Abstract
Introduction
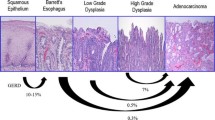
Barrett’s esophagus (BE) is the result of continuous injury of the esophageal mucosa by gastric refluxate. This condition can progress to low-grade (LGD) and high-grade dysplasia (HGD) and eventually to adenocarcinoma. While excellent results are reported in terms of reflux and symptom control in patients with BE undergoing antireflux surgery (ARS), the impact of a fundoplication on progression and regression of dysplasia is debated. The aim of this article is to review the effects of ARS on regression and progression of LGD to HGD or cancer in patients with dysplastic BE.
Materials and Methods
A review of the literature in PubMed/Medline electronic databases has been performed.
Results
ARS might decrease but not eliminate the risk of progression to dysplasia or cancer in BE patients. ARS may promote regression of dysplastic BE only in short-segment BE, but not in long-segment BE. Modulation of gene expression is involved in the genesis and reversion of short-segment intestinal metaplasia after ARS.
Conclusions
Close and long-term surveillance by 24-hour pH monitoring and upper endoscopy is recommended in BE patients who undergo ARS to identify postoperative pathological reflux, and to early detect dysplasia or even adenocarcinoma. Further studies are requested to assess the molecular effects of ARS in dysplastic BE.
Similar content being viewed by others
References
Dent J, El Serag HB, Wallander MA et al (2005) Epidemiology of gastro-oesophageal reflux disease: a systematic review. Gut 54:710–717
Patti MG, Arcerito M, Feo CV et al (1999) Barrett’s esophagus: a surgical disease. J Gastrointest Surg 3:397–403
Rugge M, Zaninotto G, Parente P et al (2012) Barrett’s esophagus and adenocarcinoma risk: the experience of the North-Eastern Italian Registry (EBRA). Ann Surg 256:788–794
Oh DS, DeMeester SR (2010) Pathophysiology and treatment of Barrett’s esophagus. World J Gastroenterol 16:3762–3772
Dallemagne B, Weerts J, Markiewicz S et al (2006) Clinical results of laparoscopic fundoplication at ten years after surgery. Surg Endosc 20:159–165
Parrilla P, Martinez de Haro LF, Ortiz A et al (2003) Long-term results of a randomized prospective study comparing medical and surgical treatment of Barrett’s esophagus. Ann Surg 237:291–298
Katz PO, Zavala S (2010) Proton pump inhibitors in the management of GERD. J Gastrointest Surg 14(Suppl 1):S62–S66
Tamhankar AP, Peters JH, Portale G et al (2004) Omeprazole does not reduce gastroesophageal reflux: new insights using multichannel intraluminal impedance technology. J Gastrointest Surg 8:890–897
Blonski W, Vela MF, Castell DO (2009) Comparison of reflux frequency during prolonged multichannel intraluminal impedance and pH monitoring on and off acid suppression therapy. J Clin Gastroenterol 43:816–820
Tutuian R, Vela MF, Hill EG et al (2008) Characteristics of symptomatic reflux episodes on acid suppressive therapy. Am J Gastroenterol 103:1090–1096
Corly DA, Kubo A, Zhao W et al (2010) Proton pump inhibitors and histamine-2 receptor antagonists are associated with hip fractures among at-risk patients. Gastroenterology 139:93–101
Abraham NS (2012) Proton pump inhibitors: potential adverse effects. Curr Opin Gastroenterol 28:615–620
Herbella FA, Tedesco P, Nipomnick I et al (2007) Effect of partial and total laparoscopic fundoplication on esophageal body motility. Surg Endosc 21:285–288
Katzka DA, Castell DO (1994) Successful elimination of reflux symptoms does not insure adequate control of acid reflux in patients with Barrett’s esophagus. Am J Gastroenterol 89:989–991
