Abstract
Introduction
Primary hyperparathyroidism (PHPT) is a relatively common condition in surgical practice. Availability of localisation studies has shifted the treatment from bilateral neck exploration to selective parathyroidectomy. Several imaging modalities, each with varying sensitivities, are available to detect abnormal parathyroid glands. Ultrasound is almost universally accepted as the first line radiological investigation however its sensitivity is particularly heterogeneous and operator-dependent.
Material and methods
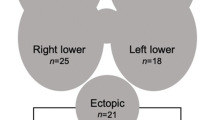
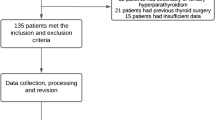
We studied 250 consecutive patients with PHPT who underwent parathyroidectomy in our hospital over a period of 33 months. Pre-operative neck ultrasound, 99mTc-sestamibi and single-photon emission computed tomography (SPECT CT) were performed in 249, 237 and 198 patients respectively. Unilateral and bilateral neck exploration was performed in 190 and 60 patients, respectively. Sensitivity, positive predictive value (PPV) and accuracy were calculated comparing the results with surgical and pathology findings.
Results
Mean pre and postoperative PTH and adjusted calcium were, 11 ± 10.6 pmol/L, 1.9 ± 3.6, 2.81 ± 0.2 and 2.45 ± 0.2 mmol/L. There were 71 (29.95%) discordant results between US, compared to sestamibi and SPECT CT. An average of 1.9 parathyroid glands were removed with a mean weight of 0.92 g. Overall success rate based on postoperative PTH levels was 94.8%. Overall sensitivity, PPV and accuracy for US were 80.80%, 92.35%, and 75.73% respectively; for sestamibi were 71.82%, 94.61%, 69.00% and for SPECT CT were; 70.21%, 97.78%, 69.11% respectively.
Conclusion
Ultrasound performed by an experienced specialist sonographer is highly sensitive in localising abnormal parathyroid glands. It can be used as a main and sole investigation in the majority of patients. Sestamibi, SPECT CT and other investigations should be performed in a step-wise manner and reserved for patients with negative US, failed primary procedure and recurrences.

Similar content being viewed by others
References
Tezelman S, Shen W, Shaver JK, Siperstein AE, Duh QY, Klein H et al (1993) Double parathyroid adenomas. Clinical and biochemical characteristics before and after parathyroidectomy. Ann Surg 218(3):300–307
Attie JN, Bock G, Auguste LJ (1990) Multiple parathyroid adenomas: report of thirty-three cases. Surgery 108(6):1014–1019
Wynne AG, van Heerden J, Carney JA, Fitzpatrick LA (1992) Parathyroid carcinoma: clinical and pathologic features in 43 patients. Medicine (Baltimore) 71(4):197–205
Mohebati A, Shaha AR (2012) Imaging techniques in parathyroid surgery for primary hyperparathyroidism. Am J Otolaryngol 33(4):457
Castleman B, Schantz A, Roth S (1976) Parathyroid hyperplasia in primary hyperparathyroidism: a review of 85 cases. Cancer 38(4):1668–1675
Lavely WC, Goetze S, Friedman KP, Leal JP, Zhang Z, Garret-Mayer E et al (2007) Comparison of SPECT/CT, SPECT, and planar imaging with single- and dual-phase 99mTc-sestamibi parathyroid scintigraphy. J Nucl Med 48(7):1084–1089
Chien D, Jacene H (2010) Imaging of parathyroid glands. Otolaryngol Clin North Am 43(2):399–415
Gayed IW, Kim EE, Broussard WF, Evans D, Lee J, Broemeling LD et al (2005) The value of 99mTc-sestamibi SPECT/CT over conventional SPECT in the evaluation of parathyroid adenomas or hyperplasia. J Nucl Med 46(2):248–252
Zerizer I, Parsaï A, Win Z, Al-Nahhas A (2011) Anatomical and functional localization of ectopic parathyroid adenomas: 6-year institutional experience. Nucl Med Commun 32(6):496–502
Roy M, Mazeh H, Chen H, Sippel RS (2013) Incidence and localization of ectopic parathyroid adenomas in previously unexplored patients. World J Surg 37(1):102–106. https://doi.org/10.1007/s00268-012-1773-z
Carpentier A, Jeannotte S, Verreault J, Lefebvre B, Bisson G, Mongeau CJ et al (1998) Preoperative localization of parathyroid lesions in hyperparathyroidism: relationship between technetium-99m-MIBI uptake and oxyphil cell content. J Nucl Med 39(8):1441–1444
