Abstract
Objective
De-centering of the shoulder joint on radiographs is used as indicator for severity of rotator cuff tears and as predictor for clinical outcome after surgery. The objective of the study was to assess the effect of malrotation on glenohumeral centering on radiographs and to identify the most reliable parameter for its quantification.
Subjects and methods.
In this retrospective study (2014–2018), 249 shoulders were included: 92 with imaging-confirmed supra- and infraspinatus tears (rupture; 65.2 ± 9.9 years) and 157 without tears (control; 41.1 ± 13.0 years). On radiographs in neutral position and external rotation, we assessed three radiographic parameters to quantify glenohumeral centering: acromiohumeral distance (ACHD), craniocaudal distance of the humeral head and glenoid center (Deutsch), and scapulohumeral arch congruity (Moloney). Non-parametric statistics was performed.
Results
In both positions, only the distance parameters ACHD (< 0.5 mm) and Deutsch (< 1 mm) were comparable in the two study groups rupture and control. Comparing the parameters between the study groups revealed only ACHD to be significantly different with a reduction of more than 2 mm in the rupture group. Among the parameters, ACHD ≤ 6 mm was the only cut-off discriminating rupture (12–21% of the shoulders with ACHD ≤ 6 mm) and control (none of the shoulders with ACHD ≤ 6 mm). Ninety percent of shoulders with ACHD ≤ 6 mm presented with a massive rotator cuff tear (defined as ≥ 67% of the greater tuberosity exposed).
Conclusion
Glenohumeral centering assessed by ACHD and Deutsch is not affected by rotation in shoulders with and without rotator cuff tear. An ACHD ≤ 6 mm has a positive predictive value of 90% for a massive rotator cuff tear.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rotator cuff tears of the shoulder often result from an acute intense trauma or a combination of tendon degeneration and repetitive minor trauma [1, 2]. The prevalence is approximately 10% in individuals younger than 20 years and > 60% in individuals older than 80 years [3]. Rotator cuff tears can be debilitating due to restriction of movement and pain. They are often accompanied by cranial migration of the humeral head attributed to the imbalance of the cranializing force of the deltoid muscle and the caudalizing effect of the rotator cuff and the long biceps tendon [4]. De-centering of the glenohumeral joint measured on conventional radiographs has been used as an indicator for the severity of rotator cuff tears and as a prognostic factor for the success of intended surgical approaches [5,6,7]. Therefore, accurate measuring of glenohumeral centering is key when being used for clinical decision-making.
Conventional radiographs of the shoulder are the first line of diagnostic imaging in patients with shoulder pain. Several radiographic parameters are available to address glenohumeral centering: acromiohumeral distance, distance of the center of the humeral head from the center of the glenoid in cranio-caudal direction according to Deutsch [8], and congruity of the scapulohumeral arch [9]. These parameter measurements are based on a two-dimensional projection of a three-dimensional anatomic relation. As such, the measurements are prone to radiographic projection errors or patient-related conditions. The latter is of special importance, since patients may not be able to take the correct positions for diagnostic radiographs due to muscle contractions and pain. It has been recently shown in a cadaver study that malrotation of the shoulder resulted in significant and clinically relevant differences in measurement parameters of the scapula [10]. There is no data available in the literature, however, on the influence of malrotation on the assessment of glenohumeral centering on conventional radiographs. We hypothesized that glenohumeral centering is dependent on the rotation of the humeral head and that this difference is more pronounced in patients with posterosuperior rotator cuff tears since shoulder centering is dependent on an intact rotator cuff. The two objectives of our study were (1) to analyze the influence of malrotation on radiographic projection and (2) to identify the most suitable parameter to measure glenohumeral centering on conventional radiographs in a clinical setting.
Subjects and methods
Study design and patient selection
The study was approved by the institutional review board (2020–01298). All patients included in this study signed a general consent on the usage of health-related data for research purposes.
In this retrospective study, the radiology information system (RIS) of our department was reviewed for patients older than 18 years who received two oblique anteroposterior shoulder radiographs (Grashey view) with both the humerus in neutral position (termed as NEUT) and 45° external rotation (termed as ER) (Fig. 1 a–b) over a period of four and a half years (January 2014 to May 2018) and also received an MRI (magnetic resonance imaging)- or CT (computed tomography)-arthrography within 90 days of the radiographs. A total of 3089 shoulders were identified.
