Abstract
Background
The clinical significance of adoptive tumor-infiltrating lymphocyte (TIL) therapy has been demonstrated in many clinical trials. We analyzed the in vitro reactivity of cultured TILs against autologous breast cancer cells.
Methods
TILs and cancer cells were cultured from 31 breast tumor tissues. Reactivity of TILs against cancer cells was determined by measuring secreted interferon-gamma. Expression levels of epithelial markers, major histocompatibility complex molecules, and programmed death-ligand 1 (PD-L1) in cancer cells, and T cell markers (memory, T cell activation and exhaustion, and regulatory T cell markers) in expanded TILs were analyzed and compared between the reactive and non-reactive groups.
Results
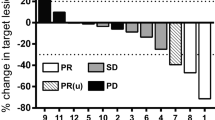
In seven cases, TILs showed reactivity to autologous cancer cells. Six of these cases were associated with triple-negative breast cancer (TNBC). All reactive TNBCs were derived from surgical specimens after neoadjuvant chemotherapy (NAC). Higher expression of Ki67 in tumor tissues and lower expression of PD-L1 in cultured cancer cells were associated with reactivity. Proliferation of reactive TILs was high. High proportions of T cells and PD-1+CD4+ and PD1+CD8+ T cells were associated with reactivity in TNBC cases, while other activation or exhaustion markers were not.
Conclusion
TILs from approximately half the TNBC cases with NAC showed reactivity against autologous cancer cells. The proportion of PD-1+ T cells was higher in the reactive group. Adoptive TIL therapy combined with PD-1 inhibitors might be promising for TNBC patients with residual tumors after NAC.





Similar content being viewed by others
Availability of data and materials
The datasets used and/or analyzed during the current study are available from the corresponding author on reasonable request.
Abbreviations
- ACT:
-
Adoptive cell transfer
- CK:
-
Cytokeratin
- EpCAM:
-
Epithelial cell adhesion molecule
- ER:
-
Estrogen receptor
- HER2+ :
-
Human epidermal growth factor receptor 2-positive
- HR:
-
Hormone receptor
- IFN-γ:
-
Interferon-gamma
- MDSCs:
-
Myeloid-derived suppressor cells
- MHC:
-
Major histocompatibility complex
- NAC:
-
Neoadjuvant chemotherapy
- NK:
-
Natural killer
- NKT:
-
Natural killer T
- PBMC:
-
Peripheral blood mononuclear cell
- PDX:
-
Patient-derived xenograft
- PR:
-
Progesterone receptor
- REP:
-
Rapid expansion
- TCR:
-
T cell receptor
- TIL:
-
Tumor-infiltrating lymphocyte
- TLS:
-
Tertiary lymphoid structure
- TNBC:
-
Triple-negative breast cancer
- Treg:
-
Regulatory T cell
References
Waks AG, Winer EP (2019) Breast cancer treatment: a review. JAMA 321(3):288–300
Bernhard H, Neudorfer J, Gebhard K, Conrad H, Hermann C, Nahrig J, Fend F, Weber W, Busch DH, Peschel C (2008) Adoptive transfer of autologous, HER2-specific, cytotoxic T lymphocytes for the treatment of HER2-overexpressing breast cancer. Cancer Immunol Immunother 57(2):271–280
Sparano JA, Fisher RI, Weiss GR, Margolin K, Aronson FR, Hawkins MJ, Atkins MB, Dutcher JP, Gaynor ER, Boldt DH et al (1994) Phase II trials of high-dose interleukin-2 and lymphokine-activated killer cells in advanced breast carcinoma and carcinoma of the lung, ovary, and pancreas and other tumors. J Immunother Emphas Tumor Immunol 16(3):216–223
