Abstract
Purpose
To develop and validate a CT-based radiomics nomogram in preoperative differential diagnosis of SCNs from mucin-producing PCNs.
Material and methods
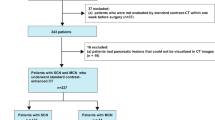
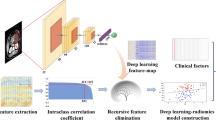
A total of 89 patients consisting of 31 SCNs, 30 IPMNs, and 28 MCNs who underwent preoperative CT were analyzed. A total of 710 radiomics features were extracted from each case. Patients were divided into training (n = 63) and validation cohorts (n = 26) with a ratio of 7:3. Least absolute shrinkage and selection operator (LASSO) method and logistic regression analysis were used for feature selection and model construction. A nomogram was created from a comprehensive model consisting of clinical features and the fusion radiomics signature. A decision curve analysis was used for clinical decisions.
Results
The radiomics features extracted from CT could assist with the differentiation of SCNs from mucin-producing PCNs in both the training and validation cohorts. The signature of the combination of the plain, late arterial, and venous phases had the largest areas under the curve (AUCs) of 0.960 (95% CI 0.910–1) in the training cohort and 0.817 (95% CI 0.651–0.983) in the validation cohort with good calibration. The value and efficacy of the nomogram was verified using decision curve analysis.
Conclusion
A comprehensive nomogram incorporating clinical features and fusion radiomics signature can differentiate SCNs from mucin-producing PCNs.






Similar content being viewed by others
Data availability
All datasets presented in this study are included in the article/supplementary material.
References
Zhong L, Chai N, Linghu E, Li H, Yang J, Tang P (2019) A prospective study on endoscopic ultrasound for the differential diagnosis of serous cystic neoplasms and mucinous cystic neoplasms. BMC Gastroenterol 19:127. https://doi.org/10.1186/s12876-019-1035-8
Kim SY, Lee JM, Kim SH, Shin KS, Kim YJ, An SK, Han CJ, Han JK, Choi BI (2006) Macrocystic neoplasms of the pancreas: CT differentiation of serous oligocystic adenoma from mucinous cystadenoma and intraductal papillary mucinous tumor. AJR Am J Roentgenol 187:1192-1198. https://doi.org/10.2214/AJR.05.0337
Wang GX, Wang ZP, Chen HL, Zhang D, Wen L (2020) Discrimination of serous cystadenoma from mucinous cystic neoplasm and branch duct intraductal papillary mucinous neoplasm in the pancreas with CT. Abdom Radiol (NY) 45:2772-2778.https://doi.org/10.1007/s00261-020-02664-7
European Study Group on Cystic Tumours of the Pancreas (2018) European evidence-based guidelines on pancreatic cystic neoplasms. Gut 67:789-804.https://doi.org/10.1136/gutjnl-2018-316027
Yang J, Guo X, Ou X, Zhang W, Ma X (2019) Discrimination of Pancreatic Serous Cystadenomas From Mucinous Cystadenomas With CT Textural Features: Based on Machine Learning. Front Oncol 9:494.https://doi.org/10.3389/fonc.2019.00494
Lennon AM, Wolfgang CL, Canto MI, Klein AP, Herman JM, Goggins M, Fishman EK, Kamel I, Weiss MJ, Diaz LA, Papadopoulos N, Kinzler KW, Vogelstein B, Hruban RH (2014) The early detection of pancreatic cancer: what will it take to diagnose and treat curable pancreatic neoplasia?. Cancer Res 74:3381-3389.https://doi.org/10.1158/0008-5472.CAN-14-0734