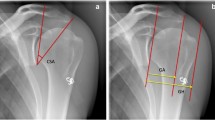
Oblique anteroposterior radiographs of a right shoulder in neutral position (NEUT) and in external rotation (ER). a, b The rotation of the humerus alters the projected shapes of the humeral head and the calcar, influencing the measurements for glenohumeral centering. c Glenohumeral centering was quantified by the acromiohumeral distance (ACHD), by the distance of the center of the humeral head to the center of the glenoid in cranio-caudal direction according to Deutsch, and d by the congruity of the scapulohumeral arch, known as the Moloney line
Study groups
The study comprised two groups: (i) patients with a rotator cuff tear (rupture group), and (ii) patients with an intact rotator cuff (control group). In the rupture group, 92 shoulders were included (65.2 ± 9.9 years), and 157 in the control group (41.1 ± 13.0 years).
The reports of the MRI- or CT-arthrography were screened for exclusion and inclusion criteria as detailed below.
Patient exclusion criteria—rupture and control group
Patients with a prior surgical history of the shoulder (open and arthroscopically), fractures (including Hill-Sachs and osseous Bankart lesions), prior shoulder dislocation, clinical or radiological signs of frozen shoulder, and patients with severe cuff arthropathy (Hamada stages 4 and 5) [11] were excluded from both study groups.
Patient inclusion criteria—rupture group
Reports indicating a rotator cuff tear involving the supra- and infraspinatus tendon, also known as posterosuperior rotator cuff tear, and an intact or a subscapularis tendon tear involving not more than the upper third of the tendon resulted in 121 potential candidates. The MRI- and CT-arthrographies were analyzed for the following parameters: (i) extent of the rotator cuff tear in anteroposterior direction [12] (see below); (ii) tendon retraction according to Patte [13]; (iii) fatty infiltration of the muscle according to Goutallier [14]; and (iv) atrophy of the supraspinatus muscle by the presence of the tangent sign [15]. The extent of the rupture in anteroposterior direction was determined based on the method introduced in a recently published paper, which identified a denominator for the term “massive rotator cuff tear” using the Delphi-method [12]. The quantification is based on the percentage of the greater tuberosity exposed by the teared rotator cuff tendons, measured in the sagittal plane with a value of ≥ 67% defining the cut off for a “massive rotator cuff tear,” while a value below 67% was considered a “non-massive rotator cuff tear.” Based on these criteria, a total of 92 shoulders were included in the rupture group, and of those 65 shoulders (65/92, 71%) presented with a massive rotator cuff tear.
Patient inclusion criteria—control group
MRI or CT were analyzed to confirm an intact rotator cuff. A total of 157 shoulders were included in the control group.
Analysis of the conventional radiographs
Measurements on oblique anteroposterior radiographs of 92 shoulders enrolled in the rupture group and 157 shoulders enrolled in the control group were independently performed by two readers: reader 1 (EW) is a final-year medical student with no previous experience in radiology; reader 2 (RE) is a board certified radiologist with 5-year experience and specializing in musculoskeletal radiology.
Glenohumeral centering was quantified by measuring three parameters (Fig. 1 c–d): (i) acromiohumeral distance (ACHD); (ii) distance of the center of the humeral head to the center of the glenoid in cranio-caudal direction according to Deutsch et al. [8] (in the following termed as Deutsch); and (iii) congruity of the scapulohumeral arch, known as the Moloney line [9] (in the following termed as Moloney). For Deutsch and Moloney, a positive value was given when the humeral head was cranially displaced in relation to the glenoid, a negative value when caudally displaced. Cut-off values based on the measurements of glenohumeral centering were established to discriminate between shoulders with and without a rotator cuff tear. Two different cut-off values were defined for each measurement: (i) the first value must not be reached by any control in both readers; (ii) the second value must not be reached by more than 5% of controls in both readers.
