Abstract
Objective
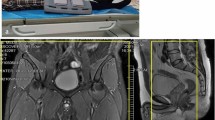
To evaluate the diagnostic accuracy of a contrast-free multimodal magnetic resonance (MR) protocol (including M2DIPEAR, THRIVE, BTFE-SPAIR, and FLAIR sequences) in the detection of iliac vein obstruction with or without thrombosis.
Materials and Methods
From May 1st, 2015, to May 1st, 2016, a total of 73 patients (aged 51.33 ± 4.21 years) who received both digital subtraction angiography (DSA) and the multimodal MR imaging were included. The protocol of the multimodal MR included M2DIPEAR and BTFE-SPAIR for presenting iliac vein obstruction, and THRIVE and FLAIR for revealing the co-existed thrombosis. Three observers who were blinded to clinical and DSA results independently analyzed all multimodal MR datasets. Per-patient evaluations on presence or absence of iliac vein obstruction were performed to calculate the diagnostic performance of MR imaging (DSA regarded as gold reference) in terms of overall accuracy, sensitivity, specificity, positive predictive value (PPV), and negative predictive value (NPV). Capability to display the co-existing venous thrombus was also evaluated per-MR sequence using a 3-point scale system.
Results
Iliac vein obstruction was depicted with DSA in 64 patients. In per-patient evaluation, the multimodal MR imaging yielded accuracy of 95.9% (70/73), sensitivity of 96.9% (62/64), specificity of 88.9% (8/9), positive predictive value of 98.4% (62/63), and negative predictive value of 80% (8/10), respectively. In the multimodal MR sequences, balanced turbo field echo—spectral attenuated inversion recovery (BTFE-SPAIR) sequence was superior to other sequences in depicting the iliac vein configuration, but fluid attenuated inversion recovery (FLAIR) and T1 high-resolution isovolumetric examination (THRIVE) seemed superior in detecting co-existing venous thrombosis.
Conclusions
M2DIPEAR and BTFE-SPAIR sequence can reveal iliac vein obstruction while THRIVE and FLAIR can detect the co-existed thrombosis. The proposed multimodal MR protocol can accurately depict the iliac vein obstruction and accurately detect the co-existing venous thrombosis comparable with that of DSA.


Similar content being viewed by others
References
May R, Thurner J. The cause of the predominantly sinistral occurrence of thrombosis of the pelvic veins. Angiology 1957;8(5):419–427.
Narayan A, Eng J, Carmi L, et al. Iliac vein compression as risk factor for left- versus right-sided deep venous thrombosis: case-control study. Radiology 2012; 265: 949–957.
Neglén P, Thrasher TL, Raju S. Venous outflow obstruction: An underestimated contributor to chronic venous disease. J Vasc Surg 2003; 38(5): 879-885.
Shi WY, Gu JP, Liu CJ, He X, Lou WS. Endovascular treatment for iliac vein compression syndrome with or without lower extremity deep vein thrombosis: A retrospective study on mid-term in-stent patency from a sing center. Eur J Radiol 2016; 85(1): 7-14.
Raju S. Treatment of iliac-caval outflow obstruction. Semin Vasc Surg 2015; 28(1): 47-53.
Neglén P. Chronic venous obstruction: diagnostic considerations and therapeutic role of percutaneous iliac stenting. Vascular 2007; 15(5): 273-280.
Ou-Yang L, Lu GM. Underlying Anatomy and Typing Diagnosis of May-Thurner Syndrome and Clinical Significance: An Observation Based on CT. Spine (Phila Pa 1976) 2016;41(21):E1284-E1291.
Shi WY, Gu JP, Liu CJ, et al. Dual compression is not an uncommon type of iliac vein compression syndrome. Int J Cardiovasc Imaging 2017; 33(9): 1277-1285.
Lamba R, Tanner DT, Sekhon S, et al. Multidetector CT of vascular compression syndromes in the abdomen and pelvis. Radiographics 2014; 34(1): 93-115.
Lugo-Fagundo C, Nance JW, Johnson PT, et al. May-Thurner syndrome: MDCT findings and clinical correlates. Abdom Radiol (NY) 2016; 41(10): 2026-30.
Begemann PG, Bonacker M, Kemper J, et al. Evaluation of the deep venous system in patients with suspected pulmonary embolism with multi-detector CT: a prospective study in comparison to Doppler sonography. J Comput Assist Tomogr. 2003;27(3):399-409.
