Abstract
Purpose
Prostate-specific membrane antigen (PSMA)-positron emission tomography (PET) is a superior method to predict patients’ risk of cancer progression and response to specific therapies. However, its performance is limited for neuroendocrine prostate cancer (NEPC) and PSMA-low prostate cancer cells, resulting in diagnostic blind spots. Hence, identifying novel specific targets is our aim for diagnosing those prostate cancers with low PSMA expression.
Methods
The Cancer Genome Atlas (TCGA) database and our cohorts from men with biopsy-proven high-risk metastatic prostate cancer were used to identify CDK19 and PSMA expression. PDX lines neP-09 and P-16 primary cells were used for cellular uptake and imaging mass cytometry in vitro. To evaluate in vivo CDK19-specific uptake of gallium(Ga)-68-IRM-015-DOTA, xenograft mice models and blocking assays were used. PET/CT imaging data were obtained to estimate the absorbed dose in organs.
Results
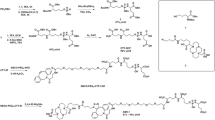
Our study group had reported the overexpression of a novel tissue-specific gene CDK19 in high-risk metastatic prostate cancer and CDK19 expression correlated with metastatic status and tumor staging, independently with PSMA and PSA levels. Following up on this new candidate for use in diagnostics, small molecules targeting CDK19 labeled with Ga-68 (68Ga-IRM-015-DOTA) were used for PET in this study. We found that the 68Ga-IRM-015-DOTA was specificity for prostate cancer cells, but the other cancer cells also took up little 68Ga-IRM-015-DOTA. Importantly, mouse imaging data showed that the NEPC and CRPC xenografts exhibited similar signal strength with 68Ga-IRM-015-DOTA, but 68Ga-PSMA-11 only stained the CRPC xenografts. Furthermore, target specificity was elucidated by a blocking experiment on a CDK19-bearing tumor xenograft. These data concluded that 68Ga-CDK19 PET/CT was an effective technology to detect lesions with or without PSMA in vitro, in vivo, and in the PDX model.
Conclusion
Thus, we have generated a novel PET small molecule with predictive value for prostate cancer. The findings indicate that 68Ga-CDK19 may merit further evaluation as a predictive biomarker for PET scans in prospective cohorts and may facilitate the identification of molecular types of prostate cancer independent of PSMA.
Graphical abstract








Similar content being viewed by others
Data availability
All data that support the findings of this study are available from the corresponding authors upon reasonable request.
Abbreviations
- AUC:
-
Area under the curve
- CRPC:
-
Castration-resistant prostate cancer
- CT:
-
Computed tomography
- mPCa:
-
Metastatic prostate cancer
- NEPC:
-
Neuroendocrine prostate cancer
- PCR:
-
Polymerase chain reaction
- PET:
-
Positron emission tomography
- qPCR:
-
Quantitative real-time PCR
- RT:
-
Radiotherapy
References
Sayegh N, Swami U, Agarwal N. Recent advances in the management of metastatic prostate cancer. JCO Oncol Pract. 2022;18:45–55. https://doi.org/10.1200/OP.21.00206.
Sathekge M, Bruchertseifer F, Vorster M, Lawal IO, Knoesen O, Mahapane J, et al. mCRPC patients receiving (225)Ac-PSMA-617 therapy in the post-androgen deprivation therapy setting: response to treatment and survival analysis. J Nucl Med. 2022;63:1496–502. https://doi.org/10.2967/jnumed.121.263618.
Violet J, Jackson P, Ferdinandus J, Sandhu S, Akhurst T, Iravani A, et al. Dosimetry of (177)Lu-PSMA-617 in metastatic castration-resistant prostate cancer: correlations between pretherapeutic imaging and whole-body tumor dosimetry with treatment outcomes. J Nucl Med. 2019;60:517–23. https://doi.org/10.2967/jnumed.118.219352.
