Abstract
Purpose
This is a retrospective study and aims to investigate the clinical outcomes of patients with knee varus deformity and extruded medial meniscus who underwent arthroscopic meniscus centralization and medial opening wedge high tibial osteotomy.
Methods
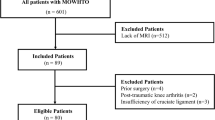
A total of 24 patients were included in the trial, and arthroscopy intraoperative photographs and standing preoperative and postoperative radiographs were taken to analyze the mechanical tibiofemoral angle and tibial plateau inclination. Postoperative complications and knee motion were recorded, and the surgical results were evaluated using the knee society score.
Results
The study observed four cases of surgery-related complications among all patients, but no major complications were reported. The surgery significantly improved knee flexion degrees and total knee range of motion. Satisfactory outcomes were shown in postoperative radiographs and secondary intraoperative photographs. The knee score increased from 39.6 ± 10.0 to 80.1 ± 9.0, and the functional score improved from 48.1 ± 6.9 to 89.4 ± 5.5. The preoperative tibial plateau inclination was 5.3 ± 0.7, while the postoperative data showed a decrease to 4.2 ± 0.7. The preoperative mechanical tibiofemoral angle was − 7.7 ± 1.0, and it improved in all patients postoperatively to 2.8 ± 0.9.
Conclusion
By alternating the knee biomechanics and significantly improving symptoms and quality of life, arthroscopic medial meniscus centralization and medial open wedge high tibial osteotomy units are confirmed to be an effective alternative treatment for knee varus deformity.







Similar content being viewed by others
Code availability
The code availability (software application or custom code) is credible.
References
McCormack DJ, Puttock D, Godsiff SP (2021) Medial compartment osteoarthritis of the knee: a review of surgical options. EFORT Open Rev 6(2):113–117. https://doi.org/10.1302/2058-5241.6.200102
Leafblad ND, Smith PA, Stuart MJ, Krych AJ (2021) Arthroscopic centralization of the extruded medial meniscus. Arthrosc Tech 10(1):e43–e48. https://doi.org/10.1016/j.eats.2020.09.005
Erquicia JI, Gil-Gonzalez S, Ibañez M, Leal-Blanquet J, Combalia A, Monllau JC et al (2022) A lower starting point for the medial cut increases the posterior slope in opening-wedge high tibial osteotomy: a cadaveric study. J Exp Orthop 9(1):124. https://doi.org/10.1186/s40634-022-00562-z
Giuseffi SA, Replogle WH, Shelton WR (2015) Opening-wedge high tibial osteotomy: review of 100 consecutive cases. Arthroscopy 31(11):2128–37. https://www.ncbi.nlm.nih.gov/pubmed/26111594 . https://doi.org/10.1016/j.arthro.2015.04.097
Sung YG, Yoon H, Park DC, Kim MS, In Y (2020) Clinical usefulness of SPECT/CT for assessing postoperative outcomes after medial opening-wedge high tibial osteotomy. Orthop J Sports Med 10(10):23259671221121084. https://doi.org/10.1177/23259671221121083
He M, Zhong X, Li Z, Shen K, Zeng W (2021) Progress in the treatment of knee osteoarthritis with high tibial osteotomy: a systematic review. Syst Rev 10(1):56. https://doi.org/10.1186/s13643-021-01601-z
Katagiri H, Nakagawa Y, Miyatake K, Ohara T, Shioda M, Sekiya I et al (2023) Short-term outcomes after high tibial osteotomy aimed at neutral alignment combined with arthroscopic centralization of medial meniscus in osteoarthritis patients. J Knee Surg 36(3):261–268. https://doi.org/10.1055/s-0041-1731738
Belsey J, Yasen SK, Jobson S, Faulkner J, Wilson AJ (2021) Return to physical activity after high tibial osteotomy or unicompartmental knee arthroplasty: a systematic review and pooling data analysis. Am J Sports Med. 49(5):1372–80. https://www.ncbi.nlm.nih.gov/pubmed/32960075. https://doi.org/10.1177/0363546520948861
Agarwalla A, Christian DR, Liu JN, Garcia GH, Redondo ML, Yanke AB, et al. (2021) Return to work following isolated opening wedge high tibial osteotomy. Cartilage 12(4):468–74. https://www.ncbi.nlm.nih.gov/pubmed/31482720. https://doi.org/10.1177/1947603519852417
Ren YM, Duan YH, Sun YB, Yang T, Hou WY, Zhu RS, et al. (2020) Opening-wedge high tibial osteotomy using autograft versus allograft: a systematic review and meta-analysis. J Knee Surg. 33(6):565–75. https://www.ncbi.nlm.nih.gov/pubmed/30861539. https://doi.org/10.1055/s-0039-1681065
Liu X, Chen Z, Gao Y, Zhang J, Jin Z (2019) (2019) High tibial osteotomy: review of techniques and biomechanics. J Healthcare Eng 2(2019):8363128. https://doi.org/10.1155/2019/8363128
Franulic N, Munoz JT, Figueroa F, Innocenti P, Gaggero N. (2023) Lateral hinge fracture in medial opening wedge high tibial osteotomy: a narrative review. EFORT Open Rev. 8(7):572–80. https://www.ncbi.nlm.nih.gov/pubmed/37395709. https://doi.org/10.1530/EOR-22-0103
Thienpont E, Schwab PE, Cornu O, Bellemans J, Victor J. (2017) Bone morphotypes of the varus and valgus knee. Arch Orthop Trauma Surg. 137(3):393–400. https://www.ncbi.nlm.nih.gov/pubmed/28110363. https://doi.org/10.1007/s00402-017-2626-x
Day M, Wolf BR (2019) Medial opening-wedge high tibial osteotomy for medial compartment arthrosis/overload. Clin Sports Med. 38(3):331–49. https://www.ncbi.nlm.nih.gov/pubmed/31079766. https://doi.org/10.1016/j.csm.2019.02.003
Ozeki N, Koga H, Sekiya I (2022) Degenerative meniscus in knee osteoarthritis: from pathology to treatment. Life (Basel, Switzerland). 12(4). https://doi.org/10.3390/life12040603
Choi HG, Kang YS, Kim JS, Lee HS, Lee YS (2021) Meniscal and cartilage changes on serial MRI after medial opening-wedge high tibial osteotomy. Orthop J Sports Med 9(12):23259671211047904. https://doi.org/10.1177/23259671211047904
Langhans MT, Lamba A, Saris DBF, Smith P, Krych AJ (2023) Meniscal extrusion: diagnosis, etiology, and treatment options. Curr Rev Musculoskelet Med 16(7):316–327. https://doi.org/10.1007/s12178-023-09840-4
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Informed consent
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
The data offered in the trial was collected by the authors and it is credible and completely authentic.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Yun-peng Bai contributed equally to this work and share first authorship.
Wei-bing Sun contributed equally to this work and share corresponding authorship.
Supplementary Information
Below is the link to the electronic supplementary material.
264_2023_5959_MOESM1_ESM.xlsx
Supplementary file1 (XLSX 10 KB)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Wang, M., Bai, Yp., Sun, Wb. et al. Two years follow-up of patients with knee varus deformity and medial meniscus extrusion after medial opening wedge high tibial osteotomy and arthroscopic meniscus centralization. International Orthopaedics (SICOT) 48, 481–486 (2024). https://doi.org/10.1007/s00264-023-05959-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-023-05959-8