Abstract
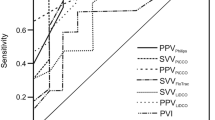
Dynamic parameters of fluid responsiveness (FR), namely aortic blood flow velocity variation (delta V peak), left ventricular velocity-time integral variation (delta VTI), stroke volume variation, and pulse pressure variation (PPV) have demonstrated good diagnostic performance for the prediction of response to fluid loading in mechanically ventilated critically ill adult patients. We aimed to evaluate these parameters in children undergoing cardiac surgery. A retrospective observational study of mechanically ventilated patients weighing less than 20 kg who received a volume expansion (VE) of 10 ml/kg after sternal closure was conducted. A 10% cardiac index (CI) increase divided patients into 7 responders (R) and 9 non-responders (NR). Transesophageal echocardiography and Pressure Recording Analytical Method data were retrieved. The percentage CI increase was 18.6 (12)% in R and 2.9 (5.7)% in NR (p = 0.037). Prior to VE, delta V peak, delta VTI, PPV, and SPV differed between R and NR (p = 0.045, 0.043, 0.048, 0,037 and 0.044, respectively). Systolic (p = 0.004), diastolic (p = 0.002), mean blood pressure (p = 0.003), delta V peak (p = 0.03), delta VTI (p = 0.04), CI (p = 0.01), PPV (p = 0.04), SPV (p = 0.04), and dP/dt max (maximal pressure-to-time ratio) (p = 0.02) changed the following VE in R patients. Delta V peak decreased after VE in NR patients (p = 0.004). Delta VTI and PPV showed the highest predictive values, with area under receiver operator characteristic curves of 0.76 (p = 0.049) and 0.76 (p = 0.045), respectively. Delta VTI and PPV were revealed to be potential predictors of FR in ventilated children after cardiac surgery. Their combined evaluation could be useful for fluid management after sternal closure.

Similar content being viewed by others
References
Wessel DL (2001) Managing low cardiac output syndrome after congenital heart surgery. Crit Care Med 29:S220–S230
Ricci Z, Iacoella C, Cogo P (2011) Fluid management in critically ill pediatric patients with congenital heart disease. Minerva Pediatr 63:399–410
Bendjelid K, Romand JA (2003) Fluid responsiveness in mechanically ventilated patients: a review of indices used in intensive care. Intensive Care Med 29:352–356
Durand P, Chevret L, Essouri S, Haas V, Devictor D (2008) Respiratory variations in aortic blood flow predict fluid responsiveness in ventilated children. Intensive Care Med 34:888–894
de Souza Neto EP, Grousson S, Duflo F, Ducreux C, Joly H, Convert J, Mottolese C, Dailler F, Cannesson M (2011) Predicting fluid responsiveness in mechanically ventilated children under general anaesthesia using dynamic parameters and transthoracic echocardiography. Br J Anaesth 106:856–864
Renner J, Broch O, Duetschke P, Scheewe J, Höcker J, Moseby M, Jung O, Bein B (2012) Prediction of fluid responsiveness in infants and neonates undergoing congenital heart surgery. Br J Anaesth 108:108–115
Michard F (2005) Changes in arterial pressure during mechanical ventilation. Anesthesiology 13:419–428
Desgranges FP, Desebbe O, de Souza Neto EP, Raphael D, Chassard D (2016) Respiratory variation in aortic blood flow peak velocity to predict fluid responsiveness in mechanically ventilated children: a systematic review and meta-analysis. Paediatr Anaesth 26:37–47
Romano SM, Pistolesi M (2002) Assessment of cardiac output from systemic arterial pressure in humans. Crit Care Med 30:1834–1841
Favia I, Rizza A, Garisto C, Haiberger R, Di Chiara L, Romagnoli S, Ricci Z. (2016) Cardiac index assessment by the pressure recording analytical method in infants after paediatric cardiac surgery: a pilot retrospective study. Interact Cardiovasc Thorac Surg. Epub ahead of print
Benes J, Giglio M, Brienza N (2014) The effect of goal-directed fluid therapy based on dynamic parameters on post-surgical outcome: a meta-analysis of randomized controlled trials. Crit Care 18:584
Akao M, Katsube Y, Kamisago M, Watanabe M, Abe M, Fukazawa R, Ogawa S, Itoh Y (2013) Developmental changes in left and right ventricular function evaluated with color tissue Doppler imaging and strain echocardiography. J Nippon Med Sch 80:260–267
Rowland DG, Gutgesell HP (1995) Noninvasive assessment of myocardial contractility, preload, and afterload in healthy newborn infants. Am J Cardiol 75:818–821
Senzaki H, Akagi M, Hishi T, Ishizawa A, Yanagisawa M, Masutani S, Kobayashi T, Awa S (2002) Age-associated changes in arterial elastic properties in children. Eur J Pediatr 161:547–551
Loosli CG, Potter EL (1959) Pre- and postnatal development of the respiratory portion of the human lung with special reference to the elastic fibers. Am Rev Respir Dis 80:5–23
De Backer D, Heenen S, Piagnerelli M, Koch M, Vincent JL (2005) Pulse pressure variations to predict fluid responsiveness: influence of tidal volume. Intensive Care Med 31:517–523
Monnet X, Rienzo M, Osman D, Anguel N, Richard C, Pinsky MR, Teboul JL (2005) Esophageal doppler monitoring predicts fluid responsiveness in critically ill ventilated patients. Intensive Care Med 31:1195–1201
Hadian M, Severyn DA, Pinsky MR (2011) The effects of vasoactive drugs on pulse pressure and stroke volume variation in postoperative ventilated patients. J Crit Care 26:328
Saxena R, Durward A, Steeley S, Murdoch IA, Tibby SM (2015) Predicting fluid responsiveness in 100 critically ill children: the effect of baseline contractility. Intensive Care Med 41:2161–2169
Kim JW, Bang JY, Park CS, Gwak M, Shin WJ, Hwang GS (2016) Usefulness of the maximum rate of pressure rise in the central and peripheral arteries after weaning from cardiopulmonary bypass in pediatric congenital heart surgery: a retrospective analysis. Medicine (Baltimore) 95:e5405
Choi DY, Kwak HJ, Park HY, Kim YB, Choi CH, Lee JY (2010) Respiratory variation in aortic blood flow velocity as a predictor of fluid responsiveness in children after repair of ventricular septal defect. Pediatr Cardiol 31:1166–1170
Romagnoli S, Ricci Z, Quattrone D, Tofani L, Tujjar O, Villa G, Romano SM, De Gaudio AR (2014) Accuracy of invasive arterial pressure monitoring in cardiovascular patients: an observational study. Crit Care 18:644
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no financial or non-financial conflict of interest.
Informed Consent
Formal consent is not required because we conducted a retrospective study.
Research Involving Human and Animal Participants
All procedures performed in this study were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. This article does not contain any studies with animals performed by any of the authors.
Rights and permissions
About this article
Cite this article
Favia, I., Romagnoli, S., Di Chiara, L. et al. Predicting Fluid Responsiveness in Children Undergoing Cardiac Surgery After Cardiopulmonary Bypass. Pediatr Cardiol 38, 787–793 (2017). https://doi.org/10.1007/s00246-017-1582-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00246-017-1582-0