Abstract
Purpose
To compare bowel wall T1 relaxation estimates in young patients with newly diagnosed ileal CD to healthy control participants, characterize their change over time in response to biologic medical therapy, and evaluate their associations with clinical markers of intestinal inflammation.
Materials and methods
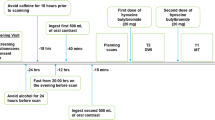
Patients with newly diagnosed ileal CD and healthy control participants were prospectively recruited between December 2018 and October 2021. Patients underwent research MRI examinations of the bowel at baseline and at 6-weeks and 6-months into biologic medical treatment; control participants underwent single MRI examinations. MRI examinations included native T1 relaxometry of the terminal ileum using a modified Look-Locker inversion recovery (MOLLI) sequence. T1 estimates were measured on scanner-generated parametric maps. Clinical markers of intestinal inflammation were recorded at each visit. Group differences were assessed using the Mann–Whitney U test; the Friedman test was used to assess longitudinal changes in T1 estimates. Spearman correlation was used to evaluate associations between T1 estimates and inflammatory markers.
Results
Nineteen participants with CD (12 males; median age 14 years) and 15 control participants (7 males; median age 17 years) were included in the study. Bowel wall T1 estimates in CD patients (median 1302 ms) were significantly longer compared to control participants (median 1159 ms) (p < 0.001). In CD patients, T1 estimates changed over time after treatment (p = 0.001), with largest reductions between baseline and 6-weeks (p < 0.001). T1 estimates correlated with inflammatory markers, including erythrocyte sedimentation rate (ρ = 0.35; p = 0.01), c-reactive protein level (ρ = 0.34; p = 0.02), and weighted Pediatric Crohn’s Disease Activity Index (ρ = 0.39; p = 0.005). T1 estimates did not correlate with serum albumin (ρ = − 0.28; p = 0.051) and fecal calprotectin (ρ = 0.07; p = 0.63).
Conclusion
Bowel wall T1 estimates are abnormally increased in newly diagnosed ileal CD patients and decrease in response to medical therapy.





Similar content being viewed by others
Abbreviations
- CD:
-
Crohn’s disease
- CRP:
-
C-reactive protein
- ESR:
-
Erythrocyte sedimentation rate
- MOLLI:
-
Modified Look-Locker inversion recovery
- TNF:
-
Tumor necrosis factor
- wPCDAI:
-
Weighted Pediatric Crohn’s Disease Activity Index
References
Shikhare G, Kugathasan S. Inflammatory bowel disease in children: current trends. J Gastroenterol 2010;45(7):673-682. https://doi.org/10.1007/s00535-010-0241-5
Benchimol EI, Fortinsky KJ, Gozdyra P, Van den Heuvel M, Van Limbergen J, Griffiths AM. Epidemiology of pediatric inflammatory bowel disease: a systematic review of international trends. Inflamm Bowel Dis 2011;17(1):423-439. https://doi.org/10.1002/ibd.21349
Herrinton LJ, Liu L, Lewis JD, Griffin PM, Allison J. Incidence and prevalence of inflammatory bowel disease in a Northern California managed care organization, 1996-2002. Am J Gastroenterol 2008;103(8):1998-2006. https://doi.org/10.1111/j.1572-0241.2008.01960.x
Kelsen J, Baldassano RN. Inflammatory bowel disease: the difference between children and adults. Inflamm Bowel Dis 2008;14 Suppl 2:S9-11. https://doi.org/10.1002/ibd.20560
Loftus CG, Loftus EV, Jr., Harmsen WS, Zinsmeister AR, Tremaine WJ, Melton LJ, 3rd, Sandborn WJ. Update on the incidence and prevalence of Crohn's disease and ulcerative colitis in Olmsted County, Minnesota, 1940-2000. Inflamm Bowel Dis 2007;13(3):254-261. https://doi.org/10.1002/ibd.20029
