Abstract
Purpose
Bone lesions on prostate MRI often raise concern about metastases. This study aimed to evaluate the prevalence of bone metastases on staging prostate MRI and evaluate associations between their MRI features and clinical/pathologic characteristics.
Methods
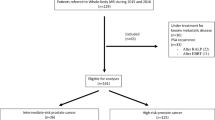
Retrospective, IRB-approved study of 3765 patients undergoing prostate MRI for newly diagnosed PCa between 2000 and 2014. The reference standard to calculate the prevalence of bone metastases was bone biopsy and/or ≥1-year follow-up after MRI. In a subsample of 228 patients, the MRI characteristics of bone lesions were recorded by two radiologists independently. Associations between MRI and clinical/pathologic findings, including National Comprehensive Cancer Network (NCCN) risk categories, were calculated.
Results
57/3765 patients (1.5%, 95% CI 1.2–2.0%) had bone metastases. No patient with NCCN low-risk PCa (Gleason < 7, PSA < 10 ng/mL, cT1-2a) had bone metastases. In the subsample, ≥1 bone lesion was present on MRI in 74% (95% CI 0.67–0.79) and 72% (95% CI 0.66–0.78) of patients (R1 and R2). Larger lesion diameter (OR 1.33/1.19; p < 0.001 for both readers) and the absence of intralesional fat (OR 0.07/0.11; p = 0.004/0.002 for R1/R2) were significantly associated with bone metastases.
Conclusion
Bone lesions are common in prostate MRI, but only rarely represent metastases. MRI should be interpreted in the context of clinical features that influence the likelihood of metastatic disease.



Similar content being viewed by others
Abbreviations
- AUC:
-
Area under the curve
- CaPSURE:
-
Cancer of the prostate strategic urologic research endeavor
- CI:
-
Confidence interval
- MRI:
-
Magnetic resonance imaging
- NCCN:
-
National Comprehensive Cancer Network
- OR:
-
Odds ratio
- PCa:
-
Prostate cancer
- PI-RADS:
-
Prostate imaging reporting and data system
- PSA:
-
Prostate-specific antigen
References
DeSantis CE, Lin CC, Mariotto AB, et al. (2014) Cancer treatment and survivorship statistics, 2014. CA Cancer J Clin. 64(4):252–271
Heidenreich A, Bastian PJ, Bellmunt J, et al. (2014) EAU guidelines on prostate cancer. part 1: screening, diagnosis, and local treatment with curative intent-update 2013. Eur Urol. 65(1):124–137
Wilt TJ, Brawer MK, Jones KM, et al. (2012) Radical prostatectomy versus observation for localized prostate cancer. N Engl J Med. 367(3):203–213
Gondo T, Hricak H, Sala E, et al. (2014) Multiparametric 3T MRI for the prediction of pathological downgrading after radical prostatectomy in patients with biopsy-proven Gleason score 3 + 4 prostate cancer. Eur Radiol. 24(12):3161–3170
Fascelli M, George AK, Frye T, et al. (2015) The role of MRI in active surveillance for prostate cancer. Curr Urol Rep. 16(6):507
Eberhardt SC, Carter S, Casalino DD, et al. (2013) ACR appropriateness criteria prostate cancer–pretreatment detection, staging, and surveillance. J Am Coll Radiol. 10(2):83–92
Wang L, Mullerad M, Chen HN, et al. (2004) Prostate cancer: incremental value of endorectal MR imaging findings for prediction of extracapsular extension. Radiology. 232(1):133–139
Donati OF, Afaq A, Vargas HA, et al. (2014) Prostate MRI: evaluating tumor volume and apparent diffusion coefficient as surrogate biomarkers for predicting tumor Gleason score. Clin Cancer Res. 20(14):3705–3711
Sartor AO, Hricak H, Wheeler TM, et al. (2008) Evaluating localized prostate cancer and identifying candidates for focal therapy. Urology. 72(6 Suppl):S12–S24
Vargas HA, Akin O, Afaq A, et al. (2012) Magnetic resonance imaging for predicting prostate biopsy findings in patients considered for active surveillance of clinically low risk prostate cancer. J Urol. 188(5):1732–1738
Sciarra A, Barentsz J, Bjartell A, et al. (2011) Advances in magnetic resonance imaging: how they are changing the management of prostate cancer. Eur Urol. 59(6):962–977
Turkbey B, Brown AM, Sankineni S, et al. (2016) Multiparametric prostate magnetic resonance imaging in the evaluation of prostate cancer. CA Cancer J Clin. 66(4):326–336
Thompson JE, van Leeuwen PJ, Moses D, et al. (2016) The diagnostic performance of multiparametric magnetic resonance imaging to detect significant prostate cancer. J Urol. 195(5):1428–1435
Weinreb JC, Barentsz JO, Choyke PL, et al. (2016) PI-RADS prostate imaging - reporting and data system: 2015, version 2. Eur Urol 69(1):16–40
Vargas HA, Hotker AM, Goldman DA, et al. (2016) Updated prostate imaging reporting and data system (PIRADS v2) recommendations for the detection of clinically significant prostate cancer using multiparametric MRI: critical evaluation using whole-mount pathology as standard of reference. Eur Radiol. 26(6):1606–1612
Sobin LH, Gospodarowicz MK, Wittekind Ch (2009) TNM Classification of Malignant Tumors. UICC International Union Against Cancer, 7th edn. Berlin: Springer
Ryan CJ, Elkin EP, Small EJ, Duchane J, Carroll P (2006) Reduced incidence of bony metastasis at initial prostate cancer diagnosis: data from CaPSURE. Urol Oncol 24(5):396–402
Jacobson AF (2000) Association of prostate-specific antigen levels and patterns of benign and malignant uptake detected. on bone scintigraphy in patients with newly diagnosed prostate carcinoma. Nucl Med Commun 21(7):617–622
Wang Y, Wan F, Xu L, et al. (2015) Is it safe to omit baseline bone scan for newly diagnosed prostate cancer patients? Urol Int 94(3):342–346
Simpfendorfer CS, Ilaslan H, Davies AM, et al. (2008) Does the presence of focal normal marrow fat signal within a tumor on MRI exclude malignancy? An analysis of 184 histologically proven tumors of the pelvic and appendicular skeleton. Skelet Radiol. 37(9):797–804
Zacho HD, Barsi T, Mortensen JC, et al. (2014) Prospective multicenter study of bone scintigraphy in consecutive patients with newly diagnosed prostate cancer. Clin Nucl Med. 39(1):26–31
Ozgur BC, Gultekin S, Ekici M, Yilmazer D, Alper M (2015) A narrowing range of bone scan in newly diagnosed prostate cancer patients: a retrospective comparative study. Urol Ann. 7(2):193–198
Lavery HJ, Brajtbord JS, Levinson AW, et al. (2011) Unnecessary imaging for the staging of low-risk prostate cancer is common. Urology. 77(2):274–278
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This study was partially funded by NIH Grant Number P30 CA008748.
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Hebert Alberto Vargas and Rachel Schor-Bardach have contributed equally to this manuscript.
Rights and permissions
About this article
Cite this article
Vargas, H.A., Schor-Bardach, R., Long, N. et al. Prostate cancer bone metastases on staging prostate MRI: prevalence and clinical features associated with their diagnosis. Abdom Radiol 42, 271–277 (2017). https://doi.org/10.1007/s00261-016-0851-3
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-016-0851-3