Lopez Hänninen E, Pech M, Ricke J, Denecke T, Amthauer H, Lehmkuhl L, Böhmig M, Röttgen R, Pinkernelle J, Felix R, Langrehr J (2006) Magnetic resonance imaging in the assessment of cystic pancreatic lesions: differentiation of benign and malignant lesion status. Acta Radiol 47:121-129. https://doi.org/10.1080/02841850500334997
Ardengh JC, Lopes CV, de Lima-Filho ER, Kemp R, Dos Santos JS (2014) Impact of endoscopic ultrasound-guided fine-needle aspiration on incidental pancreatic cysts. A prospective study. Scand J Gastroenterol 49:114-120. https://doi.org/10.3109/00365521.2013854830
Ren S, Zhang J, Chen J, Cui W, Zhao R, Qiu W, Duan S, Chen R, Chen X, Wang Z (2019) Evaluation of Texture Analysis for the Differential Diagnosis of Mass-Forming Pancreatitis From Pancreatic Ductal Adenocarcinoma on Contrast-Enhanced CT Images. Front Oncol. https://doi.org/10.3389/fonc.2019.01171
Gillies RJ, Kinahan PE, Hricak H (2016) Radiomics: Images Are More than Pictures, They Are Data. Radiology 278:563-577. https://doi.org/10.1148/radiol.2015151169
Wei R, Lin K, Yan W, Guo Y, Wang Y, Li J, Zhu J (2019) Computer-Aided Diagnosis of Pancreas Serous Cystic Neoplasms: A Radiomics Method on Preoperative MDCT Images. Technol Cancer Res Treat 18:1533033818824339. https://doi.org/10.1177/1533033818824339
Dmitriev K, Kaufman AE, Javed AA, Hruban RH, Fishman EK, Lennon AM, Saltz JH (2017) Classification of Pancreatic Cysts in Computed Tomography Images Using a Random Forest and Convolutional Neural Network Ensemble. Med Image Comput Comput Assist Interv 10435:150-158.https://doi.org/10.1007/978-3-319-66179-7_18
Hanania AN, Bantis LE, Feng Z, Wang H, Tamm EP, Katz MH, Maitra A, Koay EJ (2016) Quantitative imaging to evaluate malignant potential of IPMNs. Oncotarget 7:85776-85784 https://doi.org/10.18632/oncotarget.11769
Ren S, Zhao R, Zhang J, Guo K, Gu X, Duan S, Wang Z, Chen R (2020) Diagnostic accuracy of unenhanced CT texture analysis to differentiate mass-forming pancreatitis from pancreatic ductal adenocarcinoma. Abdom Radiol (NY) 45:1524-1533 https://doi.org/10.1007/s00261-020-02506-6
Gu D, Hu Y, Ding H, Wei J, Chen K, Liu H, Zeng M, Tian J (2019) CT radiomics may predict the grade of pancreatic neuroendocrine tumors: a multicenter study. Eur Radiol 29:6880-6890 https://doi.org/10.1007/s00330-019-06176-x
Xia W, Hu B, Li H, Geng C, Wu Q, Yang L, Yin B, Gao X, Li Y, Geng D (2021) Multiparametric-MRI-Based Radiomics Model for Differentiating Primary Central Nervous System Lymphoma From Glioblastoma: Development and Cross-Vendor Validation. J Magn Reson Imaging 53:242-250 https://doi.org/10.1002/jmri.27344
Cohen-Scali F, Vilgrain V, Brancatelli G, Hammel P, Vullierme MP, Sauvanet A, Menu Y (2003) Discrimination of unilocular macrocystic serous cystadenoma from pancreatic pseudocyst and mucinous cystadenoma with CT: initial observations. Radiology 228:727-733https://doi.org/10.1148/radiol.2283020973
Jais B, Rebours V, Malleo G, Salvia R, Fontana M, Maggino L, Bassi C, Manfredi R, Moran R, Lennon AM, Zaheer A, Wolfgang C, Hruban R, Marchegiani G, Fernández Del Castillo C, Brugge W, Ha Y, Kim MH, Oh D, Hirai I, Kimura W, Jang JY, Kim SW, Jung W, Kang H, Song SY, Kang CM, Lee WJ, Crippa S, Falconi M, Gomatos I, Neoptolemos J, Milanetto AC, Sperti C, Ricci C, Casadei R, Bissolati M, Balzano G, Frigerio I, Girelli R, Delhaye M, Bernier B, Wang H, Jang KT, Song DH, Huggett MT, Oppong KW, Pererva L, Kopchak KV, Del Chiaro M, Segersvard R, Lee LS, Conwell D, Osvaldt A, Campos V, Aguero Garcete G, Napoleon B, Matsumoto I, Shinzeki