Abstract
Objective
Induced endothelin-1 (ET-1) production and decreased nitric oxide synthase (NOS) bioavailability have been found in aneurysmal subarachnoid hemorrhage (SAH). Atorvastatin is recognized to have pleiotropic effects including increasing NOS bioavailability as well as reducing inflammation and oxidative damage other than reducing dyslipidemia. This study is of interest to examine the effect of atorvastatin on ET-1/endothelial nitric oxide synthase (eNOS) in experimental SAH.
Methods
A rodent double-hemorrhage SAH model was employed. Animals were randomly assigned as sham-operated, SAH, vehicle plus SAH, 5 mg/day atorvastatin treatment plus SAH and 5 mg/day atorvastatin precondition plus SAH groups. Administration with atorvastatin (5 mg/day) was initiated 1 week before (precondition) and 24 hr later (treatment). Cerebrospinal fluid samples were collected at 72 hr after second SAH. ET-1 (ELISA) was measured. The basilar arteries (BAs) were harvested and sliced, and their cross-sectional areas were measured. Radiolabeled NOS assay kit was used to detect eNOS.
Results
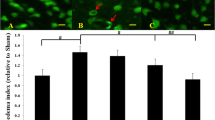
Morphologically, convoluted internal elastic lamina, distorted endothelial cells and myonecrosis of the smooth muscle were predominantly observed in the BA of SAH and vehicle-treated SAH groups, which was not detected in the atorvastatin-preconditioned SAH group or the healthy controls. Significant vasospasm was noted in the vehicle group (lumen potency 64.5%, compared with the sham group, p ≤ 0.01) and less prominent in the atorvastatin treatment group (lumen potency, 76.6%, p < 0.05). In addition, increased ET-1 levels were found in all the animals subject to SAH (SAH only, SAH plus vehicle and SAH plus atorvastatin reversal) except in the atorvastatin precognition group when compared with the healthy controls (no SAH). Likewise, the levels of expressed NOS in BAs is induced in the atorvastatin groups (both atorvastatin treatment and precondition) when compared with that in the SAH group (p < 0.01).
Conclusion
This study offers first evidence that atorvastatin in the preconditioning status reduces the level of ET-1, which corresponds to its antivasospastic effect in the condition of chronic vasospasm. Although there is increased expression of NOS in both atorvastatin precondition and reversal groups, BA’s lumen potency is significantly increased in the atorvastatin precondition group when compared with the SAH group (p < 0.01).



Similar content being viewed by others
Abbreviations
- BA:
-
basilar artery
- CTA:
-
computed tomography angiography
- DSA:
-
digital substration angiography
- eNOS:
-
endothelial nitric oxide synthase
- ET-1:
-
endothelin-1
- IEL:
-
internal elastic lamina
- MRA:
-
magnetic resonance angiography
- PBS:
-
phosphate-buffered saline
- SAH:
-
subarachnoid hemorrhage
References
Amarenco P, Tonkin AM (2004) Statins for stroke prevention: disappointment and hope. Circulation 109:III44–III49
Blanco-Colio LM, Tunon J, Martin-Ventura JL, Egido J (2003) Antiinflammatory and immunomodulatory effects of statins. Kidney Int 63:12–23
Bosel J, Gandor F, Harms C, Synowitz M, Harms U, Djoufack PC, Megow D, Dirnagl U, Hortnag H, Fink KB, Endres M (2005) Neuroprotective effects of atorvastatin against glutamate-induced excito-toxicity in primary cortical neurons. J Neurochem 92:1386–1398
Endres M, Laufs U, Huang Z, Nakamura T, Huang P, Moskowitz MA, Liao JK (1998) Stroke protection by 3-hydroxy-3-methylglutaryl (HMG)-CoA reductase inhibitors mediated by endothelial nitric oxide synthase. Proc Natl Acad Sci USA 95:8880–8885
