.1155/2018/2624591
World Health Organization. Global Health Expenditure Database. Accessed March 31, 2022. https://apps.who.int/nha/database/country_profile/Index/en
The World Bank. Sierra Leone | Financial Data. Accessed March 31, 2022. https://data.worldbank.org/country/sierra-leone?view=chart
Government of Sierra Leone. The Republic of Sierra Leone | State House | Press Release. Accessed March 31, 2022. https://statehouse.gov.sl/press-release/1502-government-of-sierra-leone-press-release
van Duinen AJ, Westendorp J, Ashley T et al (2021) Catastrophic expenditure and impoverishment after caesarean section in Sierra Leone: An evaluation of the free health care initiative. PLoS ONE 16(10 October). https://doi.org/10.1371/JOURNAL.PONE.0258532
Jalloh MB, Bah AJ, James PB, Sevalie S, Hann K, Shmueli A (2019) Impact of the free healthcare initiative on wealth-related inequity in the utilization of maternal & child health services in Sierra Leone. BMC Health Services Res 19(1). https://doi.org/10.1186/s12913-019-4181-3
Makaka A, Breen S, Binagwaho A (2012) Universal health coverage in Rwanda: a report of innovations to increase enrolment in community-based health insurance. Lancet 380:S7. https://doi.org/10.1016/s0140-6736(13)60293-7
Lindheim-Minde B, Gjøra A, Bakker JM et al (2021) Changes in surgical volume, workforce, and productivity in Sierra Leone between 2012 and 2017. Surgery 170(1):126–133. https://doi.org/10.1016/j.surg.2021.02.043
United Nations. Sustainable Development Goals (SDGs) and Disability | United Nations. Accessed March 31, 2022. https://www.un.org/development/desa/disabilities/about-us/sustainable-development-goals-sdgs-and-disability.html
Juran S, Gruendl M, Marks IH et al (2019) The need to collect, aggregate, and analyze global anesthesia and surgery data. Can J Anesth 66(2):218–229. https://doi.org/10.1007/s12630-018-1261-5
Government of Zambia. Statistics Agency Zambia. Zambia Demographic and Health Survey 2018. Published online 2020. Accessed March 31, 2022. https://www.dhsprogram.com/pubs/pdf/FR361/FR361.pdf
Powell BL, Luckett R, Bekele A, Chao TE (2020) Sex disparities in the global burden of surgical disease. World J Surg 44(7):2139–2143. https://doi.org/10.1007/s00268-020-05484-4
Nigel A, Mathers N, Fox N (2022) Surveys and Questionnaires. The NIHR RDS for the East Midlands/Yorkshire & the Humber. Published online 2007. Accessed March 31, 2022. https://www.rds-yh.nihr.ac.uk/wp-content/uploads/2013/05/12_Surveys_and_Questionnaires_Revision_2009.pdf
Acknowledgements
Without the help of all Sierra Leonean drivers, enumerators, and field supervisors deployed by Stats SL, this study would not have been possible. The authors especially thank the Field Coordinator of Masanga Hospital for all logistical arrangements, K.B.B. Kamara; additional thanks to the data collectors of the Surgical Training Program, S. Kanneh, J. Kamoh, A. Tommy, M. Mansaray †, and M.S. Kpaka; and the supervisors of the international medical students, F.W. Bloemers, M.J. Rijken, J.L. Browne, and R. Lonnee-Hoffman. PRESSCO 2020 study group: Amsterdam UMC, Department of Surgery, Amsterdam, The Netherlands (Jurre van Kesteren, Jonathan Vas Nunes); CapaCare, Trondheim, Norway (Håkon A. Bolkan, Alex J. van Duinen); CapaCare Netherlands, Wageningen, The Netherlands (Daniel van Leerdam, Josien Westendorp); Centre of Tropical Medicine and Travel Medicine, Amsterdam University Medical Centres, University of Amsterdam, The Netherlands (Martin P. Grobusch, Hanna M. Mathéron, Giulia L.E. Mönnink, Jonathan Vas Nunes); Clinic of Surgery, St. Olavs Hospital HF, Trondheim University Hospital, Trondheim, Norway (Håkon A. Bolkan, Alex J. van Duinen); Global Surgery Amsterdam, Amsterdam, The Netherlands (Jurre van Kesteren); Institute for Health & Equity and Epidemiology Division, Medical College of Wisconsin, Milwaukee, WI, USA (Laura D. Cassidy); Johns Hopkins School of Medicine, Baltimore, USA (Reinou S. Groen); Institute of Clinical and Molecular Medicine, Norwegian University of Science and Technology, Trondheim, Norway (Håkon A. Bolkan, Alex J. van Duinen, Sara Hoel, Sofie M. Løvdal, Mia N. Østensen, Helene Solberg, Josien Westendorp); Julius Global Health, Julius Centre for Health Sciences and Primary Care, University Medical Centre Utrecht, Utrecht University, The Netherlands (Daniel Boateng, Kerstin Klipstein-Grobusch); KIT, Royal Tropical Institute, Amsterdam, The Netherlands (Daniel van Leerdam); Masanga Medical Research Unit, Sierra Leone (Diede van Delft, Martin P. Grobusch, Hanna Mathéron, Jonathan Vas Nunes); Sierra Leone, Statistics Sierra Leone, Hill Tower, Freetown (Silleh Bah, Abubakarr Kamanda-Bongay, Sonnia-Magba Bu-Buakei Jabbi, James A. Medo, Osman Sankoh); SOSAS—Surgeons Over Seas, New York, USA (Reinou S. Groen); University Medical Centre Utrecht, Utrecht, The Netherlands (Daan van Herwaarden, Janine P.J. Martens); Vrije Universiteit, Faculty of Medicine, Amsterdam, The Netherlands (Karel C. Lindenbergh).
Funding
Norwegian University of Science and Technology (NTNU), CapaCare, Norway, and the University of Amsterdam’s Centre of Tropical Medicine and Travel Medicine funded this study. Statistics Sierra Leone, CapaCare Sierra Leone, and Masanga Medical Research Unit, Sierra Leone, made in-kind contributions. The funders had no role in the outcome of the data collection, analysis, or writing of the manuscript, nor the decision to submit the manuscript for publication. None of the authors had any potential conflict of interest to report.
Author information
Authors and Affiliations
Consortia
Contributions
JVK, HJB, RSG, OS, MPG, and HAB conceived and designed the study. JVK, FM, DvD, SMBBJ, SB, JAM, AKB, DvL, HMM, GLEM, JVN, KCL, SH, SML, MNO, HS, DVH, and JPJM performed the survey and data collection. JvK, AS, LDC, and AvD analyzed the data. JvK, AvD, MPG, and HAB drafted the article. All authors critically reviewed the manuscript. All members of the PRESSCO 2020 study group had access to the complete data. All authors contributed to, and endorsed, the final version submitted for publication.
Corresponding author
Ethics declarations
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
van Kesteren, J., van Duinen, A.J., Marah, F. et al. PREvalence Study on Surgical COnditions (PRESSCO) 2020: A Population-Based Cross-Sectional Countrywide Survey on Surgical Conditions in Post-Ebola Outbreak Sierra Leone. World J Surg 46, 2585–2594 (2022). https://doi.org/10.1007/s00268-022-06695-7
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-022-06695-7