Abstract
Background
Persistent hyperparathyroidism (HPT) after renal transplantation (RTx), termed tertiary HPT (THPT), is not uncommon. However, risk factors and appropriate operative procedures for THPT are poorly understood.
Methods
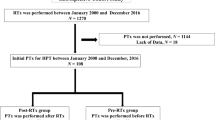
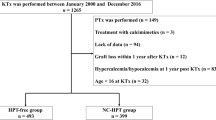
A retrospective study of patients who underwent RTx without pre-transplant parathyroidectomy (PTx) was performed at our hospital between January 2001 and March 2011. Risk factors for the development of THPT were investigated by comparing THPT and non-THPT groups. We retrospectively analyzed patients with THPT who underwent total PTx with forearm autograft. Pre- and postoperative (1 year after PTx) laboratory results were analyzed for PTx efficacy.
Results
Data for 520 patients were analyzed. On multivariate analysis, long dialysis duration (p = 0.009, hazard ratio (HR) 1.01), large maximum parathyroid gland size before RTx (p = 0.003, HR 1.23), pre-RTx high intact parathyroid hormone (iPTH) (p = 0.041, HR 1.01), post-RTx (<2 weeks) high calcium (Ca) (p < 0.001, HR 25.04), and post-RTx high alkaline phosphatase (ALP) (p = 0.027, HR 0.99) were identified as risk factors for THPT. Patients who underwent PTx showed significant improvement compared with baseline for serum Ca, phosphorus, iPTH, and ALP. Serum creatinine showed no significant difference.
Conclusions
Several risk factors for THPT development were identified. PTx for patients with THPT significantly improved serum Ca, iPTH, ALP, and phosphorous levels. There was no significant difference in renal function after PTx. Therefore, total PTx with forearm autograft may be an appropriate surgical approach for patients with THPT.



Similar content being viewed by others
Abbreviations
- HPT:
-
Hyperparathyroidism
- RTx:
-
Renal transplantation
- THPT:
-
Tertiary HPT
- Ca:
-
Calcium
- ALP:
-
Alkaline phosphatase
- PTH:
-
Parathyroid hormone
- SHPT:
-
Secondary HPT
- PTx:
-
Parathyroidectomy
- BMD:
-
Bone mineral density
- BMI:
-
Body mass index
- P:
-
Phosphorus
- iPTH:
-
Intact PTH
- Cre:
-
Creatinine
- SD:
-
Standard deviation
- HR:
-
Hazard ratio
References
Pihlstrom H, Dahle DO, Mjoen G et al (2015) Increased risk of all-cause mortality and renal graft loss in stable renal transplant recipients with hyperparathyroidism. Transplantation 99:351–359
Evenepoel P, Claes K, Kuypers D et al (2004) Natural history of parathyroid function and calcium metabolism after kidney transplantation: a single-center study. Nephrol Dial Transplant 19:1281–1287
Torres A, Rodriguez AP, Concepcion MT et al (1998) Parathyroid function in long-term renal transplant patients: importance of pre-transplant PTH concentrations. Nephrol Dial Transplant 13:94–97
Evenepoel P, Kuypers D, Maes B et al (2001) Persistent hyperparathyroidism after kidney transplantation requiring parathyroidectomy. Acta Otorhinolaryngol Belg 55:177–186
Taniguchi M, Tokumoto M, Matsuo D et al (2006) Persistent hyperparathyroidism in renal allograft recipients: vitamin D receptor, calcium-sensing receptor, and apoptosis. Kidney Int 70:363–370
Hamidian Jahromi A, Roozbeh J, Raiss-Jalali GA et al (2009) Risk factors of post renal transplant hyperparathyroidism. Saudi J Kidney Dis Transpl 20:573–576
Pitt SC, Panneerselvan R, Chen H et al (2009) Tertiary hyperparathyroidism: is less than a subtotal resection ever appropriate? A study of long-term outcomes. Surgery 146:1130–1137
Gilat H, Feinmesser R, Vinkler Y et al (2007) Clinical and operative management of persistent hyperparathyroidism after renal transplantation: a single-center experience. Head Neck 29:996–1001
Triponez F, Kebebew E, Dosseh D et al (2006) Less-than-subtotal parathyroidectomy increases the risk of persistent/recurrent hyperparathyroidism after parathyroidectomy in tertiary hyperparathyroidism after renal transplantation. Surgery 140:990–997 discussion 997–999
Kerby JD, Rue LW, Blair H et al (1998) Operative treatment of tertiary hyperparathyroidism: a single-center experience. Ann Surg 227:878–886
Okada M, Tominaga Y, Izumi K et al (2011) Tertiary hyperparathyroidism resistant to cinacalcet treatment. Ther Apher Dial 15:33–37
Triponez F, Clark OH, Vanrenthergem Y et al (2008) Surgical treatment of persistent hyperparathyroidism after renal transplantation. Ann Surg 248:18–30
Wells SA Jr, Gunnells JC, Shelburne JD et al (1975) Transplantation of the parathyroid glands in man: clinical indications and results. Surgery 78:34–44
Tominaga Y, Matsuoka S, Sato T (2005) Surgical indications and procedures of parathyroidectomy in patients with chronic kidney disease. Ther Apher Dial 9:44–47
Egbuna OI, Taylor JG, Bushinsky DA et al (2007) Elevated calcium phosphate product after renal transplantation is a risk factor for graft failure. Clin Transplant 21:558–566
Dewberry LC, Tata S, Graves S et al (2014) Predictors of tertiary hyperparathyroidism: Who will benefit from parathyroidectomy? Surgery 156:1631–1636 discussion 1636–1637
Thiem U, Gessl A, Borchhardt K (2015) Long-term clinical practice experience with cinacalcet for treatment of hypercalcemic hyperparathyroidism after kidney transplantation. Biomed Res Int 2015:292654
Evenepoel P, Cooper K, Holdaas H et al (2014) A randomized study evaluating cinacalcet to treat hypercalcemia in renal transplant recipients with persistent hyperparathyroidism. Am J Transplant 14:2545–2555
Cohen JB, Gordon CE, Balk EM et al (2012) Cinacalcet for the treatment of hyperparathyroidism in kidney transplant recipients: a systematic review and meta-analysis. Transplantation 94:1041–1048
Chou FF, Hsieh KC, Chen YT et al (2008) Parathyroidectomy followed by kidney transplantation can improve bone mineral density in patients with secondary hyperparathyroidism. Transplantation 86:554–557
Evenepoel P, Claes K, Kuypers D et al (2005) Impact of parathyroidectomy on renal graft function, blood pressure and serum lipids in kidney transplant recipients: a single center study. Nephrol Dial Transplant 20:1714–1720
Schlosser K, Endres N, Celik I et al (2007) Surgical treatment of tertiary hyperparathyroidism: the choice of procedure matters. World J Surg 31:1947–1953. doi:10.1007/s00268-007-9187-z
Acknowledgments
We thank Ms. Mitoko Imai, Ms. Mayumi Nobata, and Ms. Sayoko Ito of the Nagoya Daini Red Cross Hospital for their help with sample and data collection.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no competing interests to declare.
Rights and permissions
About this article
Cite this article
Yamamoto, T., Tominaga, Y., Okada, M. et al. Characteristics of Persistent Hyperparathyroidism After Renal Transplantation. World J Surg 40, 600–606 (2016). https://doi.org/10.1007/s00268-015-3314-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-015-3314-z