Erdos B, Snipes JA, Tulbert CD, Katakam P, Miller AW, Busija DW (2006) Rosuvastatin improves cerebrovascular function in Zucker obese rats by inhibiting NAD(P)H oxidase-dependent superoxide production. Am J Physiol Heart Circ Physiol 290:H1264–H1270
Gao F, Gao E, Yue TL, Ohlstein EH, Lopez BL, Christopher TA, Ma XL (2002) Nitric oxide mediates the antiapoptotic effect of insulin in myocardial ischemia-reperfusion: the roles of PI3-kinase, Akt, and endothelial nitric oxide synthase phosphorylation. Circulation 105:1497–1502
Grieve JP, Stacey R, Moore E, Kitchen ND, Jäger HR (1999) Artifact on MRA following aneurysm clipping: an in vitro study and prospective comparison with conventional angiography. Neuroradiology 41(9):680–686
Ho FM, Lin WW, Chen BC, Chao CM, Yang CR, Lin LY, Lai CC, Liu SH, Liau CS (2006) High glucose-induced apoptosis in human vascular endothelial cells is mediated through NF-kappaB and c-Jun NH2-terminal kinase pathway and prevented by PI3K/Akt/eNOS pathway. Cell Sign 18:391–399
Inoue I, Goto MK, Awata T, Mastunaga T, Kawai S, Nakajima T, Hokari S, Komoda T, Katayama S (2000) Lipophilic HMG-CoA reductase inhibitor has an anti-inflammatory effect: reduction of MRNA levels for interleukin-1β, interleukin-6, cyclooxygenase-2, and p22phox by regulation of peroxisome proliferator-activated receptor α (PPARα) in primary endothelial cells. Life Sci 67:863–876
Jeon H, Ai J, Sabri M, Tariq A, Shang X, Chen G, Macdonald RL (2009) Neurological and neurobehavioral assessment of experimental subarachnoid hemorrhage. BMC Neurosci 10:102–129
Jeng AY, Mulder P, Kwan AL, Battistini B (2002) Nonpeptidic endothelin-converting enzyme inhibitors and their potential therapeutic applications. Can J Physiol Pharmacol 80(5):440–449
Jolicoeur FB, Rondeau DB, Hamel E, Butterworth RF, Barbeau A (1979) Measurement of ataxia and related neurological signs in the laboratory rat. Can J Neurol Sci 6(2):209–215
Kästner S, Oertel MF, Scharbrodt W, Krause M, Böker DK, Deinsberger W (2005) Endothelin-1 in plasma, cisternal CSF and microdialysate following aneurysmal SAH. Acta Neurochir (Wien) 147(12):1271–1279, discussion 1279
Kiener PA, Davis PM, Murray JL, Youssef S, Rankin BM, Kowala M (2001) Stimulation of inflammatory responses in vitro and in vivo by lipophilic HMG-CoA reductase inhibitors. Int Immunopharmacol 1:105–118
Kureish Y, Luo Z, Shiojima I, Bialik A, Fulton D, Lefer DJ, Sessa WC, Walsh K (2000) The HMG-CoA reductase inhibitor simvastatin activates the protein kinase Akt and promotes angiogenesis in normocholesterolemic animals. Nat Med 6:1004–1010
Laufs U, Fata VL, Liao JK (1997) Inhibition of 3-hydroxy-3-methylglutaryl (HMG)-CoA reductase blocks hypoxia-mediated down-regulation of endothelial nitric oxide synthase. J Biol Chem 272:31725–31729
Jk L, Laufs U (2005) Pleiotropic effects of statins. Annu Rev Pharmacol Toxicol 45:89–118
Lindberg C, Crisby M, Winblad B, Schultzberg M (2005) Effects of statins on microglia. J Neurosci Res 82:10–19
Lynch JR, Wang H, McGirt MJ, Floyd J, Friedman AH, Coon AL, Blessing R, Alexander MJ, Graffagnino C, Warner DS, Laskowitz DT (2005) Simvastatin reduces vasospasm after aneurismal subarachnoid hemorrhage: results of a pilot randomized clinical trial. Stroke 36:2024–2026
März P, Otten U, Miserez AR (2007) Statins induce differentiation and cell death in neurons and astroglia. Glia 55:1–12
