Abstract
Total neoadjuvant treatment (TNT) for rectal cancer is becoming an accepted treatment paradigm and is changing the landscape of this disease, wherein up to 50% of patients who undergo TNT are able to avoid surgery. This places new demands on the radiologist in terms of interpreting degrees of response to treatment. This primer summarizes the Watch-and-Wait approach and the role of imaging, with illustrative “atlas-like” examples as an educational guide for radiologists. We present a brief literature summary of the evolution of rectal cancer treatment, with a focus on magnetic resonance imaging (MRI) assessment of response. We also discuss recommended guidelines and standards. We outline the common TNT approach entering mainstream practice. A heuristic and algorithmic approach to MRI interpretation is also offered. To illustrate management and common scenarios, we arranged the illustrative figures as follows: (I) Clinical complete response (cCR) achieved at the immediate post-TNT “decision point” scan time; (II) cCR achieved at some point during surveillance, later than the first post-TNT MRI; (III) near clinical complete response (nCR); (IV) incomplete clinical response (iCR); (V) discordant findings between MRI and endoscopy where MRI is falsely positive, even at follow-up; (VI) discordant cases where MRI seems to be falsely positive but is proven truly positive on follow-up endoscopy; (VII) cases where MRI is falsely negative; (VIII) regrowth of tumor in the primary tumor bed; (IX) regrowth outside the primary tumor bed; and (X) challenging scenarios, i.e., mucinous cases. This primer is offered to achieve its intended goal of educating radiologists on how to interpret MRI in patients with rectal cancer undergoing treatment using a TNT-type treatment paradigm and a Watch-and-Wait approach.
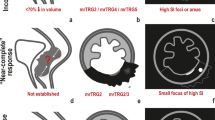
Graphical abstract
































Similar content being viewed by others
References
de Neree Tot Babberich MPM, van Groningen JT, Dekker E, Wiggers T, Wouters MWJM, Bemelman WA, et al. Laparoscopic conversion in colorectal cancer surgery; is there any improvement over time at a population level? Surg Endosc. 2018;32(7):3234–46. https://doi.org/10.1007/s00464-018-6042-2.
Paun BC, Cassie S, MacLean AR, Dixon E, Buie WD. Postoperative complications following surgery for rectal cancer. Ann Surg. 2010;251(5):807-18. https://doi.org/10.1097/SLA.0b013e3181dae4ed.
Habr-Gama A, Perez RO, Nadalin W, Sabbaga J, Ribeiro U, Jr., Silva e Sousa AH, Jr., et al. Operative versus nonoperative treatment for stage 0 distal rectal cancer following chemoradiation therapy: long-term results. Ann Surg. 2004;240(4):711–7; discussion 7–8.
Maas M, Nelemans PJ, Valentini V, Das P, Rodel C, Kuo LJ, et al. Long-term outcome in patients with a pathological complete response after chemoradiation for rectal cancer: a pooled analysis of individual patient data. Lancet Oncol. 2010;11(9):835-44. https://doi.org/10.1016/S1470-2045(10)70172-8.
Al-Sukhni E, Attwood K, Mattson DM, Gabriel E, Nurkin SJ. Predictors of Pathologic Complete Response Following Neoadjuvant Chemoradiotherapy for Rectal Cancer. Ann Surg Oncol. 2016;23(4):1177-86. https://doi.org/10.1245/s10434-015-5017-y.
Bahadoer RR, Dijkstra EA, van Etten B, Marijnen CAM, Putter H, Kranenbarg EM, et al. Short-course radiotherapy followed by chemotherapy before total mesorectal excision (TME) versus preoperative chemoradiotherapy, TME, and optional adjuvant chemotherapy in locally advanced rectal cancer (RAPIDO): a randomised, open-label, phase 3 trial. Lancet Oncol. 2021;22(1):29-42. https://doi.org/10.1016/S1470-2045(20)30555-6.
Conroy T, Bosset JF, Etienne PL, Rio E, François É, Mesgouez-Nebout N, et al. Neoadjuvant chemotherapy with FOLFIRINOX and preoperative chemoradiotherapy for patients with locally advanced rectal cancer (UNICANCER-PRODIGE 23): a multicentre, randomised, open-label, phase 3 trial. Lancet Oncol. 2021;22(5):702-15. https://doi.org/10.1016/S1470-2045(21)00079-6.
