Abstract
Background
Atorvastatin is a 3-hydroxy-3-methylglutaryl coenzyme A (HMG CoA) reductase inhibitor widely used in treatment of hypercholesterolemia and prevention of coronary heart disease and has various pleiotropic effects. In this study, the efficacy of atorvastatin emulgel (2 %) in reducing postoperative pain at rest, pain during defecation and analgesic requirement after open hemorrhoidectomy was investigated.
Methods
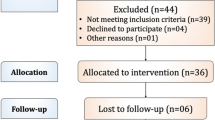
A total of 66 patients with third- and fourth-degree hemorrhoids undergoing open hemorrhoidectomy were included in this prospective, double-blind, randomized controlled trial. The patients were randomly assigned to either atorvastatin emulgel or placebo immediately after surgery and then every 12 h for 14 days. The primary outcomes were intensity of pain at rest and during defecation, measured with a visual analog scale, and the analgesic requirement, measured by amount of pethidine and acetaminophen consumption, and percent of wound healing.
Results
There was no significant difference in the average postoperative pain scores in the first 48 h (P 12h = 1, P 24h = 0.128 and P 48h = 0.079) after the surgery between the two groups, but at the week 1 the pain scores during defecation were considerably lower in the atorvastatin group than in placebo group (P = 0.004), which also was the same at the week 2 (P = 0.03). There was no significant difference in the average pethidine and acetaminophen (mg) administration at 12 h and 24 h between the two groups after surgery. Regarding the data about wound healing, at the week two the healing was much better in the treatment group than it was in control group and the difference was statistically significant (P = 0.04).
Conclusions
Compared with placebo, atorvastatin emulgel reduced postoperative pain at rest and on defecation and could improve the healing process after open hemorrhoidectomy.
Trial registration number
IRCT201404013014N8.

Similar content being viewed by others
References
Lohsiriwat V (2012) Hemorrhoids: from basic pathophysiology to clinical management. World J Gastroenterol 18(17):2009–2017
Lohsiriwat V (2015) Treatment of hemorrhoids: a coloproctologist’s view. WJG 21(31):9245
Lin H-C et al (2014) The tissue selecting technique (TST) versus the Milligan–Morgan hemorrhoidectomy for prolapsing hemorrhoids: a retrospective case–control study. Tech Coloproctol 18(8):739–744
Philip BK et al (2002) The economic impact of opioids on postoperative pain management. J Clin Anesth 14(5):354–364
Haas E et al (2012) A double-blind, randomized, active-controlled study for post-hemorrhoidectomy pain management with liposome bupivacaine, a novel local analgesic formulation. Am Surg 78(5):574–581
Rahimi M et al (2012) Comparison of topical anesthetic cream (EMLA) and diclofenac suppository for pain relief after hemorrhoidectomy: a randomized clinical trial. Surg Today 42(12):1201–1205
Sugimoto T et al (2013) A randomized, prospective, double-blind, placebo-controlled trial of the effect of diltiazem gel on pain after hemorrhoidectomy. World J Surg 37(10):2454–2457. doi:10.1007/s00268-013-2124-4
Perrotti P et al (2010) Topical nifedipine with lidocaine ointment versus active control for pain after hemorrhoidectomy: results of a multicentre, prospective, randomized, double-blind study. Can J Surg 53(1):17
Franceschilli L et al (2013) Role of 0.4% glyceryl trinitrate ointment after haemorrhoidectomy: results of a prospective randomised study. Int J Colorectal Dis 28(3):365–369
Patti R et al (2007) Botulinum toxin vs. topical glyceryl trinitrate ointment for pain control in patients undergoing hemorrhoidectomy: a randomized trial. Dis Colon Rectum 50(1):122
Ala S et al (2013) Efficacy of 10% sucralfate ointment in the reduction of acute postoperative pain after open hemorrhoidectomy: a prospective, double-blind, randomized, placebo-controlled trial. World J Surg 37(1):233–238. doi:10.1007/s00268-012-1805-8
Gupta P et al (2008) Topical sucralfate decreases pain after hemorrhoidectomy and improves healing: a randomized, blinded, controlled study. Dis Colon Rectum 51(2):231–234
Ala S et al (2013) Efficacy of cholestyramine ointment in reduction of postoperative pain and pain during defecation after open hemorrhoidectomy: results of a prospective, single-center, randomized, double-blind, placebo-controlled trial. World J Surg 37(3):657–662. doi:10.1007/s00268-012-1895-3
Ala S et al (2008) Topical metronidazole can reduce pain after surgery and pain on defecation in postoperative hemorrhoidectomy. Dis Colon Rectum 51(2):235–238
