Abstract
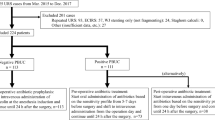
There is controversy regarding the predicting value of preoperative urine culture for post-percutaneous nephrolithotripsy (PCNL) infection. The purpose of our study was to re-evaluate the importance of preoperative urine culture for developing post-PCNL systemic inflammatory response syndrome (SIRS) in China. A total of 303 patients undergone PCNL from March 2012 to January 2018 were recruited. Urine tests, urine cultures and the perioperative data were prospectively recorded and analyzed. 95 patients (31.4%) were identified with positive preoperative urine cultures. Female patients had significantly higher rate of urine cultures positivity than that in male patients (42.9% vs. 21.5%, p < 0.01). Escherichia coli was the most common organism (56 cases, 58.9%) in patients with positive urine cultures and 35.7% of E. coli-positive patients developed SIRS after PCNL. Even with intensive perioperative prophylaxis, patients with positive urine cultures had a higher rate of post-PCNL SIRS than those patients with negative urine cultures (p = 0.043). On multivariable analysis, preoperative positive urine cultures (OR 1.943, 95% CI 1.11–3.39, p = 0.019), preoperative neutrophils (OR 1.228, 95% CI 1.07–1.41, p = 0.003), intraoperative pyonephrosis (OR 3.37, 95% CI 1.44–9.71, p = 0.01) and postoperative hospitalization (OR 1.154, 95% CI 1.05–1.28, p = 0.005) were independent risk factors for postoperative SIRS. These results demonstrated that preoperative urine culture still played a role in predicting post-PCNL SIRS, but it was unable to prevent the occurrence of SIRS even with intensive perioperative prophylaxis based on urine culture results. Further studies are required to explore the predicting role of advanced preoperative bacterial detecting techniques in post-PCNL infectious complications.


Similar content being viewed by others
References
Seitz C, Desai M, Hacker A, Hakenberg OW, Liatsikos E, Nagele U, Tolley D (2012) Incidence, prevention, and management of complications following percutaneous nephrolitholapaxy. Eur Urol 61(1):146–158. https://doi.org/10.1016/j.eururo.2011.09.016
Gutierrez J, Smith A, Geavlete P, Shah H, Kural AR, de Sio M, Amon Sesmero JH, Hoznek A, de la Rosette J, Group CPS (2013) Urinary tract infections and post-operative fever in percutaneous nephrolithotomy. World J Urol 31(5):1135–1140. https://doi.org/10.1007/s00345-012-0836-y
Benson AD, Juliano TM, Miller NL (2014) Infectious outcomes of nephrostomy drainage before percutaneous nephrolithotomy compared to concurrent access. J Urol 192(3):770–774. https://doi.org/10.1016/j.juro.2014.03.004
Erdil T, Bostanci Y, Ozden E, Atac F, Yakupoglu YK, Yilmaz AF, Sarikaya S (2013) Risk factors for systemic inflammatory response syndrome following percutaneous nephrolithotomy. Urolithiasis 41(5):395–401. https://doi.org/10.1007/s00240-013-0570-y
Korets R, Graversen JA, Kates M, Mues AC, Gupta M (2011) Post-percutaneous nephrolithotomy systemic inflammatory response: a prospective analysis of preoperative urine, renal pelvic urine and stone cultures. J Urol 186(5):1899–1903. https://doi.org/10.1016/j.juro.2011.06.064
Paonessa JE, Gnessin E, Bhojani N, Williams JC Jr, Lingeman JE (2016) Preoperative bladder urine culture as a predictor of intraoperative stone culture results: clinical implications and relationship to stone composition. J Urol 196(3):769–774. https://doi.org/10.1016/j.juro.2016.03.148
Eswara JR, Shariftabrizi A, Sacco D (2013) Positive stone culture is associated with a higher rate of sepsis after endourological procedures. Urolithiasis 41(5):411–414. https://doi.org/10.1007/s00240-013-0581-8
Mariappan P, Smith G, Bariol SV, Moussa SA, Tolley DA (2005) Stone and pelvic urine culture and sensitivity are better than bladder urine as predictors of urosepsis following percutaneous nephrolithotomy: a prospective clinical study. J Urol 173(5):1610–1614. https://doi.org/10.1097/01.ju.0000154350.78826.96