Additionally, the quality of the radiographic projection taken in NEUT position was rated by reader 2. Four radiographic criteria were analyzed for defining an appropriate radiograph, according to the qualitative analysis criteria termed “omometry” [10]: (i) anterior and posterior rim of the glenoid projects as one line; (ii) the coracoid process is in harmony with the superior glenoid rim; (iii) the diameter of the coracoid process is equal or larger than the acromial diameter; and (iv) the diameter of the acromion does not increase towards the acromio-clavicular joint. Each of the four parameters met counted as one point, resulting in a scale from 0 (poor projection) to 4 (optimal projection).
Statistics
SPSS statistics was used for data analysis (IBM SPSS Statistics, Version 26 for Windows). Based on the results of the Kolmogorov–Smirnov test, all statistical analysis was performed with non-parametric tests.
Intraclass correlation (ICC) was calculated to assess interrater reliability. Two-way mixed measures checked for consistency. ICC values of < 0.50 were rated as poor, 0.50–0.75 as moderate, 0.75–0.90 as good, and > 0.90 as excellent [16].
Measures for glenohumeral centering (ACHD, Deutsch, and Moloney) were statistically assessed using the Wilcoxon signed rank test for the comparison of NEUT versus ER, and the Mann–Whitney U test for comparison of control versus rupture. Distribution of gender and side in rupture and control was assessed with non-parametric chi-square tests. Omometry and glenohumeral centering were compared using the Kruskal–Wallis test for non-parametric and independent variables. The correlation of massive rotator cuff tears with different MR-based parameters was done using Fisher’s exact test.
Results
Patient demographics
A total of 249 shoulders were enrolled in the study, 92 in the rupture, and 157 in the control group. The patients in rupture were significantly older compared to control (65.2 ± 9.9 and 41.1 ± 13.0 years, respectively, p < 0.001). There was a significant overrepresentation of males in control, but not in rupture (61.1% (p < 0.01) and 54.3%, respectively). In both groups, right shoulders were significantly overrepresented in rupture (72.8%, p < 0.001) and in control (58.6%, p < 0.05).
Interrater correlation
The interrater correlation of the two readers for ACHD (pooled data from rupture and control) was rated excellent for both projections (NEUT 0.945, ER 0.916). For Deutsch, interrater correlation was rated moderate in NEUT and good in ER (NEUT 0.709, ER 0.782), and for Moloney good in NEUT and moderate in ER (NEUT 0.841, ER 0.737).
Glenohumeral centering in dependence of rotation of the humeral head
Glenohumeral centering assessed by ACHD, Moloney, and Deutsch was significantly different in most comparisons between NEUT and ER projections (Table 1). However, the mean differences for ACHD were < 0.5 mm and for Deutsch < 1 mm for both readers and both groups. The mean differences for Moloney were more pronounced with apparent inferior translation of the humeral head in external rotation by 2.5–3.6 mm.
Omometry and glenohumeral centering
Omometry scores were given to 21.6% (34/157, score 0), 18.5% (29/157, score 1), 24.2% (38/157, score 2), 18.5% (38/157, score 3), and 17.2% (27/157, score 4) of the NEUT projections in controls. A subgroup analysis of glenohumeral centering in dependence of the omometry score did only find a statistically significant difference for Deutsch in reader 1 (p = 0.037). Post hoc analysis after Bonferroni correction for multiple comparisons, however, did not find a statistically significant difference in any comparison, the lowest value calculated between omometry score 1 and 2 (p = 0.085). All other subgroup analyses did not show statistically significant differences for ACHD (p = 0.893 and 0.883 for reader 1 and reader 2, respectively), Deutsch (p = 0.113 for reader 2), and Moloney (p = 0.946 and 0.901 for reader 1 and reader 2, respectively).
Glenohumeral centering in dependence of rotator cuff tear
Most of the measurements for glenohumeral centering indicated a cranial migration of the humeral head in the patients of the rupture group as compared to control in both positions NEUT and ER (Table 1). The mean value of the ACHD in NEUT position of the rupture group was significantly reduced compared to control in both readers by 2.5 and 2.1 mm, respectively. The mean differences in rupture compared to control in NEUT position for Deutsch were − 0.1 mm for reader 1 and 1 mm for reader 2, and for Moloney − 0.4 mm and 1.4 mm, with significant differences only found by reader 2 (Table 1).