Kuten J, Fahoum I, Savin Z, Shamni O, Gitstein G, Hershkovitz D, et al. Head-to-head comparison of (68)Ga-PSMA-11 with (18)F-PSMA-1007 PET/CT in staging prostate cancer using histopathology and immunohistochemical analysis as a reference standard. J Nucl Med. 2020;61:527–32. https://doi.org/10.2967/jnumed.119.234187.
Lee SC, Ma JSY, Kim MS, Laborda E, Choi SH, Hampton EN, et al. A PSMA-targeted bispecific antibody for prostate cancer driven by a smallmolecule targeting ligand. Sci Adv. 2021;7(33):eabi8193. https://doi.org/10.1126/sciadv.abi8193.
Gillessen S, Armstrong A, Attard G, Beer TM, Beltran H, Bjartell A, et al. Management of patients with advanced prostate cancer: report from the Advanced Prostate Cancer Consensus Conference 2021. Eur Urol. 2022;82:115–41. https://doi.org/10.1016/j.eururo.2022.04.002.
Farolfi A, Calderoni L, Mattana F, Mei R, Telo S, Fanti S, et al. Current and emerging clinical applications of PSMA PET diagnostic imaging for prostate cancer. J Nucl Med. 2021;62:596–604. https://doi.org/10.2967/jnumed.120.257238.
Paschalis A, Sheehan B, Riisnaes R, Rodrigues DN, Gurel B, Bertan C, et al. Prostate-specific membrane antigen heterogeneity and DNA repair defects in Prostate Cancer. Eur Urol. 2019;76:469–78. https://doi.org/10.1016/j.eururo.2019.06.030.
Perera M, Papa N, Roberts M, Williams M, Udovicich C, Vela I, et al. Gallium-68 prostate-specific membrane antigen positron emission tomography in advanced prostate cancer-updated diagnostic utility, sensitivity, specificity, and distribution of prostate-specific membrane antigen-avid lesions: a systematic review and meta-analysis. Eur Urol. 2020;77:403–17. https://doi.org/10.1016/j.eururo.2019.01.049.
Fendler WP, Calais J, Eiber M, Flavell RR, Mishoe A, Feng FY, et al. Assessment of 68Ga-PSMA-11 PET accuracy in localizing recurrent prostate cancer: a prospective single-arm clinical trial. JAMA Oncol. 2019;5:856–63. https://doi.org/10.1001/jamaoncol.2019.0096.
Bakht MK, Derecichei I, Li Y, Ferraiuolo RM, Dunning M, Oh SW, et al. Neuroendocrine differentiation of prostate cancer leads to PSMA suppression. Endocr Relat Cancer. 2018;26:131–46. https://doi.org/10.1530/ERC-18-0226.
Zacherl MJ, Gildehaus FJ, Mittlmeier L, Boning G, Gosewisch A, Wenter V, et al. First clinical results for PSMA-targeted alpha-therapy using (225)Ac-PSMA-I&T in advanced-mCRPC patients. J Nucl Med. 2021;62:669–74. https://doi.org/10.2967/jnumed.120.251017.
Korsen JA, Kalidindi TM, Khitrov S, Samuels ZV, Chakraborty G, Gutierrez JA, et al. Molecular imaging of neuroendocrine prostate cancer by targeting delta-like ligand 3. J Nucl Med. 2022;63:1401–7. https://doi.org/10.2967/jnumed.121.263221.
Davies AH, Beltran H, Zoubeidi A. Cellular plasticity and the neuroendocrine phenotype in prostate cancer. Nat Rev Urol. 2018;15:271–86. https://doi.org/10.1038/nrurol.2018.22.
Fine SW. Neuroendocrine tumors of the prostate. Mod Pathol. 2018;31:S122–32. https://doi.org/10.1038/modpathol.2017.164.
