Abstract
Purpose
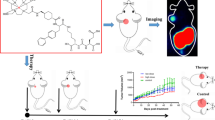
Prostate-specific membrane antigen (PSMA) is highly up-regulated in prostate tumor cells, providing an ideal target for imaging applications of prostate cancer. CTT-1297 (IC50 = 27 nM) is an irreversible phosphoramidate inhibitor of PSMA that has been conjugated to the CB-TE1K1P chelator for incorporation of Cu-64. The resulting positron emission tomography (PET) agent, [64Cu]ABN-1, was evaluated for selective uptake both in vitro and in vivo in PSMA-positive cells of varying expression levels. The focus of this study was to assess the ability of [64Cu]ABN-1 to detect and distinguish varying levels of PSMA in a panel of prostate tumor-bearing mouse models.
Procedures
CTT-1297 was conjugated to the CB-TE1K1P chelator using click chemistry and radiolabeled with Cu-64. Internalization and binding affinity of [64Cu]ABN-1 was evaluated in the following cell lines having varying levels of PSMA expression: LNCaP late-passage > LNCaP early passage ≈ C4-2B > CWR22rv1 and PSMA-negative PC-3 cells. PET/X-ray computed tomography imaging was performed in NCr nude mice with subcutaneous tumors of the variant PSMA-expressing cell lines.
Results
[64Cu]ABN-1 demonstrated excellent uptake in PSMA-positive cells in vitro, with ∼80 % internalization at 4 h for each PSMA-positive cell line with uptake (fmol/mg) correlating to PSMA expression levels. The imaging data indicated significant tumor uptake in all models. The biodistribution for late-passage LNCaP (highest PSMA expression) demonstrated the highest specific uptake of [64Cu]ABN-1 with tumor-to-muscle and tumor-to-blood ratios of 30 ± 11 and 21 ± 7, respectively, at 24 h post-injection. [64Cu]ABN-1 cleared through all tissues except for PSMA-positive kidneys.
Conclusion
[64Cu]ABN-1 demonstrated selective uptake in PSMA-positive cells and tumors, which correlated to the level of PSMA expression. The data reported herein suggest that [64Cu]ABN-1 will selectively target and image variant PSMA expression and in the future will serve as a non-invasive method to follow the progression of prostate cancer in men.




Similar content being viewed by others
References
Chu TC, Shieh F, Lavery LA et al (2006) Labeling tumor cells with fluorescent nanocrystal-aptamer bioconjugates. Biosens Bioelectron 21:1859–1866
Farokhzad OC, Khademhosseini A, Jon S et al (2005) Microfluidic system for studying the interaction of nanoparticles and microparticles with cells. Anal Chem 77:5453–5459
Guilarte TR, McGlothan JL, Foss CA et al (2005) Glutamate carboxypeptidase II levels in rodent brain using [125I]DCIT quantitative autoradiography. Neurosci Lett 387(3):141–144
Humblet V, Lapidus R, Williams LR et al (2005) High-affinity near-infrared fluorescent small-molecule contrast agents for in vivo imaging of prostate-specific membrane antigen. Mol Imaging 4:448–462
Milowsky MI, Nanus DM, Kostakoglu L et al (2007) Vascular targeted therapy with anti-prostate-specific membrane antigen monoclonal antibody J591 in advanced solid tumors. J Clin Oncol 25:540–547
Tsukamoto T, Wozniak KM, Slusher BS (2007) Progress in the discovery and development of glutamate carboxypeptidase II inhibitors. Drug Discov Today 12:767–776
Lapi SE, Wahnishe H, Pham D et al (2009) Assessment of an 18F-labeled phosphoramidate peptidomimetic as a new prostate-specific membrane antigen-targeted imaging agent for prostate cancer. J Nucl Med 50:2042–2048
Nedrow-Byers JR, Jabbes M, Jewett C et al (2012) A phosphoramidate-based prostate-specific membrane antigen-targeted SPECT agent. Prostate 72:904–912
