Abstract
Purpose
Deep learning (DL) models have been shown to outperform total perfusion deficit (TPD) quantification in predicting obstructive coronary artery disease (CAD) from myocardial perfusion imaging (MPI). However, previously published methods have depended on polar maps, required manual correction, and normal database. In this study, we propose a polar map-free 3D DL algorithm to predict obstructive disease.
Methods
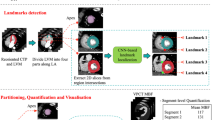
We included 1861 subjects who underwent MPI using cadmium-zinc-telluride camera and subsequent coronary angiography. The subjects were divided into parameterization and external validation groups. We implemented a fully automatic algorithm to segment myocardium, perform registration, and apply normalization. We further flattened the image based on spherical coordinate system transformation. The proposed model consisted of a component to predict patent arteries and a component to predict disease in each vessel. The model was cross-validated in the parameterization group, and then further tested using the external validation group. The performance was assessed by area under receiver operating characteristic curves (AUCs) and compared with TPD.
Results
Our algorithm preprocessed all images accurately as confirmed by visual inspection. In patient-based analysis, the AUC of the proposed model was significantly higher than that for stress-TPD (0.84 vs 0.76, p < 0.01). In vessel-based analysis, the proposed model also outperformed regional stress-TPD (AUC = 0.80 vs 0.72, p < 0.01). The addition of quantitative images did not improve the performance.
Conclusions
Our proposed polar map-free 3D DL algorithm to predict obstructive CAD from MPI outperformed TPD and did not require manual correction or a normal database.







Similar content being viewed by others
Data availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Hsu PY, Lee WJ, Cheng MF, Yen RF, Tzen KY, Wu YW. The incremental diagnostic performance of coronary computed tomography angiography added to myocardial perfusion imaging in patients with intermediate-to-high cardiovascular risk. Acta Cardiol Sin. 2016;32:145–55. https://doi.org/10.6515/acs20150707a.
Liu CJ, Wu YW, Ko KY, Chen YC, Cheng MF, Yen RF, et al. Incremental diagnostic performance of combined parameters in the detection of severe coronary artery disease using exercise gated myocardial perfusion imaging. PLoS ONE. 2015;10:e0134485. https://doi.org/10.1371/journal.pone.0134485.
Hachamovitch R, Rozanski A, Shaw LJ, Stone GW, Thomson LE, Friedman JD, et al. Impact of ischaemia and scar on the therapeutic benefit derived from myocardial revascularization vs. medical therapy among patients undergoing stress-rest myocardial perfusion scintigraphy. Eur Heart J. 2011;32:1012–24. https://doi.org/10.1093/eurheartj/ehq500.
Nudi F, Di Belardino N, Versaci F, Pinto A, Procaccini E, Neri G, et al. Impact of coronary revascularization vs medical therapy on ischemia among stable patients with or suspected coronary artery disease undergoing serial myocardial perfusion scintigraphy. J Nucl Cardiol. 2017;24:1690–8. https://doi.org/10.1007/s12350-016-0504-5.
Engbers EM, Timmer JR, Mouden M, Knollema S, Jager PL, Ottervanger JP. Prognostic value of myocardial perfusion imaging with a cadmium-zinc-telluride SPECT camera in patients suspected of having coronary artery disease. J Nucl Med. 2017;58:1459–63. https://doi.org/10.2967/jnumed.116.188516.
Knuuti J, Wijns W, Saraste A, Capodanno D, Barbato E, Funck-Brentano C, et al. 2019 ESC guidelines for the diagnosis and management of chronic coronary syndromes. Eur Heart J. 2020;41:407–77. https://doi.org/10.1093/eurheartj/ehz425.
Yamagishi M, Tamaki N, Akasaka T, Ikeda T, Ueshima K, Uemura S, et al. JCS 2018 guideline on diagnosis of chronic coronary heart diseases. Circ J. 2021;85:402–572. https://doi.org/10.1253/circj.CJ-19-1131.
Fihn SD, Blankenship JC, Alexander KP, Bittl JA, Byrne JG, Fletcher BJ, et al. 2014 ACC/AHA/AATS/PCNA/SCAI/STS focused update of the guideline for the diagnosis and management of patients with stable ischemic heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines, and the American Association for Thoracic Surgery, Preventive Cardiovascular Nurses Association, Society for Cardiovascular Angiography and Interventions, and Society of Thoracic Surgeons. J Am Coll Cardiol. 2014;64:1929–49. https://doi.org/10.1016/j.jacc.2014.07.017.