Bakht MK, Hayward JJ, Shahbazi-Raz F, Skubal M, Tamura R, Stringer KF, et al. Identification of alternative protein targets of glutamate-ureido-lysine associated with PSMA tracer uptake in prostate cancer cells. Proc Natl Acad Sci U S A. 2022;119. https://doi.org/10.1073/pnas.2025710119.
Bilinski P, Webb M. An exceptional response to (177)LuPSMA undermined by neuroendocrine transformation. Urol Case Rep. 2021;34:101467. https://doi.org/10.1016/j.eucr.2020.101467.
Vargas Ahumada J, González Rueda SD, Sinisterra Solís FA, Pitalúa Cortés Q, Torres Agredo LP, Miguel JR, et al. Multitarget molecular imaging in metastatic castration resistant adenocarcinoma prostate cancer with therapy induced neuroendocrine differentiation. Diagnostics (Basel). 2022;12(6):1387. https://doi.org/10.3390/diagnostics12061387.
Bragelmann J, Klumper N, Offermann A, von Massenhausen A, Bohm D, Deng M, et al. Pan-cancer analysis of the mediator complex transcriptome identifies CDK19 and CDK8 as therapeutic targets in advanced prostate cancer. Clin Cancer Res. 2017;23:1829–40. https://doi.org/10.1158/1078-0432.CCR-16-0094.
Pelish HE, Liau BB, Nitulescu II, Tangpeerachaikul A, Poss ZC, Da Silva DH, et al. Mediator kinase inhibition further activates super-enhancer-associated genes in AML. Nature. 2015;526(7572):273–6. https://doi.org/10.1038/nature14904.
Serrao A, Jenkins LM, Chumanevich AA, Horst B, Liang J, Gatza ML, et al. Mediator kinase CDK8/CDK19 drives YAP1-dependent BMP4-induced EMT in cancer. Oncogene. 2018;37:4792–808. https://doi.org/10.1038/s41388-018-0316-y.
Steinparzer I, Sedlyarov V, Rubin JD, Eislmayr K, Galbraith MD, Levandowski CB, et al. Transcriptional responses to IFN-gamma require mediator kinase-dependent pause release and mechanistically distinct CDK8 and CDK19 functions. Mol Cell. 2019;76:485–99 e8. https://doi.org/10.1016/j.molcel.2019.07.034.
Kuuluvainen E, Domenech-Moreno E, Niemela EH, Makela TP. Depletion of mediator kinase module subunits represses superenhancer-associated genes in colon cancer cells. Mol Cell Biol. 2018;38. https://doi.org/10.1128/MCB.00573-17.
Fant CB, Taatjes DJ. Regulatory functions of the mediator kinases CDK8 and CDK19. Transcription. 2019;10:76–90. https://doi.org/10.1080/21541264.2018.1556915.
Postlmayr A, Dumeau CE, Wutz A. Cdk8 is required for establishment of H3K27me3 and gene repression by Xist and mouse development. Development. 2020;147. https://doi.org/10.1242/dev.175141.
Zhang Z, Lu Y, Qi Y, Xu Y, Wang S, Chen F, et al. CDK19 regulates the proliferation of hematopoietic stem cells and acute myeloid leukemia cells by suppressing p53-mediated transcription of p21. Leukemia. 2022;36:956–69. https://doi.org/10.1038/s41375-022-01512-5.
Zhao Y, Peng J, Yang J, Zhang E, Huang L, Yang H, et al. Enhancing prostate-cancer-specific MRI by genetic amplified nanoparticle tumor homing. Adv Mater. 2019;31(30):e1900928. https://doi.org/10.1002/adma.201900928.
Wen S, Wei Y, Zen C, Xiong W, Niu Y, Zhao Y. Long non-coding RNA NEAT1 promotes bone metastasis of prostate cancer through N6-methyladenosine. Mol Cancer. 2020;19:171. https://doi.org/10.1186/s12943-020-01293-4.
