Abstract
Purpose
The purpose of this study was to evaluate the long-term clinical and radiographic outcomes of the Balgrist total hip replacement cup.
Methods
We report the results of a retrospective review of 195 total hip prostheses with Balgrist cup implanted in 178 patients. There were 59 men and 119 women with a mean age at surgery of 52.3 years (range, 19–72). Cox regression was used to determine the influence of independent variables on the survivorship of the prosthesis.
Results
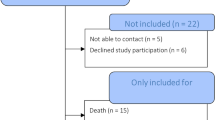
There were 117 (66 %) of 178 patients, and 131 (67 %) of 195 hips available for assessment at a mean follow-up of 17.4 years. A total of 21 patients (22 hips) were lost from follow-up (12 %). A total of 25 patients (27 hips) required some type of re-operation during the follow-up period. Eight of 27 re-operations (30 %) were directly caused by the Balgrist cup failure due to fatigue fracture of the metallic shell (n = 5; 19 %), polyethylene wear (n = 2; 7 %) and aseptic loosening (n = 1; 4 %). The mean polyethylene wear rate was 0.068 mm/year (range, 0.008–0.230; SD = 0.043). The risk of re-operation for any reason was decreased with dysplastic hip as a primary diagnosis (hazard ratio; HR = 0.250; 95 % CI 0.086–0.725) and with greater age at the time of surgery (HR = 0.923; 95 % CI 0.880–0.969). The 19-year survivorship with re-operation for any reason was 75.6 % (95 % CI 67.0–84.2). The 19-year survivorship with re-operation for the Balgrist cup failure was 90.5 % (95 % CI 83.4–97.6).
Conclusions
The Balgrist cup continues to provide excellent clinical and radiological outcomes. This is associated at least in part with a low polyethylene wear rate. The main reason for the Balgrist cup failure is fatigue fracture of the metallic shell.





Similar content being viewed by others
References
Franklin PD, Allison JJ, Ayers DC (2012) Beyond joint implant registries: a patient-centered research consortium for comparative effectiveness in total joint replacement. JAMA 308:1217–1218
Beswick AD, Wylde V, Gooberman-Hill R et al (2012) What proportion of patients report long-term pain after total hip or knee replacement for osteoarthritis? A systematic review of prospective studies in unselected patients. BMJ Open 2:e000435
Clement ND, Biant LC, Breusch SJ (2012) Total hip arthroplasty: to cement or not to cement the acetabular socket? A critical review of the literature. Arch Orthop Trauma Surg 132:411–427
Gallo J, Langova K, Havranek V et al (2008) Poor survival of ABG I hip prosthesis in younger patients. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 152:163–168
Hailer NP, Garellick G, Karrholm J (2010) Uncemented and cemented primary total hip arthroplasty in the Swedish Hip Arthroplasty Register. Acta Orthop 81:34–41
Makela KT, Eskelinen A, Pulkkinen P et al (2011) Results of 3,668 primary total hip replacements for primary osteoarthritis in patients under the age of 55 years. Acta Orthop 82:521–529
Morshed S, Bozic KJ, Ries MD et al (2007) Comparison of cemented and uncemented fixation in total hip replacement: a meta-analysis. Acta Orthop 78:315–326
Wroblewski BM, Siney PD, Fleming PA (2009) Charnley low-frictional torque arthroplasty: follow-up for 30 to 40 years. J Bone Joint Surg Br 91:447–450
Van Der Veen HC, Van Jonbergen HP, Poolman RW et al (2013) Is there evidence for accelerated polyethylene wear in uncemented compared to cemented acetabular components? A systematic review of the literature. Int Orthop 37:9–14
Harris WH (2009) The first 50 years of total hip arthroplasty: lessons learned. Clin Orthop Relat Res 467:28–31
Pokorny D, Slouf M, Fulin P (2012) Current knowledge on the effect of technology and sterilization on the structure, properties and longevity of UHMWPE in total joint replacement. Acta Chir Orthop Traumatol Cech 79:213–221
Rimnac C, Pruitt L, Implant Wear Symposium Engineering Work Group (2008) How do material properties influence wear and fracture mechanisms? J Am Acad Orthop Surg 16(Suppl 1):S94–S100
Santavirta S, Goodman SB (2005) Total hip replacement: a successful interaction of biology, mechanics, and materials science. Clin Orthop Relat Res 430:2
Jacob HA, Hilfiker B (1990) The self-locking Balgrist hip socket for cement-free fixation—history of its development and clinical experience to date. Z Orthop Ihre Grenzgeb 128:254–261
Echtler B, Jacob HA, Houweling M et al (1999) 8-year survivorship analysis and subjective results of 687 primary Balgrist hip sockets. Acta Orthop Belg 65:346–356
Ishaque BA, Basad E, Gils J et al (2009) Long-term results of the cementless conical Balgrist expansion cup—comparison analysis to the Zweymuller-Alloclassic screw cup. Z Orthop Unfall 147:707–715
Pakvis D, Van Hellemondt G, De Visser E et al (2011) Is there evidence for a superior method of socket fixation in hip arthroplasty? A systematic review. Int Orthop 35:1109–1118
Harris WH (1969) Traumatic arthritis of the hip after dislocation and acetabular fractures: treatment by mold arthroplasty. An end-result study using a new method of result evaluation. J Bone Joint Surg Am 51:737–755
Zahiri CA, Schmalzried TP, Szuszczewicz ES et al (1998) Assessing activity in joint replacement patients. J Arthroplast 13:890–895
Charnley J (1972) The long-term results of low-friction arthroplasty of the hip performed as a primary intervention. J Bone Joint Surg Br 54:61–76