Bonkat G, Bruyère F, Cai T, Geerlings SE, Köves B, Schubert S, Wagenlehner F (2019) Guidelines on urological infections. https://uroweb.org/guideline/urological-infections/. Accessed 16 June 2019
Armitage JN, Irving SO, Burgess NA, British Association of Urological Surgeons Section of E (2012) Percutaneous nephrolithotomy in the United kingdom: results of a prospective data registry. Eur Urol 61(6):1188–1193. https://doi.org/10.1016/j.eururo.2012.01.003
Koras O, Bozkurt IH, Yonguc T, Degirmenci T, Arslan B, Gunlusoy B, Aydogdu O, Minareci S (2015) Risk factors for postoperative infectious complications following percutaneous nephrolithotomy: a prospective clinical study. Urolithiasis 43(1):55–60. https://doi.org/10.1007/s00240-014-0730-8
Michel MS, Trojan L, Rassweiler JJ (2007) Complications in percutaneous nephrolithotomy. Eur Urol 51(4):899–906. https://doi.org/10.1016/j.eururo.2006.10.020(discussion 906)
Kreydin EI, Eisner BH (2013) Risk factors for sepsis after percutaneous renal stone surgery. Nat Rev Urol 10(10):598–605. https://doi.org/10.1038/nrurol.2013.183
McAleer IM, Kaplan GW, Bradley JS, Carroll SF, Griffith DP (2003) Endotoxin content in renal calculi. J Urol 169(5):1813–1814. https://doi.org/10.1097/01.ju.0000061965.51478.79
Tuzel E, Aktepe OC, Akdogan B (2013) Prospective comparative study of two protocols of antibiotic prophylaxis in percutaneous nephrolithotomy. J Endourol 27(2):172–176. https://doi.org/10.1089/end.2012.0331
Seyrek M, Binbay M, Yuruk E, Akman T, Aslan R, Yazici O, Berberoglu Y, Muslumanoglu AY (2012) Perioperative prophylaxis for percutaneous nephrolithotomy: randomized study concerning the drug and dosage. J Endourol 26(11):1431–1436. https://doi.org/10.1089/end.2012.0242
Chen D, Jiang C, Liang X, Zhong F, Huang J, Lin Y, Zhao Z (2018) Early and rapid prediction of postoperative infections following percutaneous nephrolithotomy in patients with complex kidney stones. BJU Int. https://doi.org/10.1111/bju.14484
Siddiqui H, Nederbragt AJ, Lagesen K, Jeansson SL, Jakobsen KS (2011) Assessing diversity of the female urine microbiota by high throughput sequencing of 16S rDNA amplicons. BMC Microbiol 11:244. https://doi.org/10.1186/1471-2180-11-244
Wolfe AJ, Brubaker L (2015) “Sterile urine” and the presence of bacteria. Eur Urol 68(2):173–174. https://doi.org/10.1016/j.eururo.2015.02.041
Hilt EE, McKinley K, Pearce MM, Rosenfeld AB, Zilliox MJ, Mueller ER, Brubaker L, Gai X, Wolfe AJ, Schreckenberger PC (2014) Urine is not sterile: use of enhanced urine culture techniques to detect resident bacterial flora in the adult female bladder. J Clin Microbiol 52(3):871–876. https://doi.org/10.1128/jcm.02876-13
Antunes-Lopes T, Vale L, Coelho AM, Silva C, Rieken M, Geavlete B, Rashid T, Rahnama’i SM, Cornu JN, Marcelissen T (2018) The role of urinary microbiota in lower urinary tract dysfunction: a systematic review. Eur Urol Focus. https://doi.org/10.1016/j.euf.2018.09.011
Foxman B (2002) Epidemiology of urinary tract infections: incidence, morbidity, and economic costs. Am J Med 113(Suppl 1A):5s–13s
el-Nahas AR, Eraky I, Shokeir AA, Shoma AM, el-Assmy AM, el-Tabey NA, Soliman S, Elshal AM, el-Kappany HA, el-Kenawy MR (2012) Factors affecting stone-free rate and complications of percutaneous nephrolithotomy for treatment of staghorn stone. Urology 79(6):1236–1241. https://doi.org/10.1016/j.urology.2012.01.026
Funding
This study was funded by the Key Research and Development Plan of Shandong Province (2017GSF221005; 2016GSF201011).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no competing interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Liu, J., Zhou, C., Gao, W. et al. Does preoperative urine culture still play a role in predicting post-PCNL SIRS? A retrospective cohort study. Urolithiasis 48, 251–256 (2020). https://doi.org/10.1007/s00240-019-01148-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00240-019-01148-8