Cut-off values based on the measurements of glenohumeral centering were established to discriminate between shoulders with and without a rotator cuff tear (Table 2). Two different cut-off values were defined for each measurement: (i) the first value must not be reached by any control in both readers; (ii) the second value must not be reached by more than 5% of controls in both readers. The cut-off values identified for ACHD were ≤ 6 mm and ≤ 7 mm, for Moloney ≥ 14 mm and ≥ 8 mm, and for Deutsch ≥ 8 mm and ≥ 4 mm, respectively.
The most striking differences were found for ACHD where a consistent significant over-representation of shoulders with rotator cuff tears and a reduced ACHD were measured (Table 2). In particular, 20.7% (19/92) of shoulders with a rotator cuff tear in reader 1 and 12% (11/92) in reader 2 presented with an ACHD ≤ 6 mm, while in none of the controls, an ACHD ≤ 6 mm was measured. The discrimination between shoulders with and without a rotator cuff tear was less evident for the chosen cut-off values for Moloney and Deutsch, with significant differences only for the less stringent values (< 5%) applied.
We adopted a quantitative measure for the size of the rotator cuff tear by assessing the extent of the greater tuberosity that is exposed due to tendon ruptures, with a value of ≥ 67% considered a massive tear [12]. A statistically significant, albeit, weak correlation was found between all three distance parameters and rupture size (Fig. 2). Out of the 92 shoulders from the rupture group, 65 fulfilled the characteristics of a massive tear. Shoulders with a massive rotator cuff tear showed a significantly reduced ACHD and increased Deutsch in both readers as compared to shoulders with a tear not considered to be massive, whereas no significant difference was found for Moloney (Fig. 3 and Table 3).
Correlation of the parameters for glenohumeral centering and the size of rotator cuff tear in patients of the rupture group (data from reader 2). a ACHD, b Deutsch, and c Moloney. Note that due to the measurement definitions, cranial migration of the humeral head manifests with a reduction of ACHD, but with an increased distance for Deutsch and Moloney
Massive rotator cuff tear in the left shoulder of a 56-year old woman. a, b Oblique anteroposterior radiograph in neutral position (NEUT) shows small acromiohumeral distance (ACHD) as indicated by the arrow, with no change in external rotation (ER). c Sagittal T1-weighted MR image depicts a complete tear of the supraspinatus tendon (arrowheads). d Sagittal T1-weighted MR image shows a positive tangent sign of an atrophied supraspinatus muscle; i.e., the muscle does not cross the dotted line connecting the superior border of the coracoid process to the superior border of the scapular spine
We further analyzed whether a specific abnormality of the rotator cuff was associated with a reduced ACHD in shoulders with massive tears (Table 4). Of those 65 shoulders, 17 shoulders of reader 1 (26.2%) and 10 shoulders of reader 2 (15.4%) presented with an ACHD ≤ 6 mm. In the entire study group rupture (see again Table 2), 17 of 19 shoulders with an ACHD ≤ 6 mm (89.5%) in reader 1, and 10 of 11 shoulders (90.9%) in reader 2 had a massive rotator cuff tear. Due to the low number of shoulders with massive rotator cuff tears and a reduced ACHD, retraction according to Patte was dichotomized in two groups (either 0–2 or 3), and fatty infiltration according to Goutallier was also dichotomized in two groups (either 0–2 or 3–4). In both readers, a significant association of the presence of a tangent sign with an ACHD ≤ 6 mm was found. A significant correlation of fatty infiltration of the supraspinatus muscle with a reduced ACHD was established only by reader 1. There was no statistically significant association between patients with a reduced ACHD (≤ 6 mm) for tendon retraction and atrophy of the infraspinatus muscle.
Discussion
Tears of the rotator cuff can result in cranial migration of the humeral head due to muscular imbalance of the cranializing effect of the deltoid muscle and the caudalizing effect of the rotator cuff [4]. The extent of cranial decentering has been used as an indicator for the severity of rotator cuff tears and as a prognostic factor for the success of intended surgical treatment approaches [5,6,7]. Therefore, accurate measuring of glenohumeral centering is key when being used for clinical decision making. In the present study, we compared three different parameters to quantify glenohumeral centering on conventional oblique anteroposterior radiographs (Grashey view) taken in two different positions (neutral and external rotation of the humerus) in patients with and without rotator cuff tears. We showed that glenohumeral centering measured either by ACHD or Deutsch is robust and is independent on shoulder rotation. Comparing shoulders with and without rotator cuff tear revealed that only ACHD can discriminate between those two groups, and that an ACHD ≤ 6 mm reliably predicts a rotator cuff tear.