Reid JH. Multislice CT pulmonary angiography and CT venography. Br J Radiol 2004; 77: S39-S45.
McDermott S, Oliveira G, Ergül E, et al. May-Thurner syndrome: can it be diagnosed by a single MR venography study? Diagn Interv Radiol 2013; 19(1): 44-8.
Fraser DG, Moody AR, Martel A, et al. Re-evaluation of iliac compression syndrome using magnetic resonance imaging in patients with acute deep venous thromboses. J Vasc Surg 2004; 40: 604-611.
Fan Y,Resnick S M,Wu X,et al.Structural and functional biomarkers of prodromal Alzheimer’s disease:a high-dimensional pattern classification study. Neuroimage 2008; 41(2): 277-285.
Liebeskind D S,Alexandrov A V.Advanced multimodal CT/ MRI approaches to hyperacute stroke diagnosis,treatment,and monitoring. Ann N Y Acad Sci 2012; 1268: 1-7.
Diciotti S, Ciulli S, Ginestroni A, et al. Multimodal MRI classification in vascular mild cognitive impairment. Conf Proc IEEE Eng Med Biol Soc 2015; 2015:4278-81.
Wolpert LM, Rahmani O, Stein B, et al. Magnetic resonance venography in the diagnosis and management of May-Thurner syndrome. Vasc Endovascular Surg 2002; 36(1):51-57.
Gurel K, Gurel S, Karavas E, et al. Direct contrast-enhanced MR venography in the diagnosis of May-Thurner syndrome. Eur J Radiol 2011;80(2):533-536.
Kim S, Huh YM, Song HT, et al. Chronic tibiofibular syndesmosis injury of ankle: evaluation with contrast-enhanced fat-suppressed 3D fast spoiled gradient-recalled acquisition in the steady state MR imaging. Radiology 2007; 242: 225-35.
Aydın H, Altın E, Dilli A, et al. Evaluation of jugular foramen nerves by using b-FFE, T2-weighted DRIVE, T2-weighted FSE and post-contrast T1-weighted MRI sequences. Diagn Interv Radiol 2011; 17: 3-9.
Lee YH, Hahn S, Lim D, Suh JS. Articular cartilage grading of the knee: diagnostic performance of fat-suppressed 3D volume isotropic turbo spin-echo acquisition (VISTA) compared with 3D T1 high-resolution isovolumetric examination (THRIVE). Acta Radiologica 2017; 58(2): 190-196.
Pruessm KP, Weiger M, Scheidegger MB, Boesiger P. SENSE: sensitivity encoding for fast MRI. Magn Reson Med 1999; 42(5): 952-962.
Lee YH, Choi YR, Kim S, Song HT, Suh JS. Intrinsic ligament and triangular fibrocartilage complex (TFCC) tears of the wrist: comparison of isovolumetric 3D-THRIVE sequence MR arthrography and conventional MR image at 3T. Magnetic Resonance Imaging 2013; 31:221-226.
Mendichovszky IA, Priest AN, Bowden DJ, et al. Combined MR direct thrombus imaging and non-contrast magnetic resonance venography reveal the evolution of deep vein thrombosis: a feasibility study. Eur Radiol 2017; 27: 2326-2332.
Phinikaridou A, Andia ME, Saha P, et al. In Vivo Magnetization Transfer and Diffusion-Weighted Magnetic Resonance Imaging Detects Thrombus Composition in a Mouse Model of Deep Vein Thrombosis. Circ Cardiovasc Imaging 2013; 6(3): 433-440.
Abdalla G, Fawzi Matuk R, Venugopal V, et al. The diagnostic accuracy of magnetic resonance venography in the detection of deep venous thrombosis: a systematic review and meta-analysis. Clinical Radiology 2015; 70: 858-871
Xie G, Chen H, He X, et al. Black-blood thrombus imaging (BTI): a contrast-free cardiovascular magnetic resonance approach for the diagnosis of non-acute deep vein thrombosis. Journal of Cardiovascular Magnetic Resonance 2017; 19: 4.
Funding
The study has supported by National Natural Science Foundation of China (81873916).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare there is no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shi, WY., Xue, HL., Chen, L. et al. Non-enhanced multimodal magnetic resonance imaging in assessment of iliac vein obstruction with or without thrombosis. Abdom Radiol 46, 4432–4439 (2021). https://doi.org/10.1007/s00261-021-03079-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-021-03079-8