Abstract
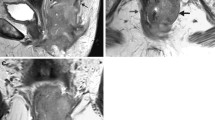
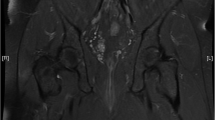
Anal complaints are very common in the general population and are caused by a variety of disorders mostly benign in nature. The aim of this article is to provide the radiologist with a detailed description of the MRI anatomy and technique, and an overview of the various diseases most commonly presenting with anal pain, by descriptions and illustrative examples of MRI features of each entity.
































Similar content being viewed by others
References
Lunniss PJ (2016) Chapter: 66 Large intestine. In: Standring S (ed) Gray’s anatomy: the anatomical basis of clinical practice, 41st edn. London: Elsevier Churchill Livingstone, pp 1155–1158
Krieglstein CF (2008) Surgical procedures for perianal sepsis: ıschiorectal abscesses, fistulas, and pilonidal sinus. In: Thomas WEG, Senninger N (eds). Short Stay Surgery. Chapter 15, Springer, Berlin, pp. 295–308
Agur AMR, Lee MJ, Grant JCB (1999) Grant’s atlas of anatomy, 10th edn. London: Lippincott Williams and Wilkins
Salerno G, Sinnatambi C, Branagan G, et al. (2006) Defining the rectum: surgically, radiologically and anatomically. Colorectal Dis 8:5–9
Erden A, Peker E, Gençtürk ZB (2017) Chronic anal fissure: morphometric analysis of the anal canal at 3.0 Tesla MR imaging. Abdom Radiol (NY) 42:423–434
Al-Ali S, Blyth P, Beatty S, et al. (2009) Correlation between gross anatomical topography, sectional sheet plastination, microscopic anatomy and endoanal sonography of the anal sphincter complex in human males. J Anat 215:212–220
Beets-Tan RG, Morren GL, Beets GL, et al. (2001) Measurement of anal sphincter muscles: endoanal US, endoanal MR imaging, or phased-array MR imaging? A study with healthy volunteers. Radiology 220:81–89
Rociu E, Stoker J, Eijkemans MJ, Laméris JS (2000) Normal anal sphincter anatomy and age- and sex-related variations at high-spatial-resolution endoanal MR imaging. Radiology 217:395–401
Huebner M, Margulies RU, Fenner DE, et al. (2007) Age effects on internal anal sphincter thickness and diameter in nulliparous females. Dis Colon Rectum 50:1405–1411
Lewicky-Gaupp C, Hamilton Q, Ashton-Miller J, et al. (2009) Anal sphincter structure and function relationships in aging and fecal incontinence. Am J Obstet Gynecol 200(559):e1
Klosterhalfen B, Offner F, Topf N, Vogel P, Mittermayer C (1990) Sclerosis of the internal anal sphincter-a process of aging. Dis Colon Rectum 33:606–609
Federative Committee on Anatomical Terminology (1998) Muscles; muscular system. In: Terminologia anatomica: international anatomical terminology. Georg Thieme Verlag, Stuttgart, pp. 39–40
Wasserman IF (1964) Puborectalis syndrome (rectal stenosis due to anorectal spasm). Dis Colon Rectum 7:87–98
Macchi V, Porzionato A, Stecco C, et al. (2008) Histo-topographic study of the longitudinal anal muscle. Clin Anat 21:447–452
Skandalakis JE, Colborn GL (2004) Chapter 18. Large intestine and anorectum. In: Skandalakis’ surgical anatomy: the embryologic and anatomic basis of modern surgery, 1st edn. Athens: Paschalidis Medical Publications
Colaiacomo MC, Masselli G, Polettini E, et al. (2009) Dynamic MR imaging of the pelvic floor: a pictorial review. Radiographics 29:e35
Goh V, Halligan S, Kaplan G, Healy JC, Bartram CI (2000) Dynamic MR imaging of the pelvic floor in asymptomatic subjects. AJR Am J Roentgenol 174:661–666
Schreyer AG, Paetzel C, Fürst A, et al. (2012) Dynamic magnetic resonance defecography in 10 asymptomatic volunteers. World J Gastroenterol 18:6836–6842