Banerjee SR, Pullambhatla M, Foss CA et al (2014) (6)(4)Cu-labeled inhibitors of prostate-specific membrane antigen for PET imaging of prostate cancer. J Med Chem 57:2657–2669
Lu J, Celis E (2002) Recognition of prostate tumor cells by cytotoxic T lymphocytes specific for prostate-specific membrane antigen. Cancer Res 62(20):5807–5812
Liu T, Wu LY, Berkman CE (2010) Prostate-specific membrane antigen-targeted photodynamic therapy induces rapid cytoskeletal disruption. Cancer Lett 296:106–112
Bander NH, Milowsky MI, Nanus DM et al (2005) Phase I trial of 177lutetium-labeled J591, a monoclonal antibody to prostate-specific membrane antigen, in patients with androgen-independent prostate cancer. J Clin Oncol 23:4591–4601
Milowsky MI, Nanus DM, Kostakoglu L et al (2004) Phase I trial of yttrium-90-labeled anti-prostate-specific membrane antigen monoclonal antibody J591 for androgen-independent prostate cancer. J Clin Oncol 22:2522–2531
Bacich DJ, Pinto JT, Tong WP, Heston WD (2001) Cloning, expression, genomic localization, and enzymatic activities of the mouse homolog of prostate-specific membrane antigen/NAALADase/folate hydrolase. Mamm Genome 12(2):117–123
Zhang L, Wang CY, Yang R et al (2008) Real-time quantitative RT-PCR assay of prostate-specific antigen and prostate-specific membrane antigen in peripheral blood for detection of prostate cancer micrometastasis. Urol Oncol 26:634–640
Perner S, Hofer MD, Kim R et al (2007) Prostate-specific membrane antigen expression as a predictor of prostate cancer progression. Hum Pathol 38:696–701
Bradford TJ, Tomlins SA, Wang X, Chinnaiyan AM (2006) Molecular markers of prostate cancer. Urol Oncol 24:538–551
Evans MJ, Smith-Jones PM, Wongvipat J et al (2011) Noninvasive measurement of androgen receptor signaling with a positron-emitting radiopharmaceutical that targets prostate-specific membrane antigen. Proc Natl Acad Sci U S A 108:9578–9582
Hillier SM, Kern AM, Maresca KP et al (2011) 123I-MIP-1072, a small-molecule inhibitor of prostate-specific membrane antigen, is effective at monitoring tumor response to taxane therapy. J Nucl Med 52:1087–1093
Baum EM, Ernestis, MC, Know HD, et al (2010) Nuclides and isotopes chart of the nuclides. In: Edward Baum. Marine B (ed) Propulsion Corporation, pp 54-55
Rockey WM, Huang L, Kloepping KC et al (2011) Synthesis and radiolabeling of chelator-RNA aptamer bioconjugates with copper-64 for targeted molecular imaging. Bioorg Med Chem 19:4080–4090
Hao G, Kumar A, Dobin T et al (2013) A multivalent approach of imaging probe design to overcome an endogenous anion binding competition for noninvasive assessment of prostate specific membrane antigen. Mol Pharm 10:2975–2985
Liu T, Wu LY, Kazak M, Berkman CE (2008) Cell-Surface labeling and internalization by a fluorescent inhibitor of prostate-specific membrane antigen. Prostate 68:955–964
Nedrow-Byers JR, Jabbes, M., Jewett, C., et al (2011) A phosphoramidate-based prostate-specific membrane antigen-targeted SPECT agent. The Prostate
Nedrow-Byers JR, Moore AL, Ganguly T et al (2013) PSMA-targeted SPECT agents: mode of binding effect on in vitro performance. Prostate 73:355–362
Zeng D, Ouyang Q, Cai Z et al (2014) New cross-bridged cyclam derivative CB-TE1K1P, an improved bifunctional chelator for copper radionuclides. Chem Commun (Camb) 50:43–45
Sprague JE, Peng Y, Sun X et al (2004) Preparation and biological evaluation of copper-64-labeled tyr3-octreotate using a cross-bridged macrocyclic chelator. Clin Cancer Res 10:8674–8682
Wadas TJ, Eiblmaier M, Zheleznyak A et al (2008) Preparation and biological evaluation of 64Cu-CB-TE2A-sst2-ANT, a somatostatin antagonist for PET imaging of somatostatin receptor-positive tumors. J Nucl Med 49:1819–1827
