Abstract
Purpose
Mild cognitive impairment (MCI) is a transitional pathological stage between normal ageing (NA) and Alzheimer’s disease (AD). Although subjects with MCI show a decline at different rates, some individuals remain stable or even show an improvement in their cognitive level after some years. We assessed the accuracy of FDG PET in discriminating MCI patients who converted to AD from those who did not.
Methods
FDG PET was performed in 42 NA subjects, 27 MCI patients who had not converted to AD at 5 years (nc-MCI; mean follow-up time 7.5 ± 1.5 years), and 95 MCI patients who converted to AD within 5 years (MCI-AD; mean conversion time 1.8 ± 1.1 years). Relative FDG uptake values in 26 meta-volumes of interest were submitted to ANCOVA and support vector machine analyses to evaluate regional differences and discrimination accuracy.
Results
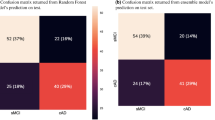
The MCI-AD group showed significantly lower FDG uptake values in the temporoparietal cortex than the other two groups. FDG uptake values in the nc-MCI group were similar to those in the NA group. Support vector machine analysis discriminated nc-MCI from MCI-AD patients with an accuracy of 89% (AUC 0.91), correctly detecting 93% of the nc-MCI patients.
Conclusion
In MCI patients not converting to AD within a minimum follow-up time of 5 years and MCI patients converting within 5 years, baseline FDG PET and volume-based analysis identified those who converted with an accuracy of 89%. However, further analysis is needed in patients with amnestic MCI who convert to a dementia other than AD.



Similar content being viewed by others
References
Davatzikos C, Bhatt P, Shaw LM, Batmanghelich KN, Trojanowski JQ. Prediction of MCI to AD conversion, via MRI, CSF biomarkers, and pattern classification. Neurobiol Aging. 2011;32:2322.e19–e27. doi:10.1016/j.neurobiolaging.2010.05.023.
Landau SM, Harvey D, Madison CM, Reiman EM, Foster NL, Aisen PS, et al. Comparing predictors of conversion and decline in mild cognitive impairment. Neurology. 2010;75:230–8. doi:10.1212/WNL.0b013e3181e8e8b8.
Petersen RC, Roberts RO, Knopman DS, Boeve BF, Geda YE, Ivnik RJ, et al. Mild cognitive impairment: ten years later. Arch Neurol. 2009;66:1447–55. doi:10.1001/archneurol.2009.266.
Pagani M, Dessi B, Morbelli S, Brugnolo A, Salmaso D, Piccini A, et al. MCI patients declining and not-declining at mid-term follow-up: FDG-PET findings. Curr Alzheimer Res. 2010;7:287–94.
Hamel R, Kohler S, Sistermans N, Koene T, Pijnenburg Y, van der Flier W, et al. The trajectory of cognitive decline in the pre-dementia phase in memory clinic visitors: findings from the 4C-MCI study. Psychol Med. 2015;45:1509–19. doi:10.1017/s0033291714002645.
Mitchell AJ, Shiri-Feshki M. Rate of progression of mild cognitive impairment to dementia – meta-analysis of 41 robust inception cohort studies. Acta Psychiatr Scand. 2009;119:252–65. doi:10.1111/j.1600-0447.2008.01326.x.
Barnes DE, Alexopoulos GS, Lopez OL, Williamson JD, Yaffe K. Depressive symptoms, vascular disease, and mild cognitive impairment: findings from the Cardiovascular Health Study. Arch Gen Psychiatry. 2006;63:273–9. doi:10.1001/archpsyc.63.3.273.
Arbizu J, Prieto E, Martinez-Lage P, Marti-Climent JM, Garcia-Granero M, Lamet I, et al. Automated analysis of FDG PET as a tool for single-subject probabilistic prediction and detection of Alzheimer’s disease dementia. Eur J Nucl Med Mol Imaging. 2013;40:1394–405. doi:10.1007/s00259-013-2458-z.
Cuingnet R, Gerardin E, Tessieras J, Auzias G, Lehericy S, Habert MO, et al. Automatic classification of patients with Alzheimer’s disease from structural MRI: a comparison of ten methods using the ADNI database. Neuroimage. 2011;56:766–81. doi:10.1016/j.neuroimage.2010.06.013.
Pagani M, De Carli F, Morbelli S, Oberg J, Chincarini A, Frisoni GB, et al. Volume of interest-based [18F]fluorodeoxyglucose PET discriminates MCI converting to Alzheimer’s disease from healthy controls. A European Alzheimer’s Disease Consortium (EADC) study. Neuroimage Clin. 2015;7:34–42. doi:10.1016/j.nicl.2014.11.007.