Tchou J, Zhao Y, Levine BL, Zhang PJ, Davis MM, Melenhorst JJ, Kulikovskaya I, Brennan AL, Liu X, Lacey SF et al (2017) Safety and efficacy of intratumoral injections of chimeric antigen receptor (CAR) T cells in metastatic breast cancer. Cancer Immunol Res 5(12):1152–1161
Martinez M, Moon EK (2019) CAR T cells for solid tumors: new strategies for finding, infiltrating, and surviving in the tumor microenvironment. Front Immunol 10:128
Zacharakis N, Chinnasamy H, Black M, Xu H, Lu YC, Zheng Z, Pasetto A, Langhan M, Shelton T, Prickett T et al (2018) Immune recognition of somatic mutations leading to complete durable regression in metastatic breast cancer. Nat Med 24(6):724–730
Egelston CA, Avalos C, Tu TY, Simons DL, Jimenez G, Jung JY, Melstrom L, Margolin K, Yim JH, Kruper L et al (2018) Human breast tumor-infiltrating CD8(+) T cells retain polyfunctionality despite PD-1 expression. Nat Commun 9(1):4297
Stanton SE, Adams S, Disis ML (2016) Variation in the incidence and magnitude of tumor-infiltrating lymphocytes in breast cancer subtypes: a systematic review. JAMA Oncol 2(10):1354–1360
Rosenberg SA, Yang JC, Sherry RM, Kammula US, Hughes MS, Phan GQ, Citrin DE, Restifo NP, Robbins PF, Wunderlich JR et al (2011) Durable complete responses in heavily pretreated patients with metastatic melanoma using T-cell transfer immunotherapy. Clin Cancer Res 17(13):4550–4557
Creelan B, Teer J, Toloza E, Mullinax J, Landin A, Gray J, Tanvetyanon T, Taddeo M, Noyes D, Kelley L et al (2018) OA05.03 safety and clinical activity of adoptive cell transfer using tumor infiltrating lymphocytes (TIL) combined with nivolumab in NSCLC. J Thorac Oncol 13(10):S330–S331
Jazaeri AA, Zsiros E, Amaria RN, Artz AS, Edwards RP, Wenham RM, Slomovitz BM, Walther A, Thomas SS, Chesney JA et al (2019) Safety and efficacy of adoptive cell transfer using autologous tumor infiltrating lymphocytes (LN-145) for treatment of recurrent, metastatic, or persistent cervical carcinoma. J Clin Oncol 37(15_suppl):2538–2538
Fujita K, Ikarashi H, Takakuwa K, Kodama S, Tokunaga A, Takahashi T, Tanaka K (1995) Prolonged disease-free period in patients with advanced epithelial ovarian cancer after adoptive transfer of tumor-infiltrating lymphocytes. Clin Cancer Res 1(5):501–507
Tran E, Robbins PF, Lu YC, Prickett TD, Gartner JJ, Jia L, Pasetto A, Zheng Z, Ray S, Groh EM et al (2016) T-cell transfer therapy targeting mutant KRAS in cancer. N Engl J Med 375(23):2255–2262
Lee HJ, Kim YA, Sim CK, Heo SH, Song IH, Park HS, Park SY, Bang WS, Park IA, Lee M et al (2017) Expansion of tumor-infiltrating lymphocytes and their potential for application as adoptive cell transfer therapy in human breast cancer. Oncotarget 8(69):113345–113359
June CH, O'Connor RS, Kawalekar OU, Ghassemi S, Milone MC (2018) CAR T cell immunotherapy for human cancer. Science 359(6382):1361–1365
Salgado R, Denkert C, Demaria S, Sirtaine N, Klauschen F, Pruneri G, Wienert S, Van den Eynden G, Baehner FL, Penault-Llorca F et al (2015) The evaluation of tumor-infiltrating lymphocytes (TILs) in breast cancer: recommendations by an International TILs Working Group 2014. Ann Oncol 26(2):259–271
Lee HJ, Park IA, Song IH, Shin SJ, Kim JY, Yu JH, Gong G (2016) Tertiary lymphoid structures: prognostic significance and relationship with tumour-infiltrating lymphocytes in triple-negative breast cancer. J Clin Pathol 69(5):422–430
