Abstract
Purpose
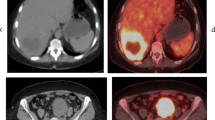
The computed tomography (CT) morphologic response of colorectal liver metastases (CLM) after chemotherapy is reportedly correlated with pathologic response and survival outcomes of patients undergoing surgery. However, they are rather subjective criteria and not evaluable without adequate quality of contrast-enhanced CT images. This study sought the potential use of fluorine-18-fluorodeoxyglucose (FDG) positron emission tomography (PET) as an objective substitute for predicting pathological viability of CLM after chemotherapy.
Methods
Predictive ability of tumor viability of ≤10% was compared between FDG-PET/CT and contrast-enhanced CT in 34 patients who underwent curative surgical resection for CLM after chemotherapy. The CT morphology and response were defined according to the reported criteria (Chun YS, JAMA 2009).
Results
The mean standard uptake value (SUV-mean) in CLM was significantly lower in patients with group 1 and group 2 CT morphology (median, 2.53 and 3.00, respectively) than in group 3 (median, 3.32). The tumor SUV-mean showed moderate correlation with the tumor pathologic viability (r = 0.660, P < 0.0001). A receiver operating characteristic curve analysis revealed that both the tumor SUV-mean (area under the curve [AUC], 0.916; the cut-off value, 3.00) and the CT morphology (AUC, 0.882) have excellent predictive power for ≤10% of tumor viability, while degree of tumor shrinkage showed lower predictive power (AUC, 0.692).
Conclusions
FDG-PET shows significant correlation with pathologic viability of CLM after chemotherapy and may offer additional objective information for estimating tumor viability when the CT morphologic response is not evaluable.




Similar content being viewed by others
References
Adam R, et al. (2004) Tumor progression while on chemotherapy: a contraindication to liver resection for multiple colorectal metastases? Ann Surg 240:1052–1061 ((discussion 61–4))
Blazer DG 3rd, et al. (2008) Pathologic response to preoperative chemotherapy: a new outcome end point after resection of hepatic colorectal metastases. J Clin Oncol 26:5344–5351
Maru DM, et al. (2010) Tumor thickness at the tumor-normal interface: a novel pathologic indicator of chemotherapy response in hepatic colorectal metastases. Am J Surg Pathol 34:1287–1294
Vigano L, et al. (2013) Liver resection for colorectal metastases after chemotherapy: impact of chemotherapy-related liver injuries, pathological tumor response, and micrometastases on long-term survival. Ann Surg 258:731–740 ((discussion 41-2))
Chun YS, et al. (2009) Association of computed tomography morphologic criteria with pathologic response and survival in patients treated with bevacizumab for colorectal liver metastases. JAMA 302:2338–2344
Shindoh J, et al. (2012) Optimal morphologic response to preoperative chemotherapy: an alternate outcome end point before resection of hepatic colorectal metastases. J Clin Oncol 30:4566–4572
Nishioka Y, et al. (2015) Radiological morphology of colorectal liver metastases after preoperative chemotherapy predicts tumor viability and postoperative outcomes. J Gastrointest Surg 19:1653–1661
Luo J, et al. (2016) The value of 18F-FDG PET/CT imaging combined with pretherapeutic Ki67 for early prediction of pathologic response after neoadjuvant chemotherapy in locally advanced breast cancer. Medicine 95:e2914
Tian F, et al. (2017) The accuracy of 18F-FDG PET/CT in predicting the pathological response to neoadjuvant chemotherapy in patients with breast cancer: a meta-analysis and systematic review. Eur Radiol. doi:10.1007/s00330-017-4831-y
Manoharan V, et al. (2017) Serial imaging using [18F]Fluorodeoxyglucose positron emission tomography and histopathologic assessment in predicting survival in a population of surgically resectable distal oesophageal and gastric adenocarcinoma following neoadjuvant therapy. Ann Nucl Med 31:315–323
Akhurst T, et al. (2005) Recent chemotherapy reduces the sensitivity of [18F]fluorodeoxyglucose positron emission tomography in the detection of colorectal metastases. J Clin Oncol 23:8713–8716
Heosprbkgpj NV (2007) F18-FDG-PET evaluation of patients for resection of colorectal liver metastases. Hepatogastroenterology 54:1667–1671
Yoshita H, et al. (2014) Predictive value of optimal morphologic response to first-line chemotherapy in patients with colorectal liver metastases. Digestion 89:43–48
Seyal AR, et al. (2015) Performance of tumor growth kinetics as an imaging biomarker for response assessment in colorectal liver metastases: correlation with FDG PET. Abdom Imaging 40:3043–3051
Zaniboni A, et al. (2015) Positron emission tomography for the response evaluation following treatment with chemotherapy in patients affected by colorectal liver metastases: a selected review. Gastroenterol Res Pract 2015:706808
Heinemann V, et al. (1990) Early tumour shrinkage (ETS) and depth of response (DpR) in the treatment of patients with metastatic colorectal cancer (mCRC). Eur J Cancer 2015(51):1927–1936
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was funded by JSPS KAKENHI (Grant No. 26861063).
Conflict of interest
The authors have no potential conflict of interest to disclose.
Ethical approval
This study was performed in accordance with the ethical guidelines for clinical studies at Toranomon Hospital and the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards under approval of institutional review board (IRB).
Informed consent
Informed consent was waived for this retrospective study with appropriate review process by IRB and release of study protocol.
Rights and permissions
About this article
Cite this article
Nishioka, Y., Yoshioka, R., Gonoi, W. et al. Fluorine-18-fluorodeoxyglucose positron emission tomography as an objective substitute for CT morphologic response criteria in patients undergoing chemotherapy for colorectal liver metastases. Abdom Radiol 43, 1152–1158 (2018). https://doi.org/10.1007/s00261-017-1287-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-017-1287-0