Becker F, Joerg V, Hupe MC, Roth D, Krupar R, Lubczyk V, et al. Increased mediator complex subunit CDK19 expression associates with aggressive prostate cancer. Int J Cancer. 2020;146(2):577–88. https://doi.org/10.1002/ijc.32551.
Offermann A, Joerg V, Hupe MC, Becker F, Muller M, Bragelmann J, et al. CDK19 as a diagnostic marker for high-grade prostatic intraepithelial neoplasia. Hum Pathol. 2021;117:60–7. https://doi.org/10.1016/j.humpath.2021.07.006.
Batool M, Ahmad B, Choi S. A structure-based drug discovery paradigm. Int J Mol Sci. 2019;20(11):2783. https://doi.org/10.3390/ijms20112783.
Risbridger GP, Clark AK, Porter LH, Toivanen R, Bakshi A, Lister NL, et al. The MURAL collection of prostate cancer patient-derived xenografts enables discovery through preclinical models of uro-oncology. Nat Commun. 2021;12:5049. https://doi.org/10.1038/s41467-021-25175-5.
Poore GD, Kopylova E, Zhu Q, Carpenter C, Fraraccio S, Wandro S, et al. Microbiome analyses of blood and tissues suggest cancer diagnostic approach. Nature. 2020;579:567–74. https://doi.org/10.1038/s41586-020-2095-1.
Cancer Genome Atlas Research N. The molecular taxonomy of primary prostate cancer. Cell. 2015;163:1011–25. https://doi.org/10.1016/j.cell.2015.10.025.
Gandaglia G, Leni R, Bray F, Fleshner N, Freedland SJ, Kibel A, et al. Epidemiology and prevention of prostate cancer. Eur Urol Oncol. 2021;4:877–92. https://doi.org/10.1016/j.euo.2021.09.006.
Evangelista L, Zattoni F, Cassarino G, Artioli P, Cecchin D, Dal Moro F, et al. PET/MRI in prostate cancer: a systematic review and meta-analysis. Eur J Nucl Med Mol Imaging. 2021;48(3):859–73. https://doi.org/10.1007/s00259-020-05025-0.
Maurer T, Eiber M, Schwaiger M, Gschwend JE. Current use of PSMA-PET in prostate cancer management. Nat Rev Urol. 2016;13(4):226–35. https://doi.org/10.1038/nrurol.2016.26.
Eiber M, Maurer T, Souvatzoglou M, Beer AJ, Ruffani A, Haller B, et al. Evaluation of hybrid (6)(8)Ga-PSMA ligand PET/CT in 248 patients with biochemical recurrence after radical prostatectomy. J Nucl Med. 2015;56:668–74. https://doi.org/10.2967/jnumed.115.154153.
Wang Q, Chen J, Singh S, Xie Z, Qin F, Shi X, et al. Profile of chimeric RNAs and TMPRSS2-ERG e2e4 isoform in neuroendocrine prostate cancer. Cell Biosci. 2022;12:153. https://doi.org/10.1186/s13578-022-00893-5.
Lin BB, Lei HQ, Xiong HY, Fu X, Shi F, Yang XW, et al. MicroRNA-regulated transcriptome analysis identifies four major subtypes with prognostic and therapeutic implications in prostate cancer. Comput Struct Biotechnol J. 2021;19:4941–53. https://doi.org/10.1016/j.csbj.2021.08.046.
Brennen WN, Zhu Y, Coleman IM, Dalrymple SL, Antony L, Patel RA, et al. Resistance to androgen receptor signaling inhibition does not necessitate development of neuroendocrine prostate cancer. JCI Insight. 2021;6. https://doi.org/10.1172/jci.insight.146827.
Grasso CS, Wu YM, Robinson DR, Cao X, Dhanasekaran SM, Khan AP, et al. The mutational landscape of lethal castration-resistant prostate cancer. Nature. 2012;487:239–43. https://doi.org/10.1038/nature11125.