The interrater correlation was excellent when glenohumeral centering was assessed by ACHD, independent on the rotation of the humerus. The two other parameters, Deutsch und Moloney, presented with lower interrater correlations; however, they were still considered moderate to good. The lower interrater agreement can be explained by the measurement method. While measuring ACHD is based on generally well-identifiable landmarks, the method of Deutsch requires proper identification of the superior and inferior glenoid tubercle, which are often less clearly identifiable on radiographs in cases where the glenoid is not well projected. For Moloney, a continuity of the scapular-humeral arch line needs to be projected, which always leaves some room for interpretation. We further evaluated the effect of the quality of radiographic projection on the parameters of glenohumeral centering using omometry [10]. Since there were no statistically significant differences observed for ACHD, Deutsch, and Moloney in dependence on the quality of the projection, it is reasonable to infer that those parameters are not substantially biased by inferior radiographic projections.
Differences in radiographic projections are a known factor that influence the measured parameters on shoulder radiographs, as was recently demonstrated in 86 shoulders, where the ACHD was significantly lower in supine radiographs than in upright weight-bearing radiographs [17], confirming the results of a study with 166 shoulders comparing supine CT and standing CT [18]. Also, the radiographic beam angle influences the measured parameters of shoulder radiographs, as was shown in a comparison between CT and radiographs in 28 shoulders [19]. Furthermore, the acromiohumeral distance is different between radiographic projections and cross-sectional imaging, as has been described in a study of 34 shoulders with massive rotator cuff tears [20].
While the effect of different radiographic projections has been investigated by several studies, the effect of shoulder rotation on the measurements of glenohumeral centering so far has not been explored in the literature. We investigated the effect of shoulder rotation on the measurement of glenohumeral centering for two reasons: the first being that patients with rotator cuff tears may not be able to hold the arm in the required position, and the second to address whether the action of the rotator cuff can affect glenohumeral centering in patients with and without rotator cuff tears. Even though statistically significant differences were found in our study when comparing the NEUT versus the ER position for ACHD and Deutsch, those cannot be considered clinically relevant, as the differences were smaller than 1 mm. Those observations were not dependent whether shoulders were in the rupture or the control group. As a side note, the small differences in ACHD can be attributed to a slightly smaller projection of the humeral head by approximately 0.5 mm in ER as compared to NEUT (data not shown) as the humerus is not perfectly spherical [21]. The finding of the rather constant results for ACHD and Deutsch is in line with a previous sonography-based study where no differences for ACHD in internal rotation, neutral position, and external rotation were found in non-abducted arms [22]. In contrast to ACHD and Deutsch, measuring glenohumeral centering using Moloney suggests the humeral head being translated caudally during external rotation by 2.5–3.5 mm. However, this is mainly due to different projections of the calcar in the radiographs. In NEUT, the calcar is projected en face, but it is out of plane and overlaid by the humeral head in ER, leading to the wrong assumption of glenohumeral decentering.
Shoulders with rotator cuff tears presented with a significantly smaller ACHD mean value of about 2–2.5 mm as compared to shoulders without a tear. For Moloney and Deutsch only by reader 2, a significant cranial migration of the humeral head by ≤ 1.4 mm was measured in patients with a rotator cuff tear as compared to controls. This inconsistency among the readers is most probably due to the difficulties to identify the landmarks for Deutsch and Moloney as stated above. The finding of a reduced ACHD in shoulders with rotator cuff tear was well expected and has been shown in many studies [23,24,25,26]. As a further refinement, our data strongly suggest that an ACHD ≤ 6 mm is a realistic threshold to infer a rotator cuff pathology since all of the 152 control shoulders had an ACHD of ≥ 7 mm. On the opposite, an ACHD of ≥ 7 mm has no predictive value with respect to the state of the rotator cuff since > 80% of shoulders with a rotator cuff tear also fall within this range. For the methods of Deutsch and Moloney, no such stringent thresholds could be established separating shoulders from the rupture and the control group as there is substantial overlap of the values in both groups.