Nudi F, Iskandrian AE, Schillaci O, Peruzzi M, Frati G, Biondi-Zoccai G. Diagnostic accuracy of myocardial perfusion imaging with CZT technology: systemic review and meta-analysis of comparison with invasive coronary angiography. JACC Cardiovasc Imaging. 2017;10:787–94. https://doi.org/10.1016/j.jcmg.2016.10.023.
Agostini D, Marie PY, Ben-Haim S, Rouzet F, Songy B, Giordano A, et al. Performance of cardiac cadmium-zinc-telluride gamma camera imaging in coronary artery disease: a review from the cardiovascular committee of the European Association of Nuclear Medicine (EANM). Eur J Nucl Med Mol Imaging. 2016;43:2423–32. https://doi.org/10.1007/s00259-016-3467-5.
Ko CL, Wu YW, Cheng MF, Yen RF, Wu WC, Tzen KY. Data-driven respiratory motion tracking and compensation in CZT cameras: a comprehensive analysis of phantom and human images. J Nucl Cardiol. 2015;22:308–18. https://doi.org/10.1007/s12350-014-9963-8.
Ko KY, Wu YW, Liu CJ, Cheng MF, Yen RF, Tzen KY. Clinical significance of right ventricular activity on treadmill thallium-201 myocardial single-photon emission computerized tomography using cadmium-zinc-telluride cameras. Nucl Med Commun. 2016;37:650–7. https://doi.org/10.1097/mnm.0000000000000494.
Tsai SY, Wang SY, Shiau YC, Wu YW. Mechanical dyssynchrony and diastolic dysfunction are common in LVH: a pilot correlation study using Doppler echocardiography and CZT gated-SPECT MPI. Sci Rep. 2018;8:4182. https://doi.org/10.1038/s41598-018-22213-z.
Liu FS, Wang SY, Shiau YC, Wu YW. The clinical value and safety of ECG-gated dipyridamole myocardial perfusion imaging in patients with aortic stenosis. Sci Rep. 2019;9:12443. https://doi.org/10.1038/s41598-019-48901-y.
Lin WL, Wang SY, Shiau YC, Wu YW. The clinical usefulness of phase analysis in detecting coronary artery disease using dipyridamole thallium-201-gated myocardial perfusion imaging with a cadmium-zinc-telluride camera. J Nucl Cardiol. 2020;27:241–50. https://doi.org/10.1007/s12350-018-1417-2.
Oddstig J, Martinsson E, Jögi J, Engblom H, Hindorf C. Differences in attenuation pattern in myocardial SPECT between CZT and conventional gamma cameras. J Nucl Cardiol. 2019;26:1984–91. https://doi.org/10.1007/s12350-018-1296-6.
Arsanjani R, Dey D, Khachatryan T, Shalev A, Hayes SW, Fish M, et al. Prediction of revascularization after myocardial perfusion SPECT by machine learning in a large population. J Nucl Cardiol. 2015;22:877–84. https://doi.org/10.1007/s12350-014-0027-x.
Nakajima K, Kudo T, Nakata T, Kiso K, Kasai T, Taniguchi Y, et al. Diagnostic accuracy of an artificial neural network compared with statistical quantitation of myocardial perfusion images: a Japanese multicenter study. Eur J Nucl Med Mol Imaging. 2017;44:2280–9. https://doi.org/10.1007/s00259-017-3834-x.
Betancur J, Otaki Y, Motwani M, Fish MB, Lemley M, Dey D, et al. Prognostic value of combined clinical and myocardial perfusion imaging data using machine learning. JACC Cardiovasc Imaging. 2018;11:1000–9. https://doi.org/10.1016/j.jcmg.2017.07.024.
Betancur J, Commandeur F, Motlagh M, Sharir T, Einstein AJ, Bokhari S, et al. Deep learning for prediction of obstructive disease from fast myocardial perfusion SPECT: a multicenter study. JACC Cardiovasc Imaging. 2018;11:1654–63. https://doi.org/10.1016/j.jcmg.2018.01.020.
Betancur J, Hu LH, Commandeur F, Sharir T, Einstein AJ, Fish MB, et al. Deep learning analysis of upright-supine high-efficiency SPECT myocardial perfusion imaging for prediction of obstructive coronary artery disease: a multicenter study. J Nucl Med. 2019;60:664–70. https://doi.org/10.2967/jnumed.118.213538.
Ronneberger O, Fischer P, Brox T. U-Net: convolutional networks for biomedical image segmentation. Cham: Springer International Publishing; 2015. p. 234–41.
