Abstract
Purpose
To compare the differences of MR features between mass-forming intrahepatic cholangiocarcinoma (IMCC) with and without lymph node metastasis (LNM) and to search for new imaging biomarkers for predicting LNM.
Materials and methods
The study included 91 patients with histopathologically confirmed single IMCC (20 patients with LNM and 71 patients without LNM). Findings of preoperative MR imaging including diffusion-weighted imaging (DWI) (b value 0, 500 mm2/s) were analyzed and apparent diffusion coefficient (ADC) values (b = 500 mm2/s) were calculated. Logistic regression analysis was performed to identify independent predictors of LNM. The diagnostic performance of independent predictors was assessed by receiver operating characteristic (ROC) and area under the curve (AUC) was compared.
Results
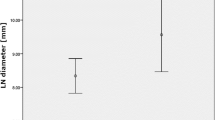
Larger tumor size (p = 0.001), diameter of largest lymph node (LN) > 1 cm (p < 0.001), higher ADC value of primary IMCC lesion (ADCIMCC value) (p = 0.001), and positive CA19-9 level (p = 0.018) were correlated with LNM. Multivariate logistic regression analysis demonstrated that ADCIMCC value (odds ratio, 3.347; p = 0.001) and diameter of largest LN > 1 cm (odds ratio, 7.571; p = 0.004) were independent predictors of LNM. The AUCs for ADCIMCC value, diameter of largest LN > 1 cm,and combined method (the combination of ADCIMCC value and diameter of largest LN > 1 cm) were 0.782, 0.701,and 0.857, respectively. The AUC for combined method was significantly higher than that of diameter of largest LN > 1 cm (p = 0.033).
Conclusion
ADCIMCC value can be a potential imaging biomarker for predicting LNM of IMCC, especially in combination with diameter of largest LN > 1 cm.


Similar content being viewed by others
Abbreviations
- ADC:
-
Apparent diffusion coefficient
- AUC:
-
Area under curve
- DWI:
-
Diffusion-weighted imaging
- IMCC:
-
Mass-forming intrahepatic cholangiocarcinoma
- LN:
-
Lymph node
- LNM:
-
Lymph node metastasis
- MRI:
-
Magnetic resonance imaging
- ROC:
-
Receiver operating characteristic curve
References
Torre LA, Bray F, Siegel RL, Ferlay J, Lortet-Tieulent J, Jemal A (2015) Global cancer statistics, 2012. CA: a cancer journal for clinicians 65 (2):87-108. https://doi.org/10.3322/caac.21262
Khan SA, Emadossadaty S, Ladep NG, Thomas HC, Elliott P, Taylor-Robinson SD, Toledano MB (2012) Rising trends in cholangiocarcinoma: is the ICD classification system misleading us? Journal of hepatology 56 (4):848-854. https://doi.org/10.1016/j.jhep.2011.11.015
Lim JH (2003) Cholangiocarcinoma: morphologic classification according to growth pattern and imaging findings. AJR American journal of roentgenology 181 (3):819-827. https://doi.org/10.2214/ajr.181.3.1810819
de Jong MC, Nathan H, Sotiropoulos GC, Paul A, Alexandrescu S, Marques H, Pulitano C, Barroso E, Clary BM, Aldrighetti L, Ferrone CR, Zhu AX, Bauer TW, Walters DM, Gamblin TC, Nguyen KT, Turley R, Popescu I, Hubert C, Meyer S, Schulick RD, Choti MA, Gigot JF, Mentha G, Pawlik TM (2011) Intrahepatic cholangiocarcinoma: an international multi-institutional analysis of prognostic factors and lymph node assessment. Journal of clinical oncology: official journal of the American Society of Clinical Oncology 29 (23):3140-3145. https://doi.org/10.1200/jco.2011.35.6519
Ali SM, Clark CJ, Mounajjed T, Wu TT, Harmsen WS, Reid-Lombardo KM, Truty MJ, Kendrick ML, Farnell MB, Nagorney DM, Que FG (2015) Model to predict survival after surgical resection of intrahepatic cholangiocarcinoma: the Mayo Clinic experience. HPB : the official journal of the International Hepato Pancreato Biliary Association 17 (3):244-250. https://doi.org/10.1111/hpb.12333
Chun YS, Pawlik TM, Vauthey JN (2018) 8th Edition of the AJCC Cancer Staging Manual: Pancreas and Hepatobiliary Cancers. Annals of surgical oncology 25 (4):845-847. https://doi.org/10.1245/s10434-017-6025-x
