Abstract
Background
The prognosis of solitary liver metastasis involving the caudate lobe is unclear. This study analyzed the outcomes after resection of the caudate lobe for solitary colorectal liver metastasis.
Methods
We reviewed the records of 114 cases in which potentially curative hepatectomy were performed for solitary colorectal liver metastasis. Solitary liver metastasis involving the caudate lobe was seen in 14 cases (Caudate group). The outcomes were compared with those of the remaining 100 cases with metastasis in a site other than the caudate lobe (Other group).
Results
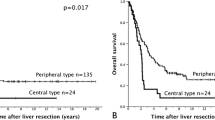
No hospital deaths occurred. The 5-year survival rate for all cases was 61%. Recurrence-free and cumulative survivals were similar in the two groups, as were the intraoperative blood loss, duration of operation, and postoperative hospital stay. The distance of the surgical margin was significantly shorter in the Caudate group than in the Other group (0.6 mm vs. 6.6 mm; p = 0.001). A concomitant resection of the inferior vena cava was performed in four patients in the Caudate group but in no patients in the Other group (p < 0.001).
Conclusions
Despite a minimal surgical margin, the resection of solitary colorectal liver metastasis offers favorable short- and long-term outcomes comparable to those for colorectal liver metastasis at other sites.

Similar content being viewed by others
References
Cunningham D, Humblet Y, Siena S, et al (2004) Cetuximab monotherapy and cetuximab plus irinotecan in irinotecan-refractory metastatic colorectal cancer. N Engl J Med 351:337–345
Hurwitz H. (2004) Integrating the anti-VEGF-A humanized monoclonal antibody bevacizumab with chemotherapy in advanced colorectal cancer. Clin Colorectal Cancer 4(Suppl 2):S62–S68
Saltz LB, Meropol NJ, Loehrer PJ Sr, et al (2004) Phase II trial of cetuximab in patients with refractory colorectal cancer that expresses the epidermal growth factor receptor. J Clin Oncol 22:1201–1208
Aloia TA, Vauthey JN, Loyer EM, et al (2006) Solitary colorectal liver metastasis: resection determines outcome. Arch Surg 141:460–466; discussion 466–467
Minagawa M, Makuuchi M, Torzilli G, et al (2000) Extension of the frontiers of surgical indications in the treatment of liver metastases from colorectal cancer: long-term results. Ann Surg 231:487–499
Wagner JS, Adson MA, Van Heerden JA, et al (1984) The natural history of hepatic metastases from colorectal cancer: a comparison with resective treatment. Ann Surg 199:502–508
Belghiti J, Hiramatsu K, Benoist S, et al (2000) Seven hundred forty-seven hepatectomies in the 1990s: an update to evaluate the actual risk of liver resection. J Am Coll Surg 191:38–46
Fong Y, Fortner J, Sun RL, et al (1999) Clinical score for predicting recurrence after hepatic resection for metastatic colorectal cancer: analysis of 1001 consecutive cases. Ann Surg 230:309–308; discussion 318–321
Hawkins WG, DeMatteo RP, Cohen MS, et al (2005) Caudate hepatectomy for cancer: a single institution experience with 150 patients. J Am Coll Surg 200:345–352
Bartlett D, Fong Y, Blumgart LH (1996) Complete resection of the caudate lobe of the liver: technique and results. Br J Surg 83:1076–1081
Sarmiento JM, Que FG, Nagorney DM (2002) Surgical outcomes of isolated caudate lobe resection: a single series of 19 patients. Surgery 132:697–708; discussion 708–709
Tanaka K, Shimada H, Matsuo K, et al (2005) Surgical outcome of solitary colorectal metastasis to the hepatic caudate lobe. Br J Surg 92:847–848
Saiura A, Yamamoto J, Koga R, et al (2006) Usefulness of LigaSure for liver resection: analysis by randomized clinical trial. Am J Surg 192:41–45
Fortner JG, Silva JS, Golbey RB, et al (1984) Multivariate analysis of a personal series of 247 consecutive patients with liver metastases from colorectal cancer. I. Treatment by hepatic resection. Ann Surg 199:306–316
Hughes KS, Simon R, Songhorabodi S, et al (1986) Resection of the liver for colorectal carcinoma metastases: a multi-institutional study of patterns of recurrence. Surgery 100:278–284
Ekberg H, Tranberg KG, Anderson R, et al (1987) Pattern of recurrence in liver resection for colorectal secondaries. World J Surg 11:541–547
Cady B, Jenkins RL, Steele GD, et al (1998) Surgical margin in hepatic resection for colorectal metastasis: a critical and improvable determinant of outcome. Ann Surg 227:566–571
Yamamoto J, Sugihara K, Kosuge T, et al (1995) Pathologic support for limited hepatectomy in the treatment of liver metastases from colorectal cancer. Ann Surg 221:74–78
Elias D, Cavalcanti A, Sabourin JC, et al (1998) Results of 136 curative hepatectomies with a safety margin of less than 10 mm for colorectal metastases. J Surg Oncol 69:88–93
Stephenson KR, Steinberg SM, Hughes KS, et al (1988) Perioperative blood transfusions are associated with decreased time to recurrence and decreased survival after resection of colorectal liver metastases. Ann Surg 208:679–687
Acknowledgments
This study was supported by a Grant–in-Aid for Basic Research from the Ministry of Education, Culture, Sports, Science, and Technology (A.S.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Saiura, A., Yamamoto, J., Koga, R. et al. Outcome After Hepatic Resection of Solitary Liver Metastasis from Colorectal Cancer in the Caudate Lobe. World J Surg 31, 2378–2383 (2007). https://doi.org/10.1007/s00268-007-9250-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-007-9250-9