Abstract
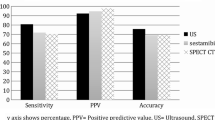
Minimal access surgery for single or multi-glandular primary hyperparathyroidism requires precise preoperative localization. A multitude of imaging and nuclear medicine techniques are available to accomplish this. In this study, we compared techniques such as neck ultrasound, parathyroid scintigraphy, single-photon emission computed tomography and computed tomography (SPECT/CT), magnetic resonance imaging (MRI), and other methods in terms of sensitivity, specificity, and accuracy in localizing parathyroid disease. A single-center retrospective cohort study was carried out on selected adult patients with primary hyperparathyroidism who had undergone parathyroidectomy. Details of preoperative imaging were charted, coded, and analyzed to determine sensitivity, specificity, accuracy, and other parameters of various techniques for preoperative localization. Parathyroid scintigraphy scanning was the most sensitive and accurate procedure for functional imaging, followed closely by SPECT/CT. The specificity and positive predictive value were higher for SPECT/CT, and both modalities outperformed neck ultrasonography. For anatomical imaging, MRI and CT neck with IV contrast had high sensitivity, while neck U/S, SPECT/CT, and scintigraphy had higher specificity, but there were no significant differences between various modalities. Study concludes that SPECT/CT had excellent accuracy in detecting and localizing single-gland disease; an additional imaging technique such as CT neck with contrast or MRI was more useful in patients with multi-glandular disease.


Similar content being viewed by others
References
Ruda JM, Hollenbeak C, Stack BC Jr (2005) A systematic review of the diagnosis and treatment of primary hyperparathyroidism from 1995 to 2003. Otolaryngol Head Neck Surg 132:359–372
Lavely WC, Goetze S, Friedman KP, Leal JP, Zhang Z, Garret-Mayer E et al (2007) Comparison of SPECT/CT, SPECT, and planar imaging with single- and dual-phase (99m)Tc-sestamibi parathyroid scintigraphy. J Nucl Med 48(7):1084–1089
Wimmer G, Profanter C, Kovacs P, Sieb M, Gabriel M, Putzer D et al (2010) CT-MIBI-SPECT image fusion predicts multiglandular disease in hyperparathyroidism. Langenbecks Arch Surg 395(1):73–80
Barber B, Moher C, Côté D, Fung E, O’Connell D, Dziegielewski P et al (2016) Comparison of single photon emission CT (SPECT) with SPECT/CT imaging in preoperative localization of parathyroid adenomas: a cost-effectiveness analysis. Head Neck 38(Suppl 1):E2062–E2065
Sharma J, Mazzaglia P, Milas M, Berber E, Schuster DM, Halkar R et al (2006) Radionuclide imaging for hyperparathyroidism (HPT): which is the best technetium-99m sestamibi modality? Surgery 140(6):856 63-discussion 863-5
McCoy KL, Ghodadra AG, Hiremath TG, Albarano A, Joyce JM, Yip L et al (2018) Sestamibi SPECT/CT versus SPECT only for preoperative localization in primary hyperparathyroidism: a single institution 8-year analysis. Surgery 163(3):643–647
Neumann DR, Obuchowski NA, Difilippo FP (2008) Preoperative 123I/99mTc-sestamibi subtraction SPECT and SPECT/CT in primary hyperparathyroidism. J Nucl Med 49(12):2012–2017
Oksüz MO, Dittmann H, Wicke C, Müssig K, Bares R, Pfannenberg C et al (2011) Accuracy of parathyroid imaging: a comparison of planar scintigraphy, SPECT, SPECT-CT, and C-11 methionine PET for the detection of parathyroid adenomas and glandular hyperplasia. Diagn Interv Radiol 17(4):297–307
von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP (2007) The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. PLoS Med 4(10):e296
