Background
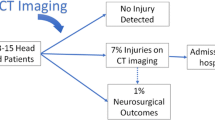
In patients with severe traumatic brain injury (TBI), early CT perfusion (CTP) provides additional information beyond the non-contrast CT (NCCT) and may alter clinical management. We hypothesized that this information may prognosticate functional outcome.
Methods
Five-year prospective observational study was performed in a level-1 trauma centre on consecutive severe TBI patients. CTP (obtained in conjunction with first routine NCCT) was interpreted as: abnormal, area of altered perfusion more extensive than on NCCT, and the presence of ischaemia. Six months Glasgow Outcome Scale-Extended of four or less was considered an unfavourable outcome. Logistic regression analysis of CTP findings and core variables [preintubation Glasgow Coma Scale (GCS), Rotterdam score, base deficit, age] was conducted using Bayesian model averaging to identify the best predicting model for unfavourable outcome.
Results
Fifty patients were investigated with CTP (one excluded for the absence of TBI) [male: 80%, median age: 35 (23–55), prehospital intubation: 7 (14.2%); median GCS: 5 (3–7); median injury severity score: 29 (20–36); median head and neck abbreviated injury scale: 4 (4–5); median days in ICU: 10 (5–15)]. Thirty (50.8%) patients had an unfavourable outcome. GCS was a moderate predictor of unfavourable outcome (AUC = 0.74), while CTP variables showed greater predictive ability (AUC for abnormal CTP = 0.92; AUC for area of altered perfusion more extensive than NCCT = 0.83; AUC for the presence of ischaemia = 0.81).
Conclusion
Following severe TBI, CTP performed at the time of the first follow-up NCCT, is a non-invasive and extremely valuable tool for early outcome prediction. The potential impact on management and its cost effectiveness deserves to be evaluated in large-scale studies.
Level of evidence III
Prospective study.



Similar content being viewed by others
References
Evans JA, van Wessem KJ, McDougall D et al (2010) Epidemiology of traumatic deaths: comprehensive population-based assessment. World J Surg 34:158–163. doi:10.1007/s00268-009-0266-1
Brain Trauma Foundation, American Association of Neurological Surgeons, Congress of Neurological Surgeons (2007) Guidelines for the management of severe traumatic brain injury. J Neurotrauma 24:S1–S106
Kubal WS (2012) Updated imaging of traumatic brain injury. Radiol Clin North Am 50:15–41
Huang AP, Tsai JC, Kuo LT et al (2014) Clinical application of perfusion computed tomography in neurosurgery. J Neurosurg 120:473–488
Bivard A, Levi C, Krishnamurthy V et al (2015) Perfusion computed tomography to assist decision making for stroke thrombolysis. Brain 138:1919–1931
Bendinelli C, Bivard A, Nebauer S et al (2013) Brain CT perfusion provides additional useful information in severe traumatic brain injury. Injury 44:1208–1212
Soustiel JF, Mahamid E, Goldsher D et al (2008) Perfusion-CT for early assessment of traumatic cerebral contusions. Neuroradiology 50:189–196
Wintermark M, Chioléro R, van Melle G et al (2004) Relationship between brain perfusion computed tomography variables and cerebral perfusion pressure in severe head trauma patients. Crit Care Med 32:1579–1587
Wintermark M, van Melle G, Schnyder P (2004) Admission perfusion CT: prognostic value in patients with severe head trauma. Radiology 232:211–220
Maas AI, Hukkelhoven CW, Marshall LF et al (2005) Prediction of outcome in traumatic brain injury with computed tomographic characteristics: a comparison between the computed tomographic classification and combinations of computed tomographic predictors. Neurosurgery 57:1173–1183
Wilson JT, Pettigrew LE, Teasdale GM (1998) Structured interviews for the Glasgow Outcome Scale and the extended Glasgow Outcome Scale: guidelines for their use. J Neurotrauma 15:573–585
Myburgh JA, Cooper DJ, Finfer SR et al (2008) Epidemiology and 12-month outcomes from traumatic brain injury in Australia and New Zealand. J Trauma 64:854–862
MRC Crash Trial Collaborators (2008) Predicting outcome after traumatic brain injury: practical prognostic models based on large cohort of international patients. BMJ 336:425–429
Marini CP, Stoller C, Shah O et al (2014) The impact of early flow and brain oxygen crisis on the outcome of patients with severe traumatic brain injury. Am J Surg 208:1071–1077
Olivecrona Z, Bobinski L, Koskinen LO (2015) Association of ICP, CPP, CT findings and S-100B and NSE in severe traumatic head injury. Prognostic value of the biomarkers. Brain Inj 29:446–454