Weber SM, Ribero D, O'Reilly EM, Kokudo N, Miyazaki M, Pawlik TM (2015) Intrahepatic cholangiocarcinoma: expert consensus statement. HPB: the official journal of the International Hepato Pancreato Biliary Association 17 (8):669-680. https://doi.org/10.1111/hpb.12441
Songthamwat M, Chamadol N, Khuntikeo N, Thinkhamrop J, Koonmee S, Chaichaya N, Bethony J, Thinkhamrop B (2017) Evaluating a preoperative protocol that includes magnetic resonance imaging for lymph node metastasis in the Cholangiocarcinoma Screening and Care Program (CASCAP) in Thailand. World journal of surgical oncology 15 (1):176. https://doi.org/10.1186/s12957-017-1246-9
Pano B, Sebastia C, Ripoll E, Paredes P, Salvador R, Bunesch L, Nicolau C (2015) Pathways of lymphatic spread in gynecologic malignancies. Radiographics : a review publication of the Radiological Society of North America, Inc 35 (3):916-945. https://doi.org/10.1148/rg.2015140086
Park HS, Lee JM, Choi JY, Lee MW, Kim HJ, Han JK, Choi BI (2008) Preoperative evaluation of bile duct cancer: MRI combined with MR cholangiopancreatography versus MDCT with direct cholangiography. AJR American journal of roentgenology 190 (2):396-405. https://doi.org/10.2214/ajr.07.2310
Hanninen EL, Pech M, Jonas S, Ricke J, Thelen A, Langrehr J, Hintze R, Rottgen R, Denecke T, Winter L, Neuhaus P, Felix R (2005) Magnetic resonance imaging including magnetic resonance cholangiopancreatography for tumor localization and therapy planning in malignant hilar obstructions. Acta Radiol 46 (5):462-470. https://doi.org/10.1080/02841850510021625
Park MS, Lee DK, Kim MJ, Lee WJ, Yoon DS, Lee SJ, Lim JS, Yu JS, Cho JY, Kim KW (2006) Preoperative staging accuracy of multidetector row computed tomography for extrahepatic bile duct carcinoma. Journal of computer assisted tomography 30 (3):362-367
Yoshida T, Matsumoto T, Sasaki A, Shibata K, Aramaki M, Kitano S (2004) Outcome of paraaortic node-positive pancreatic head and bile duct adenocarcinoma. American journal of surgery 187 (6):736-740. https://doi.org/10.1016/j.amjsurg.2003.07.031
Promsorn J, Soontrapa W, Somsap K, Chamadol N, Limpawattana P, Harisinghani M (2019) Evaluation of the diagnostic performance of apparent diffusion coefficient (ADC) values on diffusion-weighted magnetic resonance imaging (DWI) in differentiating between benign and metastatic lymph nodes in cases of cholangiocarcinoma. Abdom Radiol (NY) 44 (2):473-481. https://doi.org/10.1007/s00261-018-1742-6
Holzapfel K, Gaa J, Schubert EC, Eiber M, Kleeff J, Rummeny EJ, Loos M (2016) Value of diffusion-weighted MR imaging in the diagnosis of lymph node metastases in patients with cholangiocarcinoma. Abdom Radiol (NY) 41 (10):1937-1941. https://doi.org/10.1007/s00261-016-0791-y
Sanada Y, Kawashita Y, Okada S, Azuma T, Matsuo S (2014) Review to better understand the macroscopic subtypes and histogenesis of intrahepatic cholangiocarcinoma. World journal of gastrointestinal pathophysiology 5 (3):188-199. https://doi.org/10.4291/wjgp.v5.i3.188
Yamanaka N, Okamoto E, Ando T, Oriyama T, Fujimoto J, Furukawa K, Tanaka T, Tanaka W, Nishigami T (1995) Clinicopathologic spectrum of resected extraductal mass-forming intrahepatic cholangiocarcinoma. Cancer 76 (12):2449-2456. https://doi.org/10.1002/1097-0142(19951215)76:12<2449:aid-cncr2820761208>3.0.co;2-v
Zhu Y, Mao Y, Chen J, Qiu Y, Wang Z, He J (2019) Preoperative Computed Tomography Features of Intrahepatic Cholangiocarcinoma for Predicting Lymph Node Metastasis and Overall Survival. Journal of computer assisted tomography 43 (5):729-735. https://doi.org/10.1097/rct.0000000000000922