We adopted a measure to quantify the extent of a rotator cuff tear by assessing the percentage of the greater tubercle exposed by the cuff tear [12]. Significant, albeit weak, correlations were found between the extent of the tear and the parameters for glenohumeral centering, with larger tear sizes being associated with a larger cranial migration of the humeral head. It is important to recognize that for an individual patient, the extent of the rotator cuff tear does not allow predicting the extent of cranial migration of the humeral head, while an ACHD ≤ 6 mm does predict a massive rotator cuff tear (> 66% of the greater tubercle exposed) with a positive predictive value of 90%.
We correlated a reduced ACHD in the subpopulation of massive rotator cuff tears with other MR-based parameters of the rotator cuff. The only consistent significant correlation was found for the tangent sign, which is more frequently present in shoulders with a reduced ACHD (75–90% as compared to approximately 40%). Other parameters like tendon retraction or fatty infiltration of the muscles did not, or only inconsistently, reveal significant differences. A positive tangent sign is the result of a combination of a rotator cuff tear, tendon retraction, and muscle atrophy and may explain why the correlation of the tangent sign with a reduced ACHD stands out. This of course confirms the well-known observation that a positive tangent sign is linked to massive rotator cuff tears [15].
As a limitation of the study, the control and the rupture group were neither age- nor gender-matched. This does not invalidate the findings when shoulder rotation was tested against glenohumeral centering as those were compared within the same shoulder. A lack of difference in those comparisons between the rupture and control group further corroborates this statement. An age-related change in glenohumeral centering independent of rotator cuff tears may have affected the comparison between control and rupture. We did not find, however, any statistical significant correlation between age and glenohumeral centering in the control group.
To conclude, only ACHD and Deutsch are independent on rotation of the glenohumeral joint. ACHD is the only parameter measured allowing a statement on the integrity of the rotator cuff: an ACHD ≤ 6 mm reliably predicts a massive rotator cuff tear with a positive predictive value of 90%.
References
Mall NA, Lee AS, Chahal J, Sherman SL, Romeo AA, Verma NN, et al. An evidenced-based examination of the epidemiology and outcomes of traumatic rotator cuff tears. Arthroscopy. 2013;29(2):366–76.
Tashjian RZ. Epidemiology, natural history, and indications for treatment of rotator cuff tears. Clin Sports Med. 2012;31(4):589–604.
Teunis T, Lubberts B, Reilly BT, Ring D. A systematic review and pooled analysis of the prevalence of rotator cuff disease with increasing age. J Shoulder Elbow Surg. 2014;23(12):1913–21.
Lugo R, Kung P, Ma CB. Shoulder biomechanics. Eur J Radiol. 2008;68(1):16–24.
Favard L, Bacle G, Berhouet J. Rotator cuff repair. Joint Bone Spine. 2007;74(6):551–7.
Gilat R, Haunschild ED, Williams BT, Fu MC, Garrigues GE, Romeo AA, et al. Patient factors associated with clinical failure following arthroscopic superior capsular reconstruction. Arthroscopy. 2020
Lee KW, Lee GS, Yang DS, Park SH, Chun YS, Choy WS. Clinical outcome of arthroscopic partial repair of large to massive posterosuperior rotator cuff tears: medialization of the attachment site of the rotator cuff tendon. Clin Orthop Surg. 2020;12(3):353–63.
Deutsch A, Altchek DW, Schwartz E, Otis JC, Warren RF. Radiologic measurement of superior displacement of the humeral head in the impingement syndrome. J Shoulder Elbow Surg. 1996;5(3):186–93.
Lee BG, Cho NS, Rhee YG. Results of arthroscopic decompression and tuberoplasty for irreparable massive rotator cuff tears. Arthroscopy. 2011;27(10):1341–50.
Bouaicha S, Hoch A, Jentzsch T, Moor BK. Impact of vertical and horizontal malrotation on measurements of anteroposterior radiographs of the scapula: need for standardized images in modern omometry. J Shoulder Elbow Surg. 2018;27(4):659–66.
