Abstract
Background
Residual disease (RD) has been described as one of the most relevant prognostic factors after radical surgical resection for incidental gallbladder cancer (IGC). The purpose of the present study was to analyze patterns of RD and determinant prognostic factors in patients undergoing re-resection for IGC.
Methods
Patients undergoing re-exploration due to IGC between 1990 and 2014 were identified in two referral centers from different South-American countries. Patients submitted to a radical definitive operation were included in the study. Demographics and tumor-treated related variables were analyzed in correlation with RD and survival. The site of RD, local (gallbladder bed) or regional (lymph nodes and bile duct) was correlated with disease-specific survival (DSS).
Results
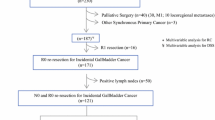
Of 265 patients with IGC submitted to surgery, 168 underwent a radical re-resection and RD was found in 58 (34.5%). Demographic, clinical and surgical variables were compared between both centers showing differences in type of resection, laparoscopic approach, T stages and disease stage. Location of RD was regional in 34 (20.2%) and local in 24 (14.3%), and no residual disease was found in 110 (65.5%) patients. T stage (T1b = 20%, T2 = 23.8%, T3 = 71.7%, p < 0.001) and disease stage (p < 0.001) were independent predictors of RD. Finding RD at any location reduced the DSS in comparison with non-RD patients (19.6 months vs. 62.7 months p < 0.001). No differences in DSS according to the location of RD were found, and all anatomic sites were equally poor (p = 0.27). RD at any site predicted DSS (p < 0.001), independently of all other IGC variables.
Conclusions
IGC presented similar clinical parameters in two different countries of South America. RD was demonstrated as the most critical prognostic variable in patients with IGC treated by a radical resection. The presence of RD was associated with poor outcome, independently of any anatomic location. Future studies incorporating neoadjuvant chemotherapy in the treatment of patients with prognostic factors for RD are required to improve survival in this entity.


Similar content being viewed by others
References
Lendoire JC, Gil L, Duek F et al (2012) Relevance of residual disease after liver resection for incidental gallbladder cancer. HPB (Oxford) 14(8):548–553
Butte JM, Waugh E, Meneses M et al (2010) Incidental gallbladder cancer: analysis of surgical findings and survival. J Surg Oncol 102(6):620–625
Maker AV, Butte JM, Oxenberg J et al (2012) Is port site resection necessary in the surgical management of gallbladder cancer? Ann Surg Oncol 19(2):409–417
Goetze TO, Paolucci V (2010) Adequate extent in radical re-resection of incidental gallbladder carcinoma: analysis of the German Registry. Surg Endosc 24(9):2156–2164
Smith GCS, Parks RW, Madhavan KK et al (2003) A 10-year experience in the management of gallbladder cancer. HPB (Oxford) 5(3):159–166
Fuks D, Regimbeau JM, Le Treut Y-P et al (2011) Incidental gallbladder cancer by the AFC-GBC-2009 study group. World J Surg 35(8):1887–1897. https://doi.org/10.1007/s00268-011-1134-3
Ito H, Ito K, D’Angelica M et al (2011) Accurate staging for gallbladder cancer: implications for surgical therapy and pathological assessment. Ann Surg 254(2):320–325
Pawlik TM, Gleisner AL, Vigano L et al (2007) Incidence of finding residual disease for incidental gallbladder carcinoma: implications for re-resection. J Gastrointest Surg 11(11):1478–1487
Gil L, Lendoire J, Duek F et al (2014) Cirugía radical en el cáncer de vesícula incidental: valor del hallazgo de enfermedad residual en el estudio histopatológico diferido. Cir Esp 92(3):168–174
Butte JM, Kingham TP, Gönen M et al (2014) Residual disease predicts outcomes after definitive resection for incidental gallbladder cancer. J Am Coll Surg 219(3):416–429
