Abstract
Objective
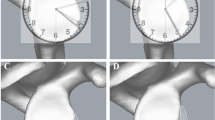
Glenoid bone loss is estimated using a best-fit circle method and requires software tools that may not be available. Our hypothesis is that a vertical reference line drawn parallel to the long axis of the glenoid and passing through the inflection point of the coracoid and glenoid will represent a demarcation line of approximately 20% of the glenoid. Our aim is to establish a more efficient method to estimate a surgical threshold for glenoid insufficiency.
Methods
Fifty patients with normal glenoid anatomy were randomly chosen from an orthopedic surgeon’s database. Two orthopedic surgeons utilized T1-weighted sagittal MRIs and the coracoglenoid line technique to determine the percentage of bony glenoid anterior to vertical line. Two musculoskeletal radiologists measured the same 50 glenoids using the circle technique. Differences were determined using dependent t test. Reliability was compared using interclass correlation coefficient and Kappa. Validity was compared using Pearson correlation coefficient.
Results
Mean surface area of the glenoid anterior to the vertical line was on average 21.69% ± 3.12%. Surface area of the glenoid using the circle method was on average 20.86% ± 2.29%. Inter-rater reliability of the circle method was 0.553 (fair). Inter-rater reliability of the vertical line technique was 0.83 (excellent). There was a linear relationship between circle and vertical line measurements, r = 0.704 (moderate to high).
Conclusion
The coracoglenoid line appears to represent a line of demarcation of approximately 21% of glenoid bone anterior to the coracoglenoid line. Our technique was found to be reliable, valid, and accurate.



Similar content being viewed by others
References
Piasecki DP, Verma NN, Romeo AA, Levine WN, Bach BR Jr, Provencher MT. Glenoid bone deficiency in recurrent anterior shoulder instability: diagnosis and management. J Am Acad Orthop Surg. 2009;17:482–93.
Taylor DC, Arciero RA. Pathologic changes associated with shoulder dislocations. Am J Sports Med. 1997;25:306–11.
Edwards TB, Boulahia A, Walch G. Radiographic analysis of bone defects in chronic anterior shoulder instability. Arthroscopy. 2003;19:732–9.
Bigliani LU, Newton PM, Steinmann SP, Connor PM, McIlveen SJ. Glenoid rim lesions associated with recurrent anterior dislocation of the shoulder. Am J Sports Med. 1998;26:41–5.
Griffith JF, Yung PS, Antonio GE, Tsang PH, Ahuja AT, Chan KM. CT compared with arthroscopy in quantifying glenoid bone loss. AJR Am J Roentgenol. 2007;189:1490–3.
Dickens JF, Slaven SE, Cameron KL, Pickett AM, Posner M, Campbell SE, Owens BD. Prospective evaluation of glenoid bone loss after first-time and recurrent anterior glenohumeral instability events. Am J Sports Med. 2019;47:1082–9.
Itoi E, Lee SB, Berglund LJ, Berge LL, An KN. The effect of a glenoid defect on anteroinferior stability of the shoulder after Bankart repair: a cadaveric study. J Bone Joint Surg Am. 2000;82:35–46.
Burkhart SS, Debeer JF, Tehrany AM, Parten PM. Quantifying glenoid bone loss arthroscopically in shoulder instability. Arthroscopy. 2002;18:488–91.
Burkhart SS, DeBeer JF. Traumatic glenohumeral bone defects and their relationship to failure of arthroscopic Bankart repairs: significance of the inverted-pear glenoid and the humeral engaging Hill-Sachs lesion. Arthroscopy. 2002;16:677–94.
Di Giacomo G, Itoi E, Burkhart SS. Evolving concept of bipolar bone loss and the Hill-Sachs lesion: From “engaging/non-engaging” lesion to “on-track/off-track” lesion. Arthroscopy. 2014;30(1):90–8.
Gowd AK, Liu JN, Cabarcas BC, Garcia GH, Cvetanovich GL, Provencher MT, Verma NN. Management of recurrent anterior shoulder instability with bipolar bone loss: a systematic review to assess critical bone loss amounts. Am J Sports Med. 2019;47(10):2484–93.
Garcia GH, Liu JN, Dines DM, Dines JS. Effect of bone loss in anterior shoulder instability. World J Orthop. 2015;6(5):421–33.
Rabinowitz J, Friedman R, Eichinger JK. Management of glenoid bone loss with anterior shoulder instability: Indications and outcomes. Curr Rev Musculoskelet Med. 2017;10:452–62.
Barchilon VS, Kotz E, Barchilon Ben-Av M, Glazer E, Nyska M. A simple method for quantitative evaluation of the missing area of the anterior glenoid in anterior instability of the glenohumeral joint. Skeletal Radiol. 2008;37:731–6.