Cercek A, Roxburgh CSD, Strombom P, Smith JJ, Temple LKF, Nash GM, et al. Adoption of Total Neoadjuvant Therapy for Locally Advanced Rectal Cancer. JAMA Oncol. 2018;4(6):e180071. https://doi.org/10.1001/jamaoncol.2018.0071.
Garcia-Aguilar J, Patil S, Kim JK, Yuval JB, Thompson H, Verheij F, et al. Preliminary results of the organ preservation of rectal adenocarcinoma (OPRA) trial. Journal of Clinical Oncology. 2020;38(15_suppl):4008-. https://doi.org/10.1200/JCO.2020.38.15_suppl.4008.
Chen TY, Wiltink LM, Nout RA, Meershoek-Klein Kranenbarg E, Laurberg S, Marijnen CA, et al. Bowel function 14 years after preoperative short-course radiotherapy and total mesorectal excision for rectal cancer: report of a multicenter randomized trial. Clin Colorectal Cancer. 2015;14(2):106-14. https://doi.org/10.1016/j.clcc.2014.12.007.
Schurink NW, Lambregts DMJ, Beets-Tan RGH. Diffusion-weighted imaging in rectal cancer: current applications and future perspectives. Br J Radiol. 2019;92(1096):20180655. https://doi.org/10.1259/bjr.20180655.
van der Paardt MP, Zagers MB, Beets-Tan RG, Stoker J, Bipat S. Patients who undergo preoperative chemoradiotherapy for locally advanced rectal cancer restaged by using diagnostic MR imaging: a systematic review and meta-analysis. Radiology. 2013;269(1):101-12. https://doi.org/10.1148/radiol.13122833.
Lambregts DMJ, Delli Pizzi A, Lahaye MJ, van Griethuysen JJM, Maas M, Beets GL, et al. A Pattern-Based Approach Combining Tumor Morphology on MRI With Distinct Signal Patterns on Diffusion-Weighted Imaging to Assess Response of Rectal Tumors After Chemoradiotherapy. Dis Colon Rectum. 2018;61(3):328-37. https://doi.org/10.1097/DCR.0000000000000915.
Mandard AM, Dalibard F, Mandard JC, Marnay J, Henry-Amar M, Petiot JF, et al. Pathologic assessment of tumor regression after preoperative chemoradiotherapy of esophageal carcinoma. Clinicopathologic correlations. Cancer. 1994;73(11):2680-6.
Sclafani F, Brown G, Cunningham D, Wotherspoon A, Mendes LST, Balyasnikova S, et al. Comparison between MRI and pathology in the assessment of tumour regression grade in rectal cancer. Br J Cancer. 2017;117(10):1478-85. https://doi.org/10.1038/bjc.2017.320.
Patel UB, Brown G, Rutten H, West N, Sebag-Montefiore D, Glynne-Jones R, et al. Comparison of magnetic resonance imaging and histopathological response to chemoradiotherapy in locally advanced rectal cancer. Ann Surg Oncol. 2012;19(9):2842-52. https://doi.org/10.1245/s10434-012-2309-3.
van den Broek JJ, van der Wolf FS, Lahaye MJ, Heijnen LA, Meischl C, Heitbrink MA, et al. Accuracy of MRI in Restaging Locally Advanced Rectal Cancer After Preoperative Chemoradiation. Dis Colon Rectum. 2017;60(3):274-83. https://doi.org/10.1097/DCR.0000000000000743.
Nahas SC, Rizkallah Nahas CS, Sparapan Marques CF, Ribeiro U, Jr., Cotti GC, Imperiale AR, et al. Pathologic Complete Response in Rectal Cancer: Can We Detect It? Lessons Learned From a Proposed Randomized Trial of Watch-and-Wait Treatment of Rectal Cancer. Dis Colon Rectum. 2016;59(4):255-63. https://doi.org/10.1097/DCR.0000000000000558.
W.A. Hall JL, Y.N. You, M.J. Gollub, J.R. Grajo, M. Rosen, G. dePrisco, G. Yothers, J. Dorth, H.M. Gross, R.A. Peterson, B. Faller, K. Moxley, S. Jacobs, P. Stella, M.G. Haddock, T.S. Hong, T.J. George,. Prospective Validation of the Magnetic Resonance Tumor Regression Grade (MR-TRG) and Correlation With Pathologic Endpoints Score in NRG Oncology GI002. International Journal of Radiation Oncology*Biology*Physics,. 2021;111(3):S37.