Yamamoto Y, Turkoglu MA, Aramaki T, Sugiura T, Okamura Y, Ito T, Ashida R, Uemura S, Miyata T, Kato Y, Kakuta Y, Nakanuma Y, Uesaka K (2016) Vascularity of Intrahepatic Cholangiocarcinoma on Computed Tomography is Predictive of Lymph Node Metastasis. Annals of surgical oncology 23 (Suppl 4):485-493. https://doi.org/10.1245/s10434-016-5382-1
Elsayes KM, Hooker JC, Agrons MM, Kielar AZ, Tang A, Fowler KJ, Chernyak V, Bashir MR, Kono Y, Do RK, Mitchell DG, Kamaya A, Hecht EM, Sirlin CB (2017) 2017 Version of LI-RADS for CT and MR Imaging: An Update. Radiographics : a review publication of the Radiological Society of North America, Inc 37 (7):1994-2017. https://doi.org/10.1148/rg.2017170098
Lee J, Kim SH, Kang TW, Song KD, Choi D, Jang KT (2016) Mass-forming Intrahepatic Cholangiocarcinoma: Diffusion-weighted Imaging as a Preoperative Prognostic Marker. Radiology 281 (1):119-128. https://doi.org/10.1148/radiol.2016151781
Zhou Y, Wang X, Xu C, Zhou G, Liu X, Gao S, Xu P (2019) Mass-forming intrahepatic cholangiocarcinoma: Can diffusion-weighted imaging predict microvascular invasion? J Magn Reson Imaging 50 (1):315-324. https://doi.org/10.1002/jmri.26566
Uno M, Shimada K, Yamamoto Y, Nara S, Esaki M, Sakamoto Y, Kosuge T, Ojima H (2012) Periductal infiltrating type of intrahepatic cholangiocarcinoma: a rare macroscopic type without any apparent mass. Surg Today 42 (12):1189-1194. https://doi.org/10.1007/s00595-012-0145-5
Shimada K, Sano T, Sakamoto Y, Esaki M, Kosuge T, Ojima H (2007) Surgical outcomes of the mass-forming plus periductal infiltrating types of intrahepatic cholangiocarcinoma: a comparative study with the typical mass-forming type of intrahepatic cholangiocarcinoma. World journal of surgery 31 (10):2016-2022. https://doi.org/10.1007/s00268-007-9194-0
Rimola J, Forner A, Reig M, Vilana R, de Lope CR, Ayuso C, Bruix J (2009) Cholangiocarcinoma in cirrhosis: absence of contrast washout in delayed phases by magnetic resonance imaging avoids misdiagnosis of hepatocellular carcinoma. Hepatology (Baltimore, Md) 50 (3):791-798. https://doi.org/10.1002/hep.23071
Lewis S, Besa C, Wagner M, Jhaveri K, Kihira S, Zhu H, Sadoughi N, Fischer S, Srivastava A, Yee E, Mortele K, Babb J, Thung S, Taouli B (2018) Prediction of the histopathologic findings of intrahepatic cholangiocarcinoma: qualitative and quantitative assessment of diffusion-weighted imaging. European radiology 28 (5):2047-2057. https://doi.org/10.1007/s00330-017-5156-6
Park HJ, Kim YK, Park MJ, Lee WJ (2013) Small intrahepatic mass-forming cholangiocarcinoma: target sign on diffusion-weighted imaging for differentiation from hepatocellular carcinoma. Abdom Imaging 38 (4):793-801. https://doi.org/10.1007/s00261-012-9943-x
Horgan AM, Amir E, Walter T, Knox JJ (2012) Adjuvant therapy in the treatment of biliary tract cancer: a systematic review and meta-analysis. Journal of clinical oncology: official journal of the American Society of Clinical Oncology 30 (16):1934-1940. https://doi.org/10.1200/jco.2011.40.5381
Kobayashi S, Tomokuni A, Gotoh K, Takahashi H, Akita H, Marubashi S, Yamada T, Teshima T, Nishiyama K, Yano M, Ohigashi H, Ishikawa O, Sakon M (2015) Evaluation of the safety and pathological effects of neoadjuvant full-dose gemcitabine combination radiation therapy in patients with biliary tract cancer. Cancer chemotherapy and pharmacology 76 (6):1191-1198. https://doi.org/10.1007/s00280-015-2908-3
Shimada K, Sano T, Nara S, Esaki M, Sakamoto Y, Kosuge T, Ojima H (2009) Therapeutic value of lymph node dissection during hepatectomy in patients with intrahepatic cholangiocellular carcinoma with negative lymph node involvement. Surgery 145 (4):411-416. https://doi.org/10.1016/j.surg.2008.11.010
Chen YX, Zeng ZC, Tang ZY, Fan J, Zhou J, Jiang W, Zeng MS, Tan YS (2011) Prediction of the lymph node status in patients with intrahepatic cholangiocarcinoma: analysis of 320 surgical cases. Frontiers in oncology 1:42. https://doi.org/10.3389/fonc.2011.00042
