Abstract
Purpose
Pilocytic astrocytoma (PA) is rare in adults, and only limited knowledge on the clinical course and prognosis has been available. The combination of clinical information and comprehensive imaging parameters could be used for accurate prognostic stratification in adult PA patients. This study was conducted to predict the prognostic factors from clinical information and conventional magnetic resonance imaging (MRI) features in adult PAs.
Methods
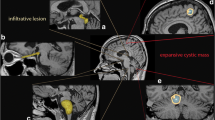
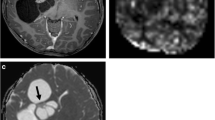
A total of 56 adult PA patients were enrolled in the institutional cohort. Clinical characteristics including age, sex, anaplastic PA, presence of neurofibromatosis type 1, Karnofsky performance status, extent of resection, and postoperative treatment were collected. MRI characteristics including major axis length, tumor location, presence of the typical ‘cystic mass with enhancing mural nodule appearance’, proportion of enhancing tumor, the proportion of edema, conspicuity of the nonenhancing margin, and presence of a cyst were evaluated. Univariable and multivariable Cox proportional hazard modeling were performed.
Results
The 5-year progression-free survival (PFS) and overall survival (OS) rates were 83.9% and 91.l%, respectively. On univariable analysis, older age, larger proportion of edema, and poor definition of nonenhancing margin were predictors of shorter PFS and OS, respectively (all Ps < .05). On multivariable analysis, older age (hazard ratio [HR] = 1.04, P = .014; HR = 1.14, P = .030) and poor definition of nonenhancing margin (HR = 3.66, P = .027; HR = 24.30, P = .024) were independent variables for shorter PFS and OS, respectively.
Conclusion
Age and the margin of the nonenhancing part of the tumor may be useful biomarkers for predicting the outcome in adult PAs.



Similar content being viewed by others
Data availability
Data will be available upon request. Currently, data will not be deposited to a specific repository.
Code availability
No specific codes were used to be disclosed.
References
Louis DN, Perry A, Reifenberger G et al (2016) The 2016 World Health Organization classification of tumors of the central nervous system: a summary. Acta Neuropathol 131(6):803–820
Ostrom QT, Gittleman H, Truitt G, Boscia A, Kruchko C, Barnholtz-Sloan JS (2018) CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2011–2015. Neuro Oncol. 20(suppl_4):iv1–iv86
Burkhard C, Di Patre PL, Schüler D et al (2003) A population-based study of the incidence and survival rates in patients with pilocytic astrocytoma. J Neurosurg 98(6):1170–1174
Bell D, Chitnavis BP, Al-Sarraj S, Connor S, Sharr MM, Gullan RW (2004) Pilocytic astrocytoma of the adult—clinical features, radiological features and management. Br J Neurosurg 18(6):613–616
Garcia DM, Fulling KH (1985) Juvenile pilocytic astrocytoma of the cerebrum in adults. A distinctive neoplasm with favorable prognosis. J Neurosurg. 63(3):382–386
Brown PD, Anderson SK, Carrero XW et al (2015) Adult patients with supratentorial pilocytic astrocytoma: long-term follow-up of prospective multicenter clinical trial NCCTG-867251 (Alliance). Neurooncol Pract 2(4):199–204
Johnson DR, Brown PD, Galanis E, Hammack JE (2012) Pilocytic astrocytoma survival in adults: analysis of the Surveillance, Epidemiology, and End Results Program of the National Cancer Institute. J Neurooncol 108(1):187–193
Mair MJ, Wöhrer A, Furtner J et al (2020) Clinical characteristics and prognostic factors of adult patients with pilocytic astrocytoma. J Neurooncol 148(1):187–198
Tabash MA (2019) Characteristics, survival and incidence rates and trends of pilocytic astrocytoma in children in the United States; SEER-based analysis. J Neurol Sci 400:148–152
Dodgshun AJ, Maixner WJ, Hansford JR, Sullivan MJ (2016) Low rates of recurrence and slow progression of pediatric pilocytic astrocytoma after gross-total resection: justification for reducing surveillance imaging. J Neurosurg Pediatr 17(5):569–572
Ishkanian A, Laperriere NJ, Xu W et al (2011) Upfront observation versus radiation for adult pilocytic astrocytoma. Cancer 117(17):4070–4079
Lee KJ, Marchan E, Peterson J et al (2018) Management and survival of adult patients with pilocytic astrocytoma in the National Cancer Database. World Neurosurg 112:e881–e887
Jungk C, Reinhardt A, Warta R, et al (2019) Extent of resection, MGMT promoter methylation status and tumor location independently predict progression-free survival in adult sporadic pilocytic astrocytoma. Cancers11:8