Barbaros U, Erbil Y, Salmashoğlu A, Işsever H, Aral F, Tunaci M et al (2009) The characteristics of concomitant thyroid nodules cause false-positive ultrasonography results in primary hyperparathyroidism. Am J Otolaryngol 30(4):239–243
Edafe O, Collins E, Ubhi C, Balasubramanian S (2018) Current predictive models do not accurately differentiate between single and multi gland disease in primary hyperparathyroidism: a retrospective cohort study of two endocrine surgery units. Ann R Coll Surg Engl 100(2):140–145
Wei WJ, Shen CT, Song HJ, Qiu ZL, Luo QY (2015) Comparison of SPET/CT, SPET and planar imaging using 99mTc-MIBI as independent techniques to support minimally invasive parathyroidectomy in primary hyperparathyroidism: a meta-analysis. Hell J Nucl Med 18(2):127–135
Lee GS, McKenzie TJ, Mullan BP, Farley DR, Thompson GB, Richards ML (2016) A multimodal imaging protocol, (123)I/(99)Tc-Sestamibi, SPECT, and SPECT/CT, in primary hyperparathyroidism adds limited benefit for preoperative localization. World J Surg 40(3):589–594. https://doi.org/10.1007/s00268-015-3389-6
Moosvi SR, Smith S, Hathorn J, Groot-Wassink T (2017) Evaluation of the radiation dose exposure and associated cancer risks in patients having preoperative parathyroid localization. Ann R Coll Surg Engl 99(5):363–368
Varadharajan K, Choudhury N (2018) Current practice in the surgical management of parathyroid disorders: a United Kingdom survey. Eur Arch Oto-Rhino-Laryngology 275(10):2549–2553
Morris LF, Zanocco K, Ituarte PHG, Ro K, Duh Q-Y, Sturgeon C et al (2010) The value of intraoperative parathyroid hormone monitoring in localized primary hyperparathyroidism: a cost analysis. Ann Surg Oncol 17(3):679–685
Miura D, Wada N, Arici C, Morita E, Duh Q-Y, Clark OH (2002) Does intraoperative quick parathyroid hormone assay improve the results of parathyroidectomy? World J Surg 26(8):926–930. https://doi.org/10.1007/s00268-002-6620-1
Mownah OA, Pafitanis G, Drake WM, Crinnion JN (2015) Contemporary surgical treatment of primary hyperparathyroidism without intraoperative parathyroid hormone measurement. Ann R Coll Surg Engl 97(8):603–607
Berri RN, Lloyd LR (2006) Detection of parathyroid adenoma in patients with primary hyperparathyroidism: the use of office-based ultrasound in preoperative localization. Am J Surg 191(3):311–314
Bhansali A, Masoodi SR, Bhadada S, Mittal BR, Behra A, Singh P (2006) Ultrasonography in detection of single and multiple abnormal parathyroid glands in primary hyperparathyroidism: comparison with radionuclide scintigraphy and surgery. Clin Endocrinol (Oxf) 65(3):340–345
Tresoldi S, Pompili G, Maiolino R, Flor N, De Pasquale L, Bastagli A et al (2009) Primary hyperparathyroidism: can ultrasonography be the only preoperative diagnostic procedure? Radiol Med 114(7):1159–1172
Solorzano CC, Carneiro-Pla DM, Irvin GL (2006) Surgeon-performed ultrasonography as the initial and only localizing study in sporadic primary hyperparathyroidism. J Am Coll Surg 202(1):18–24
Haber RS, Kim CK, Inabnet WB (2002) Ultrasonography for preoperative localization of enlarged parathyroid glands in primary hyperparathyroidism: comparison with (99m)technetium sestamibi scintigraphy. Clin Endocrinol (Oxf) 57(2):241–249
Cheung K, Wang TS, Farrokhyar F, Roman SA, Sosa JA (2012) A meta-analysis of preoperative localization techniques for patients with primary hyperparathyroidism. Ann Surg Oncol 19(2):577–583
Acknowledgement
We thank our radiologists, sonographers and our patients. Without their help and support, it was impossible to complete our work.
Funding
No grants were obtained for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Korwar, V., Yuen Chang, F., Teasdale, E. et al. Stepwise Approach for Parathyroid Localisation in Primary Hyperparathyroidism. World J Surg 44, 803–809 (2020). https://doi.org/10.1007/s00268-019-05269-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-019-05269-4