Lambregts DMJ, van Heeswijk MM, Delli Pizzi A, van Elderen SGC, Andrade L, Peters N, et al. Diffusion-weighted MRI to assess response to chemoradiotherapy in rectal cancer: main interpretation pitfalls and their use for teaching. Eur Radiol. 2017;27(10):4445-54. https://doi.org/10.1007/s00330-017-4830-z.
Fernandes MC, Gollub MJ, Brown G. The importance of MRI for rectal cancer evaluation. Surg Oncol. 2022:101739. https://doi.org/10.1016/j.suronc.2022.101739.
Jayaprakasam VS, Javed-Tayyab S, Gangai N, Zheng J, Capanu M, Bates DDB, et al. Does microenema administration improve the quality of DWI sequences in rectal MRI? Abdom Radiol (NY). 2021;46(3):858-66. https://doi.org/10.1007/s00261-020-02718-w.
Horvat N, Hope TA, Pickhardt PJ, Petkovska I. Mucinous rectal cancer: concepts and imaging challenges. Abdom Radiol (NY). 2019. https://doi.org/10.1007/s00261-019-02019-x.
Haak HE, Žmuc J, Lambregts DMJ, Beets-Tan RGH, Melenhorst J, Beets GL, et al. The evaluation of follow-up strategies of watch-and-wait patients with a complete response after neoadjuvant therapy in rectal cancer. Colorectal Dis. 2021;23(7):1785-92. https://doi.org/10.1111/codi.15636.
Gollub MJ, Das JP, Bates DDB, Fuqua JL, Golia Pernicka JS, Javed-Tayyab S, et al. Rectal cancer with complete endoscopic response after neoadjuvant therapy: what is the meaning of a positive MRI? Eur Radiol. 2021;31(7):4731-8. https://doi.org/10.1007/s00330-020-07657-0.
Yoon JH, Lee JM, Chang W, Kang HJ, Bandos A, Lim HJ, et al. Initial M Staging of Rectal Cancer: FDG PET/MRI with a Hepatocyte-specific Contrast Agent versus Contrast-enhanced CT. Radiology. 2020;294(2):310-9. https://doi.org/10.1148/radiol.2019190794.
Hope TA, Kassam Z, Loening A, McNamara MM, Paspulati R. The use of PET/MRI for imaging rectal cancer. Abdom Radiol (NY). 2019;44(11):3559-68. https://doi.org/10.1007/s00261-019-02089-x.
Crimi F, Valeggia S, Baffoni L, Stramare R, Lacognata C, Spolverato G, et al. [18F]FDG PET/MRI in rectal cancer. Ann Nucl Med. 2021;35(3):281-90. https://doi.org/10.1007/s12149-021-01580-0.
Crimi F, Spolverato G, Lacognata C, Garieri M, Cecchin D, Urso ED, et al. 18F-FDG PET/MRI for Rectal Cancer TNM Restaging After Preoperative Chemoradiotherapy: Initial Experience. Dis Colon Rectum. 2020;63(3):310-8. https://doi.org/10.1097/DCR.0000000000001568.
Capelli G, Campi C, Bao QR, Morra F, Lacognata C, Zucchetta P, et al. 18F-FDG-PET/MRI texture analysis in rectal cancer after neoadjuvant chemoradiotherapy. Nucl Med Commun. 2022;43(7):815-22. https://doi.org/10.1097/MNM.0000000000001570.
Napoletano M, Mazzucca D, Prosperi E, Aisa MC, Lupattelli M, Aristei C, et al. Locally advanced rectal cancer: qualitative and quantitative evaluation of diffusion-weighted magnetic resonance imaging in restaging after neoadjuvant chemo-radiotherapy. Abdom Radiol (NY). 2019;44(11):3664-73. https://doi.org/10.1007/s00261-019-02012-4.
Yang L, Qiu M, Xia C, Li Z, Wang Z, Zhou X, et al. Value of High-Resolution DWI in Combination With Texture Analysis for the Evaluation of Tumor Response After Preoperative Chemoradiotherapy for Locally Advanced Rectal Cancer. AJR Am J Roentgenol. 2019:1–8. https://doi.org/10.2214/AJR.18.20689.
Horvat N, Veeraraghavan H, Khan M, Blazic I, Zheng J, Capanu M, et al. MR Imaging of Rectal Cancer: Radiomics Analysis to Assess Treatment Response after Neoadjuvant Therapy. Radiology. 2018;287(3):833-43. https://doi.org/10.1148/radiol.2018172300.