Yang Y, Bai Y, He Y, Zhao Y, Chen J, Ma L, et al. PTEN Loss Promotes intratumoral androgen synthesis and tumor microenvironment remodeling via aberrant activation of RUNX2 in castration-resistant prostate cancer. Clin Cancer Res. 2018;24:834–46. https://doi.org/10.1158/1078-0432.CCR-17-2006.
Cyrta J, Prandi D, Arora A, Hovelson DH, Sboner A, Rodriguez A, et al. Comparative genomics of primary prostate cancer and paired metastases: insights from 12 molecular case studies. J Pathol. 2022;257(3):274–84. https://doi.org/10.1002/path.5887.
Hofman MS, Lawrentschuk N, Francis RJ, Tang C, Vela I, Thomas P, et al. Prostate-specific membrane antigen PET-CT in patients with high-risk prostate cancer before curative-intent surgery or radiotherapy (proPSMA): a prospective, randomised, multicentre study. Lancet. 2020;395:1208–16. https://doi.org/10.1016/S0140-6736(20)30314-7.
Hussain M, Carducci MA, Clarke N, Fenton SE, Fizazi K, Gillessen S, et al. Evolving role of prostate-specific membrane antigen-positron emission tomography in metastatic hormone-sensitive prostate cancer: more questions than answers? J Clin Oncol. 2022;40(26):3011–4. https://doi.org/10.1200/JCO.22.00208.
Yin L, Rao P, Elson P, Wang J, Ittmann M, Heston WD. Role of TMPRSS2-ERG gene fusion in negative regulation of PSMA expression. PLoS ONE. 2011;6:e21319. https://doi.org/10.1371/journal.pone.0021319.
Zhang Z, Chng KR, Lingadahalli S, Chen Z, Liu MH, Do HH, et al. An AR-ERG transcriptional signature defined by long-range chromatin interactomes in prostate cancer cells. Genome Res. 2019;29:223–35. https://doi.org/10.1101/gr.230243.117.
Vazzano JL, Patton A, Tinoco G, Iwenofu OH. Primary intranodal epithelioid hemangioendothelioma with molecular confirmation. Int J Surg Pathol. 2022;30:557–63. https://doi.org/10.1177/10668969211070174.
Acknowledgements
We thank the patients and their families for their altruism in participating in research studies. We thank Dr. Yuanjie Niu for reagents, plasmids, and suggestions about PDXs.
Funding
This work was supported in part by grants from the Non-profit Central Research Institute Fund of Chinese Academy of Medical Sciences (2021-RC310-010 to Y.Z.), the CAMS Innovation Fund for Medical Sciences (2021-I2M-1-060 to Y.Z.).
Author information
Authors and Affiliations
Contributions
DD, TH, YL, SY, YL (Yanli), SW, DL, WH, and WG performed the experiments. JY, SL, and YL performed the synthesis of molecules. DD and ZW performed the PET imaging. YL, JY, and YZ prepared all the figures and wrote the manuscript. DD collected the patients’ samples. YZ, SF, and YL supervised the project. YZ, SF, and YL provided fund for the whole project. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Ethics declarations
All experimental protocols were approved by the Ethics Committee of Tianjin Medical University and performed in accordance with the relevant guidelines and regulations (Ethical approval number: KY2019K036). Written informed consents were obtained from all patients. All animal experiments were approved by the Institutional Animal Care and Use Committee of Tianjin Medical University (Tianjin, China).
Competing interests
DD, JY, TH, YL, WZ, SY, YL (Yanli), WG, DL, WH, YL, and YZ disclosed no relevant relationships. L: Activities related to the present article: grants pending from Hospital; other relationships: disclosed no relevant relationships.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.




Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Dai, D., Yu, J., Huang, T. et al. PET imaging of new target CDK19 in prostate cancer. Eur J Nucl Med Mol Imaging 50, 3452–3464 (2023). https://doi.org/10.1007/s00259-023-06277-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-023-06277-2