Runtti H, Mattila J, van Gils M, Koikkalainen J, Soininen H, Lotjonen J, et al. Quantitative evaluation of disease progression in a longitudinal mild cognitive impairment cohort. J Alzheimers Dis. 2014;39:49–61. doi:10.3233/JAD-130359.
Ardekani BA, Bermudez E, Mubeen AM, Bachman AH; Alzheimer’s Disease Neuroimaging Initiative. Prediction of incipient Alzheimer’s disease dementia in patients with mild cognitive impairment. J Alzheimers Dis. 2017;55:269–81. doi:10.3233/JAD-160594.
Lange C, Suppa P, Frings L, Brenner W, Spies L, Buchert R. Optimization of statistical single subject analysis of brain FDG PET for the prognosis of mild cognitive impairment-to-Alzheimer’s disease conversion. J Alzheimers Dis. 2016;49:945–59. doi:10.3233/JAD-150814.
Lee SH, Bachman AH, Yu D, Lim J, Ardekani BA. Predicting progression from mild cognitive impairment to Alzheimer’s disease using longitudinal callosal atrophy. Alzheimers Dement (Amst). 2016;2:68–74. doi:10.1016/j.dadm.2016.01.003.
Shaffer JL, Petrella JR, Sheldon FC, Choudhury KR, Calhoun VD, Coleman RE, et al. Predicting cognitive decline in subjects at risk for Alzheimer disease by using combined cerebrospinal fluid, MR imaging, and PET biomarkers. Radiology. 2013;266:583–91. doi:10.1148/radiol.12120010.
Liu Y, Mattila J, Ruiz MA, Paajanen T, Koikkalainen J, van Gils M, et al. Predicting AD conversion: comparison between prodromal AD guidelines and computer assisted PredictAD tool. PLoS One. 2013;8:e55246. doi:10.1371/journal.pone.0055246.
Young J, Modat M, Cardoso MJ, Mendelson A, Cash D, Ourselin S, et al. Accurate multimodal probabilistic prediction of conversion to Alzheimer’s disease in patients with mild cognitive impairment. Neuroimage Clin. 2013;2:735–45. doi:10.1016/j.nicl.2013.05.004.
Yu P, Dean RA, Hall SD, Qi Y, Sethuraman G, Willis BA, et al. Enriching amnestic mild cognitive impairment populations for clinical trials: optimal combination of biomarkers to predict conversion to dementia. J Alzheimers Dis. 2012;32:373–85. doi:10.3233/JAD-2012-120832.
Ewers M, Brendel M, Rizk-Jackson A, Rominger A, Bartenstein P, Schuff N, et al. Reduced FDG-PET brain metabolism and executive function predict clinical progression in elderly healthy subjects. Neuroimage Clin. 2014;4:45–52. doi:10.1016/j.nicl.2013.10.018.
Moradi E, Pepe A, Gaser C, Huttunen H, Tohka J. Alzheimer’s disease neuroimaging I. Machine learning framework for early MRI-based Alzheimer’s conversion prediction in MCI subjects. Neuroimage. 2015;104:398–412. doi:10.1016/j.neuroimage.2014.10.002.
Haense C, Buerger K, Kalbe E, Drzezga A, Teipel SJ, Markiewicz P, et al. CSF total and phosphorylated tau protein, regional glucose metabolism and dementia severity in Alzheimer’s disease. Eur J Neurol. 2008;15:1155–62. doi:10.1111/j.1468-1331.2008.02274.x.
Walhovd KB, Fjell AM, Dale AM, McEvoy LK, Brewer J, Karow DS, et al. Multi-modal imaging predicts memory performance in normal aging and cognitive decline. Neurobiol Aging. 2010;31:1107–21. doi:10.1016/j.neurobiolaging.2008.08.013.
Chen K, Ayutyanont N, Langbaum JB, Fleisher AS, Reschke C, Lee W, et al. Characterizing Alzheimer’s disease using a hypometabolic convergence index. Neuroimage. 2011;56:52–60. doi:10.1016/j.neuroimage.2011.01.049.
Ito K, Fukuyama H, Senda M, Ishii K, Maeda K, Yamamoto Y, et al. Prediction of outcomes in mild cognitive impairment by using 18F-FDG-PET: a multicenter study. J Alzheimers Dis. 2015;45:543–52. doi:10.3233/JAD-141338.