Jayaprakasam VS, Paroder V, Gibbs P, Bajwa R, Gangai N, Sosa RE, et al. MRI radiomics features of mesorectal fat can predict response to neoadjuvant chemoradiation therapy and tumor recurrence in patients with locally advanced rectal cancer. Eur Radiol. 2022;32(2):971-80. https://doi.org/10.1007/s00330-021-08144-w.
Palta M, Willett CG, Czito BG. Short-course versus long-course chemoradiation in rectal cancer--time to change strategies? Curr Treat Options Oncol. 2014;15(3):421-8. https://doi.org/10.1007/s11864-014-0296-2.
Sauer R, Becker H, Hohenberger W, Rödel C, Wittekind C, Fietkau R, et al. Preoperative versus postoperative chemoradiotherapy for rectal cancer. N Engl J Med. 2004;351(17):1731-40. https://doi.org/10.1056/NEJMoa040694.
Cedermark B, Dahlberg M, Glimelius B, Påhlman L, Rutqvist LE, Wilking N, et al. Improved survival with preoperative radiotherapy in resectable rectal cancer. N Engl J Med. 1997;336(14):980-7. https://doi.org/10.1056/NEJM199704033361402.
Garcia-Aguilar J, Chow OS, Smith DD, Marcet JE, Cataldo PA, Varma MG, et al. Effect of adding mFOLFOX6 after neoadjuvant chemoradiation in locally advanced rectal cancer: a multicentre, phase 2 trial. Lancet Oncol. 2015;16(8):957-66. https://doi.org/10.1016/S1470-2045(15)00004-2.
Probst CP, Becerra AZ, Aquina CT, Tejani MA, Wexner SD, Garcia-Aguilar J, et al. Extended Intervals after Neoadjuvant Therapy in Locally Advanced Rectal Cancer: The Key to Improved Tumor Response and Potential Organ Preservation. J Am Coll Surg. 2015;221(2):430-40. https://doi.org/10.1016/j.jamcollsurg.2015.04.010.
Yuval JB, Garcia-Aguilar J. Watch-and-wait Management for Rectal Cancer After Clinical Complete Response to Neoadjuvant Therapy. Adv Surg. 2021;55:89-107. https://doi.org/10.1016/j.yasu.2021.05.007.
Santiago I, Rodrigues B, Barata M, Figueiredo N, Fernandez L, Galzerano A, et al. Re-staging and follow-up of rectal cancer patients with MR imaging when "Watch-and-Wait" is an option: a practical guide. Insights Imaging. 2021;12(1):114. https://doi.org/10.1186/s13244-021-01055-w.
Goffredo P, Khan A, Mott SL, Jensen CC, Madoff RD, Gaertner WB, et al. Total Neoadjuvant Therapy Versus Standard Neoadjuvant Chemoradiation in Patients with Locally Advanced Rectal Cancer: A Comparison of Short- and Long-term Oncologic Outcomes. Ann Surg. 2022;276(6):e819-e24. https://doi.org/10.1097/SLA.0000000000005141.
Benson AB, Venook AP, Al-Hawary MM, Azad N, Chen YJ, Ciombor KK, et al. Rectal Cancer, Version 2.2022, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Canc Netw. 2022;20(10):1139–67. https://doi.org/10.6004/jnccn.2022.0051.
Maas M, Lambregts DM, Nelemans PJ, Heijnen LA, Martens MH, Leijtens JW, et al. Assessment of Clinical Complete Response After Chemoradiation for Rectal Cancer with Digital Rectal Examination, Endoscopy, and MRI: Selection for Organ-Saving Treatment. Ann Surg Oncol. 2015;22(12):3873-80. https://doi.org/10.1245/s10434-015-4687-9.
Macchia G, Gambacorta MA, Masciocchi C, Chiloiro G, Mantello G, di Benedetto M, et al. Time to surgery and pathologic complete response after neoadjuvant chemoradiation in rectal cancer: A population study on 2094 patients. Clin Transl Radiat Oncol. 2017;4:8-14. https://doi.org/10.1016/j.ctro.2017.04.004.
Goodman KA. Timing Is Everything: What Is the Optimal Duration After Chemoradiation for Surgery for Rectal Cancer? J Clin Oncol. 2016;34(31):3724-8. https://doi.org/10.1200/JCO.2016.68.3698.