Van Acker HH, Capsomidis A, Smits EL, Van Tendeloo VF (2017) CD56 in the immune system: More than a marker for cytotoxicity? Front Immunol 8:892
Ohtani H (2007) Focus on TILs: prognostic significance of tumor infiltrating lymphocytes in human colorectal cancer. Cancer Immun 7(1):4
Liakou CI, Narayanan S, Ng Tang D, Logothetis CJ, Sharma P (2007) Focus on TILs: prognostic significance of tumor infiltrating lymphocytes in human bladder cancer. Cancer Immun 7(1):10
Dunn GP, Dunn IF, Curry WT (2007) Focus on TILs: prognostic significance of tumor infiltrating lymphocytes in human glioma. Cancer Immun 7(1):12
Uppaluri R, Dunn GP, Lewis JS (2008) Focus on TILs: prognostic significance of tumor infiltrating lymphocytes in head and neck cancers. Cancer Immun 8(1):16
Oble DA, Loewe R, Yu P, Mihm MC (2009) Focus on TILs: prognostic significance of tumor infiltrating lymphocytes in human melanoma. Cancer Immun 9(1):3
Denkert C, von Minckwitz G, Darb-Esfahani S, Lederer B, Heppner BI, Weber KE, Budczies J, Huober J, Klauschen F, Furlanetto J et al (2018) Tumour-infiltrating lymphocytes and prognosis in different subtypes of breast cancer: a pooled analysis of 3771 patients treated with neoadjuvant therapy. Lancet Oncol 19(1):40–50
Shang B, Liu Y, Jiang S-J, Liu Y (2015) Prognostic value of tumor-infiltrating FoxP3+ regulatory T cells in cancers: a systematic review and meta-analysis. Sci Rep 5:15179
Shen T, Zhou L, Shen H, Shi C, Jia S, Ding GP, Cao L (2017) Prognostic value of programmed cell death protein 1 expression on CD8+ T lymphocytes in pancreatic cancer. Sci Rep 7(1):7848
Zhou C, Tang J, Sun H, Zheng X, Li Z, Sun T, Li J, Wang S, Zhou X, Sun H et al (2017) PD-L1 expression as poor prognostic factor in patients with non-squamous non-small cell lung cancer. Oncotarget 8(35):58457–58468
Jung HI, Jeong D, Ji S, Ahn TS, Bae SH, Chin S, Chung JC, Kim HC, Lee MS, Baek MJ (2017) Overexpression of PD-L1 and PD-L2 is associated with poor prognosis in patients with hepatocellular carcinoma. Cancer Res Treat 49(1):246–254
Koganemaru S, Inoshita N, Miura Y, Miyama Y, Fukui Y, Ozaki Y, Tomizawa K, Hanaoka Y, Toda S, Suyama K et al (2017) Prognostic value of programmed death-ligand 1 expression in patients with stage III colorectal cancer. Cancer Sci 108(5):853–858
Nair S, Dhodapkar MV (2017) Natural killer T cells in cancer immunotherapy. Front Immunol 8:1178
Shi B, Li Q, Ma X, Gao Q, Li L, Chu J (2018) High expression of programmed cell death protein 1 on peripheral blood T-cell subsets is associated with poor prognosis in metastatic gastric cancer. Oncol Lett 16(4):4448–4454
Badoual C, Hans S, Merillon N, Van Ryswick C, Ravel P, Benhamouda N, Levionnois E, Nizard M, Si-Mohamed A, Besnier N et al (2013) PD-1-expressing tumor-infiltrating T cells are a favorable prognostic biomarker in HPV-associated head and neck cancer. Cancer Res 73(1):128–138
Carreras J, Lopez-Guillermo A, Roncador G, Villamor N, Colomo L, Martinez A, Hamoudi R, Howat WJ, Montserrat E, Campo E (2009) High numbers of tumor-infiltrating programmed cell death 1-positive regulatory lymphocytes are associated with improved overall survival in follicular lymphoma. J Clin Oncol 27(9):1470–1476
Li Y, Liang L, Dai W, Cai G, Xu Y, Li X, Li Q, Cai S (2016) Prognostic impact of programed cell death-1 (PD-1) and PD-ligand 1 (PD-L1) expression in cancer cells and tumor infiltrating lymphocytes in colorectal cancer. Mol Cancer 15(1):55