Baudi P, Righi P, Bolognesi D, Rivetta S, Rossi Urtoler E, Guicciardi N, et al. How to identify and calculate glenoid bone defect. Chir Organi Mov. 2005;90(2):145–52.
Griffith JF. Measuring glenoid and humeral bone loss in shoulder dislocation. Quant Imaging Med Surg. 2019;9:134–43.
Chuang TY, Adams CR, Burkhart SS. Use of preoperative three-dimensional computed tomography to quantify glenoid bone loss in shoulder instability. Arthroscopy. 2008;24:376–82.
Sugaya H, Moriishi J, Dohi M, Kon Y, Tsuchiya A. Glenoid rim morphology in recurrent anterior glenohumeral instability. J Bone Joint Surg Am. 2003;85:878–84.
Walter WR, Samim M, LaPolla FWZ, Gyftopoulos S. Imaging quantification of glenoid bone loss in patients with glenohumeral instability: A systematic review. Am J Roentgenol. 2019;212:1096–105. https://doi.org/10.2214/AJR.18.20504.
Bakshi NK, Cibulas GA, Sekya JK, Bedi A. A Clinical comparison of linear and surface area-based methods of measuring glenoid bone loss. Am J Sports Med. 2018;46(10):2472–7.
Souza PM, Brandao BL, Brown E, Motta G, Monteiro M, Marchiori E. Recurrent anterior glenohumeral instability: the quantification of glenoid bone loss using magnetic resonance imaging. Skeletal Radiol. 2014;43:1085–92.
Stillwater L, Koenig J, Maycher B, Davidson M. 3D-MR vs. 3D-CT of the shoulder in patients with glenohumeral instability. Skeletal Radio.l. 2017;46:325–31.
Vopat BG, Cai W, Torriani M, Vopat ML, Hemma M, Harris GJ, et al. Measurement of glenoid bone loss with 3-dimensional magnetic resonance imaging: a matched computed tomography analysis. Arthroscopy. 2018;34:3141–7.
Shrout PE, Fleiss JL. Intraclass correlations: uses in assessing rater reliability. Psychol Bull. 1979;86(2):420–8.
Cicchetti DV. Guidelines, criteria, and rules of thumb for evaluating normed and standardized assessment instruments in psychology. Psychol Assess. 1994;6(4):284–90.
Bishop JY, Hidden KA, Jones GL, Hettrich CM, Wolf BR. MOON shoulder group. Factors influencing surgeon’s choice of procedure for anterior shoulder instability: A multicenter prospective cohort study. Arthroscopy. 2019;35:2014–25.
Klemt C, Toderita D, Nolte D, Di Federico E, Reilly P, Bull AMJ. The critical size of a defect in the glenoid causing anterior instability of the shoulder after a Bankart repair, under physiological joint loading. Bone Joint J. 2019;101-B(68):74.
Jeon YS, Jeong HY, Lee DK, Rhee YG. Borderline glenoid bone defect in anterior shoulder instability: Laterjet procedure versus Bankart repair. Am J Sports Med. 2018;46:2170–6.
Lacheta L, Herbst E, Voss A, Braun S, Jungmann P, Millett PJ, Imhoff A, Martetschlager F. Insufficient consensus regarding circle size and bone loss width using the ratio- “best fit circle”- method even with three-dimensional computed tomography. Knee Surg Sports Traumatol Arthrosc. 2019;27:3222–9.
Lansdown DA, Wang K, Bernardoni E, Frank RM, Yanke AB, Cole BJ, et al. Variability in the contour of cadaveric anterior and posterior glenoids based on ipsilateral 3-dimensional computed tomography reconstructions: Implications for clinical estimation of bone loss. Arthroscopy. 2018;34:2560–6.
Moroder P, Plachel F, Huettner A, Ernstbrunner L, Minkus M, Boehm E, et al. The effect of scapula tilt and best-fit circle placement when measuring glenoid bone loss in shoulder instability patients. Arthroscopy. 2018;34:398–404.
Acknowledgements
The authors would like to acknowledge and thank John Popovich Jr., PhD, DPT, ATC for his expertise and assistance with performing the statistical analysis for this project.
Each author certifies that he or she has no commercial associations (e.g., consultancies, stock ownership, equity interest, patent/licensing arrangements, etc.) that might pose a conflict of interest in connection with the submitted article.
IRB approval was obtained through Michigan State University. MSU study ID: STUDY00002101. This study was performed in accordance with the ethical standards in the 1964 Declaration of Helsinki and well as the US Health Insurance Portability and Accountability Act (HIPAA)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest related to this project.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Olmscheid, N., Crawford, S.D., Dickinson, C. et al. Novel anterior coracoglenoid line utilizing magnetic resonance imaging (MRI) corresponds with critical glenoid bone loss. Skeletal Radiol 51, 1433–1438 (2022). https://doi.org/10.1007/s00256-021-03981-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-021-03981-8