Pagnano W, Hanssen AD, Lewallen DG et al (1996) The effect of superior placement of the acetabular component on the rate of loosening after total hip arthroplasty. J Bone Joint Surg Am 78:1004–1014
Engh CA, Massin P, Suthers KE (1990) Roentgenographic assessment of the biologic fixation of porous-surfaced femoral components. Clin Orthop Relat Res 257:107–128
Massin P, Schmidt L, Engh CA (1989) Evaluation of cementless acetabular component migration. An experimental study. J Arthroplasty 4:245–251
Delee JG, Charnley J (1976) Radiological demarcation of cemented sockets in total hip replacement. Clin Orthop Relat Res 121:20–32
Gruen TA, Mcneice GM, Amstutz HC (1979) "Modes of failure" of cemented stem-type femoral components: a radiographic analysis of loosening. Clin Orthop Relat Res 141:17–27
Gallo J, Havranek V, Zapletalova J (2010) Risk factors for accelerated polyethylene wear and osteolysis in ABG I total hip arthroplasty. Int Orthop 34:19–26
Dorr LD, Wan Z (1995) Ten years of experience with porous acetabular components for revision surgery. Clin Orthop Relat Res 319:191–200
Rowden NJ, Harrison JA, Graves SE et al (2012) Loss to follow-up after arthroplasty: a new use for registry data. J Bone Joint Surg Br 94:493–496
Lachiewicz PF, Soileau ES (2012) Second-generation modular acetabular components provide fixation at 10 to 16 years. Clin Orthop Relat Res 470:366–372
Suckel A, Geiger F, Kinzl L et al (2009) Long-term results for the uncemented Zweymuller/Alloclassic hip endoprosthesis. A 15-year minimum follow-up of 320 hip operations. J Arthroplasty 24:846–853
Terre RA (2010) Estimated survival probability of the Spotorno total hip arthroplasty after a 15- to 21-year follow-up: one surgeon’s results. Hip Int 20(Suppl 7):70–78
Laupacis A, Bourne R, Rorabeck C et al (2002) Comparison of total hip arthroplasty performed with and without cement: a randomized trial. J Bone Joint Surg Am 84:1823–1828
Rorabeck CH, Bourne RB, Laupacis A et al (1994) A double-blind study of 250 cases comparing cemented with cementless total hip arthroplasty. Cost-effectiveness and its impact on health-related quality of life. Clin Orthop Relat Res 298:156–164
Corten K, Bourne RB, Charron KD et al (2011) What works best, a cemented or cementless primary total hip arthroplasty? Minimum 17-year followup of a randomized controlled trial. Clin Orthop Relat Res 469:209–217
Martín-Guinea J, Álvarez-Gonzáles P, Nieva-Navarro F (2004) Analysis of 10-year survival rates for 100 cementless Balgrist cups in primary hip prostheses. J Bone Joint Surg Br 86:141
Rozkydal Z, Janicek P, Tomas T et al (2009) Long-term results of the CLS acetabular cup in primary total hip replacement. Acta Chir Orthop Traumatol Cech 76:90–97
Dottl C, Steinhauser E, Koch U et al (2006) Fractures of cementless thin-walled cups. J Arthroplasty 21:144–147
Gallo J, Goodman SB, Konttinen YT et al (2013) Particle disease: Biologic mechanisms of periprosthetic osteolysis in total hip arthroplasty. Innate Immun 19:213–224
Gallo J, Goodman SB, Lostak J et al (2012) Advantages and disadvantages of ceramic on ceramic total hip arthroplasty: a review. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub 156:204–212
Shetty V, Shitole B, Shetty G et al (2011) Optimal bearing surfaces for total hip replacement in the young patient: a meta-analysis. Int Orthop 35:1281–1287
Battenberg AK, Hopkins JS, Kupiec AD et al (2013) The 2012 Frank Stinchfield Award: Decreasing patient activity with aging: implications for crosslinked polyethylene wear. Clin Orthop Relat Res 471:386–392
Kinkel S, Wollmerstedt N, Kleinhans JA et al (2009) Patient activity after total hip arthroplasty declines with advancing age. Clin Orthop Relat Res 467:2053–2058
Schmalzried TP, Shepherd EF, Dorey FJ et al (2000) The John Charnley Award. Wear is a function of use, not time. Clin Orthop Relat Res 381:36–46
Schmalzried TP, Szuszczewicz ES, Northfield MR et al (1998) Quantitative assessment of walking activity after total hip or knee replacement. J Bone Joint Surg Am 80:54–59
Romano CL, Frigo C, Randelli G et al (1996) Analysis of the gait of adults who had residua of congenital dysplasia of the hip. J Bone Joint Surg Am 78:1468–1479
Gould VC, Blom AW, Wylde V (2012) Long-term patient-reported outcomes after total hip replacement: comparison to the general population. Hip Int 22:160–165
Roder C, Staub LP, Eichler P et al (2006) Avoiding misclassification bias with the traditional Charnley classification: rationale for a fourth Charnley class BB. J Orthop Res 24:1803–1808
Sheffler LC, Yoo B, Bhandari M et al (2013) Observational studies in orthopaedic surgery: the STROBE statement as a tool for transparent reporting. J Bone Joint Surg Am 95:e112–141
Joshi AB, Gill GS, Smith PL (2003) Outcome in patients lost to follow-up. J Arthroplasty 18:149–153
Acknowledgments
The work on the study was supported by IGA Ministry of Health Czech Republic (IGA MZ CR NT/11049 and NT/14267). The authors thank Prof. Stuart B. Goodman from the Stanford Medical School for critical reading of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gallo, J., Lostak, J. & Langova, K. Long-term survival of the uncemented Balgrist total hip replacement cup. International Orthopaedics (SICOT) 37, 1449–1456 (2013). https://doi.org/10.1007/s00264-013-1946-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-013-1946-x