Horvat N, El Homsi M, Miranda J, Mazaheri Y, Gollub MJ, Paroder V. Rectal MRI Interpretation After Neoadjuvant Therapy. J Magn Reson Imaging. 2022. https://doi.org/10.1002/jmri.28426.
Fokas E, Appelt A, Glynne-Jones R, Beets G, Perez R, Garcia-Aguilar J, et al. International consensus recommendations on key outcome measures for organ preservation after (chemo)radiotherapy in patients with rectal cancer. Nat Rev Clin Oncol. 2021;18(12):805-16. https://doi.org/10.1038/s41571-021-00538-5.
Ho VP, Lee Y, Stein SL, Temple LK. Sexual function after treatment for rectal cancer: a review. Dis Colon Rectum. 2011;54(1):113-25. https://doi.org/10.1007/DCR.0b013e3181fb7b82.
Toz E, Kurt S, Sahin C, Canda MT. Frequency of recurrent urinary tract infection in patients with pelvic organ prolapse. Res Rep Urol. 2015;7:9-12. https://doi.org/10.2147/RRU.S77061.
Garcia-Aguilar J, Patil S, Gollub MJ, Kim JK, Yuval JB, Thompson HM, et al. Organ Preservation in Patients With Rectal Adenocarcinoma Treated With Total Neoadjuvant Therapy. J Clin Oncol. 2022:JCO2200032. https://doi.org/10.1200/JCO.22.00032.
Brown G, Richards CJ, Newcombe RG, Dallimore NS, Radcliffe AG, Carey DP, et al. Rectal carcinoma: thin-section MR imaging for staging in 28 patients. Radiology. 1999;211(1):215-22. https://doi.org/10.1148/radiology.211.1.r99ap35215.
Group MS. Diagnostic accuracy of preoperative magnetic resonance imaging in predicting curative resection of rectal cancer: prospective observational study. BMJ. 2006;333(7572):779. https://doi.org/10.1136/bmj.38937.646400.55.
Beets-Tan RGH, Lambregts DMJ, Maas M, Bipat S, Barbaro B, Curvo-Semedo L, et al. Magnetic resonance imaging for clinical management of rectal cancer: Updated recommendations from the 2016 European Society of Gastrointestinal and Abdominal Radiology (ESGAR) consensus meeting. Eur Radiol. 2017. https://doi.org/10.1007/s00330-017-5026-2.
Panel SoARSCaACD-F. https://abdominalradiology.org/wp-content/uploads/2021/03/MR-Protocols.pdf.
Custers PA, Geubels BM, Beets GL, Lambregts DMJ, van Leerdam ME, van Triest B, et al. Defining near-complete response following (chemo)radiotherapy for rectal cancer: systematic review. Br J Surg. 2022;110(1):43-9. https://doi.org/10.1093/bjs/znac372.
Smith JJ, Chow OS, Gollub MJ, Nash GM, Temple LK, Weiser MR, et al. Organ Preservation in Rectal Adenocarcinoma: a phase II randomized controlled trial evaluating 3-year disease-free survival in patients with locally advanced rectal cancer treated with chemoradiation plus induction or consolidation chemotherapy, and total mesorectal excision or nonoperative management. BMC Cancer. 2015;15:767. https://doi.org/10.1186/s12885-015-1632-z.
Thompson H, Kim JK, Yuval JB, Verheij F, Patil S, Gollub MJ, et al. Survival and organ preservation according to clinical response after total neoadjuvant therapy in locally advanced rectal cancer patients: A secondary analysis from the organ preservation in rectal adenocarcinoma (OPRA) trial. Journal of Clinical Oncology. 2021;39(15_suppl):3509-. https://doi.org/10.1200/JCO.2021.39.15_suppl.3509.
Hupkens BJP, Maas M, Martens MH, van der Sande ME, Lambregts DMJ, Breukink SO, et al. Organ Preservation in Rectal Cancer After Chemoradiation: Should We Extend the Observation Period in Patients with a Clinical Near-Complete Response? Ann Surg Oncol. 2018;25(1):197-203. https://doi.org/10.1245/s10434-017-6213-8.
Conroy T, Bosset JF, Etienne PL, Rio E, Francois E, Mesgouez-Nebout N, et al. Neoadjuvant chemotherapy with FOLFIRINOX and preoperative chemoradiotherapy for patients with locally advanced rectal cancer (UNICANCER-PRODIGE 23): a multicentre, randomised, open-label, phase 3 trial. Lancet Oncol. 2021;22(5):702-15. https://doi.org/10.1016/S1470-2045(21)00079-6.