Anderson CJ, Jones LA, Bass LA et al (1998) Radiotherapy, toxicity and dosimetry of copper-64-TETA-octreotide in tumor-bearing rats. J Nucl Med 39:1944–1951
Aggarwal S, Ricklis RM, Williams SA, Denmeade SR (2006) Comparative study of PSMA expression in the prostate of mouse, dog, monkey, and human. Prostate 66:903–910
Gregor PD, Wolchok JD, Turaga V et al (2005) Induction of autoantibodies to syngeneic prostate-specific membrane antigen by xenogeneic vaccination. Int J Cancer 116:415–421
Chen Y, Foss CA, Byun Y et al (2008) Radiohalogenated prostate-specific membrane antigen (PSMA)-based ureas as imaging agents for prostate cancer. J Med Chem 51:7933–7943
Kularatne SA, Wang K, Santhapuram HK, Low PS (2009) Prostate-specific membrane antigen targeted imaging and therapy of prostate cancer using a PSMA inhibitor as a homing ligand. Mol Pharm 6:780–789
Weiner RE, Thakur ML (2005) Radiolabeled peptides in oncology: role in diagnosis and treatment. BioDrugs : Clin Immunother Biopharm Gene Ther 19:145–163
Weiner RE, Thakur ML (2002) Radiolabeled peptides in the diagnosis and therapy of oncological diseases. Appl Radiat Isot 57:749–763
Foss CA, Mease RC, Fan H et al (2005) Radiolabeled small-molecule ligands for prostate-specific membrane antigen: in vivo imaging in experimental models of prostate cancer. Clin Cancer Res 11:4022–4028
Lesche R, Kettschau G, Gromov AV et al (2014) Preclinical evaluation of BAY 1075553, a novel (18)F-labelled inhibitor of prostate-specific membrane antigen for PET imaging of prostate cancer. Eur J Nucl Med Mol Imaging 41:89–101
Liu AY, Brubaker KD, Goo YA et al (2004) Lineage relationship between LNCaP and LNCaP-derived prostate cancer cell lines. Prostate 60:98–108
Liu H, Rajasekaran AK, Moy P et al (1998) Constitutive and antibody-induced internalization of prostate-specific membrane antigen. Cancer Res 58:4055–4060
Ganguly T, Dannoon S, Hopkins MR, et al (2015) A high-affinity [F]-labeled phosphoramidate peptidomimetic PSMA-targeted inhibitor for PET imaging of prostate cancer. Nucl Med Biol
Banerjee SR, Foss CA, Castanares M et al (2008) Synthesis and evaluation of technetium-99m- and rhenium-labeled inhibitors of the prostate-specific membrane antigen (PSMA). J Med Chem 51:4504–4517
Ray Banerjee S, Pullambhatla M, Foss CA et al (2013) Effect of chelators on the pharmacokinetics of (99m)Tc-labeled imaging agents for the prostate-specific membrane antigen (PSMA). J Med Chem 56:6108–6121
Muller C, Struthers H, Winiger C et al (2013) DOTA conjugate with an albumin-binding entity enables the first folic acid-targeted 177Lu-radionuclide tumor therapy in mice. J Nucl Med 54:124–131
Acknowledgments
This research was supported by NIH/NCI (R01CA140617) and Department of Energy/NIBIB, DE-SC0008833. UPCI shared resources (In Vivo Imaging Facility and Biostatistics) were used in this research and supported in part by NCI P30CA047904.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Dr. Berkman is the inventor on issued patents related to PSMA inhibitors described in this report and presently also serves as the CSO of Cancer Targeted Technology.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 9492 kb)
Rights and permissions
About this article
Cite this article
Nedrow, J.R., Latoche, J.D., Day, K.E. et al. Targeting PSMA with a Cu-64 Labeled Phosphoramidate Inhibitor for PET/CT Imaging of Variant PSMA-Expressing Xenografts in Mouse Models of Prostate Cancer. Mol Imaging Biol 18, 402–410 (2016). https://doi.org/10.1007/s11307-015-0908-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11307-015-0908-7