Brockhoff G, Seitz S, Weber F, Zeman F, Klinkhammer-Schalke M, Ortmann O, Wege AK (2018) The presence of PD-1 positive tumor infiltrating lymphocytes in triple negative breast cancers is associated with a favorable outcome of disease. Oncotarget 9(5):6201–6212
Simon S, Labarriere N (2017) PD-1 expression on tumor-specific T cells: Friend or foe for immunotherapy? Oncoimmunology 7(1):e1364828
Josefowicz SZ, Lu LF, Rudensky AY (2012) Regulatory T cells: mechanisms of differentiation and function. Annu Rev Immunol 30:531–564
Niakan A, Faghih Z, Talei AR, Ghaderi A (2019) Cytokine profile of CD4(+)CD25(-)FoxP3(+) T cells in tumor-draining lymph nodes from patients with breast cancer. Mol Immunol 116:90–97
Ferreira RC, Simons HZ, Thompson WS, Rainbow DB, Yang X, Cutler AJ, Oliveira J, Castro Dopico X, Smyth DJ, Savinykh N et al (2017) Cells with Treg-specific FOXP3 demethylation but low CD25 are prevalent in autoimmunity. J Autoimmun 84:75–86
Schuster M, Plaza-Sirvent C, Visekruna A, Huehn J, Schmitz I (2019) Generation of Foxp3(+)CD25(-) regulatory T-cell precursors requires c-Rel and IkappaBNS. Front Immunol 10:1583
Thornton AM, Lu J, Korty PE, Kim YC, Martens C, Sun PD, Shevach EM (2019) Helios(+) and Helios(-) treg subpopulations are phenotypically and functionally distinct and express dissimilar TCR repertoires. Eur J Immunol 49(3):398–412
Han S, Toker A, Liu ZQ, Ohashi PS (2019) Turning the tide against regulatory T cells. Front Oncol 9:279
Barroso-Sousa R, Jain E, Cohen O, Kim D, Buendia-Buendia J, Winer E, Lin N, Tolaney SM, Wagle N (2020) Prevalence and mutational determinants of high tumor mutation burden in breast cancer. Ann Oncol 31(3):387–394
Lee HJ, Song IH, Park IA, Heo SH, Kim YA, Ahn JH, Gong G (2016) Differential expression of major histocompatibility complex class I in subtypes of breast cancer is associated with estrogen receptor and interferon signaling. Oncotarget 7(21):30119–30132
Funding
This study was supported by the Korean Health Technology R&D Project, Ministry of Health & Welfare (HI15C0708 and HI17C0337) and the Asan Institute for Life Sciences, Asan Medical Center, Seoul, Korea (2018IL0169, 2019IL0169, and 2019IL0839).
Author information
Authors and Affiliations
Contributions
HjL interpreted the data associated with tumor-infiltrating lymphocyte reactivity in breast cancer and was a major contributor in writing the manuscript. YAK and HSP participated in sample preparation and analysis. YK and JHS analyzed the TCR repertoire of the TILs. HL, GG, and HJL contributed as pathologists and revised the manuscript. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Ethics approval and consents to participate
Tumor tissues were obtained from patients along with their consent to the use of the specimen for research purposes. This study was approved by the Institutional Review Board of Asan Medical Center (IRB#2015-0438).
Consent for publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Lee, H., Kim, YA., Kim, Y. et al. Clinicopathological factors associated with tumor-infiltrating lymphocyte reactivity in breast cancer. Cancer Immunol Immunother 69, 2381–2391 (2020). https://doi.org/10.1007/s00262-020-02633-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-020-02633-5