Kinugasa Y, Arakawa T, Abe S, et al. (2011) Anatomical reevaluation of the anococcygeal ligament and its surgical relevance. Dis Colon Rectum 54:232–237
Santoro GA, Shobeiri SA, Petros PP, Zapater P, Wieczorek AP (2016) Perineal body anatomy seen by three-dimensional endovaginal ultrasound of asymptomatic nulliparae. Colorectal Dis 18:400–409
Shafik A, Sibai OE, Shafik AA, Shafik IA (2007) A novel concept for the surgical anatomy of the perineal body. Dis Colon Rectum 50:2120–2125
Lunniss PJ, Armstrong P, Barker PG, et al. (1992) Magnetic resonance imaging of anal fistulae. Lancet 340:394–396
Spencer JA, Chapple K, Wilson D, et al. (1998) Outcome after surgery for perianal fistula: predictive value of MR imaging. AJR Am J Roentgenol 171:403–406
Glynne-Jones R, Northover JM, Cervantes A (2010) ESMO guidelines working group. Anal cancer: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 21:87–92
Brown G, Daniels IR, Richardson C, et al. (2005) Techniques and trouble-shooting in high spatial resolution thin slice MRI for rectal cancer. Br J Radiol 78:245–251
Halligan S, Stoker J (2006) Imaging of fistula in ano. Radiology 239:18–33
Parks AG, Gordon PH, Hardcastle JD (1976) A classification of fistula-in-ano. Br J Surg 63:1–12
Morris J, Spencer JA, Ambrose NS (2000) MR imaging classification of perianal fistulas and its implications for patient management. Radiographics 20:623–635
de Miguel Criado J, del Salto LG, Rivas PF, et al. (2012) MR imaging evaluation of perianal fistulas: spectrum of imaging features. Radiographics 32:175–194
van Koperen PJ, Bemelman WA, Gerhards MF, et al. (2011) The anal fistula plug treatment compared with the mucosal advancement flap for cryptoglandular high transsphincteric perianal fistula: a double-blinded multicenter randomized trial. Dis Colon Rectum 54:387–393
Beets-Tan RG, Beets GL, van der Hoop AG, et al. (2001) Preoperative MR imaging of anal fistulas: does it really help the surgeon? Radiology 218:75–84
Buchanan G, Halligan S, Williams A, et al. (2002) Effect of MRI on clinical outcome of recurrent fistula-in-ano. Lancet 360:1661–1662
Makris GM, Poulakaki N, Papanota AM, et al. (2017) Vulvar, perianal and perineal cancer after hidradenitis suppurativa: a systematic review and pooled analysis. Dermatol Surg 43:107–115
Thomas M, Bienkowski R, Vandermeer TJ, Trostle D, Cagir B (2010) Malignant transformation in perianal fistulas of Crohn’s disease: a systematic review of literature. J Gastrointest Surg 14:66–73
Schwartz DA, Loftus EV Jr, Tremaine WJ, et al. (2002) The natural history of fistulizing Crohn’s disease in Olmsted County, Minnesota. Gastroenterology 122:875–880
Hellers G, Bergstrand O, Ewerth S, et al. (1980) Occurrence and outcome after primary treatment of anal fistulae in Crohn’s disease Gut 21:525–527
Langman JM, Rowland R (1992) Density of lymphoid follicles in the rectum and at the anorectal junction. J Clin Gastroenterol 14:81–84
Tang LY, Rawsthorne P, Bernstein CN (2006) Are perineal and luminal fistulas associated in Crohn’s disease? A population-based study. Clin Gastroenterol Hepatol 4:1130–1134
Wise PE, Schwartz DA (2012) The Evaluation and treatment of Crohn perianal fistulae: EUA, EUS, MRI, and other imaging modalities. Gastroenterol Clin N Am 41:379–391
Van Assche G, Vanbeckevoort D, Bielen D, et al. (2003) Persistent fistula tracks in perianal Crohn’s disease after long-term infliximab treatment: correlation with clinical outcome. Gastroenterology 125:1025–1031