Majdan M, Lingsma HF, Nieboer D et al (2014) Performance of IMPACT, CRASH and Nijmegen models in predicting six month outcome of patients with severe or moderate TBI: an external validation study. Scand J Trauma Resusc Emerg Med 19(22):68
Yuh EL, Cooper SR, Ferguson AR et al (2012) Quantitative CT improves outcome prediction in acute traumatic brain injury. J Neurotrauma 29:735–746
Osler T, Cook A, Glance LG et al (2016) The differential mortality of Glasgow Coma Score in patients with and without head injury. Injury 47:1879–1885
Han J, King NK, Neilson SJ et al (2014) External validation of the CRASH and IMPACT prognostic models in severe traumatic brain injury. J Neurotrauma 31:1146–1152
van der Ploeg T, Nieboer D, Steyerberg EW (2016) Modern modelling techniques had limited external validity in predicting mortality from traumatic brain injury. J Clin Epidemiol 78:83–89
Saatman KE, Duhaime AC, Bullock R et al (2008) Classification of traumatic brain injury for targeted therapies. J Neurotrauma 25:719–738
Chieregato A, Fainardi E, Servadei F et al (2004) Centrifugal distribution of regional cerebral blood flow and its time course in traumatic intracerebral hematomas. J Neurotrauma 21:655–666
Furuya Y, Hlatky R, Valadka AB et al (2003) Comparison of cerebral blood flow in computed tomographic hypodense areas of the brain in head-injured patients. Neurosurgery 52:340–346
Fridley J, Robertson C, Gopinath S (2015) Quantitative lobar cerebral blood flow for outcome prediction after traumatic brain injury. J Neurotrauma 32:75–82
Kaloostian P, Robertson C, Gopinath SP et al (2012) Outcome prediction within twelve hours after severe traumatic brain injury by quantitative cerebral blood flow. J Neurotrauma 29:727–734
Garnett MR, Blamire AM, Corkill RG et al (2001) Abnormal cerebral blood volume in regions of contused and normal appearing brain following traumatic brain injury using perfusion magnetic resonance imaging. J Neurotrauma 18:585–593
Abdel-Dayem HM, Sadek SA, Kouris K et al (1987) Changes in cerebral perfusion after acute head injury: comparison of CT with Tc-99 m HM-PAO SPECT. Radiology 165:221–226
Hattori N, Huang SC, Wu HM et al (2003) PET investigation of post-traumatic cerebral blood volume and blood flow. Acta Neurochir Suppl 86:49–52
Signoretti S, Marmarou A, Aygok GA, Fatouros PP, Portella G, Bullock RM (2008) Assessment of mitochondrial impairment in traumatic brain injury using high-resolution proton magnetic resonance spectroscopy. J Neurosurg 108:42–52
Takahashi S, Tanizaki Y, Kimura H et al (2015) Comparison of cerebral blood flow data obtained by computed tomography (CT) perfusion with that obtained by xenon CT using 320-row CT. J Stroke Cerebrovasc Dis 24:635–641
Honda M, Ichibayashi R, Yokomuro H et al (2016) Early cerebral circulation disturbance in patients suffering from severe traumatic brain injury (TBI): a xenon CT and perfusion CT study. Neurol Med Chir (Tokyo) 56:501–509
Schroder MI, Muizelaar JP, Bullock MR et al (1995) Focal ischemia due to traumatic contusions documented by stable xenon-CT and ultrastructual studies. J Neurosurg 82:966–971
Wen L, Lou HY, Xu J et al (2015) The impact of cranioplasty on cerebral blood perfusion in patients treated with decompressive craniectomy for severe traumatic brain injury. Brain Inj 29:1654–1660
Metting Z, Rödiger LA, De Keyser J et al (2007) Structural and functional neuroimaging in mild-to-moderate head injury. Lancet Neurol 6:699–710
Metting Z, Spikman JM, Rödiger LA et al (2014) Cerebral perfusion and neuropsychological follow up in mild traumatic brain injury: acute versus chronic disturbances? Brain Cogn 86:24–31
Authors’ Contributions
CB contributed to the study design, writing, and literature search; SC contributed to the data collection and interpretation; TE contributed to the statistical analysis; AB contributed to the data interpretation; DP contributed to functional outcome data acquisition; MP contributed to the study design, writing, and critical revision; and ZB contributed to the study design, writing, and critical revision.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Rights and permissions
About this article
Cite this article
Bendinelli, C., Cooper, S., Evans, T. et al. Perfusion Abnormalities are Frequently Detected by Early CT Perfusion and Predict Unfavourable Outcome Following Severe Traumatic Brain Injury. World J Surg 41, 2512–2520 (2017). https://doi.org/10.1007/s00268-017-4030-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-017-4030-7