Ma C, Battat R, Parker CE, Khanna R, Jairath V, Feagan BG. Update on C-reactive protein and fecal calprotectin: are they accurate measures of disease activity in Crohn’s disease? Expert Review of Gastroenterology & Hepatology 2019;13(4):319-330. https://doi.org/10.1080/17474124.2019.1563481
Sostegni R, Daperno M, Scaglione N, Lavagna A, Rocca R, Pera A. Review article: Crohn's disease: monitoring disease activity. Aliment Pharmacol Ther 2003;17 Suppl 2:11-17. https://doi.org/10.1046/j.1365-2036.17.s2.17.x
Cellier C, Sahmoud T, Froguel E, Adenis A, Belaiche J, Bretagne JF, Florent C, Bouvry M, Mary JY, Modigliani R. Correlations between clinical activity, endoscopic severity, and biological parameters in colonic or ileocolonic Crohn's disease. A prospective multicentre study of 121 cases. The Groupe d'Etudes Therapeutiques des Affections Inflammatoires Digestives. Gut 1994;35(2):231-235. https://doi.org/10.1136/gut.35.2.231
Martin DR, Kalb B, Sauer CG, Alazraki A, Goldschmid S. Magnetic resonance enterography in Crohn's disease: techniques, interpretation, and utilization for clinical management. Diagn Interv Radiol 2012;18(4):374-386. https://doi.org/10.4261/1305-3825.DIR.4893-11.2
Ordas I, Rimola J, Rodriguez S, Paredes JM, Martinez-Perez MJ, Blanc E, Arevalo JA, Aduna M, Andreu M, Radosevic A, Ramirez-Morros AM, Pino S, Gallego M, Jauregui-Amezaga A, Ricart E, Panes J. Accuracy of magnetic resonance enterography in assessing response to therapy and mucosal healing in patients with Crohn's disease. Gastroenterology 2014;146(2):374-382 e371. https://doi.org/10.1053/j.gastro.2013.10.055
Lee S, Choi YH, Cho YJ, Cheon JE, Moon JS, Kang GH, Kim WS. Quantitative evaluation of Crohn's disease using dynamic contrast-enhanced MRI in children and young adults. Eur Radiol 2020;30(6):3168-3177. https://doi.org/10.1007/s00330-020-06684-1
Evrimler S, Swensson JK, Are VS, Tirkes T, Vuppalanchi R, Akisik F. Quantitative assessment of disease severity of primary sclerosing cholangitis with T1 mapping and extracellular volume imaging. Abdom Radiol (NY) 2020. https://doi.org/10.1007/s00261-020-02839-2
Hoad CL, Palaniyappan N, Kaye P, Chernova Y, James MW, Costigan C, Austin A, Marciani L, Gowland PA, Guha IN, Francis ST, Aithal GP. A study of T(1) relaxation time as a measure of liver fibrosis and the influence of confounding histological factors. NMR Biomed 2015;28(6):706-714. https://doi.org/10.1002/nbm.3299
Ntusi NAB, Piechnik SK, Francis JM, Ferreira VM, Matthews PM, Robson MD, Wordsworth PB, Neubauer S, Karamitsos TD. Diffuse Myocardial Fibrosis and Inflammation in Rheumatoid Arthritis: Insights From CMR T1 Mapping. JACC Cardiovasc Imaging 2015;8(5):526-536. https://doi.org/10.1016/j.jcmg.2014.12.025
Taylor AJ, Salerno M, Dharmakumar R, Jerosch-Herold M. T1 Mapping: Basic Techniques and Clinical Applications. JACC Cardiovasc Imaging 2016;9(1):67-81. https://doi.org/10.1016/j.jcmg.2015.11.005
Horsthuis K, Nederveen AJ, de Feiter MW, Lavini C, Stokkers PC, Stoker J. Mapping of T1-values and Gadolinium-concentrations in MRI as indicator of disease activity in luminal Crohn's disease: a feasibility study. J Magn Reson Imaging 2009;29(2):488-493. https://doi.org/10.1002/jmri.21535
Ata NA, Dillman JR, Gandhi D, Dudley JA, Trout AT, Imbus R, Towbin AJ, Denson LA, Tkach JA. Velocity-Encoded Phase Contrast MRI for Measuring Mesenteric Blood Flow in Patients with Newly Diagnosed Small Bowel Crohn Disease. AJR Am J Roentgenol 2022. https://doi.org/10.2214/AJR.22.27437
Hyams JS, Ferry GD, Mandel FS, Gryboski JD, Kibort PM, Kirschner BS, Griffiths AM, Katz AJ, Grand RJ, Boyle JT, et al. Development and validation of a pediatric Crohn's disease activity index. J Pediatr Gastroenterol Nutr 1991;12(4):439-447.