Fouquet M, Desgranges B, Landeau B, Duchesnay E, Mezenge F, de la Sayette V, et al. Longitudinal brain metabolic changes from amnestic mild cognitive impairment to Alzheimer’s disease. Brain. 2009;132:2058–67. doi:10.1093/brain/awp132.
Pagani M, Giuliani A, Oberg J, Chincarini A, Morbelli S, Brugnolo A, et al. Predicting the transition from normal aging to Alzheimer’s disease: a statistical mechanistic evaluation of FDG-PET data. Neuroimage. 2016;141:282–90. doi:10.1016/j.neuroimage.2016.07.043.
Pagani M, Giuliani A, Ӧberg J, De Carli F, Morbelli S, Girtler N, et al. Progressive disintegration of brain networking from normal aging to Alzheimer’s Disease. Analysis of Independent Components of 18F-FDG PET Data. J Nucl Med. 2017;58:1132–1139. doi:10.2967/jnumed.116.184309.
Petersen RC, Negash S. Mild cognitive impairment: an overview. CNS Spectr. 2008;13:45–53.
Gorelick PB, Scuteri A, Black SE, Decarli C, Greenberg SM, Iadecola C, et al. Vascular contributions to cognitive impairment and dementia: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2011;42:2672–713. doi:10.1161/STR.0b013e3182299496.
Wahlund LO, Barkhof F, Fazekas F, Bronge L, Augustin M, Sjogren M, et al. A new rating scale for age-related white matter changes applicable to MRI and CT. Stroke. 2001;32:1318–22.
Loeb C, Gandolfo C. Diagnostic evaluation of degenerative and vascular dementia. Stroke. 1983;14:399–401.
Dubois B, Feldman HH, Jacova C, Hampel H, Molinuevo JL, Blennow K, et al. Advancing research diagnostic criteria for Alzheimer’s disease: the IWG-2 criteria. Lancet Neurol. 2014;13:614–29. doi:10.1016/s1474-4422(14)70090-0.
Picco A, Polidori MC, Ferrara M, Cecchetti R, Arnaldi D, Baglioni M, et al. Plasma antioxidants and brain glucose metabolism in elderly subjects with cognitive complaints. Eur J Nucl Med Mol Imaging. 2014;41:764–75. doi:10.1007/s00259-013-2638-x.
Della Rosa PA, Cerami C, Gallivanone F, Prestia A, Caroli A, Castiglioni I, et al. A standardized [18F]-FDG-PET template for spatial normalization in statistical parametric mapping of dementia. Neuroinformatics. 2014;12:575–93. doi:10.1007/s12021-014-9235-4.
Tzourio-Mazoyer N, Landeau B, Papathanassiou D, Crivello F, Etard O, Delcroix N, et al. Automated anatomical labeling of activations in SPM using a macroscopic anatomical parcellation of the MNI MRI single-subject brain. Neuroimage. 2002;15:273–89. doi:10.1006/nimg.2001.0978.
Cortes C, Vapnik V. Support-vector networks. Mach Learn. 1995;20:273–97. doi:10.1007/bf00994018.
Brown LD, Cai TT, DasGupta A. Interval estimation for a binomial proportion. Statist Sci. 2001;16:101–33. doi:10.1214/ss/1009213286.
Qin G, Hotilovac L. Comparison of non-parametric confidence intervals for the area under the ROC curve of a continuous-scale diagnostic test. Stat Methods Med Res. 2008;17:207–21. doi:10.1177/0962280207087173.
Ossenkoppele R, Jansen WJ, Rabinovici GD, Knol DL, van der Flier WM, van Berckel BN, et al. Prevalence of amyloid PET positivity in dementia syndromes: a meta-analysis. JAMA. 2015;313:1939–49. doi:10.1001/jama.2015.4669.
Caroli A, Prestia A, Chen K, Ayutyanont N, Landau SM, Madison CM, et al. Summary metrics to assess Alzheimer disease-related hypometabolic pattern with 18F-FDG PET: head-to-head comparison. J Nucl Med. 2012;53:592–600. doi:10.2967/jnumed.111.094946.
Dukart J, Mueller K, Villringer A, Kherif F, Draganski B, Frackowiak R, et al. Relationship between imaging biomarkers, age, progression and symptom severity in Alzheimer’s disease. Neuroimage Clin. 2013;3:84–94. doi:10.1016/j.nicl.2013.07.005.
Casanova R, Hsu FC, Sink KM, Rapp SR, Williamson JD, Resnick SM, et al. Alzheimer’s disease risk assessment using large-scale machine learning methods. PLoS One. 2013;8:e77949. doi:10.1371/journal.pone.0077949.