Slomka PJ, Nishina H, Berman DS, Akincioglu C, Abidov A, Friedman JD, et al. Automated quantification of myocardial perfusion SPECT using simplified normal limits. J Nucl Cardiol. 2005;12:66–77. https://doi.org/10.1016/j.nuclcard.2004.10.006.
Cerqueira MD, Weissman NJ, Dilsizian V, Jacobs AK, Kaul S, Laskey WK, et al. Standardized myocardial segmentation and nomenclature for tomographic imaging of the heart. A statement for healthcare professionals from the Cardiac Imaging Committee of the Council on Clinical Cardiology of the American Heart Association. Circulation. 2002;105:539–42. https://doi.org/10.1161/hc0402.102975.
Zhao C, Han J, Jia Y. 3D inception convolutional neural networks for automatic lung nodule detection. In: 2017 international conference on computational science and computational intelligence (CSCI); 2017. p. 1649–53.
Ioffe S, Szegedy C. Batch normalization: accelerating deep network training by reducing internal covariate shift. Proceedings of the 32nd international conference on international conference on machine learning - volume 37. Lille, France: JMLR.org; 2015. p. 448–56.
Szegedy C, Ioffe S, Vanhoucke V, Alemi AA. Inception-v4, inception-ResNet and the impact of residual connections on learning. In: Proceedings of the thirty-first AAAI conference on artificial intelligence. San Francisco, California, USA: AAAI Press; 2017. p. 4278–84.
Molinaro AM, Simon R, Pfeiffer RM. Prediction error estimation: a comparison of resampling methods. Bioinformatics. 2005;21:3301–7. https://doi.org/10.1093/bioinformatics/bti499.
Bleeker SE, Moll HA, Steyerberg EW, Donders AR, Derksen-Lubsen G, Grobbee DE, et al. External validation is necessary in prediction research: a clinical example. J Clin Epidemiol. 2003;56:826–32. https://doi.org/10.1016/s0895-4356(03)00207-5.
Juarez-Orozco LE, Knol RJJ, Sanchez-Catasus CA, Martinez-Manzanera O, van der Zant FM, Knuuti J. Machine learning in the integration of simple variables for identifying patients with myocardial ischemia. J Nucl Cardiol. 2020;27:147–55. https://doi.org/10.1007/s12350-018-1304-x.
Shibutani T, Nakajima K, Wakabayashi H, Mori H, Matsuo S, Yoneyama H, et al. Accuracy of an artificial neural network for detecting a regional abnormality in myocardial perfusion SPECT. Ann Nucl Med. 2019;33:86–92. https://doi.org/10.1007/s12149-018-1306-4.
Liu H, Wu J, Miller EJ, Liu C, Yaqiang, Liu, et al. Diagnostic accuracy of stress-only myocardial perfusion SPECT improved by deep learning. Eur J Nucl Med Mol Imaging. 2021;48:2793-2800. https://doi.org/10.1007/s00259-021-05202-9.
Slomka PJ, Betancur J, Liang JX, Otaki Y, Hu LH, Sharir T, et al. Rationale and design of the REgistry of Fast Myocardial Perfusion Imaging with NExt generation SPECT (REFINE SPECT). J Nucl Cardiol. 2020;27:1010–21. https://doi.org/10.1007/s12350-018-1326-4.
Kim J, Jung W, Kim H, Lee J. CyCNN: a rotation invariant CNN using polar mapping and cylindrical convolution layers. arXiv:2007.10588[cs.CV]. https://doi.org/10.48550/arXiv.2007.10588
Funding
This study was partly supported by grants MOST107-2314-B-418-006-MY3 and 108-2314-B-418-002-MY3 from the Ministry of Science and Technology of Taiwan and FEMH107-2314-B-418-006-MY3 and 108-2314-B-418-002-MY3 from Far Eastern Memorial Hospital. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation and data collection were performed by Chi-Lun Ko, Kuan-Yin Ko, and Mei-Fang Cheng. Algorithm design, model training, and data analysis were performed by Chung-Ming Chen, Yen-Wen Wu, Chi-Lun Ko, Shau-Syuan Lin, Cheng-Wen Huang, and Yu-Hui Chang. The first draft of the manuscript was written by Chi-Lun Ko and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics approval
An informed consent waiver was granted by the National Taiwan University Hospital Institutional Review Board for this retrospective analysis.
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Advanced Image Analyses (Radiomics and Artificial Intelligence)
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ko, CL., Lin, SS., Huang, CW. et al. Polar map-free 3D deep learning algorithm to predict obstructive coronary artery disease with myocardial perfusion CZT-SPECT. Eur J Nucl Med Mol Imaging 50, 376–386 (2023). https://doi.org/10.1007/s00259-022-05953-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-022-05953-z