Banerjee R, Pavlides M, Tunnicliffe EM, Piechnik SK, Sarania N, Philips R, Collier JD, Booth JC, Schneider JE, Wang LM, Delaney DW, Fleming KA, Robson MD, Barnes E, Neubauer S. Multiparametric magnetic resonance for the non-invasive diagnosis of liver disease. J Hepatol 2014;60(1):69-77. https://doi.org/10.1016/j.jhep.2013.09.002
Cassinotto C, Feldis M, Vergniol J, Mouries A, Cochet H, Lapuyade B, Hocquelet A, Juanola E, Foucher J, Laurent F, De Ledinghen V. MR relaxometry in chronic liver diseases: Comparison of T1 mapping, T2 mapping, and diffusion-weighted imaging for assessing cirrhosis diagnosis and severity. Eur J Radiol 2015;84(8):1459-1465. https://doi.org/10.1016/j.ejrad.2015.05.019
Puntmann VO, Peker E, Chandrashekhar Y, Nagel E. T1 Mapping in Characterizing Myocardial Disease: A Comprehensive Review. Circ Res 2016;119(2):277-299. https://doi.org/10.1161/CIRCRESAHA.116.307974
Yoon HM, Suh CH, Kim JR, Lee JS, Jung AY, Kim KM, Cho YA. Diagnostic Performance of Magnetic Resonance Enterography for Detection of Active Inflammation in Children and Adolescents With Inflammatory Bowel Disease: A Systematic Review and Diagnostic Meta-analysis. JAMA Pediatr 2017;171(12):1208-1216. https://doi.org/10.1001/jamapediatrics.2017.3400
Oto A, Kayhan A, Williams JT, Fan X, Yun L, Arkani S, Rubin DT. Active Crohn's disease in the small bowel: evaluation by diffusion weighted imaging and quantitative dynamic contrast enhanced MR imaging. J Magn Reson Imaging 2011;33(3):615-624. https://doi.org/10.1002/jmri.22435
Zhu J, Zhang F, Luan Y, Cao P, Liu F, He W, Wang D. Can Dynamic Contrast-Enhanced MRI (DCE-MRI) and Diffusion-Weighted MRI (DW-MRI) Evaluate Inflammation Disease: A Preliminary Study of Crohn's Disease. Medicine (Baltimore) 2016;95(14):e3239. https://doi.org/10.1097/MD.0000000000003239
Qiu Y, Chen BL, Mao R, Zhang SH, He Y, Zeng ZR, Ben-Horin S, Chen MH. Systematic review with meta-analysis: loss of response and requirement of anti-TNFalpha dose intensification in Crohn's disease. J Gastroenterol 2017;52(5):535-554. https://doi.org/10.1007/s00535-017-1324-3
Funding
Funding was supported by National Institutes of Health (Grant No. R21DK114657).
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Mahalingam, N., Tkach, J.A., Denson, L.A. et al. Bowel wall MRI T1 relaxation estimates for assessment of intestinal inflammation in pediatric Crohn’s disease. Abdom Radiol 47, 2730–2738 (2022). https://doi.org/10.1007/s00261-022-03560-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-022-03560-y