Attwood SE, Lundell L, Hatlebakk JG et al (2008) Medical or surgical management of GERD patients with Barrett’s esophagus: the LOTUS trial 3-year experience. J Gastrointest Surg 12:1646–1654
Kauer WK, Peters JH, DeMeester TR et al (1995) Mixed reflux of gastric and duodenal juices is more harmful to the esophagus than gastric juice alone. The need for surgical therapy re-emphasized. Ann Surg 222:525–531
McCallum R, Polepalle S, Davenport K et al (1991) Role of anti-reflux surgery against dysplasia in Barrett’s esophagus. Gastroenterology 100:A121
Katz D, Rothstein R, Schned A et al (1998) The development of dysplasia and adenocarcinoma during endoscopic surveillance of Barrett’s esophagus. Am J Gastroenterol 93:536–541
Ortiz A, Martinez de Haro LF, Parrilla P et al (1996) Conservative treatment versus antireflux surgery in Barrett’s oesophagus: long-term results of a prospective study. Br J Surg 83:274–278
Öberg S, Wenner J, Johansson J et al (2005) Barrett esophagus: risk factors for progression to dysplasia and adenocarcinoma. Ann Surg 242:49–54
Oelschlager BK, Barreca M, Chang L et al (2003) Clinical and pathologic response of Barrett’s esophagus to laparoscopic antireflux surgery. Ann Surg 238:458–464
Chang EY, Morris CD, Seltman AK et al (2007) The effect of antireflux surgery on esophageal carcinogenesis in patients with Barrett esophagus: a systematic review. Ann Surg 246:11–21
Csendes A, Burdiles P, Braghetto I et al (2002) Dysplasia and adenocarcinoma after classic antireflux surgery in patients with Barrett’s esophagus: the need for long-term subjective and objective follow-up. Ann Surg 235:178–185
O’Riordan JM, Byrne PJ, Ravi N et al (2004) Long-term clinical and pathologic response of Barrett’s esophagus after antireflux surgery. Am J Surg 188:27–33
Lagergren J, Viklund P (2007) Is esophageal adenocarcinoma occurring late after antireflux surgery due to persistent postoperative reflux? World J Surg 31:465–469
Zehetner J, deMeester SR, Ayazi S et al (2010) Long-term follow-up after anti-reflux surgery in patients with Barrett’s esophagus. J Gastrointest Surg 14:1483–1491
Wang KK, Sampliner RE (2008) Practice Parameters Committee of the American College of Gastroenterology. Updated guidelines 2008 for the diagnosis, surveillance and therapy of Barrett’s esophagus. Am J Gastroenterol 103:788–797
Gurski RR, Peters JH, Hagen JA et al (2003) Barrett’s esophagus can and does regress after antireflux surgery: a study of prevalence and predictive features. J Am Coll Surg 196:706–712
Rossi M, Barreca M, de Bortoli N et al (2006) Efficacy of Nissen fundoplication versus medical therapy in the regression of low-grade dysplasia in patients with Barrett esophagus. A prospective study. Ann Surg 243:58–63
Oh DS, DeMeester SR, Vallbohmer D et al (2007) Reduction of interleukin-8 gene expression in reflux esophagitis and Barrett’s esophagus with antireflux surgery. Arch Surg 142:554–559
Babar M, Ennis D, Abdel-Latif M et al (2010) Differential molecular changes in patients with asymptomatic long-segment Barrett’s esophagus treated by antireflux surgery or medical therapy. Am J Surg 199:137–143
Zaninotto G, Cassaro M, Pennelli G et al (2005) Barrett’s epithelium after antireflux surgery. J Gastrointest Surg 9:1253–1261
Zaninotto G, Parente P, Salvador R et al (2012) Long-term follow-up of Barrett’s epithelium: medical versus antireflux surgical therapy. J Gastrointest Surg 16:7–14
Conflict of interest
The authors have no conflicts of interest to declare.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Allaix, M.E., Patti, M.G. Antireflux Surgery for Dysplastic Barrett. World J Surg 39, 588–594 (2015). https://doi.org/10.1007/s00268-014-2632-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-014-2632-x