Mayberg MR, Okada T, Bark DH (1990) The role of hemoglobin in arterial narrowing after subarachnoid hemorrhage. J Neurosurg 72:634–640
McGirt MJ, Lynch JR, Parra A, Sheng H, Pearlstein RD, Laskowitz DT, Pelligrino DA, Warner DS (2002) Simvastatin increases endothelial nitric oxide synthase and ameliorates cerebral vasospasm resulting from subarachnoid hemorrhage. Stroke 33:2950–2965
McGirt MJ, Blessing R, Alexander MJ, Nimjee SM, Woodworth GF, Friedman AH, Graffagnino C, Laskowitz DT, Lynch JR (2006) Risk of cerebral vasospasm after subarachnoid hemorrhage reduced by statin therapy: a multivariate analysis of an institutional experience. J Neurosurg 105:671–674
McGirt MJ, Pradilla G, Legnani FG, Thai QA, Recinos PF, Tamargo RJ, Clatterbuck RE (2006) Systemic administration of simvastatin after the onset of experimental subarachnoid hemorrhage attenuates cerebral vasospasm. Neurosurgery 58:945–951
Ohkita M, Sugii M, Ka Y, Kitamura A, Mori T, Hayashi T, Takaoka M, Matsumura Y (2006) Differential effects of different statins on endothelin-1 gene expression and endothelial NOS phosphorylation in porcine aortic endothelial cells. Exp Biol Med 231(6):772–776
Ongini E, Impagnatiello F, Bonazzi A, Guzzetta M, Govoni M, Monopoli A, Del Soldato P, Ignarro LJ (2004) Nitric oxide (NO)-releasing statin derivatives; a class of drugs showing enhanced antiproliferative and anti-inflammatory properties. Proc Natl Acad USA 101:8497–8502
Patel TR, Corbett SA (2004) Simvastatin suppresses LPS-induced Akt phosphrylation in the human monocyte cell line THP-1. J Surg Res 116:116–120
Pelat M, Dessy C, Massion P, Desager JP, Feron O, Balligand JL (2003) Rosuvastatin decreases caveolin-1 and improves nitric oxide-dependent heart rate and blood pressure variability in apolipoprotein E −/− mice in vivo. Circulation 107:2480–2486
Pezzini A, Del Zotto E, Volonghi I, Giossi A, Costa P, Padovani A (2009) New insights into the pleiotropic effects of statins for stroke prevention. Mini Rev Med Chem (7):794–804.
Puglielli L, Tanzi RE, Kovacs DM (2003) Alzheimer’s disease: the cholesterol connection. Nat Neurosci 6:345–351
Rosenson RS, Tangney CC, Casey LC (1999) Inhibition of proinflammatory cytokine production by pravastatin. Lancet 353:245–257
Sellner J, Greeve I, Findling O, Kamm CP, Minten C, Engelhardt B, Grandgirard D, Leib SL, Mattle HP (2008) Effect of interferon-beta and atorvastatin on Th1/Th2 cytokines in multiple sclerosis. Neurochem Int 53(1–2):17–21
Shinichi T, Osamu S, Shigekazu T, Yukihiko F, Tetsuo K, Ryuichi T (1997) Detection of delayed cerebral vasospasm, after rupture of intracranial aneurysms, by magnetic resonance angiography. Neurosurgery 40(4):748–754
Sugawara T, Ayer R, Jadhav V, Chen W, Tsubokawa ZJH (2008) Simvastatin attenuation of cerebral vasospasm after subarachnoid hemorrhage in rats via increased phosphorylation of Akt and endothelial nitric oxide synthase. J Neurosci Res 86:3635–3643
Tanaka T, Tatsuno I, Uchida D, Moroo I, Morio H, Nakamura NY, Yasuda T, Kitagawa M, Saito Y, Harai A (2000) Geranylgeranylpyrophosphate, an isoprenoid of mevalonate cascade, is a critical compound for rat primary cultured cortical neurons to protect the cell death induced by 3-hydoxy-3-methlyglutary-CoA reductase inhibition. J Neursci 20:2852–2859
Tseng MY, Czosnyka M, Richards H, Pickard JD, Kirkpatrick PJ (2005) Effects of acute treatment with pravastatin on cerebral vasospasm, autoregulation, and delayed ischemic deficits after aneurismal subarachnoid hemorrhage: a phase II randomized placebo-controlled trial. Stroke 36:1627–1632
