Abstract
Introduction
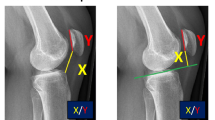
Many patella height indices exist in the literature. There is no single universally accepted radiological assessment for measuring patella height. The aims of this study were to determine which of the commonly used indices can most reliably measure patella height and compare the findings on both plain X-ray and magnetic resonance imaging (MRI) of the knee.
Methods
This case-controlled study compared patients with recurrent patella instability (patella group) to a control group. Two observers measured six validated patella height indices on X-ray and MRI of both groups at two separate time periods. Between-group and within-group statistical analysis was undertaken of the data. The inter- and intra-observer reliability was assessed using the intraclass correlation coefficient (ICC) and the kappa measure of agreement (k).
Results
Forty-four patients comprised the patella group and 50 patients the control group. There was a significant difference of most indices between the two groups (p < 0.05). There was a significant difference of most indices between the two imaging modalities (p < 0.05). The Insall-Salvati ratio had the greatest inter-observer reliability for both X-ray and MRI (ICC = 0.79 to 0.97; p < 0.001) (k = 0.50 to 1.00; p < 0.001).
Conclusion
Patella height indices significantly differ when measured on X-ray as compared to MRI. This may infer that a different set of normative values are required for each radiological modality, which we have proposed in this study. Overall, the Insall-Salvati ratio performed best and shows a high degree of intra- and inter-observer reliability on both X-ray and MRI.


Similar content being viewed by others
References
Fithian DC, Paxton EW, Stone ML, Silva P, Davis DK, Elias DA, et al. Epidemiology and natural history of acute patellar dislocation. Am J Sports Med. 2004;32:1114–21.
Buchanan G, Torres L, Czarkowski B, Giangarra CE. Current Concepts In The Treatment Of Gross Patellofemoral Instability. Int J Sports Phys Ther. 2016;11(6):867–76.
Dejour H, Walch G, Nove-Josserand L, Guier C. Factors of patellar instability: an anatomic radiographic study. Knee Surg Sports Traumatol Arthrosc. 1994;2:19–26.
Ward SR, Terk MR, Powers CM. Patella alta: association with patellofemoral alignment and changes in contact area during weight-bearing. J Bone Jt Surg. 2007;89:1749–55.
Biedert RM, Tscholl PM. Patella alta: a comprehensive review of current knowledge. Am J Orthop Belle Mead NJ. 2017;46:290–300.
Askenberger M, Janarv P-M, Finnbogason T, Arendt EA. Morphology and anatomic patellar instability risk factors in first-time traumatic lateral patellar dislocations: a prospective magnetic resonance imaging study in skeletally immature children. Am J Sports Med. 2017;45:50–8.
Insall J, Salvati E. Patella position in the normal knee joint. Radiology. 1971;101:101–4.
Grelsamer RP, Meadows S. The modified insall-salvati ratio for assessment of patellar height. Clin Orthop Relat Res. 1992;282:170–6.
Caton J, Deschamps G, Chambat P, Lerat JL, Dejour H. Patella infera. Apropos of 128 cases. Rev Chir Orthop Reparatrice Appar Mot. 1982;68:317–25.
Blackburne JS, Peel TE. A new method of measuring patellar height. J Bone Joint Surg Br. 1977;59:241–2.
Biedert RM, Albrecht S. The patellotrochlear index: a new index for assessing patellar height. Knee Surg Sports Traumatol Arthrosc. 2006;14:707–12.
Ali SA, Helmer R, Terk MR. Patella alta: lack of correlation between patellotrochlear cartilage congruence and commonly used patellar height ratios. Am J Roentgenol. 2009;193:1361–6.
Smith TO, Davies L, Toms AP, Hing CB, Donell ST. The reliability and validity of radiological assessment for patellar instability. A systematic review and meta-analysis. Skeletal Radiol. 2011;40:399–414.
Verhulst FV, van Sambeeck JDP, Olthuis GS, van der Ree J, Koëter S. Patellar height measurements: Insall-Salvati ratio is most reliable method. Knee Surg Sports Traumatol Arthrosc. 2020;28:869–75.
van Duijvenbode D, Stavenuiter M, Burger B, van Dijke C, Spermon J, Hoozemans M. The reliability of four widely used patellar height ratios. Int Orthop. 2016;40:493–7.
Yue R, Arendt E, Tompkins M. Patellar height measurements on radiograph and magnetic resonance imaging in patellar instability and control patients. J Knee Surg. 2017;30:943–50.
Shrout PE, Fleiss JL. Intraclass correlations: uses in assessing rater reliability. Psychol Bull US Am Psychol Assoc. 1979;86:420–8.
Landis JR, Koch GG. The measurement of observer agreement for categorical data. Biometrics. 1977;33:159–74.
Becher C, Fleischer B, Rase M, Schumacher T, Ettinger M, Ostermeier S, et al. Effects of upright weight bearing and the knee flexion angle on patellofemoral indices using magnetic resonance imaging in patients with patellofemoral instability. Knee Surg Sports Traumatol Arthrosc. 2017;25:2405–13.
Ye Q, Yu T, Wu Y, Ding X, Gong X. Patellar instability: the reliability of magnetic resonance imaging measurement parameters. BMC Musculoskelet Disord. 2019;20:317.
Lee PP, Chalian M, Carrino JA, Eng J, Chhabra A. Multimodality correlations of patellar height measurement on X-ray, CT, and MRI. Skeletal Radiol. 2012;41:1309–14.
Munch JL, Sullivan JP, Nguyen JT, Mintz D, Green DW, Shubin Stein BE, et al. Patellar Articular Overlap on MRI Is a Simple Alternative to Conventional Measurements of Patellar Height. Orthop J Sports Med. 2016;4:232596711665632.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethics approval
This was a retrospective case–control radiological study which did not require IRB/ethics committee approval.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Picken, S., Summers, H. & Al-Dadah, O. Inter- and intra-observer reliability of patellar height measurements in patients with and without patellar instability on plain radiographs and magnetic resonance imaging. Skeletal Radiol 51, 1201–1214 (2022). https://doi.org/10.1007/s00256-021-03937-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00256-021-03937-y