Park YW, Han K, Ahn SS et al (2018) Prediction of IDH1-mutation and 1p/19q-codeletion status using preoperative MR imaging phenotypes in lower grade gliomas. AJNR Am J Neuroradiol 39(1):37–42
Park YW, Park JE, Ahn SS, et al (2021) Magnetic resonance imaging parameters for noninvasive prediction of epidermal growth factor receptor amplification in isocitrate dehydrogenase-wild-type lower-grade gliomas: a multicenter study. Neurosurgery
Park CJ, Han K, Shin H et al (2020) MR image phenotypes may add prognostic value to clinical features in IDH wild-type lower-grade gliomas. Eur Radiol 30(6):3035–3045
Gutman DA, Cooper LA, Hwang SN et al (2013) MR imaging predictors of molecular profile and survival: multi-institutional study of the TCGA glioblastoma data set. Radiology 267(2):560–569
Yan H, Parsons DW, Jin G et al (2009) IDH1 and IDH2 mutations in gliomas. N Engl J Med 360(8):765–773
Collins VP, Jones DT, Giannini C (2015) Pilocytic astrocytoma: pathology, molecular mechanisms and markers. Acta Neuropathol 129(6):775–788
Gaudino S, Martucci M, Russo R et al (2017) MR imaging of brain pilocytic astrocytoma: beyond the stereotype of benign astrocytoma. Childs Nerv Syst 33(1):35–54
Nicolasjilwan M, Hu Y, Yan C et al (2015) Addition of MR imaging features and genetic biomarkers strengthens glioblastoma survival prediction in TCGA patients. J Neuroradiol 42(4):212–221
Park YW, Kim D, Eom J et al (2021) “A diagnostic tree for differentiation of adult pilocytic astrocytomas from high-grade gliomas.” Eur J Radiol 143:109946
Nabors LB, Portnow J, Ahluwalia M et al (2020) Central nervous system cancers, version 3.2020, NCCN clinical practice guidelines in oncology. J Natl Compr Canc Netw. 18(11):1537–1570
Cho BK, Jung HL, Ghim TT et al (2005) KSPNO protocol for glioma. Korean J Pediatr Hematol-Oncol 12(2):244–285
Ye JM, Ye MJ, Kranz S, Lo P (2014) A 10 year retrospective study of surgical outcomes of adult intracranial pilocytic astrocytoma. J Clin Neurosci 21(12):2160–2164
Theeler BJ, Ellezam B, Sadighi ZS et al (2014) Adult pilocytic astrocytomas: clinical features and molecular analysis. Neuro Oncol 16(6):841–847
Stüer C, Vilz B, Majores M, Becker A, Schramm J, Simon M (2007) Frequent recurrence and progression in pilocytic astrocytoma in adults. Cancer 110(12):2799–2808
Saunders DE, Phipps KP, Wade AM, Hayward RD (2005) Surveillance imaging strategies following surgery and/or radiotherapy for childhood cerebellar low-grade astrocytoma. J Neurosurg 102(2 Suppl):172–178
Park JH, Jung N, Kang SJ et al (2019) Survival and prognosis of patients with pilocytic astrocytoma: a single-center study. Brain Tumor Res Treat 7(2):92–97
Lee M, Han K, Ahn SS et al (2019) The added prognostic value of radiological phenotype combined with clinical features and molecular subtype in anaplastic gliomas. J Neurooncol 142(1):129–138
Coakley KJ, Huston J 3rd, Scheithauer BW, Forbes G, Kelly PJ (1995) Pilocytic astrocytomas: well-demarcated magnetic resonance appearance despite frequent infiltration histologically. Mayo Clin Proc 70(8):747–751
Hayostek CJ, Shaw EG, Scheithauer B et al (1993) Astrocytomas of the cerebellum. A comparative clinicopathologic study of pilocytic and diffuse astrocytomas. Cancer. 72(3):856–869
Jain R, Poisson LM, Gutman D et al (2014) Outcome prediction in patients with glioblastoma by using imaging, clinical, and genomic biomarkers: focus on the nonenhancing component of the tumor. Radiology 272(2):484–493
Wu CX, Lin GS, Lin ZX et al (2015) Peritumoral edema on magnetic resonance imaging predicts a poor clinical outcome in malignant glioma. Oncol Lett 10(5):2769–2776
Funding
This research was supported by Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (2020R1I1A1A01071648).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Ethics approval
Approval was obtained from the ethics committee of Severance Hospital, Yonsei University, College of Medicine (IRB#: 4–2021-0444).
Consent to participate
Informed consent was waived by the institutional review board of our institution (refer to “Ethics approval” section).
Consent for publication
Informed consent was waived by the institutional review board of our institution (refer to “Ethics approval” section).
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Shin, I., Park, Y.W., Ahn, S.S. et al. Clinical factors and conventional MRI may independently predict progression-free survival and overall survival in adult pilocytic astrocytomas. Neuroradiology 64, 1529–1537 (2022). https://doi.org/10.1007/s00234-021-02872-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00234-021-02872-y