Jc VD, Peters MJ, van Halm VP, van der Horst-Bruinsma IE, Dijkmans BA, Nurmohamed MT (2006) Statin therapy might be beneficial for patients with ankylosing spondylitis. Ann Rheum Dis 65(5):695–696
Vaughan CJ, Delanty N (1999) Neuroprotective properties of statins in cerebral ischemia and stroke. Stroke 30:1969–1973
Vauzour D, Vafeiadou K, Rice-Evans C, Williams RJ, Spencer JP (2007) Activation of pro-survival Akt and ERK1/2 signalling pathways underlie the anti-apoptotic effects of flavanones in cortical neurons. J Neurochem 103:1355–1367
Wang J, Tokoro T, Matsui K, Higa S, Kitajima I (2005) Pitavastatin at low dose activates endothelial nitric oxide synthase through PI3-AKT pathway in endothelial cells. Life Sci 76:2257–2268
Wei X, Chen X, Fontanilla C, Zhao L, Liang Z, Dodel R, Hampel H, Farlow M, Du Y (2007) C/T conversion alters interleukin-1A promoter function in a human astrocyte cell line. Life Sci 80(12):1152–1156
Wolfrum S, Dendorfer A, Schutt M, Weidtmann B, Heep A, Tempel K, Llein HH, Dominiak P, Richardt G (2004) Simvastatin acutely reduces myocardial reperfusion injury in vivo by activating the phosphatidylinositide 3-kinase/Akt pathway. J Cardiovas Pharmacol 44:348–355
Disclaimer
There are no conflicts of interest related to this paper.
Author information
Authors and Affiliations
Corresponding author
Additional information
Comments
Treatment of SAH related vasospasm remains a major clinical problem, for which new vasoactive and neuroprotective drug therapies are very much needed.
Quite recently, prior use of statins has been reported to reduce SAH related neurological deficits. Although clinical studies on the subject have been controversial, a recent meta-analysis confirms the beneficial effect of statin using on SAH induced vasospasm, ischemic deficits, and neurological injury (1). The molecular basis for the protective effect of statins after SAH is a subject of intense investigation.
Another promising drug therapy for vasospasm are endothelin antagonists that are undergoing clinical trials for the treatment of SAH induced vasospasm. The molecular basis for their use in vasospasm has been well demonstrated in animal models of SAH.
The data reported by Chang et al. shows that statin use prior to SAH reduces SAH related vasospasm and neurological deficits by increasing eNOS production and decreasing endothelin-1 levels, which might suggest that atorvastatin preconditioned rats, had a healthier endothelium or a less severe inflammatory response as a reaction to the SAH.
This study by Chang et al. links the effects of statins to the biology of endothelins, which are well documented to have an important role in vasospasm in animal models. As such, this study contributes to our understanding of why statin use may be beneficial for SAH patients.
1. Sillberg VA, Wells GA, Perry JJ. Do Statins Improve Outcomes and Reduce the Incidence of Vasospasm After Aneurysmal Subarachnoid Hemorrhage? A Meta-Analysis. Stroke 2008;39:2622-2626.
Juhana Frösen
Mika Niemelä
Juha Hernesniemi
Helsinki, Finland
Aij-Lie Kwan same contribution as the first author.
Rights and permissions
About this article
Cite this article
Chang, CZ., Wu, SC., Lin, CL. et al. Atorvastatin preconditioning attenuates the production of endothelin-1 and prevents experimental vasospasm in rats. Acta Neurochir 152, 1399–1406 (2010). https://doi.org/10.1007/s00701-010-0652-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-010-0652-3