Eshghi F et al (2010) Effects of Aloe vera cream on posthemorrhoidectomy pain and wound healing: results of a randomized, blind, placebo-control study. J Alter Complement Med 16(6):647–650
Yoon S-G et al (2003) Effect of 0.2 percent glyceryl trinitrate ointment on wound healing after a hemorrhoidectomy. Dis Colon Rectum 46(7):950–954
Farsaei S et al (2012) Potential role of statins on wound healing: review of the literature. Int wound J 9(3):238–247
Edsman K et al (1998) Rheological evaluation of poloxamer as an in situ gel for ophthalmic use. Eur J Pharm Sci 6(2):105–112
Tristano AG, Fuller K (2006) Immunomodulatory effects of statins and autoimmune rheumatic diseases: novel intracellular mechanism involved. Int Immunopharmacol 6(12):1833–1846
Khattri S, Zandman-Goddard G (2013) Statins and autoimmunity. Immunol Res 56(2–3):348–357
Soehnlein O et al (2004) Atorvastatin induces tissue transglutaminase in human endothelial cells. Biochem Biophys Res Commun 322(1):105–109
Lopez S et al (2000) Effect of atorvastatin and fluvastatin on the expression of plasminogen activator inhibitor type-1 in cultured human endothelial cells. Atherosclerosis 152(2):359–366
Chang C-Z et al (2010) Atorvastatin preconditioning attenuates the production of endothelin-1 and prevents experimental vasospasm in rats. Acta Neurochir (Wien) 152(8):1399–1406
Pathak NN et al (2013) Antihyperalgesic and anti-inflammatory effects of atorvastatin in chronic constriction injury-induced neuropathic pain in rats. Inflammation 36(6):1468–1478
Ghaisas MM et al (2010) Antioxidant, antinociceptive and anti-inflammatory activities of atorvastatin and rosuvastatin in various experimental models. Inflammopharmacology 18(4):169–177
Mahmoodzadeh SV et al (2012) Solubility of atorvastatin calcium in water-ethanol mixture: solution-mediated phase transformation. Res Pharm Sci 7(5):S564
Murata Y et al (2000) Use of floating alginate gel beads for stomach-specific drug delivery. Eur J Pharm Biopharm 50(2):221–226
Aly UF (2012) Preparation and evaluation of novel topical gel preparations for wound healing in diabetics. Int J Pharm Pharm Sci 4(4):76
Wolverton SE (2012) Comprehensive dermatologic drug therapy. Elsevier Health Sciences, New York
Gupta PJ et al (2011) Topical sucralfate treatment of anal fistulotomy wounds: a randomized placebo-controlled trial. Dis Colon Rectum 54(6):699–704
Milligan E et al (1937) Surgical anatomy of the anal canal, and the operative treatment of haemorrhoids. Lancet 230(5959):1119–1124
Kirchhoff P et al (2010) Complications in colorectal surgery: risk factors and preventive strategies. Patient Saf Surg 4(1):1
Oderda G (2012) Challenges in the management of acute postsurgical pain. Pharmacother J Hum Pharmacol Drug Therapy 32(9pt2):6–11
Uzzaman MM, Siddiqui MRS (2011) A brief literature review on the management of post-haemorrhoidectomy pain. Surg Tech Dev 1(2):32
Garcia G et al (2011) Antinociception induced by atorvastatin in different pain models. Pharmacol Biochem Behav 100(1):125–129
Pathak NN et al (2015) Effect of atorvastatin, a HMG-CoA reductase inhibitor in monosodium iodoacetate-induced osteoarthritic pain: implication for osteoarthritis therapy. Pharmacol Rep 67(3):513–519
Pathak NN et al (2014) Atorvastatin attenuates neuropathic pain in rat neuropathy model by down-regulating oxidative damage at peripheral, spinal and supraspinal levels. Neurochem Int 68:1–9
Farsaei S et al (2014) Efficacy of topical atorvastatin for the treatment of pressure ulcers: a randomized clinical trial. Pharmacother J Hum Pharmacol Drug Therapy 34(1):19–27
Toker S et al (2009) Topical atorvastatin in the treatment of diabetic wounds. Am J Med Sci 338(3):201–204
Suzuki-Banhesse VF et al (2015) Effect of Atorvastatin on Wound Healing in Rats. Biol Res Nurs 17(2):159–168
Acknowledgments
This research is recorded under trial registration number: IRCT201404013014N8. The study was funded by the Vice-Chancellor of Research of Mazandaran University of Medical Sciences. The authors are grateful to Dr. Khalilian for assistance in data analysis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Ala, S., Alvandipour, M., Saeedi, M. et al. Effects of Topical Atorvastatin (2 %) on Posthemorrhoidectomy Pain and Wound Healing: A Randomized Double-Blind Placebo-Controlled Clinical Trial. World J Surg 41, 596–602 (2017). https://doi.org/10.1007/s00268-016-3749-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-016-3749-x