Meng ZW, Lin XQ, Zhu JH, Han SH, Chen YL (2018) A nomogram to predict lymph node metastasis before resection in intrahepatic cholangiocarcinoma. The Journal of surgical research 226:56-63. https://doi.org/10.1016/j.jss.2018.01.024
Tang Y, Rao S, Yang C, Hu Y, Sheng R, Zeng M (2018) Value of MRI morphologic features with pT1-2 rectal cancer in determining lymph node metastasis. Journal of surgical oncology 118 (3):544-550. https://doi.org/10.1002/jso.25173
Kang Y, Lee JM, Kim SH, Han JK, Choi BI (2012) Intrahepatic mass-forming cholangiocarcinoma: enhancement patterns on gadoxetic acid-enhanced MR images. Radiology 264 (3):751-760. https://doi.org/10.1148/radiol.12112308
Koh J, Chung YE, Nahm JH, Kim HY, Kim KS, Park YN, Kim MJ, Choi JY (2016) Intrahepatic mass-forming cholangiocarcinoma: prognostic value of preoperative gadoxetic acid-enhanced MRI. European radiology 26 (2):407-416. https://doi.org/10.1007/s00330-015-3846-5
Malayeri AA, El Khouli RH, Zaheer A, Jacobs MA, Corona-Villalobos CP, Kamel IR, Macura KJ (2011) Principles and applications of diffusion-weighted imaging in cancer detection, staging, and treatment follow-up. Radiographics : a review publication of the Radiological Society of North America, Inc 31 (6):1773-1791. https://doi.org/10.1148/rg.316115515
Maetani Y, Itoh K, Watanabe C, Shibata T, Ametani F, Yamabe H, Konishi J (2001) MR imaging of intrahepatic cholangiocarcinoma with pathologic correlation. AJR American journal of roentgenology 176 (6):1499-1507. https://doi.org/10.2214/ajr.176.6.1761499
Murakami T, Nakamura H, Tsuda K, Ishida T, Tomoda K, Hori S, Monden M, Kanai T, Wakasa K, Sakurai M, et al. (1995) Contrast-enhanced MR imaging of intrahepatic cholangiocarcinoma: pathologic correlation study. J Magn Reson Imaging 5 (2):165-170.
Ni P, Lin Y, Zhong Q, Chen Z, Sandrasegaran K, Lin C (2016) Technical advancements and protocol optimization of diffusion-weighted imaging (DWI) in liver. Abdom Radiol (NY) 41 (1):189-202. https://doi.org/10.1007/s00261-015-0602-x
Xu P, Zeng M, Liu K, Shan Y, Xu C, Lin J (2014) Microvascular invasion in small hepatocellular carcinoma: is it predictable with preoperative diffusion-weighted imaging? Journal of gastroenterology and hepatology 29 (2):330-336. https://doi.org/10.1111/jgh.12358
Suh YJ, Kim MJ, Choi JY, Park MS, Kim KW (2012) Preoperative prediction of the microvascular invasion of hepatocellular carcinoma with diffusion-weighted imaging. Liver transplantation: official publication of the American Association for the Study of Liver Diseases and the International Liver Transplantation Society 18 (10):1171-1178. https://doi.org/10.1002/lt.23502
Kwee TC, Takahara T, Koh DM, Nievelstein RA, Luijten PR (2008) Comparison and reproducibility of ADC measurements in breathhold, respiratory triggered, and free-breathing diffusion-weighted MR imaging of the liver. J Magn Reson Imaging 28 (5):1141-1148. https://doi.org/10.1002/jmri.21569
Funding
This study was supported by grants from the Shanghai Municipal Key Clinical Specialty (W2019-018).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This study does not contain any studies with animals performed by any of the authors. For this type of study formal consent is not required.
Informed consent
The institutional review board approved this study and waived informed consent because of retrospective study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Zhou, Y., Zhou, G., Gao, X. et al. Apparent diffusion coefficient value of mass-forming intrahepatic cholangiocarcinoma: a potential imaging biomarker for prediction of lymph node metastasis. Abdom Radiol 45, 3109–3118 (2020). https://doi.org/10.1007/s00261-020-02458-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-020-02458-x