Ng SC, Plamondon S, Gupta A, et al. (2009) Prospective evaluation of anti-tumor necrosis factor therapy guided by magnetic resonance imaging for Crohn’s perineal fistulas. Am J Gastroenterol 104:2973–2986
Makowiec F, Jehle EC, Becker HD, et al. (1997) Perianal abscess in Crohn’s disease. Dis Colon Rectum 40:443–450
Williamson PR, Hellinger MD, Larach SW, et al. (1995) Twenty-year review of the surgical management of perianal Crohn’s disease. Dis Colon Rectum 38:389–392
Bayer I, Gordon PH (1994) Selected operative management of fistula-in-ano in Crohn’s disease. Dis Colon Rectum 37:760–765
Van Assche G, Vanbeckevoort D, Bielen D, et al. (2003) Persistent fistula tracks in perianal Crohn’s disease after long-term infliximab treatment: correlation with clinical outcome. Gastroenterology 125:1025–1031
Savoye-Collet C, Savoye G, Koning E, et al. (2011) Fistulizing perianal Crohn’s disease: contrast-enhanced magnetic resonance imaging assessment at 1 year on maintenance anti-TNF-alpha therapy. Inflamm Bowel Dis 17:1751–1758
Karmiris K, Bielen D, Vanbeckevoort D, et al. (2011) Long-term monitoring of infliximab therapy for perianal fistulizing Crohn’s disease by using magnetic resonance imaging. Clin Gastroenterol Hepatol 9:130–136
Baker B, Al-Salman M, Daoud F (2014) Management of acute perianal sepsis in neutropenic patients with hematological malignancy. Tech Coloproctol 18:327–333
Plumb AA, Halligan S, Bhatnagar G, Taylor SA (2015) Perianal sepsis in hematologic malignancy: MR imaging appearances and distinction from cryptoglandular infection in immunocompetent patients. Radiology 276:147–155
Billingham RP, Isler JT, Kimmins MH, et al. (2004) The diagnosis and management of common anorectal disorders. Curr Probl Surg 41:586–645
Taylor SA, Halligan S, Bartram CI (2003) Pilonidal sinus disease: MR imaging distinction from fistula in ano. Radiology. 226:662–667
Kelly AM, Cronin P (2005) MRI features of hidradenitis suppurativa and review of the literature. AJR Am J Roentgenol 185:1201–1204
Takiyama H, Kazama S, Tanoue Y, et al. (2015) Efficacy of magnetic resonance imaging in the diagnosis of perianal hidradenitis suppurativa, complicated by anal fistulae: a report of two cases and review of the literature. Int J Surg Case Rep 15:107–111
Griffin N, Williams AB, Anderson S, et al. (2014) Hidradenitis suppurativa: MRI features in anogenital disease. Dis Colon Rectum 57:762–771
Das B, Snyder M (2016) Rectovaginal fistulae. Clin Colon Rectal Surg. 29:50–56
Dwarkasing S, Hussain SM, Hop WC, Krestin GP (2004) Anovaginal fistulas: evaluation with endoanal MR imaging. Radiology 231:123–128
Felt-Bersma RJ, Bartelsman JF (2009) Haemorrhoids, rectal prolapse, anal fissure, peri-anal fistulae and sexually transmitted diseases. Best Pract Res Clin Gastroenterol 23:575–592
Perry WB, Dykes SL, Buie WD, Rafferty JF (2010) Practice parameters for the management of anal fissures (3rd revision). Dis Colon Rectum 53:1110–1115
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No funding was received.
Conflict of interest
The author declares that she has no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. For this type of study formal consent is not required.
Rights and permissions
About this article
Cite this article
Erden, A. MRI of anal canal: normal anatomy, imaging protocol, and perianal fistulas: Part 1. Abdom Radiol 43, 1334–1352 (2018). https://doi.org/10.1007/s00261-017-1305-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-017-1305-2