Abstract
Purpose
Develop a 64Cu labeled radiopharmaceutical targeting prostate specific membrane antigen (PSMA) and investigate its application for prostate cancer imaging.
Methods
64Cu-PSMA-BCH was prepared and investigated for stability, PSMA specificity, and micro-PET imaging. With the approval of Ethics Committee of Beijing Cancer Hospital (No. 2017KT97), PET/CT imaging in 4 patients with suspected prostate cancer was performed and the radiation dosimetry was estimated. Then, PSMA PET-ultrasound image-guided biopsies were performed on 3 patients and the fine needle aspirates were further performed for autoradiography and immunohistochemistry analysis.
Results
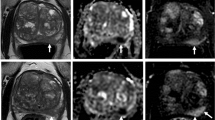
64Cu-PSMA-BCH was prepared with high radiochemical yield and stability. In vivo study showed higher uptake in PSMA ( +) 22Rv1 cells than PSMA ( −) PC-3 cells (5.59 ± 0.36 and 1.97 ± 0.22 IA%/106 cells at 1 h). It accumulated in 22Rv1 tumor with increasing radioactivity uptake and T/N ratios from 1 to 24 h post-injection. In patients with suspected prostate cancer, SUVmax and T/N ratios increased within 24 h post-injection. Compared with image at 1 h post-injection, more tumor lesions were detected at 6 h and 24 h post-injection. The human organ radiation dosimetry showed gallbladder wall was most critical, liver and kidneys were followed, and the whole-body effective dose was 0.0292 mSv/MBq. Two fine needle aspirates obtained by PET-ultrasound-guided targeted biopsy showed high radioactive signal by autoradiography, with 100% PSMA expression in cytoplasm and 30% expression in nucleus.
Conclusion
64Cu-PSMA-BCH was PSMA specific and showed high stability in vivo with lower uptake in liver than 64Cu-PSMA-617. Biodistribution in mice and PCa patients showed similar profile compared with other PSMA ligands and it was safe with moderate effective dosimetry. The increased tumor uptake and T/N ratios by delayed imaging may facilitate the detection of small lesions and guiding targeted biopsies.





Similar content being viewed by others
References
Perera M, Papa N, Christidis D, Wetherell D, Hofman MS, Murphy DG, et al. Sensitivity, specificity, and predictors of positive 68Ga-prostate-specific membrane antigen positron emission tomography in advanced prostate cancer: a systematic review and meta-analysis. Eur Urol. 2016;70(6):926–37. https://doi.org/10.1016/j.eururo.2016.06.021.
Fendler WP, Schmidt DF, Wenter V, Thierfelder KM, Zach C, Stief C, et al. 68Ga-PSMA PET/CT detects the location and extent of primary prostate cancer. J Nucl Med. 2016;57(11):1720–5. https://doi.org/10.2967/jnumed.116.172627.
Liu C, Liu T, Zhang Z, Zhang N, Du P, Yang Y, et al. PSMA PET/CT and standard plus PET/CT-ultrasound fusion targeted prostate biopsy can diagnose clinically significant prostate cancer in men with previous negative biopsies. J Nucl Med. 2020;61(9):1314–9. https://doi.org/10.2967/jnumed.119.235333.
Xie Q, Zhu H, Wang F, Meng X, Ren Q, Xia C, et al. Establishing reliable Cu-64 production process: from target plating to molecular specific tumor micro-PET imaging. Molecules. 2017;22(4):641–50. https://doi.org/10.3390/molecules22040641.
Cui C, Hanyu M, Hatori A, Zhang Y, Xie L, Ohya T, et al. Synthesis and evaluation of [64Cu]PSMA-617 targeted for prostate-specific membrane antigen in prostate cancer. Am J Nucl Med Mol Imaging. 2017;7(2):40–52.
Cantiello F, Gangemi V, Cascini GL, Calabria F, Moschini M, Ferro M, et al. Diagnostic accuracy of 64copper prostate-specific membrane antigen positron emission tomography/computed tomography for primary lymph node staging of intermediate-to high-risk prostate cancer: our preliminary experience. Urology. 2017;106:139–45. https://doi.org/10.1016/j.urology.2017.04.019.
Han XD, Liu C, Liu F, Xie QH, Liu TL, Guo XY, et al. 64Cu-PSMA-617: a novel PSMA-targeted radio-tracer for PET imaging in gastric adenocarcinoma xenografted mice model. Oncotarget. 2017;8(43):74159–69. https://doi.org/10.18632/oncotarget.18276.
Grubmüller B, Baum RP, Capasso E, Singh A, Ahmadi Y, Knoll P, et al. 64Cu-PSMA-617 PET/CT imaging of prostate adenocarcinoma: first in-human studies. Cancer Biother Radiopharm. 2016;31(8):277–86.
Hoberuck S, Wunderlich G, Michler E, Holscher T, Walther M, Seppelt D, et al. Dual-time-point 64Cu-PSMA-617-PET/CT in patients suffering from prostate cancer. J Labelled Comp Radiopharm. 2019;62(8):523–32. https://doi.org/10.1002/jlcr.3745.
Wong P, Lin L, Chea J, Delgado MK, Crow D, Poku E, et al. PET imaging of 64Cu-DOTA-scFv-anti-PSMA lipid nanoparticles (LNPs): enhanced tumor targeting over anti-PSMA scFv or untargeted LNPs. Nucl Med Biol. 2017;47:62–8. https://doi.org/10.1016/j.nucmedbio.2017.01.004.