Hindié E, Ugur O, Fuster D, O’Doherty M, Grassetto G, Ureña P et al (2009) 2009 EANM parathyroid guidelines. Eur J Nucl Med Mol Imaging 36(7):1201–1216
AIUM (2013) practice guideline for the performance of a thyroid and parathyroid ultrasound examination. J Ultrasound Med 32(7):1319–29
Arifin WN (2021) Sample size calculator. Available from: http://wnarifin.github.io. Accessed 31 Oct 2021
Buderer NM (1996) Statistical methodology: I Incorporating the prevalence of disease into the sample size calculation for sensitivity and specificity. Acad Emerg Med 3(9):895–900
Kunstman JW, Udelsman R (2012) Superiority of minimally invasive parathyroidectomy. Adv Surg 46(1):171–189
Wilhelm SM, Wang TS, Ruan DT, Lee JA, Asa SL, Duh QY, Doherty GM, Herrera MF, Pasieka JL, Perrier ND, Silverberg SJ (2016) The American Association of Endocrine Surgeons guidelines for definitive management of primary hyperparathyroidism. JAMA Surg 151(10):959–968
Minisola S, Cipriani C, Diacinti D, Tartaglia F, Scillitani A, Pepe J, Scott-Coombes D (2016) Imaging of the parathyroid glands in primary hyperparathyroidism. Eur J Endocrinol 174(1):D1-8
Giovanella L, Bacigalupo L, Treglia G, Piccardo A (2021) Will 18 F-fluorocholine PET/CT replace other methods of preoperative parathyroid imaging? Endocrine 71(2):285–297
Cheung K, Wang TS, Farrokhyar F, Roman SA, Sosa JA (2012) A meta-analysis of preoperative localization techniques for patients with primary hyperparathyroidism. Ann Surg Oncol 19(2):577–583
Parikh AM, Grogan RH, Moron FE (2020) Localization of parathyroid disease in reoperative patients with primary hyperparathyroidism. I J Endocrinol 25:2020
Scattergood S, Marsden M, Kyrimi E, Ishii H, Doddi S, Sinha P (2019) Combined ultrasound and Sestamibi scintigraphy provides accurate preoperative localisation for patients with primary hyperparathyroidism. Ann R Coll Surg Engl 101(2):97–102
Aydin H, Dural AC, Sahbaz NA, Karli M, Guzey D, Akarsu C, Ferahman S, Piskinpasa H, Yegul D, Sipahi M, Koyuncu A (2021) Clinical adaptation of auxiliary methods and multidisciplinary approach to changing trends in parathyroid surgery. Medicine 1;100(39)
McCoy KL, Ghodadra AG, Hiremath TG, Albarano A, Joyce JM, Yip L, Carty SE, Muthukrishnan A (2018) Sestamibi SPECT/CT versus SPECT only for preoperative localization in primary hyperparathyroidism: a single institution 8-year analysis. Surgery 163(3):643–647
Kedarisetty S, Fundakowski C, Ramakrishnan K, Dadparvar S (2019) Clinical value of Tc99m-MIBI SPECT/CT versus 4D-CT or US in management of patients with hyperparathyroidism. Ear Nose Throat J 98(3):149–157
Cuderman A, Senica K, Rep S, Hocevar M, Kocjan T, Sever MJ, Zaletel K, Lezaic L (2020) 18F-Fluorocholine PET/CT in primary hyperparathyroidism: superior diagnostic performance to conventional scintigraphic imaging for localization of hyperfunctioning parathyroid glands. J Nucl Med 61(4):577–583
Khafif A, Masalha M, Landsberg R, Domachevsky L, Bernstine H, Groshar D, Azoulay O, Lockman Y (2019) The role of F18-fluorocholine positron emission tomography/magnetic resonance imaging in localizing parathyroid adenomas. Eur Arch Otorhinolaryngol 276(5):1509–1516
Lee SW, Shim SR, Jeong SY, Kim SJ (2021) Direct comparison of preoperative imaging modalities for localization of primary hyperparathyroidism: a systematic review and network meta-analysis. JAMA Otolaryngology–Head & Neck Surgery 3.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Alessa, M., Algouhi, A., Alsowailmi, G. et al. Preoperative Localization for Primary Hyperparathyroidism Surgery: Comparison of Imaging Techniques at a Tertiary Center. Indian J Surg (2022). https://doi.org/10.1007/s12262-022-03561-7
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12262-022-03561-7