Abstract
Background
Despite the recent wide availability of ultrasonography and fine-needle aspiration biopsy, endocrine surgeons often encounter incidental papillary carcinoma (IPC), that is a papillary carcinoma that had gone undetected by preoperative imaging studies but was identified by pathological examination of surgical specimens resected for benign thyroid diseases.
Methods
The present study was developed to investigate the prognoses of 317 patients who underwent surgery for benign diseases involving IPC in comparison with the prognoses of 1,674 patients with clinically apparent papillary carcinoma detected preoperatively and diagnosed.
Results
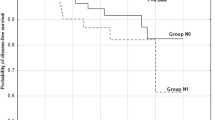
None of the patients underwent further surgery such as completion total thyroidectomy and node dissection immediately after the diagnosis of IPC. To date, 7 patients (2.2%) have had recurrences; 6 of those were locoregional recurrences and one was a bone metastasis. None of the patients have died of thyroid carcinoma. The disease-free survival of IPC patients was significantly better than that of clinically apparent papillary carcinoma patients and was similar to that of the subset of patients with papillary microcarcinoma without clinically apparent metastasis.
Conclusions
Because IPC is associated with good prognosis, further surgery, such as completion total thyroidectomy or lymph node dissection immediately after the diagnosis of IPC is not necessary.


Similar content being viewed by others
References
Sobin LH, Wittekind CH. (2002) UICC: TNM Classification of Malignant Tumors, 6th Edition, New York, Wiley-Liss
Takebe K, Date M, Yamamoto Y, et al. (1994) Mass screening for thyroid cancer with ultrasonography. KARKINOS 7:309–317 (in Japanese)
Renshaw AA (2005) Papillary carcinoma of the thyroid <1.0 cm. Cancer Cytopathol 105:217–219
Steele SR, Martin MJ, Mullenix PS, et al. (2005) The significance of incidental thyroid abnormalities identified during carotid duplex ultrasonography. Arch Surg 140:981–985
Harach HR, Franssila KO, Wasenius VM. (1985) Occult papillary carcinoma of the thyroid: a “normal” finding in Finland. A systematic autopsy study. Cancer 56:531–538
Fukunaga FH, Yatani R. (1975) Geographic pathology of occult thyroid carcinomas. Cancer 36:1095–1099
Thorvaldsson SE, Tulinius H, Bjornsson J, et al. (1992) Latent thyroid carcinoma in Iceland at autopsy. Pathol Res Pract 188:747–750
Lang W, Borrusch G, Bauer L. (1988) Occult carcinomas of the thyroid. Am J Clin Pathol 90:72–76
Iida F, Sugenoya A, Muramatsu A. (1991) Clinical and pathologic properties of small differentiated carcinomas of the thyroid gland. World J Surg 15:511–515
Hay ID, Grant CS, van Heerden JA, et al. (1992) Papillary thyroid microcarcinoma: a study of 535 cases observed in a 50-year period. Surgery 112:1139–1147
Rodriguez JM, Moreno A, Parrila P, et al. (1997) Papillary thyroid microcarcinoma: clinical study and prognosis. Eur J Surg 163:255–259
Sugitani I, Fumimoto Y. (1999) Symptomatic versus asymptomatic papillary thyroid microcarcinoma: a retrospective analysis of surgical outcome and prognostic factors. Endocrine J 46:209–216
Wada N, Duh QY, Sugino K, et al. (2003) Lymph node metastasis from 259 papillary thyroid microcarcinomas. Ann Surg 237:399–407
Ito Y, Uruno R, Nakano K, et al. (2003) An observation trial without surgical treatment in patients with papillary microcarcinoma of the thyroid. Thyroid 13:381–388
Ito Y, Tomoda C, Uruno T, et al. (2004) Papillary microcarcinoma of the thyroid: how should it be treated? World J Surg 28:1115–1121
Mori I, Miyauchi A, Kuma S, et al. (2003) Thyroid nodular lesion: analysis of cancer risk based on Kuma Hospital experience. Pathol Int 53:579–583
Chigot JP, Menegaux F, Keopadabsky K, et al. (2000) Thyroid cancer in patients with hyperthyroidism. Presse Med 29:1969–1972 (in French)
Miccoli P, Minuto MN, Galleri D, et al. (2006) Incidental thyroid carcinoma in a large series of consecutive patients operated on for benign thyroid disease. Aust N Z J Surg 76:123–126
Lokey JS, Palmer RM, Macfie JA, et al. (2005) Unexpected findings during thyroid surgery in a regional community hospital: a 5-year experience of 738 consecutive cases. Am Surg 11:911–915
Barbaro D, Simit U, Meucci G, et al. (2005) Thyroid papillary cancers; microcarcinoma and carcinoma, incidental cancers and non-incidental cancers—are they different diseases? Clin Endocrinol 63:577–581
Sampson RJ, Key CR. (1970) Smallest forms of papillary carcinoma of the thyroid. Arch Pathol 91:334–339
Carlini M, Giovannini C, Castaldi F, et al. (2005) High risk for microcarcinoma in thyroid benign diseases. Incidence in a one year period of total thyroidectomy. J Exp Cin Cancer Res 24:231–236
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ito, Y., Higashiyama, T., Takamura, Y. et al. Prognosis of Patients with Benign Thyroid Diseases Accompanied by Incidental Papillary Carcinoma Undetectable on Preoperative Imaging Tests. World J Surg 31, 1672–1676 (2007). https://doi.org/10.1007/s00268-007-9131-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00268-007-9131-2