Hamada K, Fukuda H, Mikasa M, Kobayashi Y. Roentgenographic findings in massive rotator cuff tears. A long-term observation. Clin Orthop Relat Res. 1990;254:92–6.
Schumaier A, Kovacevic D, Schmidt C, Green A, Rokito A, Jobin C, et al. Defining massive rotator cuff tears: a Delphi consensus study. J Shoulder Elbow Surg. 2020;29(4):674–80.
Patte D. Classification of rotator cuff lesions. Clin Orthop Relat Res. 1990;254:81–6.
Goutallier D, Postel JM, Bernageau J, Lavau L, Voisin MC. Fatty muscle degeneration in cuff ruptures. Pre- and postoperative evaluation by CT scan. Clin Orthop Relat Res. 1994;304:78–83.
Zanetti M, Gerber C, Hodler J. Quantitative assessment of the muscles of the rotator cuff with magnetic resonance imaging. Invest Radiol. 1998;33(3):163–70.
Koo TK, Li MY. A guideline of selecting and reporting intraclass correlation coefficients for reliability research. J Chiropr Med. 2016;15(2):155–63.
Sanguanjit P, Apivatgaroon A, Boonsun P, Srimongkolpitak S, Chernchujit B. The differences of the acromiohumeral interval between supine and upright radiographs of the shoulder. Sci Rep. 2022;12(1):9404.
Yoshida Y, Matsumura N, Yamada Y, Yamada M, Yokoyama Y, Matsumoto M, et al. Evaluation of three-dimensional acromiohumeral distance in the standing position and comparison with its conventional measuring methods. J Orthop Surg Res. 2020;15(1):436.
Ongbumrungphan W, Srikhum W, Chernchujit B. The effect of radiographic beam angle on acromiohumeral interval: 3D-CT analytic study. J Med Assoc Thai. 2015;98(Suppl 3):S61-65.
Mirzayan R, Donohoe S, Batech M, Suh BD, Acevedo DC, Singh A. Is there a difference in the acromiohumeral distances measured on radiographic and magnetic resonance images of the same shoulder with a massive rotator cuff tear? J Shoulder Elbow Surg. 2020;29(6):1145–51.
Jun BJ, Iannotti JP, McGarry MH, Yoo JC, Quigley RJ, Lee TQ. The effects of prosthetic humeral head shape on glenohumeral joint kinematics: a comparison of non-spherical and spherical prosthetic heads to the native humeral head. J Shoulder Elbow Surg. 2013;22(10):1423–32.
White CE, Dedrick GS, Apte GG, Sizer PS, Brismee JM. The effect of isometric shoulder internal and external rotation on the acromiohumeral distance. Am J Phys Med Rehabil. 2012;91(3):193–9.
Abrams JS, Song FS. Arthroscopic repair techniques for massive rotator cuff tears. Instr Course Lect. 2012;61:121–30.
Goutallier D, Le Guilloux P, Postel JM, Radier C, Bernageau J, Zilber S. Acromio humeral distance less than six millimeter: its meaning in full-thickness rotator cuff tear. Orthop Traumatol Surg Res. 2011;97(3):246–51.
Saupe N, Pfirrmann CW, Schmid MR, Jost B, Werner CM, Zanetti M. Association between rotator cuff abnormalities and reduced acromiohumeral distance. AJR Am J Roentgenol. 2006;187(2):376–82.
Siow MY, Mitchell BC, Hachadorian M, Wang W, Bastrom T, Kent WT, et al. Association between rotator cuff tears and superior migration of the humeral head: an MRI-based anatomic study. Orthop J Sports Med. 2021;9(6):23259671211009850.
Acknowledgements
The authors are thankful to Sabine Schrimpf, PhD, for careful proofreading of the manuscript.
Funding
Open access funding provided by University of Bern
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments of comparable ethical standards.
The study was approved by the institutional review board (2020–01298).
Consent to participate
All patients included in this study signed a general consent on the usage of health-related data for research purposes.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Egli, R.J., Widmer, E.C.J., Waltenspül, M. et al. The robustness of glenohumeral centering measurements in dependence of shoulder rotation and their predictive value in shoulders with rotator cuff tears. Skeletal Radiol 52, 183–191 (2023). https://doi.org/10.1007/s00256-022-04159-6
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-022-04159-6