Ethun CG, Postlewait LM, Le N et al (2017) Association of optimal time interval to re-resection for incidental gallbladder cancer with overall survival. JAMA Surg 152(2):143
Edge SB, Byrd DR, Compton CC et al (eds) (2010) AJCC cancer staging manual, 7th edn. Springer, New York
Arroyo GF, Gentile A, Parada LA (2016) Gallbladder cancer: South American experience. Chin Clin Oncol 5(5):67
Pitt SC, Jin LX, Hall BL et al (2014) Incidental gallbladder cancer at cholecystectomy. Ann Surg 260(1):128–133
Yip VS, Gomez D, Brown S et al (2014) Management of incidental and suspicious gallbladder cancer: focus on early referral to a tertiary centre. HPB 16(7):641–647
Tsirlis T, Ausania F, White SA et al (2015) Implications of the index cholecystectomy and timing of referral for radical resection of advanced incidental gallbladder cancer. Ann R Coll Surg Engl 97(2):131–136
Sternby Eilard M, Lundgren L, Cahlin C et al (2017) Surgical treatment for gallbladder cancer—a systematic literature review. Scand J Gastroenterol 52(5):505–514
Aloia TA, Járufe N, Javle M et al (2015) Gallbladder cancer: expert consensus statement. HPB 17(8):681–690
Ethun CG, Postlewait LM, Le N et al (2017) A novel pathology-based preoperative risk score to predict locoregional residual and distant disease and survival for incidental gallbladder cancer: a 10-institution study from the U.S. extrahepatic biliary malignancy consortium. Ann Surg Oncol 24(5):1343–1350
Shindoh J, de Aretxabala X, Aloia TA et al (2015) Tumor location is a strong predictor of tumor progression and survival in T2 gallbladder cancer. Ann Surg 261(4):733–739
Adsay NV, Bagci P, Tajiri T et al (2012) Pathologic staging of pancreatic, ampullary, biliary, and gallbladder cancers: pitfalls and practical limitations of the current AJCC/UICC TNM staging system and opportunities for improvement. Semin Diagn Pathol 29(3):127–141
Roa I, Ibacache G, Muñoz S et al (2014) Gallbladder cancer in Chile: pathologic characteristics of survival and prognostic factors: analysis of 1366 cases. Am J Clin Pathol 141(5):675–682
Butte JM, Gönen M, Allen PJ et al (2011) The role of laparoscopic staging in patients with incidental gallbladder cancer. HPB (Oxford) 13(7):463–472
Creasy JM, Goldman DA, Gonen M et al (2017) Predicting residual disease in incidental gallbladder cancer: risk stratification for modified treatment strategies. J Gastrointest Surg 21(8):1254–1261
Birnbaum DJ, Viganò L, Russolillo N et al (2015) Lymph node metastases in patients undergoing surgery for a gallbladder cancer. Extension of the lymph node dissection and prognostic value of the lymph node ratio. Ann Surg Oncol 22(3):811–818
Shibata K, Uchida H, Iwaki K et al (2009) Lymphatic invasion: an important prognostic factor for stages T1b–T3 gallbladder cancer and an indication for additional radical resection of incidental gallbladder cancer. World J Surg 33(5):1035–1041. https://doi.org/10.1007/s00268-009-9950-4
Sirohi B, Mitra A, Jagannath P et al (2015) Neoadjuvant chemotherapy in patients with locally advanced gallbladder cancer. Future Oncol 11(10):1501–1509
Engineer R, Goel M, Chopra S et al (2016) Neoadjuvant chemoradiation followed by surgery for locally advanced gallbladder cancers: a new paradigm. Ann Surg Oncol 23:3009–3015
Matsuda T, Matsuda A, Birnbaum DJ et al (2015) Clinical characteristics of incidental or unsuspected gallbladder cancers diagnosed during or after cholecystectomy: a systematic review and meta-analysis. Ann Surg Oncol 22(3):299–305
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gil, L., de Aretxabala, X., Lendoire, J. et al. Incidental Gallbladder Cancer: How Residual Disease Affects Outcome in Two Referral HPB Centers from South America. World J Surg 43, 214–220 (2019). https://doi.org/10.1007/s00268-018-4762-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-018-4762-z