Hinrichs C, Singh V, Xu G, Johnson SC. Alzheimers disease neuroimaging I. Predictive markers for AD in a multi-modality framework: an analysis of MCI progression in the ADNI population. Neuroimage. 2011;55:574–89. doi:10.1016/j.neuroimage.2010.10.081.
Ritter K, Schumacher J, Weygandt M, Buchert R, Allefeld C, Haynes JD. Multimodal prediction of conversion to Alzheimer’s disease based on incomplete biomarkers. Alzheimers Dement (Amst). 2015;1:206–15. doi:10.1016/j.dadm.2015.01.006.
Sanchez-Catasus CA, Stormezand GN, van Laar PJ, De Deyn PP, Sanchez MA, Dierckx RA. FDG-PET for prediction of AD dementia in mild cognitive impairment. A review of the state of the art with particular emphasis on the comparison with other neuroimaging modalities (MRI and perfusion SPECT). Curr Alzheimer Res. 2017;14:127–42.
Rizk-Jackson A, Insel P, Petersen R, Aisen P, Jack C, Weiner M. Early indications of future cognitive decline: stable versus declining controls. PLoS One. 2013;8:e74062. doi:10.1371/journal.pone.0074062.
Scola E, Bozzali M, Agosta F, Magnani G, Franceschi M, Sormani MP, et al. A diffusion tensor MRI study of patients with MCI and AD with a 2-year clinical follow-up. J Neurol Neurosurg Psychiatry. 2010;81:798–805. doi:10.1136/jnnp.2009.189639.
Wei R, Li C, Fogelson N, Li L. Prediction of conversion from mild cognitive impairment to Alzheimer’s disease using MRI and structural network features. Front Aging Neurosci. 2016;8:76. doi:10.3389/fnagi.2016.00076.
Schroeter ML, Stein T, Maslowski N, Neumann J. Neural correlates of Alzheimer’s disease and mild cognitive impairment: a systematic and quantitative meta-analysis involving 1351 patients. Neuroimage. 2009;47:1196–206. doi:10.1016/j.neuroimage.2009.05.037.
Teipel SJ, Kurth J, Krause B, Grothe MJ; Alzheimer’s Disease Neuroimaging Initiative. The relative importance of imaging markers for the prediction of Alzheimer’s disease dementia in mild cognitive impairment – beyond classical regression. Neuroimage Clin. 2015;8:583–93. doi:10.1016/j.nicl.2015.05.006.
Brendel M, Reinisch V, Kalinowski E, Levin J, Delker A, Darr S, et al. Hypometabolism in brain of cognitively normal patients with depressive symptoms is accompanied by atrophy-related partial volume effects. Curr Alzheimer Res. 2016;13:475–86.
Seo SW, Cho SS, Park A, Chin J, Na DL. Subcortical vascular versus amnestic mild cognitive impairment: comparison of cerebral glucose metabolism. J Neuroimaging. 2009;19:213–9. doi:10.1111/j.1552-6569.2008.00292.x.
Chen K, Langbaum JB, Fleisher AS, Ayutyanont N, Reschke C, Lee W, et al. Twelve-month metabolic declines in probable Alzheimer’s disease and amnestic mild cognitive impairment assessed using an empirically pre-defined statistical region-of-interest: findings from the Alzheimer’s Disease Neuroimaging Initiative. Neuroimage. 2010;51:654–64. doi:10.1016/j.neuroimage.2010.02.064.
Frisoni GB, Bocchetta M, Chetelat G, Rabinovici GD, de Leon MJ, Kaye J, et al. Imaging markers for Alzheimer disease: which vs how. Neurology. 2013;81:487–500. doi:10.1212/WNL.0b013e31829d86e8.
Garibotto V, Herholz K, Boccardi M, Picco A, Varrone A, Nordberg A, et al. Clinical validity of brain fluorodeoxyglucose positron emission tomography as a biomarker for Alzheimer’s disease in the context of a structured 5-phase development framework. Neurobiol Aging. 2017;52:183–195. doi:10.1016/j.neurobiolaging.2016.03.033
Acknowledgments
The authors thank Ms. Katja Gasperini for helping with the English editing.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Conflicts of interest
None.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the principles of the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards
Rights and permissions
About this article
Cite this article
Pagani, M., Nobili, F., Morbelli, S. et al. Early identification of MCI converting to AD: a FDG PET study. Eur J Nucl Med Mol Imaging 44, 2042–2052 (2017). https://doi.org/10.1007/s00259-017-3761-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-017-3761-x