Dos Santos JC, Beijer B, Bauder-Wust U, Schafer M, Leotta K, Eder M, et al. Development of novel PSMA ligands for imaging and therapy with copper isotopes. J Nucl Med. 2019. https://doi.org/10.2967/jnumed.119.229054.
Boswell CA, Sun X, Niu W, Weisman GR, Wong EH, Rheingold AL, et al. Comparative in vivo stability of copper-64-labeled cross-bridged and conventional tetraazamacrocyclic complexes. J Med Chem. 2004;47(6):1465–74.
Bass LA, Wang M, Welch MJ, Anderson CJ. In vivo transchelation of copper-64 from TETA-octreotide to superoxide dismutase in rat liver. Bioconjug Chem. 2000;11(4):527–32.
Woodin KS, Heroux KJ, Boswell CA, Wong EH, Weisman GR, Niu W, et al. Kinetic inertness and electrochemical behavior of copper(II) tetraazamacrocyclic complexes: possible implications for in vivo stability. Eur J Inorg Chem. 2005;2005(23):4829–33. https://doi.org/10.1002/ejic.200500579.
Ceci F, Fendler W, Eiber M. A new type of prostate cancer imaging: will 64CuCl2 PET/CT flourish or vanish? J Nucl Med. 2018;59(3):442–3. https://doi.org/10.2967/jnumed.117.199885.
Wadas TJ, Wong EH, Weisman GR, Anderson CJ. Coordinating radiometals of copper, gallium, indium, yttrium, and zirconium for PET and SPECT imaging of disease. Chem Rev. 2010;110(5):2858–902.
Ghosh SC, Pinkston KL, Robinson H, Harvey BR, Wilganowski N, Gore K, et al. Comparison of DOTA and NODAGA as chelators for 64Cu-labeled immunoconjugates. Nucl Med Biol. 2015;42(2):177–83. https://doi.org/10.1016/j.nucmedbio.2014.09.009.
Liu T, Liu C, Xu X, Liu F, Guo X, Li N, et al. Preclinical evaluation and pilot clinical study of Al18F-PSMA-BCH for prostate cancer imaging. J Nucl Med. 2019;60:1284–92. https://doi.org/10.2967/jnumed.118.221671.
Eiber M, Herrmann K, Calais J, Hadaschik B, Giesel FL, Hartenbach M, et al. Prostate cancer molecular imaging standardized evaluation (PROMISE): proposed miTNM classification for the interpretation of PSMA-ligand PET/CT. J Nucl Med. 2018;59(3):469–78. https://doi.org/10.2967/jnumed.117.198119.
Qin C, Liu H, Chen K, Hu X, Ma X, Lan X, et al. Theranostics of malignant melanoma with 64CuCl2. J Nucl Med. 2014;55(5):812–7. https://doi.org/10.2967/jnumed.113.133850.
Olszewski RT, Bukhari N, Zhou J, Kozikowski AP, Wroblewski JT, Shamimi-Noori S, et al. NAAG peptidase inhibition reduces locomotor activity and some stereotypes in the PCP model of schizophrenia via group II mGluR. J Neurochem. 2004;89(4):876–85. https://doi.org/10.1111/j.1471-4159.2004.02358.x.
Kunikowska J, Kujda S. 68Ga-PSMA PET/CT in recurrence prostate cancer. Should we perform delayed image in cases of negative 60 minutes postinjection examination? Clin Nucl Med. 2020;45(4):e213–4. https://doi.org/10.1097/rlu.0000000000002966.
Derlin T, Weiberg D, von Klot C, Wester H-J, Henkenberens C, Ross TL, et al. 68Ga-PSMA I&T PET/CT for assessment of prostate cancer: evaluation of image quality after forced diuresis and delayed imaging. Eur Radiol. 2016;26(12):4345–53. https://doi.org/10.1007/s00330-016-4308-4.
Schmuck S, Nordlohne S, von Klot C-A, Henkenberens C, Sohns JM, Christiansen H, et al. Comparison of standard and delayed imaging to improve the detection rate of [68Ga]PSMA I&T PET/CT in patients with biochemical recurrence or prostate-specific antigen persistence after primary therapy for prostate cancer. Eur J Nucl Med Mol Imaging. 2017;44(6):960–8. https://doi.org/10.1007/s00259-017-3669-5.
Barber TW, Singh A, Kulkarni HR, Niepsch K, Billah B, Baum RP. Clinical outcomes of 177Lu-PSMA radioligand therapy in earlier and later phases of metastatic castration-resistant prostate cancer grouped by previous taxane chemotherapy. J Nucl Med. 2019;60(7):955–62. https://doi.org/10.2967/jnumed.118.216820.
Funding
This study was fund by Beijing Natural Science Foundation (Nos. 7194246, 7202028), Science Foundation of Peking University Cancer Hospital 2020–17, Beijing Excellent Talents Funding (2017000021223ZK33), Beijing Millions of Talents Projects A level funding (No. 2019A38), and Municipal Administration of Hospitals-Yangfan Project (ZYLX201816).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Ethical approval
All animal experiments were conducted in accordance with the guidelines approved by Peking University Cancer Hospital Animal Care and Use Committee. All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. The study was approved by Ethics Committee of Beijing Cancer Hospital and Institute (No.2017KT97).
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Radiopharmacy
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Liu, T., Liu, C., Zhang, Z. et al. 64Cu-PSMA-BCH: a new radiotracer for delayed PET imaging of prostate cancer. Eur J Nucl Med Mol Imaging 48, 4508–4516 (2021). https://doi.org/10.1007/s00259-021-05426-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-021-05426-9