M, Bolado F, Fernandez JM, Keane MG, Pereira SP, Acuna IA, Vaquero EC, Angiolini MR, Zerbi A, Tang J, Leong RW, Faccinetto A, Morana G, Petrone MC, Arcidiacono PG, Moon JH, Choi HJ, Gill RS, Pavey D, Ouaïssi M, Sastre B, Spandre M, De Angelis CG, Rios-Vives MA, Concepcion-Martin M, Ikeura T, Okazaki K, Frulloni L, Messina O, Lévy P (2016) Serous cystic neoplasm of the pancreas: a multinational study of 2622 patients under the auspices of the International Association of Pancreatology and European Pancreatic Club (European Study Group on Cystic Tumors of the Pancreas). Gut 65:305-312https://doi.org/10.1136/gutjnl-2015-309638
Ketwaroo GA, Mortele KJ, Sawhney MS (2016) Pancreatic Cystic Neoplasms: An Update. Gastroenterol Clin North Am 45:67-81 https://doi.org/10.1016/j.gtc.2015.10.006
Carmicheal J, Patel A, Dalal V, Atri P, Dhaliwal AS, Wittel UA, Malafa MP, Talmon G, Swanson BJ, Singh S, Jain M, Kaur S, Batra SK (2020) Elevating pancreatic cystic lesion stratification: Current and future pancreatic cancer biomarker(s). Biochim Biophys Acta Rev Cancer 1873:188318. https://doi.org/10.1016/j.bbcan.2019.188318
Dalal V, Carmicheal J, Dhaliwal A, Jain M, Kaur S, Batra SK (2020) Radiomics in stratification of pancreatic cystic lesions: Machine learning in action. Cancer Lett 469:228-237https://doi.org/10.1016/j.canlet.2019.10.023
Chu LC, Solmaz B, Park S, Kawamoto S, Yuille AL, Hruban RH, Fishman EK (2020) Diagnostic performance of commercially available vs. in-house radiomics software in classification of CT images from patients with pancreatic ductal adenocarcinoma vs. healthy controls. Abdom Radiol (NY) 45:2469-2475 https://doi.org/10.1007/s00261-020-02556-w
Acknowledgements
We thank all authors for their continuous and excellent support with patient data collection, imaging analysis, statistical analysis and valuable suggestions for the article.
Funding
This study was funded by the National Natural Science Foundation of China (No. 81771899) for Zhongqiu Wang, Postgraduate Research & Practice Innovation Program of Jiangsu Province (No. KYCX20_1477) for Shuai Ren, China Scholarship Council (No. 201909077001) for Shuai Ren, Jiangsu Provincial Key research and development program (No. BE2017772) for Zhongqiu Wang, Administration of Traditional Chinese Medicine of Jiangsu Province (No. ZD201907) for Zhongqiu Wang, and Developing Program for High-level Academic Talent in Jiangsu Hospital of TCM (No. y2018rc04) for Zhongqiu Wang.
Author information
Authors and Affiliations
Contributions
Study design and funds collection: SC, SR, ZQW; provision of study materials or patients: SC, KG; data processing, analysis, and interpretation: SC, SR, RC; manuscript writing and editing: SR, MJD, ZQW, RC.
Corresponding author
Ethics declarations
Conflict of interest
We declare no competing interests.
Ethical approval
This study was a retrospective study, which was approved by the institutional review board of our hospital (2017NL-137-05), wherein the requirements for informed consent was waived due to its retrospective nature.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, S., Ren, S., Guo, K. et al. Preoperative differentiation of serous cystic neoplasms from mucin-producing pancreatic cystic neoplasms using a CT-based radiomics nomogram. Abdom Radiol 46, 2637–2646 (2021). https://doi.org/10.1007/s00261-021-02954-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-021-02954-8