Abstract
Background
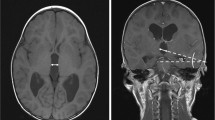
Third ventricle morphological changes reflect changes in the ventricular system in pediatric hydrocephalus, so visual inspection of the third ventricle shape is standard practice. However, normal pediatric reference data are not available.
Objective
To investigate both the normal development of the third ventricle in the 0–18-year age group and changes in its biometry due to hydrocephalus.
Materials and methods
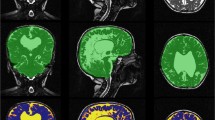
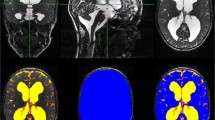
For this retrospective study, we selected individuals ages 0–18 years who had magnetic resonance imaging (MRI) from 2012 to 2020. We included 700 children (331 girls) who had three-dimensional (3-D) T1-weighted sequences without and 25 with hydrocephalus (11 girls). We measured the distances between the anatomical structures limiting the third ventricle by dividing the third ventricle into anterior and posterior regions. We made seven linear measurements and three index calculations using 3DSlicer and MRICloud pipeline, and we analyzed the results of 23 age groups in normal and hydrocephalic patients using SPSS (v. 23).
Results
Salient findings are: (1) The posterior part of the third ventricle is more affected by both developmental and hydrocephalus-related changes. (2) For third ventricle measurements, gender was insignificant while age was significant. (3) Normal third ventricular volumetric development showed a segmental increase in the 0–18 age range. The hydrocephalic third ventricle volume cut-off value in this age group was 3 cm3.
Conclusion
This study describes third ventricle morphometry using a linear measurement method. The ratios defined in the midsagittal plane were clinically useful for diagnosing the hydrocephalic third ventricle. The linear and volumetric reference data and ratios are expected to help increase diagnostic accuracy in distinguishing normal and hydrocephalic third ventricles.





Similar content being viewed by others
References
Dinçer A, Özek MM (2011) Radiologic evaluation of pediatric hydrocephalus. Childs Nerv Syst 27:1543–1562
Dlouhy BJ, Capuano AW, Madhavan K et al (2012) Preoperative third ventricular bowing as a predictor of endoscopic third ventriculostomy success. J Neurosurg Pediatr 9:182–190
Kerscher SR, Schweizer LL, Nägele T et al (2019) Changes of third ventricle diameter (TVD) mirror changes of the entire ventricular system after initial therapy and during follow-up in pediatric hydrocephalus. Eur J Paediatr Neurol 23:571–580
Birnbaum R, Parodi S, Donarini G et al (2018) The third ventricle of the human fetal brain: normative data and pathologic correlation. A 3D transvaginal neurosonography study. Prenat Diagn 38:664–672
Ambarki K, Israelsson H, Wåhlin A et al (2010) Brain ventricular size in healthy elderly: comparison between Evans index and volume measurement. Neurosurgery 67:94–99
Toma AK, Holl E, Kitchen ND, Watkins LD (2011) Evans’ index revisited: the need for an alternative in normal pressure hydrocephalus. Neurosurgery 68:939–944
Evans WA (1942) An encephalographic ratio for estimating ventricular enlargement and cerebral atrophy. Arch Neurol Psychiatr 47:931–937
Orellana C, Ferreira D, Muehlboeck JS et al (2016) Measuring global brain atrophy with the brain volume/cerebrospinal fluid index: normative values, cut-offs and clinical associations. Neurodegener Dis 16:77–86
Wu D, Ma T, Ceritoglu C et al (2016) Resource atlases for multi-atlas brain segmentations with multiple ontology levels based on T1-weighted MRI. Neuroimage 125:120–130
Lang J (1985) Surgical anatomy of the hypothalamus. Acta Neurochir 75:5–22
De Divitiis O, Angileri FF, D’Avella D et al (2002) Microsurgical anatomic features of the lamina terminalis. Neurosurgery 50:563–570
Yamamoto I, Rhoton AL, Peace DA (1981) Microsurgery of the third ventricle: part I. Microsurgical anatomy. Neurosurgery 8:334–356
Foroughi M, Wong A, Steinbok P et al (2011) Third ventricular shape: a predictor of endoscopic third ventriculostomy success in pediatric patients. J Neurosurg Pediatr 7:389–396
Segev Y, Metser U, Beni-Adani L et al (2001) Morphometric study of the midsagittal MR imaging plane in cases of hydrocephalus and atrophy and in normal brains. AJNR Am J Neuroradiol 22:1674–1679
Linninger AA, Tsakiris C, Zhu DC et al (2005) Pulsatile cerebrospinal fluid dynamics in the human brain. IEEE Trans Biomed Eng 52:557–565
Aydin S, Yilmazlar S, Aker S, Korfali E (2009) Anatomy of the floor of the third ventricle in relation to endoscopic ventriculostomy. Clin Anat 22:916–924
Metwally MI, Alkhalik Basha MA, Abdelhamid GA et al (2021) Neuroanatomical MRI study: reference values for the measurements of brainstem, cerebellar vermis, and peduncles. Br J Radiol 94:20201353
Raininko R, Autti T, Vanhanen SL et al (1994) The normal brain stem from infancy to old age. A morphometric MRI study. Neuroradiology 36:364–368
Koşar MI, Otaǧ I, Sabancioǧullari V et al (2013) Frontal lobe morphometry with MRI in a normal age group of 6-17 year-olds. Iran J Radiol 10:8–12
Lee T-O, Hwang H-S, De Salles A et al (2008) Inter-racial, gender and aging influences in the length of anterior commissure-posterior commissure line. J Korean Neurosurg Soc 43:79–84
Feletti A, Fiorindi A, Lavecchia V et al (2021) A light on the dark side: in vivo endoscopic anatomy of the posterior third ventricle and its variations in hydrocephalus. J Neurosurg 135:309–317
Cinalli G, Spennato P, Nastro A et al (2011) Hydrocephalus in aqueductal stenosis. Childs Nerv Syst 27:1621–1642
Siyahhan B, Knobloch V, De Zélicourt D et al (2014) Flow induced by ependymal cilia dominates near-wall cerebrospinal fluid dynamics in the lateral ventricles. J R Soc Interface 11:20131189
Østby Y, Tamnes CK, Fjell AM et al (2009) Heterogeneity in subcortical brain development: a structural magnetic resonance imaging study of brain maturation from 8 to 30 years. J Neurosci 29:11772–11782
Xenos C, Sgouros S, Natarajan K (2002) Ventricular volume change in childhood. J Neurosurg 97:584–590
Pinggera D, Kerschbaumer J, Petr O et al (2017) The volume of the third ventricle as a prognostic marker for shunt dependency after aneurysmal subarachnoid hemorrhage. World Neurosurg 108:107–111
Acer N (2021) A comparison of automated segmentation and manual tracing for quantifying lateral ventricle volumes using MR imaging. Erciyes Med J 44:148–155
Yepes-Calderon F, Nelson MD, McComb JG (2018) Automatically measuring brain ventricular volume within PACS using artificial intelligence. PLoS One 13:e0193152
Cutler NS, Srinivasan S, Aaron BL et al (2020) Normal cerebral ventricular volume growth in childhood. J Neurosurg Pediatr 26:517–524
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Isıklar, S., Turan Ozdemir, S., Ozkaya, G. et al. Morphological evaluation of the normal and hydrocephalic third ventricle on cranial magnetic resonance imaging in children: a retrospective study. Pediatr Radiol 53, 282–296 (2023). https://doi.org/10.1007/s00247-022-05475-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00247-022-05475-8