Diefenhardt M, Schlenska-Lange A, Kuhnt T, Kirste S, Piso P, Bechstein WO, et al. Total Neoadjuvant Therapy for Rectal Cancer in the CAO/ARO/AIO-12 Randomized Phase 2 Trial: Early Surrogate Endpoints Revisited. Cancers (Basel). 2022;14(15). https://doi.org/10.3390/cancers14153658.
van der Valk MJM, Hilling DE, Bastiaannet E, Meershoek-Klein Kranenbarg E, Beets GL, Figueiredo NL, et al. Long-term outcomes of clinical complete responders after neoadjuvant treatment for rectal cancer in the International Watch & Wait Database (IWWD): an international multicentre registry study. Lancet. 2018;391(10139):2537-45. https://doi.org/10.1016/S0140-6736(18)31078-X.
Smith JJ, Strombom P, Chow OS, Roxburgh CS, Lynn P, Eaton A, et al. Assessment of a Watch-and-Wait Strategy for Rectal Cancer in Patients With a Complete Response After Neoadjuvant Therapy. JAMA Oncol. 2019;5(4):e185896. https://doi.org/10.1001/jamaoncol.2018.5896.
Renehan AG, Malcomson L, Emsley R, Gollins S, Maw A, Myint AS, et al. Watch-and-wait approach versus surgical resection after chemoradiotherapy for patients with rectal cancer (the OnCoRe project): a propensity-score matched cohort analysis. Lancet Oncol. 2016;17(2):174-83. https://doi.org/10.1016/S1470-2045(15)00467-2.
Dossa F, Chesney TR, Acuna SA, Baxter NN. A watch-and-wait approach for locally advanced rectal cancer after a clinical complete response following neoadjuvant chemoradiation: a systematic review and meta-analysis. Lancet Gastroenterol Hepatol. 2017;2(7):501-13. https://doi.org/10.1016/S2468-1253(17)30074-2.
Martens MH, Maas M, Heijnen LA, Lambregts DM, Leijtens JW, Stassen LP, et al. Long-term Outcome of an Organ Preservation Program After Neoadjuvant Treatment for Rectal Cancer. J Natl Cancer Inst. 2016;108(12). https://doi.org/10.1093/jnci/djw171.
Habr-Gama A, Perez RO, Proscurshim I, Nunes Dos Santos RM, Kiss D, Gama-Rodrigues J, et al. Interval between surgery and neoadjuvant chemoradiation therapy for distal rectal cancer: does delayed surgery have an impact on outcome? Int J Radiat Oncol Biol Phys. 2008;71(4):1181–8. https://doi.org/10.1016/j.ijrobp.2007.11.035.
Garcia-Aguilar J, Patil S, Gollub MJ, Kim JK, Yuval JB, Thompson HM, et al. Organ Preservation in Patients With Rectal Adenocarcinoma Treated With Total Neoadjuvant Therapy. J Clin Oncol. 2022;40(23):2546-56. https://doi.org/10.1200/JCO.22.00032.
Cercek A, Lumish M, Sinopoli J, Weiss J, Shia J, Lamendola-Essel M, et al. PD-1 Blockade in Mismatch Repair-Deficient, Locally Advanced Rectal Cancer. N Engl J Med. 2022;386(25):2363-76. https://doi.org/10.1056/NEJMoa2201445.
Acknowledgements
The authors thank Joanne Chin, MFA, ELS, for her help in editing this manuscript.
Funding
This research was funded in part through the NIH/NCI Cancer Center Support Grant (P30 CA008748).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
JRC: Travel expense money from Galera therapeutics to attend an investigator seminar where he presented and had complete control over the intellectual content of his talk. APW: No disclosures related to this manuscript. Unrelated disclosures: Royalty, Elsevier Inc.; Royalty, Intellectual property (IP), licensed by the University of Michigan to Applied Morphomics, Inc; and Research support, Sequana Medical, NV, through the University of Michigan. All other authors have nothing to disclose.
Ethical approval
For this paper, no ethical approval is required.
Informed consent
For this paper, formal consent is not required.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Gollub, M.J., Costello, J.R., Ernst, R.D. et al. A primer on rectal MRI in patients on watch-and-wait treatment for rectal cancer. Abdom Radiol 48, 2836–2873 (2023). https://doi.org/10.1007/s00261-023-03900-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-023-03900-6